Playlist
Show Playlist
Hide Playlist
Goiter and Thyroid Nodules
-
Slides GoiterThyroidNodules EndocrinePathology.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
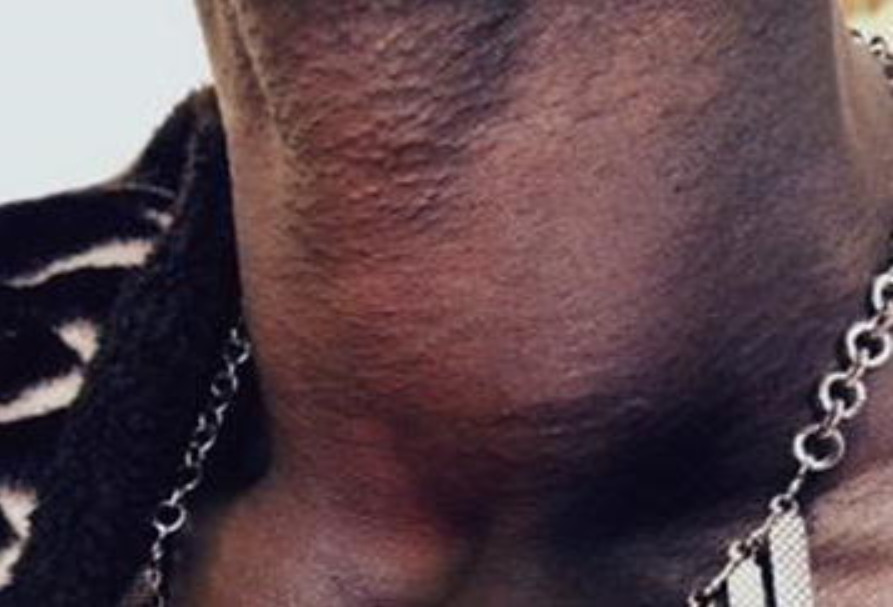
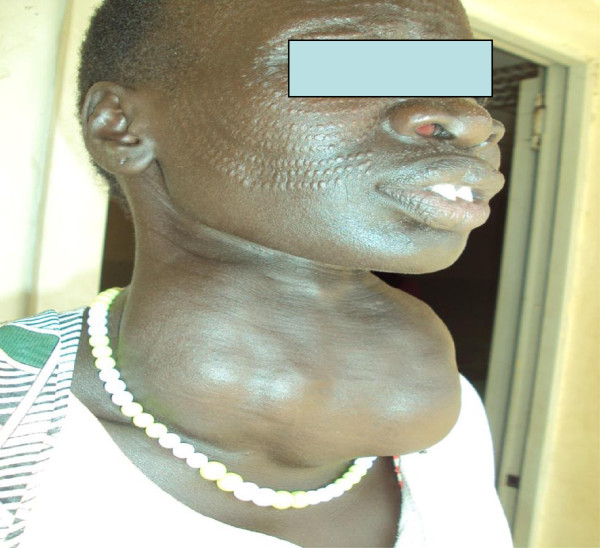
00:01 Here, we’ll take a look at the differences of goiter versus nodules. 00:04 By the time we’re done with this section, you should be able to clearly define the differences between the two so that you never get confused on the wards or on your boards. 00:15 Let’s take a look at goiter, defined as a large thyroid, period. 00:21 Here, in the neck of this patient, a pretty large thyroid gland. 00:28 Multiple etiologies of goiter including hypo or hyperthyroidism; could be physiologic, lack of hormone production. 00:37 What happens if your thyroid hormone is not coming out? The feedback mechanism increases TSH from the anterior pituitary, bombards your thyroid gland and may result in a goiter. 00:49 If you don’t have iodine, once again, increased TSH bombarding the thyroid gland resulting in enlargement. 00:56 Foods… important; goitrogens, drugs that suppress synthesis of thyroid hormones, enzyme deficiencies of hormone synthesis… number of causes of goiter. 01:12 Does not describe the functional status of the thyroid, that’s important for you to understand whereas the nodules will. 01:17 So, just because you find a thyroid… a goiter, an enlargement of the thyroid gland doesn’t necessarily mean that you have a hyper or hypofunctioning thyroid, you just know that there is a pathology. 01:29 If it’s non-toxic, we call that euthyroid; if it’s a toxic type of goiter, it’s hyperthyroid. 01:37 Stop here for one second. 01:38 Last time we talked about toxic was either solitary or multi… multitoxic type of goiter, multinodular toxic and those were the elderly patients that are presenting with hyperthyroidism… elderly, nodular. 01:54 Okay, so, when we talk about nodules, this is interesting. 01:58 With nodules, it means that the… well, this area within the thyroid gland is either taking up iodine or it’s not. 02:05 If it’s taking it up and it’s focal, you call this a hot nodule, focal… focal not diffused, huh? Whereas if it’s cold, it’s not taking up the iodine; it then appears as being black. 02:17 Hot is almost always benign, that’s what you stick with. 02:19 Cold, however, is extremely concerning and you’re worried about malignancy, but, but usually, clinically, it is benign, but of the two, it’s the cold that you should be investigating further. 02:32 I’ll show you an algorithm coming up in which we will then follow… you will follow these with me so that you can then clearly narrow as to what steps are necessary so that you can confirm your diagnosis. 02:43 Only a biopsy can tell definitively whether your nodule is malignant or benign. 02:49 What you’re seeing here in the neck of this individual is a normal thyroid gland in which it is the taking up normal amounts of iodine; nothing here that is truly pathologic. 03:02 Continue our discussion. 03:04 Now, goiter, chronic enlargement of thyroid. 03:06 Remember, it does not, does not define functioning and nodule a discrete lump and whether or not it’s taking up iodine or not will then determine if it’s hot or cold. 03:17 If it’s cold then definitive. 03:19 Definitive biopsy will tell you if your nodule is either malignant or benign. 03:24 If frequency of small thyroid nodule detected by ultrasound is greater than 50 percent; 5 to 10 percent of your nodules may then even contain thyroid cancer. 03:34 Most patients are asymptomatic unless the nodule gets so big and the goiter, there is so much enlargement in the thyroid gland that you then cause compression effects on the surrounding structures including the trachea… dyspnoea; upon the esophagus dysphagia. 03:50 Substernal goiter can be nonpalpable… substernal, but causes airway obstruction to thoracic inlet obstruction… that is a very important point. 04:03 So, substernal, okay, won’t be palpable for obvious reasons, but is then going to cause thoracic inlet obstruction. 04:13 Here, we’ll take a look at the clinical approach at thyroid nodule. 04:18 If the size of the nodule is less than 1 centimetre, no concerning patients, no concerning risk factors for the patient including head/neck radiation or nodule features such as microcalcification. 04:31 If there aren’t any risk factors for the patient, then your next step of management over to the right versus, yes, there are no risk factors then it would be follow-up in imagery. 04:44 If however there are risk factors, so it is larger than 1 centimetre or the patient has a history of having neck radiation or you find microcalcification, then you check TSH. 04:55 You find this to be low then you move to thyroid scan. 04:58 Upon thyroid scan, you check to see as to how much iodine uptake is going to be handled by that nodule and focally, if you find there to be uptake, it’s hot. 05:06 Your next step of management, you follow-up because most likely it will be benign. 05:11 If it’s cold, iodine is not being taken up, C as in cold, C this is concerning. 05:17 Your next step of management is biopsy with the fine needle aspiration and maybe perhaps you find cancer or malignancy… definitive diagnosis. 05:29 A clear picture is very simplistic view, but yet very effective for you to approach your thyroid nodule clinically. 05:40 These arrows that you’re seeing here on the thyroid scan is showing you those areas of a thyroid gland that are not taking up iodine. 05:49 Look at it, it is blending in or camouflaging with the rest of the picture here whereas the region of the black that you see is trying to form the outline or silhouette of the thyroid gland, but those areas or arrows in this areas that it’s pointing to is not taking up iodine, it’s a cold nodule. 06:11 What’s your next step of management? Fine needle aspiration, definitive diagnosis… Is it malignant? Is it benign?
About the Lecture
The lecture Goiter and Thyroid Nodules by Carlo Raj, MD is from the course Thyroid Gland Disorders.
Included Quiz Questions
What are goitrogens?
- Foods/drugs that suppress the synthesis of thyroid hormone.
- Antigens to thyroid tissue, causing an enlarged thyroid.
- The autoimmune process that causes goiters.
- Enzymes that break down goiters and return the thyroid to normal size.
- These are cystic micronodules found inside thyroid nodules.
What is NOT true of goiters?
- It always denotes the malfunctioning of the thyroid.
- It can be physiologic.
- It is defined as a large thyroid.
- It can be caused by a lack of iodine.
- It can be caused by goitrogens.
Which statement about a cold thyroid nodule is correct?
- It is a focal area that does not take up iodine on the RAI scan.
- It is always malignant.
- It shows diffuse RAI uptake.
- It is the most common cause of goiter.
- It is always substernal.
What is required to make a definitive diagnosis of a thyroid nodule?
- Fine needle aspiration/biopsy
- Ultrasound
- TSH levels
- MRI
- RAI scan
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |