Playlist
Show Playlist
Hide Playlist
Esophagus
-
Slides Digestive system espohagus and stomach.pdf
-
Reference List Histology.pdf
-
Download Lecture Overview
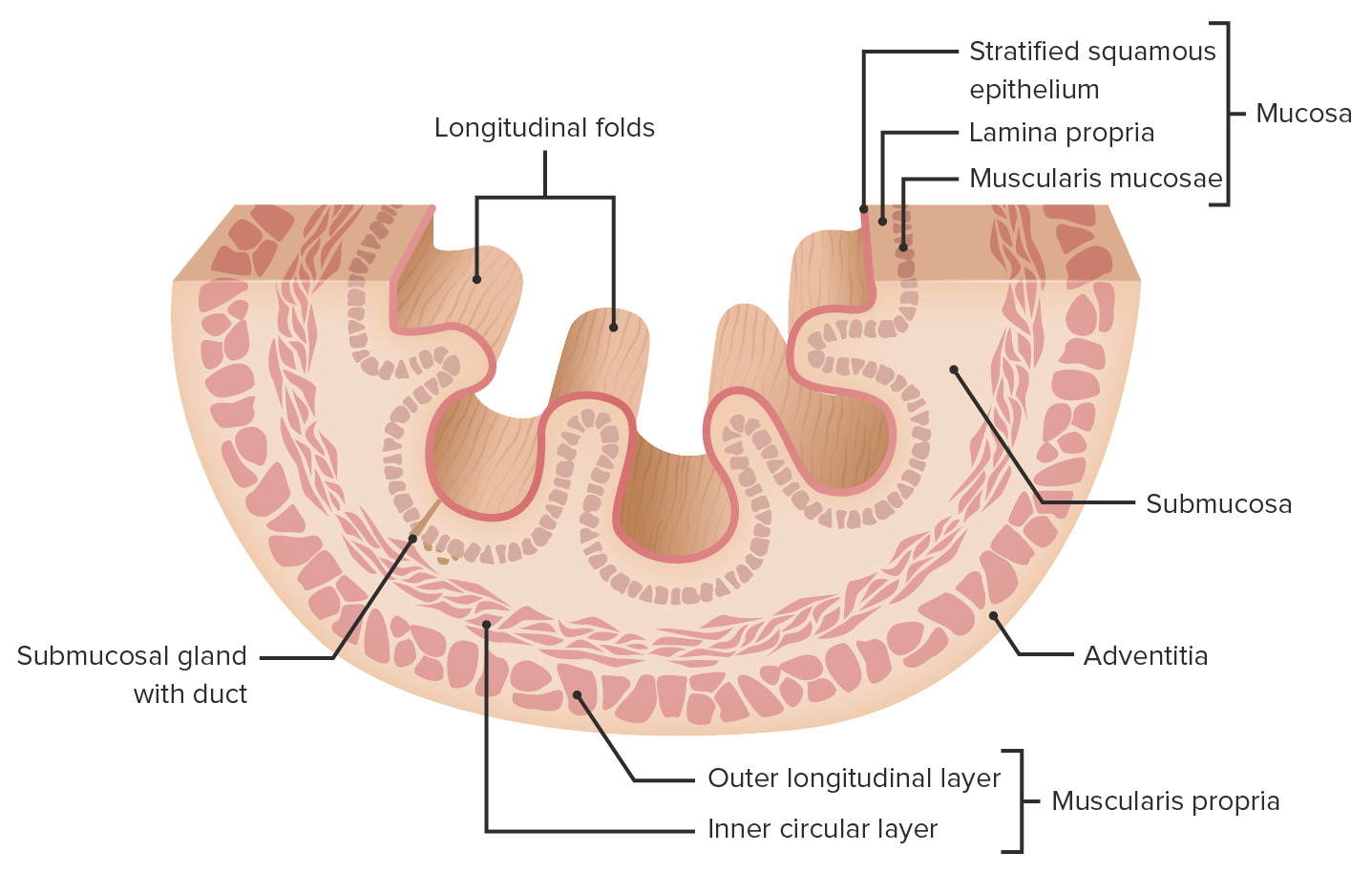
00:00 Here is a section taken through the esophagus, a histological section that's stained with hematoxylin and eosin, and it shows and labels a number of unique features with the esophagus. First of all, look at the top part. The surface has got various papillae and folds, which is what you normally see unless the esophagus is stretched wide apart as it's swallowing food. But those folds allow or expand because of that submucosal layer that I've mentioned earlier. So when you identify the mucosa there, you can see the epithelial surface, which is stratified squamous epithelium, designed to be a wear and tear epithelium, to resist the abrasive forces during swallowing. That epithelium is supported by a fairly strong lamina propria which is very vascular. And then you can just see a very thin slip, perhaps the muscularis mucosa. That's the mucosa, the main part of the gut, as I keep saying, that changes as we go down to the stomach and then further into other parts of the elementary tract. In this section of the esophagus, you can see the submucosa, and it's full of these pale staining structures. They are glands, mucus secreting esophageal glands. They are important because they lubricate the esophagus. They lubricate the surface during swallowing. 01:43 They are also important as we go down and approach the entry into the stomach, because along with special cardiac glands in the stomach, they help to neutralize the lumen, should there be any acid reflux from the stomach. 02:04 Apart from the stomach, and also an area at the very first part of the small intestine, the duodenum, the submucosa doesn't contain glands as much as you see in this image. And then there's the muscularis externa, consisting of two layers, the inner circular, and the outer longitudinal layer. You know the esophagus carries the food from the oral cavity into the stomach. And so, when you examine the muscularis externa, you'll find the top part, the top third of the esophagus, that muscle is actually striated muscle. It's continuous with the striated muscle of the pharynx, and it's controlled by the motor, the somatic motor component of the vagus nerve. So we're conscious of it. We can regurgitate, at some stage, food in that part of the esophagus because we have voluntary control through the somatic division, motor division of the vagus nerve that innervates that muscle. 03:19 In the middle third of the esophagus, there's a mixture. There's some muscle that's striated, and there's some that's smooth muscle. And then finally down towards the lower end, the lower third of the esophagus, the muscle is entirely smooth muscle. And that's controlled by the visceral component of the vagus nerve. We're not conscious of that. 03:44 It's under automatic control, but it's motor. It brings about contraction of that smooth muscle. 03:55 And that contraction can be very, very rapid to deliver that food all the way down the esophagus into the stomach. 04:06 Well, now is your turn to have a look at this section. I'll give you a hint and I'll say it's the esophagus. But have a look at this section and just see if you can now identify the layers of the gut wall using the esophagus as an example. Oops! I just gave away what the section was, but that doesn't matter. Have a look and now see if you can identify the mucosa. 04:37 Did you get it right? Yes. Because I hope you, first of all, look for the lumen and found and know that the mucosa is immediately adjacent. It lines that lumen. What about the submucosa? Can you locate that? Did you get it right? You can't see many glands in this part of the submucosa. 05:06 But as I said before, towards the esophageal rather towards the stomach end, you will. See if you can locate now the muscularis externa. Did you get it right? I hope so. If you look at the muscularis externa here, try and work out the orientation of the muscle fibres, the inner circular, follows a pattern wrapping around the lumen. This is the transverse section through the esophagus. 05:43 And the outer component is the longitudinal layers of the esophagus of the muscularis externa. So well done. You now have a very good understanding, hopefully, of the gut wall. And if you got some notes in front of you, put a big star next to the word mucosa, because that's the layer, as I've mentioned a number of times now because I want to stress it, that is going to change. And we'll see that when we look at the stomach. 06:17 Under very high magnification now, we can see features of the mucosa. In this situation, it's a stratified squamous epithelium. You can see that the epithelial cells at the base are stem cells that give rise to layers above them, which are shed into the lumen of the esophagus because this is a wear and tear lumen, abrasion from the food passing down through it. In other parts of the gut, particularly in the stomach we're going to see in a moment, that epithelium changes. It becomes glandular, and it forms secretory cells that have a very important role as we'll see as we go through. The epithelium is supported by the lamina propria. Lamina propria is that loose connective tissue that supports all epithelia. And then you have some very small components of smooth muscle layer being part of the muscularis mucosa. I should point out that all muscularis mucosa is smooth muscle. It's only the muscularis externa in that upper third and some in the middle third of the muscularis externa that's actually striated muscle, where we have voluntary control to regurgitate or to swallow food.
About the Lecture
The lecture Esophagus by Geoffrey Meyer, PhD is from the course Gastrointestinal Histology.
Included Quiz Questions
Which type of epithelium lines the mucosa of the esophagus?
- Stratified squamous
- Simple squamous
- Simple columnar
- Stratified columnar
- Pseudostratified columnar
Which of the following layers of the esophagus contains mucus-secreting glands?
- Submucosa
- Muscularis interna
- Lamina propria
- Epithelium
- Adventitia
Which of the following is NOT a structural feature of the muscularis externa of the esophagus?
- The lower third consists of a mixture of skeletal and smooth muscles.
- It has inner circular and outer longitudinal layers.
- The upper third is composed of striated muscle.
- It is innervated by the vagus nerve.
- The muscle layers are separated by the myenteric plexus.
What is the thin layer of areolar connective tissue which lies immediately beneath the epithelium of the gut?
- Lamina propria
- Mucosa
- Muscularis mucosa
- Submucosa
- Adventitia
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Dr. Meyer, you are awesome!!! I never thought that I will start to like Histology! The entire chapter is great! My favourite part is your interactive technique bonus, used in Esophagus video! :)
very easily and well explained lecture about the esophagus. thank you for the explination