Playlist
Show Playlist
Hide Playlist
Localized Rashes: Dermatitis and Fungal Infections
-
Slides LocalizedRashes AcuteCare.pdf
-
Download Lecture Overview
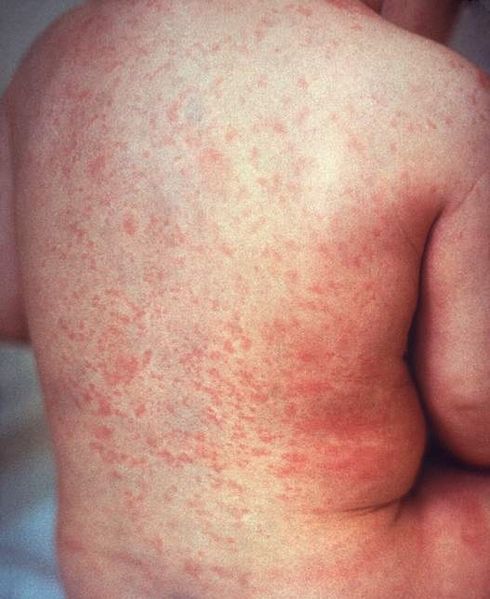
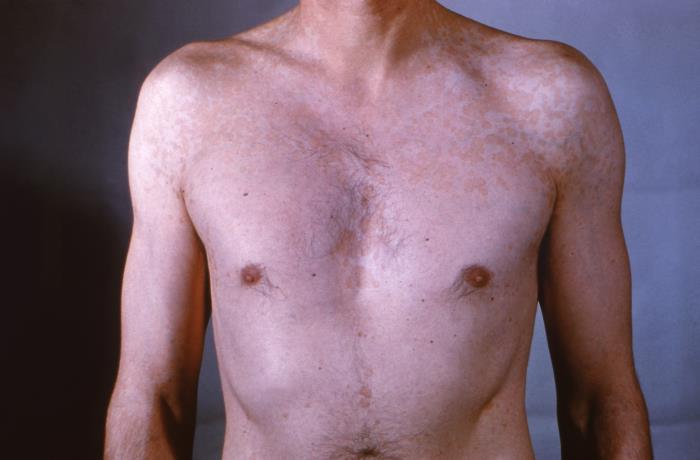
00:01 So, I have a question for you. 00:02 Do you feel itchy? Because you will soon. 00:05 We’re going to cover localized rashes, and so it's very natural every time I see a patient with particularly a more severe rash or something really itchy like scabies, like I come away and I just - I know as I’m some scratching myself. 00:16 So, see if this happens to you after we describe localized rashes. 00:20 In all seriousness, these are important diagnoses that we make in primary care. 00:25 We see patients with skin complaints all the time. 00:28 And it’s important I think to be able to manage, particularly low level and common things, in your practice without necessarily referring to a skin specialist. 00:38 So, we’ll cover dermatitis and that's - and then we’ll be moving on to fungal infections and these are just really great pictures. 00:46 I’ll kind of describe them as we go through. 00:48 This is a really bad case of cellulitis with eschar formation. 00:52 But impetigo and cellulitis, we’ll cover. 00:54 And then, we’ll finish with herpes zoster. 00:56 So, not comprehensive, not every rash, but these are the common ones. 00:59 I thought for a brief time together where we want to focus our attention. 01:03 So, dermatitis. Maculopapular, so make sure you describe your rash well. 01:07 That's always a key. 01:09 So, maculopapular, meaning it’s flat and raised in parts. 01:12 Look hard for exposure to allergens and contacts, and that's why distribution of the rash is really, really important. 01:21 Remember that an allergen may produce this broad rash, as you see here with the wrist. 01:25 Kind of the redness is spread around. 01:27 It’s pretty diffused. 01:29 I’d have a hard time believing that's more of a contact dermatitis. 01:33 But say that the rash was just limited right here to this part around the wrist, and especially there's a circle on the backside, that's not allergic, that’s a contact dermatitis probably due to something like a nickel in my watch, for example, is a common one. 01:48 Or if it has a distribution just around a necklace. 01:52 Or even just in sun exposed areas. 01:54 Looking at the distribution of rash is really, really important. 01:58 But this kind of broader rash might be more of a systemic allergy. 02:02 You can also see it if there is a significant reaction to a particular soap, be that something that somebody is washing their body with or with a detergent as well. 02:12 And if it’s really a generalized rash, think about atopic dermatitis, which is more of a generalized type of rash and we’ll talk about that in our discussion of generalized rashes. 02:23 So, how do you treat dermatitis? Obviously, avoid the triggers with contact dermatitis. 02:27 That should be pretty obvious. 02:29 With allergic dermatitis, we don't always find a trigger. 02:32 I’d say, we’re lucky if we can find something in half of cases. 02:36 But it doesn't mean we necessarily send for allergy testing. 02:39 Patients sometimes know cold, drier conditions and other things can make them break out in rash. 02:46 And so, that's when they step up their therapy. 02:49 The primary therapy is just treating dyshidrosis. 02:51 I'm a big believer in using moisturizers, the kind you dip your hand into and rub on are much better than the kind you pump because they are a little greasier, but still tolerable as well. 03:03 Topical corticosteroids certainly have a role in the management of dermatitis. 03:08 We try to avoid using them on a chronic basis. 03:10 But particularly for these cases where it's allergic or it’s contact dermatitis and it’s a finite amount of time when the rash is present, topical corticosteroids for a week or two aren’t going to hurt anything. 03:22 And then going back to that emollients and using them very religiously in order to prevent this from occurring again. 03:33 So, fungal infections, you typically see as another maculopapular rash. 03:40 This one has a central clearing and a scale associated with it. 03:43 And think about it in those areas that have a lot of moisture, the intertriginous areas, feet and hands, more common in obese patients who have more intertriginous areas. 03:52 Tinea versicolor is a superficial fungal infection caused by the fungus Malassezia furfur. 03:57 It presents as either hypopigmented or hyperpigmented macules. 04:01 Occasionally a patient can manifest with pruritus, but most commonly the lesions are asymptomatic. 04:06 The diagnosis is usually clinical. 04:09 Although not necessary most of the times, the diagnosis can be confirmed by application of KOH on the skin scrapings and examination under a microscope. 04:17 This test shows the characteristic spaghetti and meatballs or the bacon and eggs sign. 04:21 Tinea versicolor can be successfully treated by topical application of selenium sulfide or azole antifungals, such as ketoconazole. 04:30 And here's a picture. That sounds like before a minute ago. 04:33 There is - so you can see, that's a great example of central clearing. 04:36 It doesn't have as much of a scale in the picture in the middle, but you can see some of the lesions on the upper corner have a more of a scale to them. 04:46 And so, that's really pathognomonic. 04:50 And usually - especially if it's a little itchy and if it’s in the right area, you've got a diagnosis of - in this case, tinea corporis. 05:00 If it’s on the body, a fungal infection. 05:02 So, first, consider over the - for prevention, consider over-the-counter products to reduce moisture. 05:07 I've actually seen significant weight loss, even like associated with bariatric surgery, helped cases that are really hard to control because without controlling that moisture with something like talc or zinc oxide, it’s really hard to get the fungal infection resolved. 05:22 Many times, it will come back. 05:24 But topical antifungals doesn’t have to be fancy, but regular application of even a medication like clotrimazole, which has been around, is usually going to be effective. 05:33 You may need to be more persistent, particularly in patients with diabetes and obesity. 05:38 One week is probably not going to do it. 05:40 They may need a couple weeks. 05:41 And then they really do need to work on maintaining a drier environment in those intertriginous areas to prevent the recurrence of fungal infections.
About the Lecture
The lecture Localized Rashes: Dermatitis and Fungal Infections by Charles Vega, MD is from the course Acute Care. It contains the following chapters:
- Localized Rashes
- Dermatitis
- Fungal Infections
Included Quiz Questions
A 45-year-old obese woman complains of an itchy rash under her breasts for the past 2–3 weeks. She has a history of diabetes. On physical examination, the rash is distributed under the skin folds under her breasts. It consists of moist, red patches. Which of the following is the most appropriate next step in management?
- Topical clotrimazole and moisture reduction
- Topical steroids
- Topical moisturizers
- Topical ciprofloxacin
- Nafcillin
An 8-year-old boy is brought to the clinic by his father because of an itchy rash that has developed overnight over his back, chest, abdomen, and thighs, sparing the region of skin under his underwear. The family is not using any new soaps or detergents. His uncle just bought him a new jersey set which he wore all day yesterday. On physical examination, he is well and afebrile. Which of the following is the most likely diagnosis?
- Contact dermatitis
- Intertrigo
- Viral exanthem
- Atopic dermatitis
- Tinea coropris
Which of the following best describes the clinical presentation of allergic contact dermatitis?
- Well-demarcated, pruritic, eczematous eruption localized to the area of skin that comes in contact with the allergen
- Well-demarcated, nonpruritic, eczematous eruption localized to the area of skin that comes in contact with the allergen
- Well-demarcated, nonpruritic, eczematous generalized eruption
- Well-demarcated, pruritic, eczematous generalized eruption
- Well-demarcated, nonpruritic, non-eczematous eruption localized to the area of skin that comes in contact with the allergen
Which of the following is NOT effective in the treatment of tinea corporis?
- Nystatin
- Wearing moisture absorbing clothing
- Weight loss
- Oral antifungal therapy
- Topical antifungal treatment
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Very good presentation, with colorful visualization, and explanation. The lecturer was specific.