Playlist
Show Playlist
Hide Playlist
Frostbite: Symptoms
-
Emergency Medicine Cold Illness.pdf
-
Download Lecture Overview
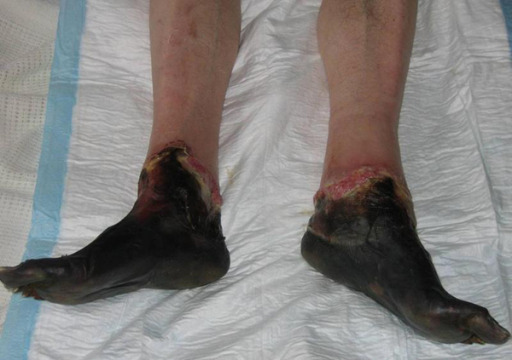
00:01 So now we’re gonna switch gears a little bit and talk about another cold related problem. 00:05 So in this case, we have a 46-year-old gentleman who comes into the Emergency Department with bilateral foot pain. 00:11 He’s homeless and he spends most of his time walking around on the street wearing sneakers which is the only pair of shoes that he owns. 00:17 It’s February and there’s snow and slush on the ground, so his shoes are getting wet. 00:23 He’s been in our waiting room for about 7 hours and by the time we see him in the care area, you can see that his feet look like what you see here in this picture. 00:33 So he’s got some swelling and he’s got some blue discoloration of all of his toes. 00:39 What’s the diagnosis for this gentleman? Unfortunately, this man has frostbite. 00:46 So risk factors for frostbite include obviously, low temperatures. 00:52 You don’t get frostbite when it’s warm out. 00:54 Also, high velocity wind, exposure to water or snow, and that’s very, very important. 01:00 Remember, we mentioned that you lose much more heat through conduction when you’re wet. 01:06 So anytime you have digits that are exposed to water or snow, the risk of frostbite increases significantly. 01:13 Wearing clothing that’s wet, constrictive, or inadequately insulating increases your risk and of course, anything that impairs your judgement. 01:21 So alcohol, drugs, fear or panic in a wilderness setting can raise your risk of developing frostbite. 01:29 So you can get frostbite anywhere on the body but we see it most often in peripheral areas that have relatively poor vascularization. 01:40 So fingertips, toes, the tip of the nose, the tips of the ears, and the penis. 01:46 I do wanna mention also that occupational exposures can lead to frostbite. 01:51 So for people who work with supercooled substances like in the air-conditioning industry for example, they can have frostbite as a result of exposures to those substances. 02:02 So the way frostbite works is basically, when your tissue actually cools below the freezing point and ice crystals form in the tissue, that’s what leads to frostbite. 02:14 So there’s four different phases of frostbite. 02:18 So there’s the period before the tissue actually freezes when it’s gotten very, very cold but has not yet formed ice crystals. 02:26 So the tissue cools, it vasoconstricts which causes ischemia, and then, there’s inflammation related to the ischemia that leads to endothelial leakage and tissue damage from inflammatory mediators. 02:39 Then, there’s the freeze-thaw stage. 02:42 So at that point, ice crystals begin to form in the tissues. 02:45 The cells become dehydrated because the water that belongs inside of them is now inside of ice crystals and cells die as a result of that. 02:56 After the freeze-thaw stage, you develop vascular stasis. 03:00 So basically in the region of the body that’s frozen, you start to get microvascular thrombus formation which occludes the vasculature and further exacerbates ischemia. 03:11 After that, there’s the late phase which is called late progressive ischemia, and basically, as a result of all of the other things that we’ve talked about, you see hypoperfusion of the tissue in the region, a lot of inflammatory change, and tissue necrosis. 03:26 Clinically speaking, frostbite can be divided into three phases. 03:30 So early on in the course of frostbite, the patient will complain that the affected area feels cold, it’s painful, they’ll often complain of paresthesias. 03:39 When you examine them, they might have relatively few findings on their physical exam. 03:47 So just like the picture we saw of our patient’s slightly discovered blue toes, that might be all you see. 03:53 Sometimes it’ll be a waxy or still texture to the tissue as well, but it can actually look more benign than it is early on. 04:02 The middle phase of frostbite is gonna involve basically complete sensory loss. 04:07 The patient is gonna be numb and insensate in the affected area and that’s because the nerve endings are actually frozen and killed. 04:14 They’re of course gonna lose dexterity as well because they’re not gonna have normal neurologic function in the affected extremities. 04:22 In the middle phase when you examine them, you’re gonna start to see blister or bullae formation, and they’re gonna start to desquamate or slough their skin. 04:31 Finally, in the late phase, this is where the patient really begins to experience pain. 04:38 So they’ll have throbbing pain and it can persist for weeks or months well after the tissue damage has actually stopped evolving. 04:48 This is the phase in which we’ll start to see tissue loss. 04:51 We’ll see demarcation of the area that is no longer viable and development of dry gangrene. 04:58 And here’s some pictures that illustrate the progression of frostbite. 05:02 So early on, you see that blueish discoloration that you can see in this patient on the toe and on the heel. 05:08 As you move into the middle phase, you can see formation of bullae and blisters over the affected area and this patient as these bullae rupture will begin to desquamate. 05:20 And then, in the final picture, you see demarcation and dry gangrene of all of the affected digits.
About the Lecture
The lecture Frostbite: Symptoms by Julianna Jung, MD, FACEP is from the course Toxicologic and Environmental Emergencies. It contains the following chapters:
- Frostbite
- Symptoms of Frostbite
Included Quiz Questions
Which of the following statements regarding the risk factors of frostbite is NOT true?
- Ethanol ingestion is protective against frostbite.
- Wearing inadequately insulating clothes is a risk factor in the development of frostbite.
- Exposure to super-cooled substances may lead to frostbite.
- More body heat is lost due to conduction when exposed to cold water.
- Frostbite is seen most commonly in poorly vascularized body parts.
Ice crystals start to form in which phase of frostbite formation?
- Freeze-thaw
- Pre-freeze
- Vascular stasis
- Late progressive ischemia
- Tissue necrosis
Which of the following statements regarding the clinical presentation of frostbite is NOT true?
- Late phase signs are limited to numbness and loss of sensation.
- Bullae develops in the middle phase of frostbite formation.
- There are few signs of frostbite formation in the early phase.
- Loss of tissue/necrosis is only observed in the late phase.
- The symptoms of the early phase of frostbite formation are cold sensation and pain.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |