Playlist
Show Playlist
Hide Playlist
Gastroesophageal Reflux Disease (GERD)
-
Slides GERD General Surgery.pdf
-
Download Lecture Overview
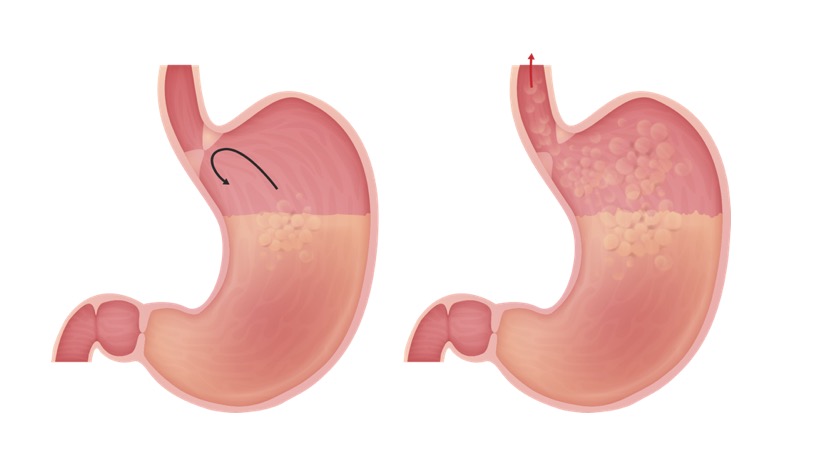
00:00 Welcome back. Thanks for joining me on this discussion of stomach gastroesophageal reflux disease in this section of general surgery. Reflux is incredibly common. In fact, some reflux of the stomach content into the esophagus is physiologic. Therefore, not all reflux is pathologic. Most episodes however are very brief. You probably have had a few episodes of reflux yourself after a hard exam or right before one if one is nervous. Officially though, the diagnosis of gastroesophageal reflux results in symptoms or complications such as esophagitis, chest pain, or disturbances in quality of life. 00:47 So, what does that mean? Patients go beyond the intermittent brief episodes of self-contained reflux. 00:54 These patients have significant symptoms that last for a long time. What are some common history and physical findings? Heartburn, regurgitation, these are common. In fact, some patients complaining of chest pain/cough and when they come to the emergency department complaining of chest pain, one gets very worried that it’s in fact, the patient having a myocardial infarction or heart attack. It’s important to keep that in differential but common things being common, these patients sometimes present with atypical chest pain. Patients can also describe dysphagia or difficulty swallowing after prolonged esophagitis or inflammation of the esophagus as well as water brash. Water brash leads to hypersalivation due to particularly the recumbent reflux of gastric content into the proximal esophagus. Additionally, many patients feel some nausea and vomiting with chronic reflux disease. Laboratories generally are not very helpful. 01:57 Your chemistries and your CBCs can be completely normal. So, how do we diagnose? A clinical diagnosis can be made in the presence of classic symptoms. No further workup is necessary in the absence of alarm features (such as dysphagia, long-standing symptoms, weight loss, or anemia) and with a normal physical examination. 02:22 Additional workup is warranted if alarm features are present or there is recurrence or incomplete resolution of symptoms despite standard GERD therapy. This may include an upper endoscopy. In this picture of an endoscopy, you show signs of esophagitis. 02:43 Some patients undergo 24-hour pH monitoring. The gastroesophageal reflux disease is diagnosed when there’s persistent disease despite initial treatment and the pH monitoring records a percentage of time where the pH drops below 4 in the esophagus. Recall that intermittent, brief episodes of reflux may be physiologic. Therefore, the overall percentage of time where the pH drops below 4 in the esophagus as evidence or indirect evidence of exposure to gastric content which as you know is very acidic.
About the Lecture
The lecture Gastroesophageal Reflux Disease (GERD) by Kevin Pei, MD is from the course General Surgery.
Included Quiz Questions
A 47-year-old lawyer with a past history of smoking cigarettes presents to the outpatient clinic with complaints of several months of chest pain, especially when she lays down to go to bed. She denies any radiation of the chest pain but has occasionally felt chest tightness when rushing to catch a taxi-cab when she is late to work. She also complains of a dry cough in the mornings, but no shortness of breath, and she denies any fevers. She occasionally feels nauseous in the morning and has had a few episodes of acidic emesis after her morning coffee, which she takes on an empty stomach because she doesn’t feel like she has time for breakfast in the mornings. She is working on a very important case at work that is causing her anxiety. Although her presentation appears quite typical of gastroesophageal reflux disease, which of her symptoms should raise a red flag for a possibly more serious health concern?
- Chest pain with activity may indicate cardiovascular compromise.
- Cough in the morning is consistent with infectious pulmonary disease.
- Emesis suggests cholecystitis and she needs surgical evaluation.
- Her nausea and vomiting are more consistent with acute pancreatitis than reflux disease.
- Her dry cough is concerning for chronic obstructive pulmonary disease.
What is the best way of visually identifying esophagitis in gastroesophageal reflux disease?
- Esophagogastroduodenoscopy (upper endoscopy)
- 24-hour esophageal pH monitoring
- Chest x-ray
- Barium swallow
- Capsule endoscopy
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |