Playlist
Show Playlist
Hide Playlist
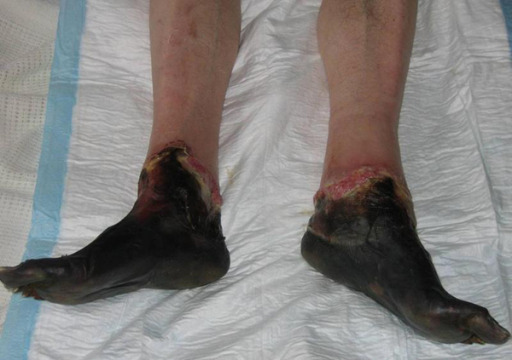
Frostbite: Management
-
Emergency Medicine Cold Illness.pdf
-
Download Lecture Overview
00:01 So how do you manage frost bite? As you can imagine, it’s a disease of tissue freezing. 00:07 So our goal is gonna be tissue thawing. 00:11 Now, we don’t wanna thaw the frozen tissue if there’s a risk of re-freezing. 00:14 So if you’re working in a wilderness setting, you’re the expedition doctor in Antarctica or something like that, and you have a patient with frostbite, do not thaw them until you get them back to a reliable indoor warm environment. 00:29 If you thaw them out in the field, you can actually cause more harm and more tissue damage associated with refreezing. 00:37 However, assuming you’re practicing in an Emergency Department setting where you can control the climate, you wanna of course stabilize their hypothermia and address their ABC’s before you begin thawing. 00:47 Life clearly comes before limb, but once you’ve decided your patient is stable, you wanna thaw them in circulating water that’s just a little above body temperature. 00:57 So 37 to 39 degrees. 00:59 Water that’s warmer than that doesn’t actually thaw any more quickly but patients do have a lot more pain. 01:04 So we really wanna limit ourselves to minimally warm water. 01:08 Rewarming no matter what is gonna be painful even when you do it correctly. 01:14 So you need to make sure you’re giving your patient’s parenteral analgesia. 01:18 Typically, they’re gonna need opioids to tolerate this because they’re taking nerve endings that were numb and non-functional and sort of bringing them back to life, and there’s gonna be a lot of pain associated with that. 01:31 After you have the patient thawed, you wanna elevate the affected extremity to minimize swelling. 01:39 You wanna cover the affected area with loose, dry, sterile dressings and that’s basically just to keep digits from sticking to one another and to protect them from further trauma. 01:49 Topical aloe vera has actually been shown to decrease inflammation and pain. 01:54 So that’s something that you definitely should consider using. 01:57 And you wanna give aspirin or NSAIDs even if patients don’t get analgesic benefit from those, the anti-inflammatory benefit is actually significant. 02:07 So every patient who doesn’t have a contraindication should receive either aspirin or NSAIDs as part of their treatment for frostbite. 02:15 You wanna aspirate any blisters basically to get the inflammatory mediators out and to allow the skin to heal. 02:23 Aspiration of non hemorrhagic blisters is controversial. 02:28 Some clinicians advocate, leaving them in place to support a sterile environment for wound epithelialization. 02:34 You wanna make sure that you provide tetanus prophylaxis and in really severe cases, you can consider use of thrombolysis because there are situations where patients will have larger vessel thrombi that can lead to significant tissue loss. 02:51 So if you think you have some viable tissue that you can salvage, you can consider thrombolysis in cases if you expect you’re gonna have a lot of tissue loss although,that is rarely done. 03:01 One really important thing to remember is that no surgical treatment should be performed until you actually see demarcation. 03:10 So a lot of times, frostbite can look really, really bad but actually heal better than you expect or the patient can have progressive ischemia and lose more tissue than you think they’re gonna at the beginning. 03:23 So you really wanna just give it time and see how the frostbite develops before you start making decisions about debridement or amputation. 03:34 Alright, so take home points about cold related illness are one, that hypothermia is a life-threatening emergency and it affects every organ system. 03:44 Two, when you have severe hypothermia, you wanna provide active core rewarming. 03:49 So get that patient warm back up to stabilize them. 03:53 Three, you’re not dead till you’re warm and dead. 03:56 So hypothermic patients who have no signs of life can still be revived and can actually survive neurologically intact. 04:02 So don’t give up prematurely. 04:04 Regarding frostbite, it’s caused by tissue freezing and it leads to significant tissue loss. 04:10 You wanna provide thawing as your primary treatment for frostbite and no surgical treatment until demarcation occurs. 04:17 Thank you very much.
About the Lecture
The lecture Frostbite: Management by Julianna Jung, MD, FACEP is from the course Toxicologic and Environmental Emergencies.
Included Quiz Questions
What is the ideal temperature range of water for thawing patients with frostbite?
- 37–39 degrees Celsius
- 35–36 degrees Celsius
- 39–40 degrees Celsius
- 36–37 degrees Celsius
- 34–35 degrees Celsius
Which of the following procedures must NOT be done after thawing a patient with frostbite?
- Surgical debridement immediately after thawing before demarcation occurs
- Application of loose, dry dressings around affected digits
- Elevation of the affected extremity to prevent swelling
- Topical application of aloe vera to decrease pain and inflammation
- Aspiration of any blisters to allow the skin to heal faster
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |