Playlist
Show Playlist
Hide Playlist
Graves Disease
-
Slides Thyroid Disease.pdf
-
Reference List Endocrinology.pdf
-
Reference List Thyroid Disorders.pdf
-
Download Lecture Overview
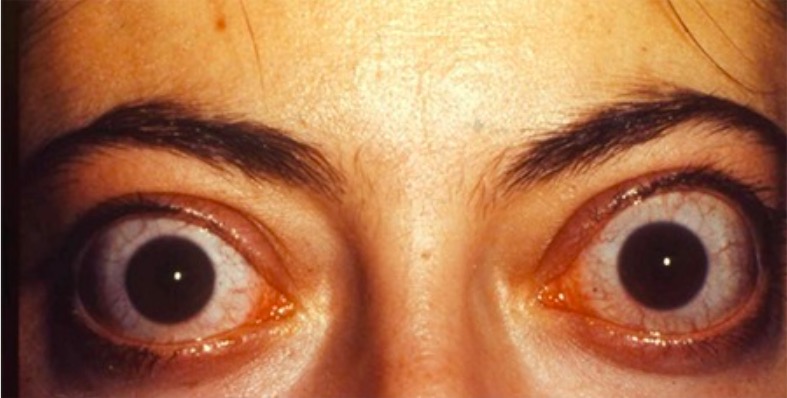
00:01 Graves' disease is an autoimmune disorder that can affect the thyroid, the eyes and the skin. 00:06 It is the most common cause of hyperthyroidism in the United States. 00:12 Stimulation of autonomous production of T4 and T3 is through antibodies against TSH receptors. 00:19 These receptors can be checked in the serum as a TSI or thyroid stimulating immunoglobulin or thyroid releasing antibody. 00:28 A positive family history is always a frequent accompaniment. 00:32 A new diagnosis of Graves' disease, one would start by checking thyroid stimulating immunoglobulins which are there to stimulate TSH receptors present on the thyroid gland which in turn increase the activity of the gland with consequent increased production of thyroid hormones, usually T4 and occassionally T3. 00:52 Thyroid function test reveal the classic features of low TSH, high T4 and/or T3. 01:01 Let's go through some of the clinical signs of Graves' disease. 01:05 Patients may have an elevated blood pressure on physical exam and may also have a widening of their pulse pressure. 01:12 A widening of the pulse pressure manifests when the systolic blood pressure is much higher than the diastolic blood pressure. 01:19 This is the hallmark of thyroid hormone effect on the heart where increased cardiac output and increased pumping of the myocardium occurs, thus widening the pulse pressure. 01:32 Patients also manifest clinically with tachycardias. 01:36 These tachycardias may be regular or irregular. 01:39 If they're irregular, they're called atrial fibrillation. 01:43 There's also a diffusely enlarged thyroid and occassionally, a thyroid bruit which is the abnormal sound that the blood vessels of the thyroid make as blood flows through them rapidly. 01:56 Patients may also manifest pretibial myxedema which we'll describe in subsequent slides And they have the characteristic eye signs. 02:04 These eye signs can include lid retraction or lid lag, proptosis which look like bulging of the eye in the orbit, scleral injection where the sclera of the eye appears red and finally, periorbital edema with the entire orbit seems to be swollen In the right image, you see many of the features of classic dysthyroid eye disease. 02:28 The diagnosis of Graves' disease is made clinically in most cases. 02:32 The first lab to check off the TSH and free T4 would be the thryoid stimulating antibodies Radio active iodine uptake and scan will show increased uptake with diffuse activity on the scan image. 02:47 The treatment of Graves' disease is a stepwise approach, usually starting with thioanamide drugs, followed by beta blockers to control heart rate. 02:56 If the thyrotoxicosis recurs or if there are any compressive symptoms of the thyroid gland, surgery is considered. 03:04 In the absence of a response to medications, one can also consider radioactive iodine ablation therapy. 03:11 Thionamide drugs can be used consecutively for up to two years. 03:15 Methimazole, one of the first line agents has a higher intrathyroid retention rate and therefore is more effective. 03:24 Typically, once-daily dosing also makes this drug quite convenient and it has a reduced side effect profile. 03:30 One important thing to be aware of is a first trimester teratogen causing a condition called aplasia cutis in the fetus. 03:39 This should be taken into account especially when prescribing methimazole to women of reproductive age. 03:45 Another drug is called propylthiouracil or PTU which has limitations based on its side effects. 03:52 It can increase aminotransferase levels and affect the liver and in very rare cases lead to fatal hepatotoxicity. 04:00 Second line treatment for Graves' disease includes radioactive iodine ablation which will, in most cases, render the patient completely hypothyroid. 04:09 As a consequence, they then would require lifelong thyroid replacement. 04:13 Finally, surgery is considered in patients in whom control cannot be achieved with drugs and who are not comfortable with radioiodine therapy. 04:23 Other lab pattern of thyroid disease worth mentioning. 04:26 When you see an elevated TSH with an elevated T4 and/or T3, consider the rare condition of secondary hyperthyroidism that is caused by TSH-secreting pituitary adenoma. 04:39 Where the TSH is low plus a normal free T4 but an elevated T3, this is the condition we described earlier known as T3 toxicosis. 04:49 And then finally if the TSH is low with a normal T4 and T3, consider the condition of subclinical hyperthyroidsm. 04:57 Typical causes of which include pregnancy and other non-thyroidal illness.
About the Lecture
The lecture Graves Disease by Michael Lazarus, MD is from the course Thyroid Disorders. It contains the following chapters:
- Graves' Disease
- Graves' Disease – Treatment
- Other Lab Patterns of Thyroid Disease
Included Quiz Questions
Which of the following best describes the pathophysiology of Graves' disease?
- Thyroid-stimulating immunoglobulins stimulate the thyroid gland to produce excess T4, causing systemic effects.
- Thyroid-stimulating immunoglobulins stimulate the pituitary to produce excess T4, causing systemic effects.
- Thyroid-stimulating immunoglobulins inhibit TSH production, allowing for excess T4, causing systemic effects.
- Thyroid-stimulating immunoglobulins increase TSH production, causing excess T4 and systemic effects.
- Thyroid-stimulating immunoglobulins directly stimulate thyroid hormone receptors in parenchymal tissue, causing systemic effects.
What radioactive iodine uptake scan finding best correlate with Graves' disease?
- Increased uptake, diffuse activity
- Decreased uptake, diffuse activity
- Increased uptake, localized activity
- Decreased uptake, localized activity
- Increased uptake, no clear activity
Which treatment for Graves' disease is not recommended in first trimester of pregnancy?
- Methimazole
- Metoprolol
- Propylthiouracil (PTU)
- Surgical thyroid resection
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Simply amazing.. everything explained clearly based on clinical scenarios. Thank you