Playlist
Show Playlist
Hide Playlist
Derma Case: 23-year-old Man with Bumps on His Penis
-
Slides Virally-mediated Skin Lesions.pdf
-
Reference List Dermatology.pdf
-
Download Lecture Overview
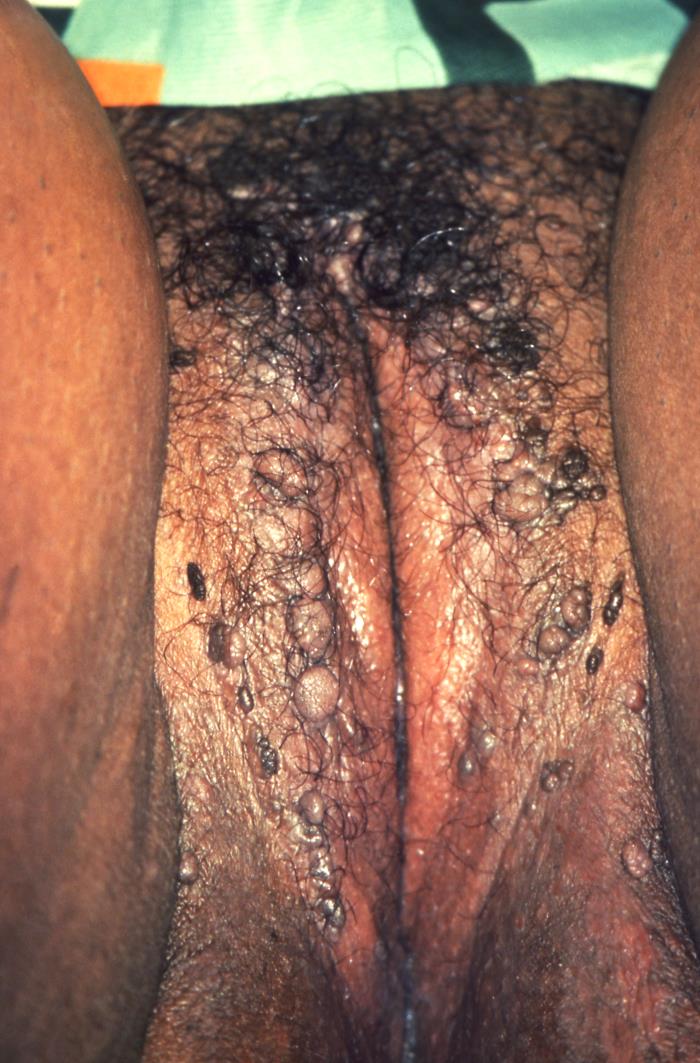
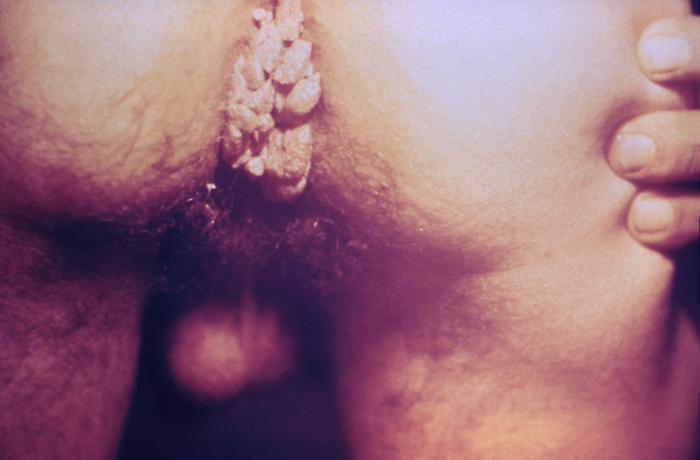
00:01 Alright, I think it's time we moved on to case number 2. 00:05 A 23-year-old man now presents to your office, concerned about some bumps on his penis. 00:11 He noticed them several weeks ago in the shower. 00:13 He tried rubbing alcohol, God knows why, and then a topical antifungal, to no avail. 00:19 These lesions are not itchy or painful, he denies any fevers or chills, no dysuria, no penile discharge. 00:26 His social and family history is essentially non-contributory, except that he has been sexually active with 5 female partners in the past 12 months. 00:35 Review of systems is negative, his vital signs are over the normal limits. 00:39 And then on exam of his genitourinary system, he has numerous, nontender, skin colored, fleshy papules, scattered on the shaft and base of his penis. 00:49 No mucosal involvement and no inguinal lymphadenopathy. 00:53 So, highlighting a few key features here, the time course appears to be subacute. 00:58 He noticed them several weeks ago. 01:00 In terms of the pattern of skin involvement, it is asymmetric involvement exclusively of his genitalia. 01:06 Skin inflammation, they're nontender, there don't appear to be pustules so doesn't sound there's much skin inflammation. 01:13 And lastly, systemic involvement - we're not seeing any. 01:16 So, that's basically what we've got at this point. 01:20 Alright, let's take a look at our differential diagnosis. 01:23 Condyloma acuminata, acrochordon, genital herpes, verruca vulgaris and chancres. 01:30 Well that's a mess of Greek and Latin. 01:32 Let's see if we can make our way through it all. 01:34 First off, condylomata acuminata, that's a fancy term for genital warts. 01:40 The etymology actually means pointed, round tumor which distinguishes a genital wart from the more flat appearance of plantar and common warts which are also caused by HPV. 01:52 In any event, these asymptomatic lesions are incredibly common. 01:56 In fact, they're the most common sexually transmitted disease above all else and they manifest on the shaft of the penis. 02:02 They're more common in sexually active men and women so this one clearly is gonna stay on our list. 02:10 Next stop, acrochordon. 02:12 What's with the fancy words? Okay, an acrochordon is the official term for a skin tag which is depicted here in our image. 02:20 It's a fleshy papilloma that most often occurs in flexural creases, like the nape of the neck, the axilla, the groin. 02:26 We should probably keep this one on our list for now. 02:30 Genital herpes, finally some english. 02:33 Genital herpes is typically caused by herpes simplex virus 2, though it can also be caused by HSV 1. 02:40 It's relatively common viral infection with myriad skin manifestations but the lesions of HSV 2 are more of the painful vesicular or ulcerative type rather than our patient's painless, fleshy papules. 02:54 So I think we can safely take HSV-2 and genital herpes off the list. 03:01 And here we're back to the latin. 03:02 Verruca vulgaris This is a fancy word for common wart. 03:07 Common warts is one subtype of cutaneous warts. 03:11 The others of which include plantar warts and flat warts, we've already mentioned another type of wart above. 03:16 Cutaneous wart is an umbrella term for warts caused by HPV that are not occuring in the anogenital region which is we've already discussed are called condylomata acuminata. 03:27 see above. 03:28 Hence, since our patient's lesions are in fact in the anogenital area, if they were gonna have any kind of wart, it would be condylomata acuminata. 03:37 So we can safely take verruca vulgaris off of our list. 03:41 A bit of taxonomy goes a long way. 03:44 Lastly, chancre. 03:46 A chancre is the classic lesion of primary syphilis. 03:50 Now it starts as a painless papule, similar to our patient at the site of inoculation. 03:56 though it eventually progresses to a painless ulcer. 04:00 It'd be unusual to have multiple lesions like we have on our patient and also, you'd more likely have some accompanying lymphadenopathy. 04:07 Now, while the chancre represents the primary syphilis lesion, the spirochete bacterium of syphilis, Treponema palliidum, soon goes systemic even as the ulcer heals over several weeks. 04:18 So, patients develop some systemic manifestations. 04:21 And later, secondary syphilis can occur with a diffuse, classic, maculopapular rash eruption on the trunk and extremities, including the palms and soles. 04:30 It's really not sounding at all like what our patient has had for the past several weeks, so I think we can safely take off chancre and syphilis.
About the Lecture
The lecture Derma Case: 23-year-old Man with Bumps on His Penis by Stephen Holt, MD, MS is from the course Skin Infections.
Included Quiz Questions
Genital herpes is most commonly associated with which of the following viruses?
- Herpes simplex virus 2
- Herpes simplex virus 1
- Human papillomavirus
- Herpes simplex virus 3
- Herpes simplex virus 4
Which of the following statements is true regarding condylomata acuminata?
- It commonly presents as asymptomatic skin lesions over the genitalia in sexually active patients.
- It is the third most common sexually-transmitted disease.
- It commonly affects palms and soles.
- It is caused by cytomegalovirus.
- Inguinal lymph nodes are usually enlarged and tender.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |