Playlist
Show Playlist
Hide Playlist
Functions and Segments – Urinary System
-
Slides 01 GeneralFunctions UrinarySystem.pdf
-
Download Lecture Overview
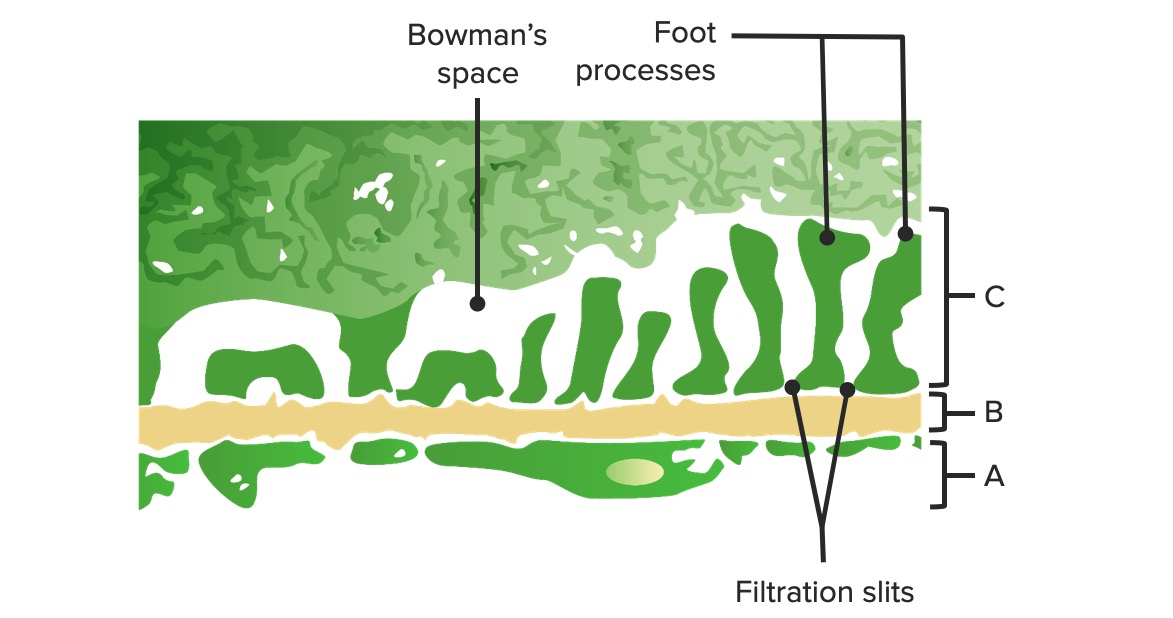
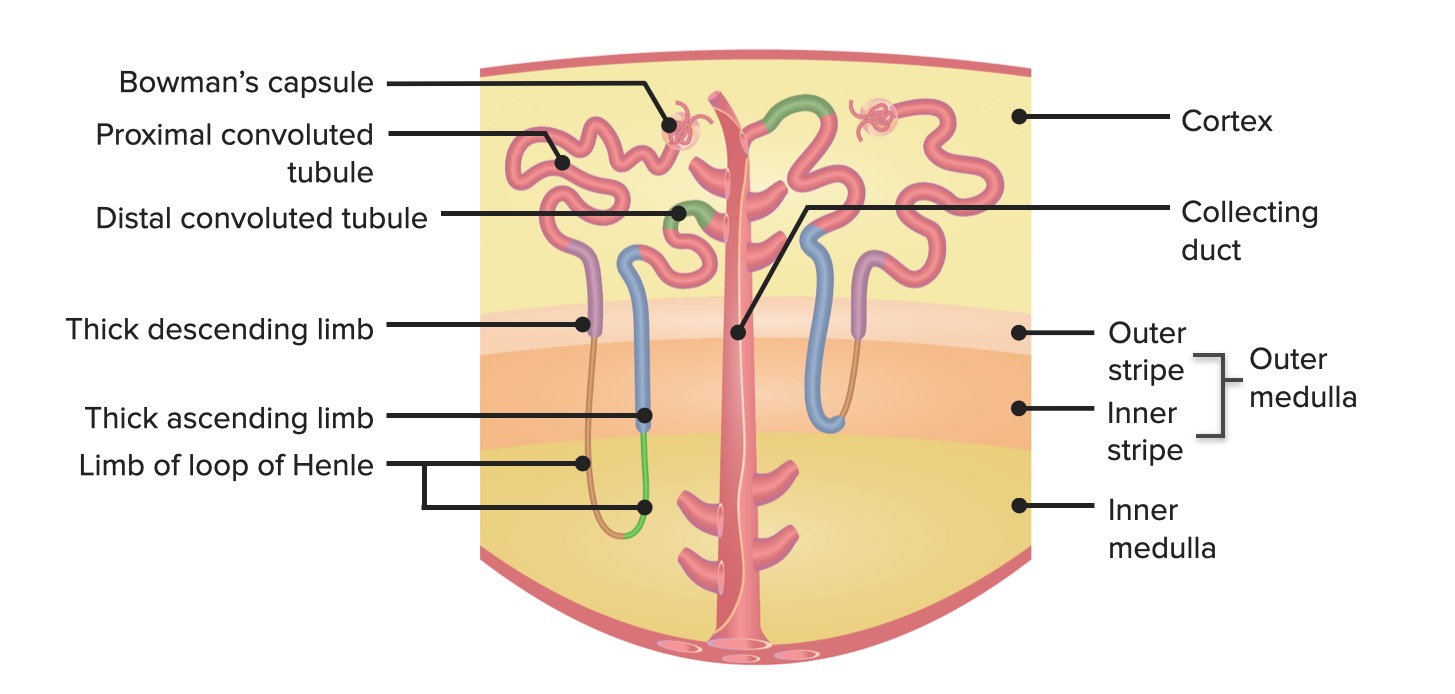
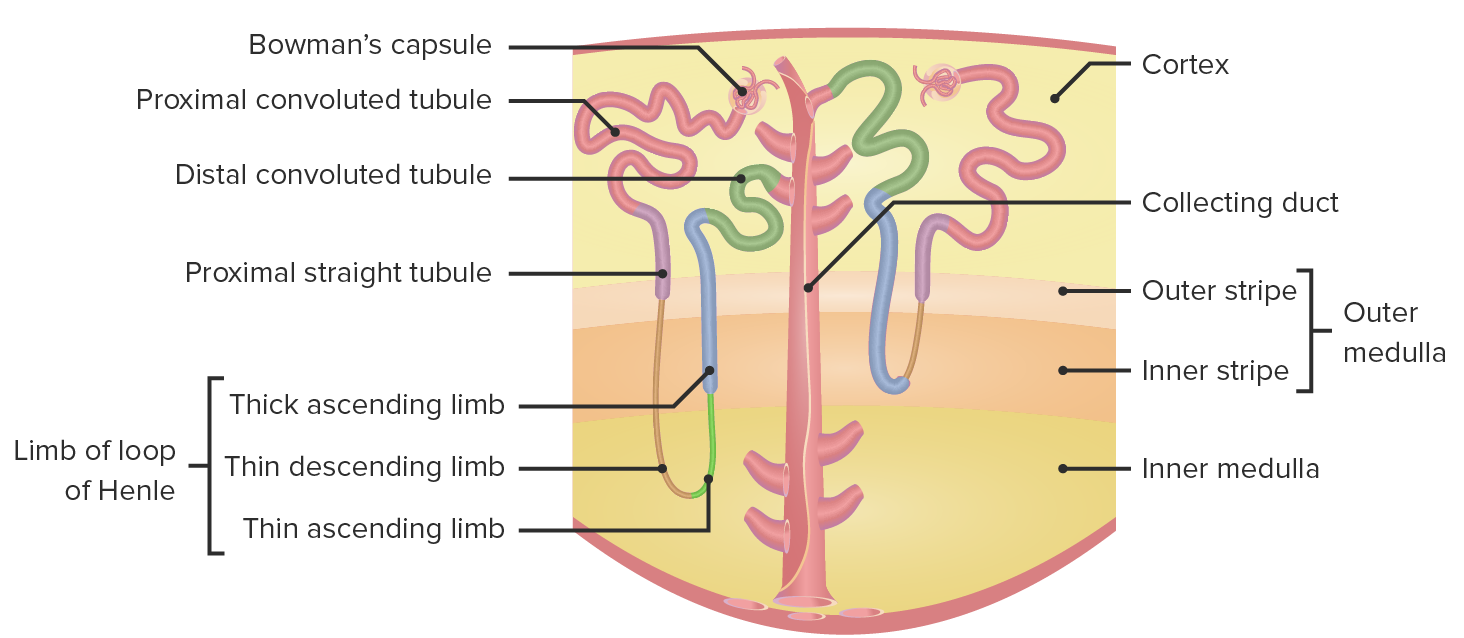
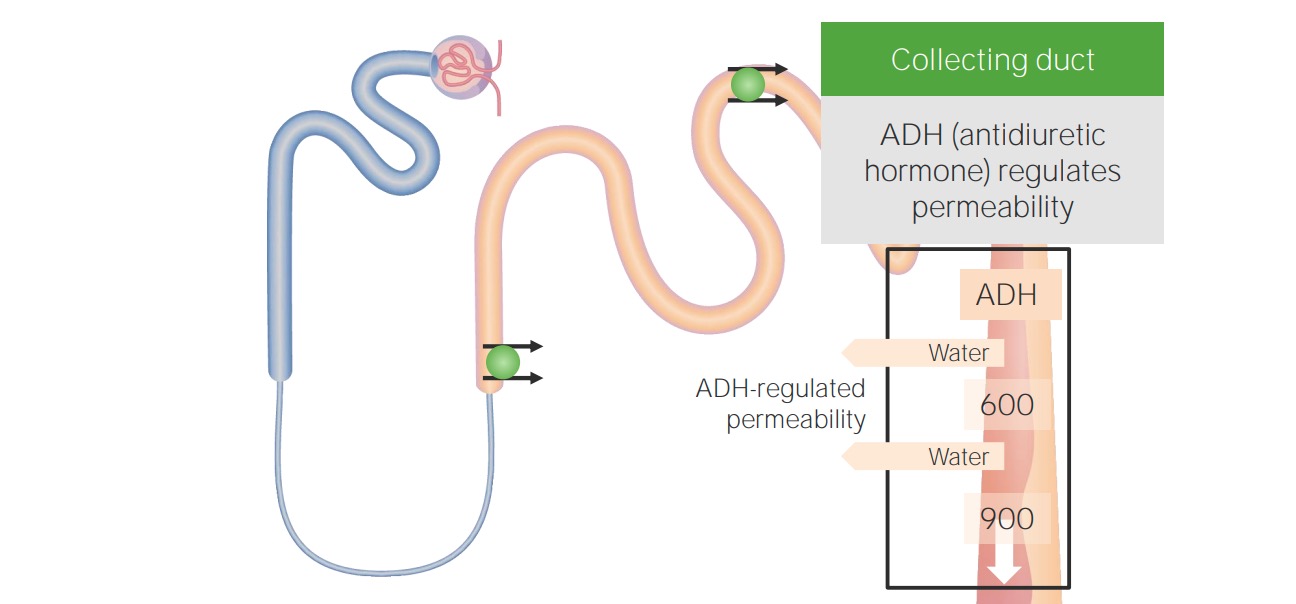
00:02 We're going to talk about the renal system. 00:04 We're going to go through a lot of primary functions. These are the overall biggest things of the kidney. 00:10 That is filtration, reabsorption, secretion, and finally excretion. 00:16 To look at these in more of a diagramatic form, let's look at what the blood is doing, or what are the kidneys doing to the blood. 00:23 Its most important function will be to filter the blood. 00:28 So this is as the blood travels through various glomerular capillaries, some of that plasma is going to exit from the particular blood vessel into what's called the glomerular capsule. 00:41 That process is called filtration. 00:44 The next particular item is reabsorption. 00:47 So once you have that filtered solution in the renal tubule, to reabsorb is to bring it back into the blood. 00:58 Finally, the third particular process or general function of the kidney is to secrete certain waste products. 01:06 Now these waste products either weren't filtered, or even after filtration has occured, you want to move even more of them back into the renal tubule. 01:16 That process is called secretion, where you remove waste products. 01:22 And finally is excretion. 01:24 Excretion is removing the particular substrates from the tubule and eventually into the urine, and then you exit it out of the body. 01:34 So our four primary topics: filtration, reabsorption, secretion, and excretion. 01:40 Now, where does these occur in the various portions of the kidney? The kidney can be broken up into three kind of primary aspects. 01:49 One is what part of the kidney we're talking about. 01:52 Is it in the cortex? Is it in the outer medulla? Is it in the inner medulla? The second is there's two different types of nephrons. 02:01 One is a juxtamedullary nephron and the other is a cortical, sometimes referred to as superficial nephron. 02:09 And finally, each of these nephrons, whether it be cortical or juxtamedullary, have a lot of different segments. 02:17 And we're going to go through these segments in good detail right now to kind of bring you into thinking about how the anatomy and physiology fits together. 02:26 And then in our subsequent topics, we're going to go through each one of those sections and see how they transport a particular solute. 02:36 A solute is the thing that is suspended in the fluid. 02:41 It could be something like sodium. It could be potassium. 02:44 It's the particular ion or substance in the fluid. 02:50 So if we look at the anatomical and also the osmotic components of the kidney, the anatomical are things that where the cortex is located, where the inner medula, the outer medulla is located, and why that becomes important for the nephron is there are a number of osmotic gradient associated from the lowest -- about 300 milliosmoles in the cortex to a maximal on the inner medulla of about 1200 milliosmoles. 03:21 So we have quite a bit of fluctuation betwen how much we can concentrate the urine, and it's going to be in between 300-1200 in normal conditions. 03:32 You can dilute the urine a little bit more by going below 300, but that only happens in specialized circumstances. 03:39 So we have our two different types of nephrons. We have the juxtamedullary nephron and the superficial or cortical nephron. 03:47 Now what are the differences between these two? Hopefully, you can appreciate from this particular diagram that one of the biggest differences are the size of the nephron loops. 03:57 So let's start with the juxtamedullary nephron. 04:00 That is where you can see that nephron loop drop through the outer medulla and all the way into inner medulla, have a hairpin turn, and then come back up again. 04:10 Now, you can contrast this now to the superficial or the cortical nephron, which only goes into the outer medulla and never reaches the inner medulla. 04:20 So what is the advantage and disadvantage of that? Well, hopefully you remember from the osmotic components of the depth of the medulla matters in terms of the osmotic gradient. 04:32 So a juxtamedullary nephron can reach a higher osmolality than a cortical nephron. 04:40 And these higher osmalility-reaching nephrons will allow us to better concentrate urine so that we can say things like body of water. 04:52 Now, the nephron is pretty complex. 04:55 So we're going to break it down into a number of small segments because if we can learn each of these small segments, we're going to be able to put it together and really understand what the nephron and the kidney does for us in terms of homeostatic regulation. 05:11 So the first part is the glomerular capsule. 05:15 In the glomerular capsule is where -- what happens? -- filtration. 05:19 And that occurs as blood travels through the afferent arteriole into the glomerular capillaries, and then out the efferent arteriole. 05:30 From this portion, a small amount of the plasma is filtered out. 05:35 That is then going to travel into the proximal convoluted tubule. 05:41 Now the proximal convoluted tubule is where a lot of the action happens of reabsorption. 05:48 In fact, it has specialized apical membranes that increase the amount of surface area to be able to transport more substances from the apical membrane across and eventually into the blood. 06:04 Now the proximal convoluted tubule, notice, is very high in terms of is it in the cortex -- yes. 06:12 It's not in the medulla yet, and therefore it's going to have a low osmolality - about 300 milliosmoles. 06:18 So when the process of transport happens, it's going to be iso-osmotic. 06:25 We moved down a little bit more into the nephron into the proximal straight tubule. 06:30 This also is heavily involved in reabsorption. 06:34 You can notice though there's a little bit of anatomical difference between these two. 06:39 There's less surface area, or less invaginations on the apical membrane, which is the membrane on the top part of your little diagram. 06:51 Then we go into the thin descending limb. 06:54 Now the thin descending limb will vary in terms of its length, depending upon if you're juxtamedullary nephron or a cortical nephron. 07:03 Its primary purpose though is to allow water to move out. 07:11 You go through a hairpin turn, and then you enter the thin ascending limb. 07:17 So you notice that thin descending, the hairpin turn, and the thin ascending, all are called thin. 07:26 Why? Because they're shorter or less thick. 07:30 What they're going to be involved with is utilizing the medulla's osmolality to do most of the work. 07:36 Things that are thicker, such as the thick ascending limb, is going to have to work on transporting things. 07:45 In this case, you're going to use a little bit of energy to help you transport from the apical membrane, through the tubule cell, to the basal lateral membrane, and then into the blood. 07:59 The distal convoluted tubule is located a bit higher. 08:03 And remember from the medullary region all the way up to the cortical region, the importance about this height has to do with the amount of osmolality. 08:14 So in the distal convoluted tubule, we're about at 300 milliosmoles, just like you were in the proximal convoluted tubule. 08:21 But that is much, much, much less osmolality than what was located in the inner medulla, which is where that hairpin turn was for juxtamedullary nephrons. 08:35 Finally, we plunged back into the areas of high osmolality by going through the collecting duct. 08:42 So in the collecting duct, we utilize some of the inherent osmolality that's in that area by if we insert a certain channel in the collecting duct, we can allow water to be transported across. 08:57 So the collecting duct doesn't do a lot of transport except for water, and that only occurs when certain hormones are present. 09:07 This is our nephron segment. So there's a lot to remember. 09:11 We started it off with the proximal convoluted tubule, proximal straight thin descending, thin ascending, thick ascending, the distal convoluted tubule, and then finally, the collecting duct. 09:25 All of these are going to be very important for aspects of transport that we're going get into in a subsequent time.
About the Lecture
The lecture Functions and Segments – Urinary System by Thad Wilson, PhD is from the course Urinary Tract Physiology. It contains the following chapters:
- Primary Renal Functions
- Nephron Segments
Included Quiz Questions
What is the term used to describe a substance moving from a peritubular capillary into the renal tubule?
- Secretion
- Filtration
- Reabsorption
- Excretion
Which of the following structures traverses the greatest depth from the renal cortex to the medulla?
- Collecting duct
- Proximal convoluted tubule
- Proximal straight tubule
- Thick ascending limb
Which of the following components of a nephron perform the function of filtration?
- Bowman's capsule
- Thin ascending limb
- Thin descending limb
- Proximal convoluted tubule
- Medulla
Which of the following is FALSE?
- Urine osmolality can never be below 300 mmol/L.
- More energy is required for reabsorption in the distal convoluted tubule than in the thin descending limb.
- Water reabsorption occurs in the descending limb of the loop of Henle.
- Reabsorption in the proximal convoluted tubule is best described as isoosmotic.
- Sodium reabsorption occurs in the ascending limb of the loop of Henle.
Customer reviews
4,7 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
1 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Great way of teaching, I am Impressed by this and learnt it
I think if you're looking for a very detailed explanation of the system, I think this video is perfect and it goes at a very good pace too. I only needed an specific amount of information, so I ended up watching a video that was too specific for me to use.
1 customer review without text
1 user review without text