Playlist
Show Playlist
Hide Playlist
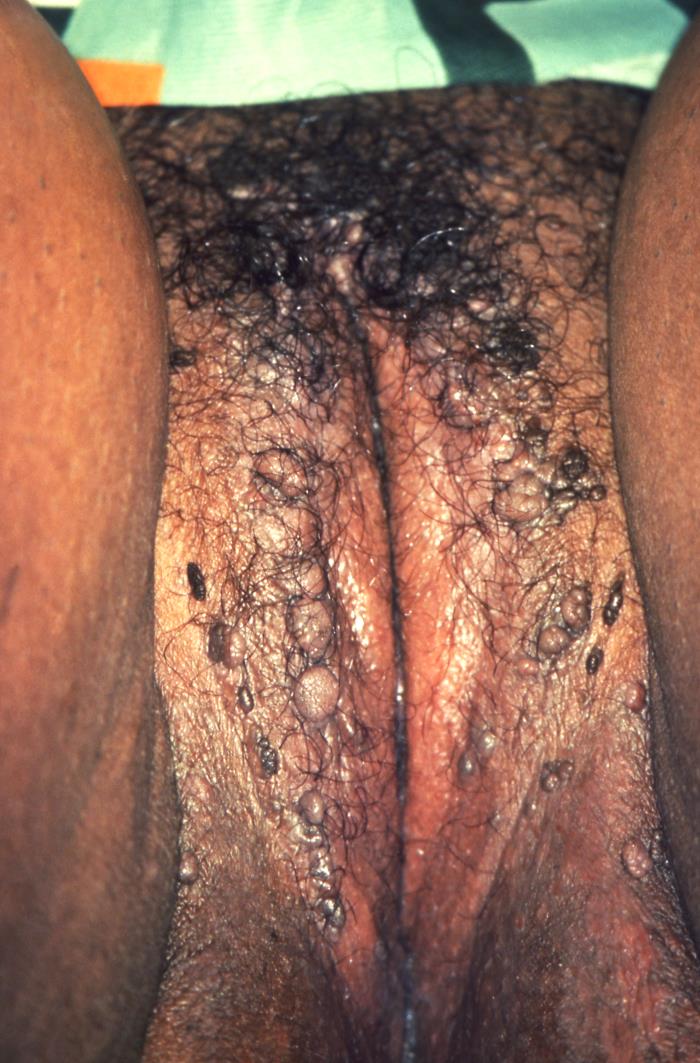
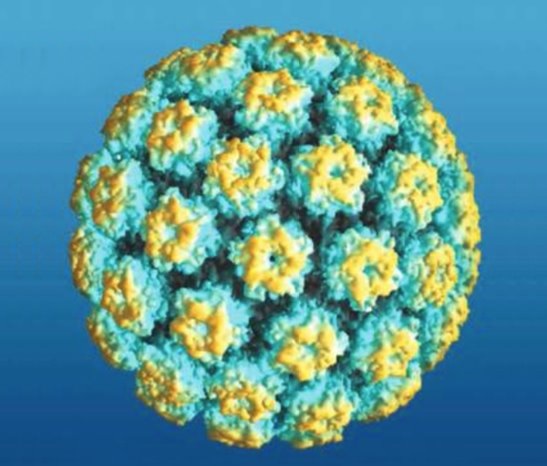
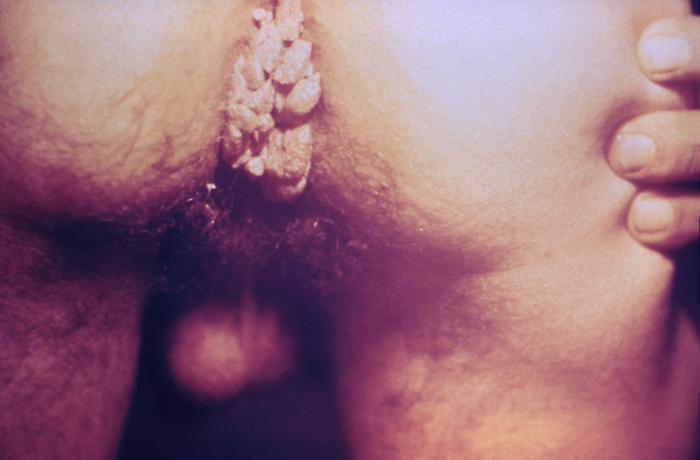
Genital Warts (Condyloma Acuminatum): Diagnosis and Management
-
Slides GenitalWarts InfectiousDiseases.pdf
-
Reference List Infectious Diseases.pdf
-
Download Lecture Overview
00:01 So this is usually a clinical diagnosis and there's rare confusion with other things, such as condylomalata, those elevated lesions of secondary syphilis. 00:19 Scabies, which are little itchy pustules. 00:24 Genital herpes, which is usually quite painful series of ulcers. 00:29 LGV, lymphogranuloma venereum, with its inguinal lymphadenopathy and its groove sign. 00:38 And donovanosis with these festering ulcers that are characteristic. 00:44 And occasionally, molluscum contagiosum, which are papules that look umbilicated. 00:51 They've for their sunk in the center. 00:53 This is classic molluscum contagiosum virus infection. 00:58 The diagnosis of genital warts is usually based around the physical exam. 01:02 Clinicians look for a single or multiple soft, papulated or smooth surface papules or plaques, that are limited to the anogenital region. 01:10 In rare cases the examiner may wish to perform a biopsy if the appearance of the lesion is ambigious. 01:16 It's important to evaluate or be able to exclude other conditions. 01:20 These includes common benign popular cutaneous conditions, such as seborrheic keratosis, skin tags, pearly penile papules, squamous papillomas, Fordyce spots, and other sexually transmitted infections. 01:33 They must also exclude premalignant conditions, and malignant disorders, such as those cause by other HPV genotypes. 01:40 These include things like Bowenoid papulosis, and condyloma acuminatum. 01:44 It's also important to note that viral cultures are not used in clinical practice. 01:49 The treatment is not good. 01:53 Highly effective and safe treatments are not yet available for this. 01:57 So we don't have good current therapy, so we need to either decrease or eliminate the clinical manifestations if we possibly can. 02:08 What's tried, especially on small lesions, is podofilox, which is a derivative of podophyllin. 02:16 This is a derivative of fungal organism. We don't know its mode of action. 02:25 It's in the form of a cream or lotion applied directly to the wart once a week. 02:33 So one of the big problems is chemical burns develop in 1/3 to 1/2 of the patients when podofilox is applied. 02:43 And obviously for that reason, we want to stay away from areas greater than 10 square centimeters. 02:49 It's also contraindicated in pregnancy. 02:53 Imiquimod is another agent, which is available as a cream. 02:58 And what this does is it increases the production of interferon alpha and other cytokines, and that's where its antiviral action comes from. 03:09 Polyphenon E is a green tea extract, which is available as an ointment. 03:14 But this, too, is contraindicated in pregnancy. 03:18 Cidofovir is an acyclic pyrimidine. 03:22 It's a chain terminator and causes apoptosis of HPV infected cells. 03:29 When discussing treatment options, we generally separate them into being either patient-applied therapies or clinician-administered therapies. 03:37 For patient-applied therapies, we can consider imiquimod which stimulates the antitumor immune response, than multiple cytokines There's also podophyllotoxin, an antimitotic agent derived from plants. 03:49 And finally, there's sinecatechins, which modulate programmed cell death. 03:54 Resulting in antiviral, antiproliferative, and antiangionenic action. 03:58 On the other side, we have cryotherapy, TCA, surgery, electrocautery, and laser treatment. 04:05 And while these later methods are a bit more aggressive they can result in permanent scarring. 04:10 In refractory cases that fail initial first-line treatments, we do have several other options. 04:15 The first is combination therapy, where one of the patient-applied medications is used during the interval between clinician-applied treatments. 04:23 Another available option is topical or intralesional treatments with antiviral medications like cidofovir and interferons. 04:30 Finally, in some severely refractory cases, systemic treatment may even be considered, these may include low-dose cyclophosphamide, fluorouracil followed by radiation, and in some cases, tumor hyperthermia followed by radiation. 04:45 The mechanisms of the available treatment interventions are relatively varied. 04:48 As mentioned before some of the treatments focused on antiproliferative properties, some work through immunomodulation pathways, and some are focused primarily on direct tissue distraction. 04:58 I would again like to reiterate that while there are some other more aggressive treatments available for refractory cases, these treatments are much less common due to safety concerns and the limited evidence regarding their efficacy. 05:10 Now, let's talk about prevention, sexual activity is generally considered to be the primary risks factor for these disease. 05:16 Vaccination with the 9-valent vaccine prior to the onset of sexual activity has been shown to be very effective in preventing it. 05:23 Anogenital wart are normally cause by HPV type 6 and 11. 05:27 While the other HPV types covered by vaccine are associated with various cancers, Including cervical, vaginal, vulvar, anal and oropharyngeal. 05:36 Other methods of prevention include, limiting the number of lifetime sexual partners, as well as delaying the age of first intercourse. 05:43 We should also pulse, to make two important points here. 05:46 Firstly, condoms only provide partial protection, as they do not completely cover the anogenital region where skin exposure could occur. 05:54 The other important point is due to the HPV vaccine itself has no effect on existing lesions, and should not be use as a form of treatment. 06:03 So, as a summary of what we've discussed about the treatment, there are patient-applied treatments, such as topical imiquimod and podoflilox. 06:12 And there's also clinician-applied treatments, such as podophyllin, bichloroacetic acid, and trichloroacetic acid. 06:20 As far as preventing genital warts, there's really no effective method that we know of, except perhaps to avoid contact with infectious lesions. Condoms do not provide perfect protection. 06:34 And unlike the HPV vaccine, we have to prevent cervical cancer, we don't have a vaccine yet for this particular HPV infection. 06:47 And that brings me to the conclusion of my discussion on genital warts.
About the Lecture
The lecture Genital Warts (Condyloma Acuminatum): Diagnosis and Management by John Fisher, MD is from the course Genital and Sexually Transmitted Infections.
Included Quiz Questions
Which of the following is the most common method of diagnosing genital warts?
- Clinical findings
- Culture
- Serologic
- Biopsy
- Polymerase chain reaction
Which of the following therapies for genital warts is office based?
- Trichloroacetic acid
- Sinecatechins
- Imiquimod
- Podophyllotoxin
- None of the options provided are office based.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
I really aprecciate this video because he explained the treatment and action mechanisim