Playlist
Show Playlist
Hide Playlist
Dacryocystitis
-
Slides External Eye Diseases Dacryocystitis.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
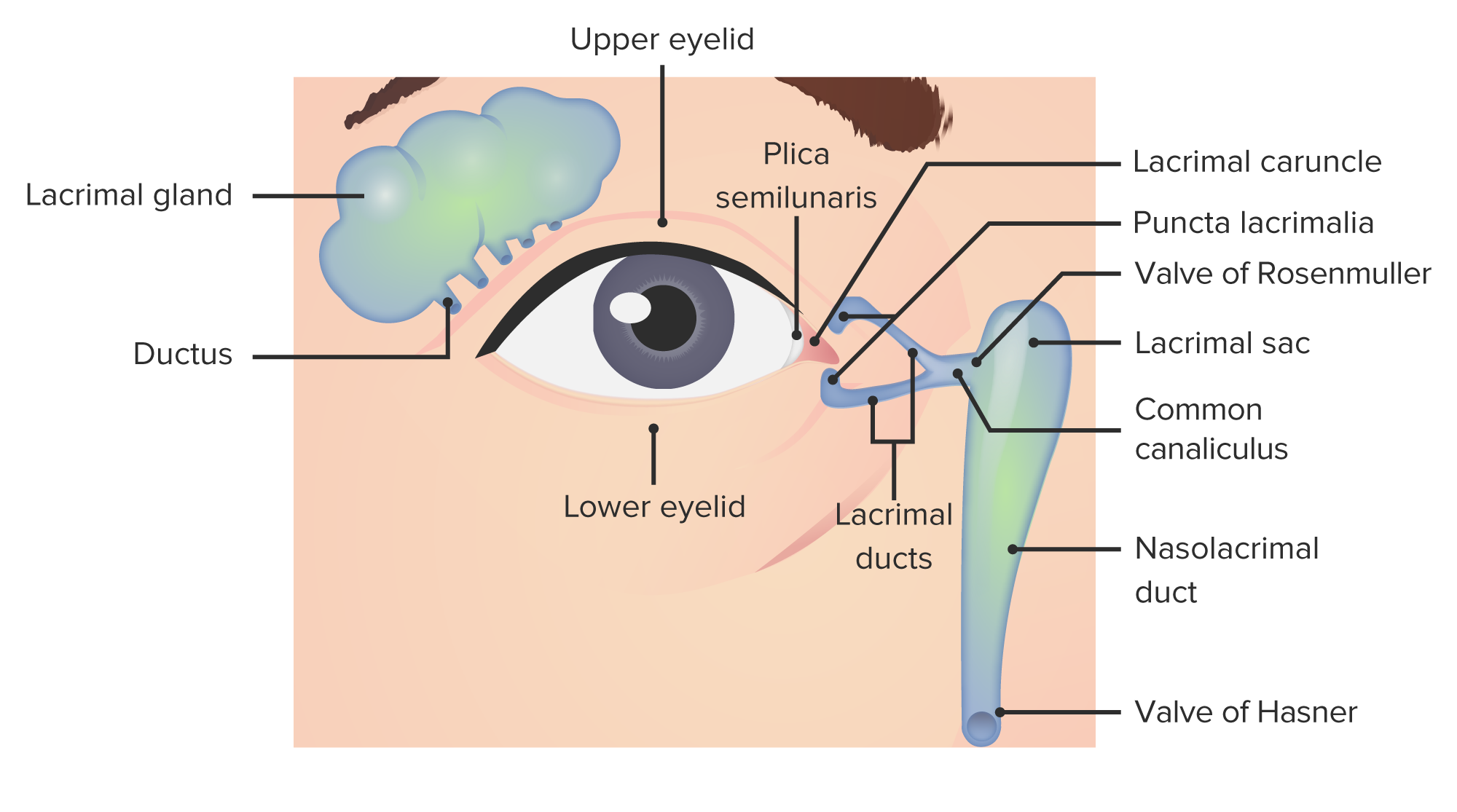
00:01 All right here, we are continuing down into deeper structures within the eye to look at the various pathologies that can occur. 00:11 This session is all about diseases of the lacrimal structures. 00:15 So by way of a quick review, remember that the lacrimal gland that sits up kind of in the upper outer portion of the eyes, of the external eyes, is where we are going to generate fluid and that fluid includes mucin, aqueous components and fat, And its job is to lubricate the anterior surface of the eye. 00:37 That fluid is going to move from the lacrimal gland as it gets secreted, wash across the eye and then exit from the lacrimal caruncle at the medial canthus into the superior, inferior lacrimal canaliculi. 00:51 From there, those little tiny ducts, we're going to go into the lacrimal sac and then it's going to drain out into the nose. 00:58 Remember that if you have excess tearing, you're crying, you also end up with a runny nose. 01:03 Well, that's because those tears are washing across, going out the various little canaliculi to the lacrimal sac and out your nose, and that's, you're draining tears from your nose. 01:13 Cool, huh? All right. 01:15 We're going to talk about inflammation of the structures and in particular, inflammation of the lacrimal sac and this is going to be dacryocystitis. 01:24 There is also inflammation that can occur more upstream in the lacrimal gland called dacryoadenitis, but that's relatively uncommon. 01:32 Won't be on the boards for you. 01:34 And we're going to just say, yeah, that can happen there, too. 01:37 Of course it can. 01:38 But we're going to focus on the inflammation of the lacrimal sac. 01:41 So there are a couple of different ideologies that we need to consider. 01:46 One is congenital and one is acquired, broad strokes. 01:51 So you can have stenosis. 01:52 Remember those little canaliculi? Well, they can become stenotic, or the drainage from the lacrimal sac can become stenotic, or can be stenotic just the way that it developed. 02:03 That's your dacryostenosis. 02:05 You can also have a dacryocystocele. 02:08 In other words, an abnormal dilation of those little canaliculi or dilation of the sac. 02:14 And we get kind of a little puddle and accumulation of stagnant tears that aren't draining effectively. 02:22 And all it takes is a few bacteria to wander in there and all that mucin and fat and aqueous stuff. 02:28 That's a wonderful culture medium, and they grow. 02:31 So they can grow in that stagnant tear pool happening when there is obstruction of the little duct work or if we have a little abnormal outpouching. 02:40 Okay, those are the congenital causes. 02:42 There can also be acquired causes. 02:44 So if you think about it, any tumor kind of in the nose, in the lacrimal sac and in the various sinuses as we're draining out of the lacrimal sac and into the nose, is potentially going to block outflow. 02:59 And again, we're going to get inflammation behind that as that becomes infected. 03:03 Trauma. 03:04 So you get punched in the nose, that can actually impinge on those very delicate little canalicular structures. 03:10 You can develop a stone, so the material that is draining or is being produced by the lacrimal gland, in fact can become dehydrated, can become viscous, and you can actually get a little lith, a little stone, a dacryolith, and it can sit in that in our various little drainage pathways and cause an obstruction. 03:33 So a dacryolith. 03:35 You can have inflammatory disease, so sarcoidosis and other inflammations, that specifically or just unfortunately impact on either the lacrimal sac or the canaliculi will cause obstruction of flow. 03:50 And then finally, sinusitis. 03:52 Any inflammation, particularly in the ethmoid or maxillary sinuses, are going to impact on the ability to get what's in the lacrimal sac out because the inflammation, the sinusitis is causing edema, which is going to end up compressing extrinsically, all of those passages out of the lacrimal sac. 04:13 So in all those cases, what is happening is that we've got an accumulation, a puddle, a stagnant tear pool that we can't drain effectively. 04:22 And again, it will become infected. 04:24 Okay, prepare yourselves because the next pictures are not pretty, but are important that you recognize. 04:31 This is what it looks like. 04:33 And basically, we are looking mostly at the inner canthus, the top three pictures, A, B and C, we're looking at the inner canthus. 04:41 That's where the lacrimal sac is. 04:43 And in these cases, it's become inflamed, infected, it's full of pus. 04:49 Okay, so it's going to be red. 04:50 That's inflammation, right? Erythema, rubor, there's going to be edema. 04:55 So there's going to be swelling or tumor. 04:58 It's going to be tender. 04:59 Oh my goodness. 05:01 I'm just looking at this, I, I hurt. 05:03 Okay, so there's, it's going to be quite painful. 05:05 Again, this is part and parcel of the normal inflammatory process. 05:10 There will be a purulent discharge so frequently, these areas of swelling, it's basically a big abscess behind there, will come to a head and burst and you will get yellow bacterial and neutrophilic discharge. 05:25 Because we are blocking the normal flow of tears out across the eye and then down through the canaliculi into the tear sac, that will accumulate. 05:36 It has no place to go. 05:37 So the eyes will feel like they're constantly tearing. 05:40 We're not draining appropriately. 05:42 And if we get damage to the walls of the canaliculi or damage to the sac itself, we can develop a mucocele. 05:50 So if we currently have inflammation there, we will get weakening of the wall or we'll have a little outpouching. 05:56 And then you may be prone to the dacryocystitis over and over and over again. 06:00 Complications of this. 06:02 Clearly, if we are accumulating bacteria there in our drainage pathway, we are going to and we have infection there, we're going to get likely bacterial conjunctivitis. 06:13 So we will get now bacteria that are backing up into the conjunctiva. 06:19 We will get orbital cellulitis. 06:21 So we will get infection that extends not only from just underneath the medial canthus, but up into the all the way around the eyes. 06:30 Importantly, because there are structures right behind the eyes called the brain, you can get meningitis and you can get sepsis. 06:38 This can progress to the point where you are having bacteremia and systemic inflammatory responses to a very nasty infection. 06:48 So how do we treat this? So fortunately, typically, with time, the openings that have been blocked either by a little stone or inflammation or a variety of other things will open and we'll get drainage and it'll go away. 07:02 That's if it's not as bad as we were looking back on those pictures A, B, C and D. 07:06 You can put on warm compresses. 07:08 By doing that, you will cause dilation of the ductwork and hopefully get better drainage. 07:14 And then finally, if you've got really severe kind of involvement and you've got, you've got conjunctivitis or you've got cellulitis, you need to have antibiotics. 07:24 And in some cases, with really severe nasal lacrimal duct obstruction, surgery may be necessary and that's why we have the scalpel blade standing there. 07:33 Okay, with that, we finished looking at inflammatory processes, infections mostly involving the lacrimal apparatus.
About the Lecture
The lecture Dacryocystitis by Richard Mitchell, MD, PhD is from the course External Eye Diseases.
Included Quiz Questions
What structure is affected in dacryocystitis?
- Lacrimal sac
- Lacrimal caruncle
- Lacrimal canaliculi
- Lacrimal gland
- Lacrimal duct
What congenital abnormality can result in dacryocystitis?
- Stenosis of the lacrimal sac
- Trauma to the lacrimal sac
- Tumor of the lacrimal sac
- Infection of the lacrimal sac
- Agenesis of the lacrimal sac
What is an abnormal dilation of the lacrimal canaliculi called?
- Dacryocystocele
- Dacryostenosis
- Dacryoadenitis
- Dacryocystitis
- Dacryoagenesis
What is a stone in the lacrimal apparatus called?
- Dacryolith
- Dacryocystocele
- Rhinolith
- Sialolith
- Nephrolith
What is a life-threatening complication of dacryocystitis?
- Sepsis
- Mucocele
- Dacryoadenitis
- Dacryolith
- Dacryocystocele
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |