Playlist
Show Playlist
Hide Playlist
Esophagitis with Case
-
Slides Gastroenterology 05 Esophageal Diseases.pdf
-
Reference List Gastroenterology.pdf
-
Download Lecture Overview
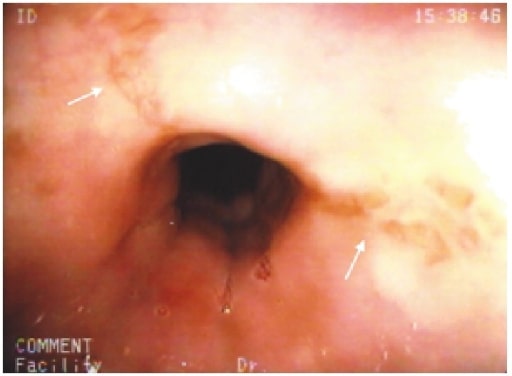
00:00 So now that we've gone through some of those tests, let's talk about our first case. 00:04 We have a 44-year-old man with HIV who presents to urgent care complaining of painful swallowing with both liquids and solids. 00:12 He otherwise feels well. He takes no medications. 00:15 He stopped taking his antiretroviral medications two years ago after he moved to a new city and has not yet established with a new primary care doctor. 00:24 On exam, vitals are normal, oropharynx and abdominal exam is unremarkable. 00:29 And his upper endoscopy findings are shown here. 00:33 So what is the best next step in management? So let's identify some key features in this case. He has odynophagia or pain with swallowing. 00:42 In addition, he's a patient with HIV off his antiretroviral therapy. He has a normal exam otherwise. 00:50 And on endoscopy he has these white raised, kind of thick looking plaques throughout his esophagus. 00:57 So the most likely diagnosis here is esophageal thrush or Candida albicans. 01:05 We'll talk a bit more about that next. 01:08 So there are three main types of esophagitis; the first is an infectious esophagitis, the second is pill-induced esophagitis, and the third is eosinophilic esophagitis. 01:19 We'll talk about each three of these in detail. 01:22 So infectious esophagitis can be caused by many organisms. 01:27 One of the most common causes is Candida albicans. 01:30 It can affect both immunocompromised and immunocompetent patients. 01:34 They tend to have a white raised plaques on their endoscopy. 01:38 And treatment is with an antifungal agent like fluconazole. 01:42 Patients may also have infection with Cytomegalovirus or CMV. In general, this usually affects immunocompromised patients. 01:51 They may have large, superficial ulcerations on endoscopy and they should be treated with ganciclovir or valganciclovir. 01:59 Lastly, they may also have herpes simplex virus or HSV. 02:04 This can affect both immunocompromised and immunocompetent patients but tends to mostly affect immunocompromised. 02:11 They may have small, deep ulcerations on their endoscopy And you treat them with acyclovir. 02:17 Our second type of esophagitis is pill-induced esophagitis. 02:23 This is when pills become stuck in the esophagus and cause local erosions. 02:28 Patients will present with pain with swallowing, difficulty swallowing, and may have chest pain. 02:34 Common medications that cause this are basically any pills that are large and difficult to swallow. 02:41 So some common culprits are; bisphosphonates like alendronate, antibiotics such as doxycycline, potassium supplements, and Iron supplements. 02:52 All of these are known to be large pills that commonly cause esophagitis. 02:57 Over here on the right you can see an upper endoscopy that shows stellate erosions that are consistent with pill-induced esophagitis. 03:05 So in general, what you want to do is prevent this from happening. 03:09 In general, you tell patients to drink plenty of water with their medications and avoid lying down for 30 mins after they take their pills. 03:17 Our third type of esophagitis is eosinophilic esophagitis. 03:22 This is a rare condition but it is commonly tested. 03:25 So it is an esophageal squamous mucosal inflammation that results from eosinophils infiltrating the esophageal tissue. 03:34 Some keywords to note for test-taking purposes are; young man with atopy who presents with dysphagia and frequent food impactions. 03:43 It tends to be associated with food allergies, asthma, eczema, and GERD. 03:50 The diagnosis is made by upper endoscopy. 03:55 And the typical features you may see are these longitudinal furrows along the length of the esophagus, some fragile mucosa, you may see what's called a trachealized esophagus; when you begin to see rings around the esophagus much like the appearance of the trachea, and you may see small white plaques that may look like candidiasis. 04:18 This patient should be treated with an eight-week trial of a proton pump inhibitor or topical glucocorticoids. There are also emerging treatments for eosinophilic esophagitis such as dupilumab, which is an interleukin-4 (IL-4) receptor antagonist that has been approved to treat certain populations with eosinophilic esophagitis. 04:40 So now let's return to our case. 04:42 We had a 44-year-old man with HIV off his medications with a normal exam but his endoscopy shows these white raised thick plaques throughout the esophagus. 04:52 So the first step is to make the diagnosis since he's immunocompromised and he has pain with swallowing, you should think about candidiasis. 05:01 And the next step is to treat with oral fluconazole.
About the Lecture
The lecture Esophagitis with Case by Kelley Chuang, MD is from the course Disorders of the Esophagus and the Stomach.
Included Quiz Questions
Which of the following endoscopic findings is characteristic of cytomegalovirus esophagitis?
- Large, superficial ulcerations
- Small, deep ulcerations
- White raised plaques
- Longitudinal mucosal furrows
- Fixed esophageal rings
Which of the following medications is associated with medication-induced esophagitis?
- Alendronate
- Omeprazole
- Glucocorticoids
- Ranitidine
- Fluconazole
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |