Playlist
Show Playlist
Hide Playlist
Congenital Adrenal Hyperplasia (CAH) – Adrenal Insufficiency
-
Slides AdrenalInsufficiencyCongenitalHyperplasia EndocrinePathology.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
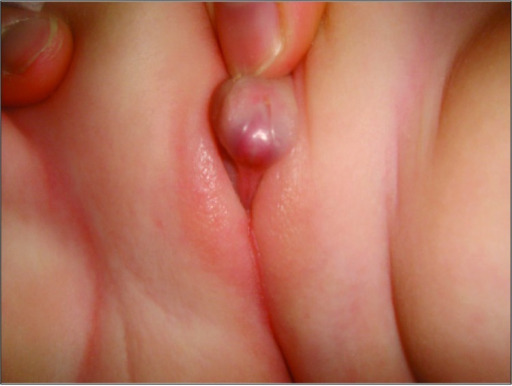
00:02 Let’s do Congenital Adrenal Hyperplasia. 00:04 Another cause of adrenal insufficiency, but let’s get away from the adrenals being damaged, let’s get away from the pituitary being damaged. 00:15 Congenital adrenal hyperplasia, as the name implies, how old is your patient? A child. 00:20 What’s going on in the child? Enzyme deficiency. 00:26 Here, in the very beginning section of adrenal patho-physiology, I walked you through, in great detail, the physiology of your adrenal cortex with your various enzymes. 00:37 Name me the enzyme that will take you from zona glomerulosa into the zona fasciculate. 00:42 17 alpha-hydroxylase. 00:45 Name me the enzyme that will take you from the first step of your zona glomerulosa, fasciculata, reticularis from your pregnenolone into progesterone. 00:56 3 beta- hydroxysteroid dehydrogenase. 00:58 We talked about that. 01:00 Give me the next two enzymes that we will be focusing upon. 01:03 21 and 11, go in chronological order. 01:08 Of all the enzymes that you want to know, which one do you want to know for sure? 90 percent of your congenital adrenal hyperplasia… 90 percent of congenital adrenal hyperplasia is due to 21 beta-hydroxylase insufficiency, that’s where you look first. 01:28 Be smart about how you study. 01:31 What about the other enzyme deficiencies, could they occur? Yes, of course. 01:35 The other five percent is actually 11 beta, that’s already 95 percent of all congenital adrenal hyperplasia. 01:42 You have a measly three percent for the other enzymes. 01:45 Whatever, I’m not even going to discuss them. 01:47 So, I’ll do the 95 percent obviously. 01:51 What happens? Child and when this occurs, enzyme is not present. 02:00 If the enzyme isn’t present, it doesn’t matter which one actually and if there isn’t, then you don’t have enough cortisol. 02:07 If you don’t have enough cortisol, what’s the feedback? ACTH. 02:14 All congenital adrenal hyperplasia will have patients… will not have sufficient cortisol as a child; all congenital adrenal hyperplasia patients as a child will have increased ACTH. 02:29 All congenital adrenal hyperplasia will have hyperplasia of the adrenal, why? ACTH is bombarding both of the adrenals granted you don’t have the enzymes, but what will be the adrenals undergoing? Hyperplasia. 02:47 Is that clear? That’s why your child doesn’t have cortisol, that’s why your child has excess ACTH. 02:55 The next question I always get from residents and students, “Dr. Raj, why did these children not have hyperpigmentation around the oral mucosa?” That is an excellent question. 03:05 Because you don’t have enough influence of your pre… proopiomelanocortin like you would with Addison’s. 03:10 Interesting, isn’t it? Darn good question, but you will not find… that’s not what your focus is, the hyperpigmentation, no, no, no. 03:20 Infants, children. 03:21 Take a look at this. 03:23 Here you have… that is not a penis, that’s a clitoris that’s undergoing enlargement. 03:29 This is a female? Yes. 03:31 So, that’s a vagina? That is correct. 03:35 What is going on? It’s called virilisation. 03:37 What’s the most important sign of virilisation? What does virilisation mean? It means actual, physical attributes of a male in a female; increased muscle mass in a female, increased acne in a female. 03:52 But, the most important sign will be clitoromegaly. 03:57 There are two major enzyme deficiencies. 03:59 We’ve seen this picture before, I’m not going to walk you through this again. 04:02 Your focus will be on 21 beta hydroxylase deficiency and when there is 21 beta hydroxylase deficiency, you’re not going to form any mineralocorticoid, the blood pressure’s decreased and if that first column is your glomerulosa, you cannot form any mineralocorticoid. 04:19 What’s that blue box forming? Good, cortisol. 04:23 There’s no cortisol, there’s increased ACTH. 04:27 Now, you can see the feedback, what happens to both the adrenals? Hyperplasia, but you can’t go through your fasciculate. 04:37 You are then forced into the deepest layer of the cortex which is the green box, that is your reticularis. 04:46 What are you producing there? Androgen, aha, excessively. 04:52 In a young this… remember this started in utero, so of course, the clitoris looks like a penis, clitoromegaly. 05:04 And when it comes down to your cortisol, your blue layer, I’ll run through that quickly because we’ve already done all these. 05:13 We’ve done this earlier when I began the discussion of adrenocortical patho-physiology. 05:20 If you’ve missed that discussion, please go back and take a look at our extensive discussion of adrenocortical patho-physiology while I walk you through layer by layer by layer and its functioning and what you’re producing. 05:35 Your focus here in this pathology will be 21 beta-hydroxylase. 05:40 The middle bar that you see there 21 beta, that enzyme will be deficient. 05:45 If you take a look at the glomerulosa, you do not form any mineralocorticoid, that child is going to have decreased blood pressure. 05:52 You’re not going to have… that child is not going to have any cortisol, you’re going to shunt into the reticularis the green box excessively, having increased androgen. 06:03 Here’s a table to summarize all of your congenital adrenal hyperplasia. 06:07 Let’s first begin with 21 beta, 90 percent of your cases, this is your priority. 06:11 Remember that virilisation, I showed you clitoromegaly. 06:14 There will be salt-wasting, your patient will have hypotension. 06:18 There isn’t enough aldosterone, there will be hyponatremia, hyperkalemia. 06:22 The problem is this, enzyme deficiency you can’t form cortisol, but you sure as heck will have 17- hydroxyprogesterone elevated, elevated, elevated. 06:33 You’re going to shunt into your reticularis therefore, you will have increased androstenedione and androgen. 06:38 What’s your treatment here? It is going to be glucocorticoid for sure and also mineralocorticoid because in 21 beta… go back and take a look at the picture, you’re not forming any. 06:49 Now, we have 11 beta, this is five percent; these are the only two that I’ll cover, the rest are a measly three percent. 06:58 The rest including 17-hydroxy or 17 alpha-hydroxylase and the other one being 3 beta-hydroxysteroid dehydrogenase. 07:05 If it’s 11 beta, I’d like for you to pay attention here though. 07:10 If it’s 11 beta, what ends up happening here is that you will have too much 11 deox. 07:16 Physiologically, 11-deox has what kind of mineralocorticoid activity? Very weak, but pathologically, you find it to be excessive. 07:27 Take a look at the diagnostic study where we see high 11-dexoycorticosterone… welcome to 11 deox that then causes… you see where I have put in bold hypertension? So, imagine connecting the dots, high 11-deox causes hypertension, as simple as that. 07:49 So, you have excessive mineralocorticoid activity. 07:52 So, why in the world would you want to give mineralocorticoid as being part of management? That makes no sense. 07:58 Therefore, glucocorticoid therapy only. 08:01 Do you see how everything’s connected? Obviously, here, you’re going to shunt into reticularis. 08:05 Here, once again, virilisation, welcome to clitoromegaly. 08:09 Just to be complete, here’s your 17 alpha-hydroxylase, go back and take a look at the picture, you are stuck in your glomerulosa. 08:17 You’re not going to have virilisation because you cannot go into the reticularis, it is rare. 08:24 You’re not going to have virilisation in this patient. 08:26 And by the way, just to make sure we’re-we’re clear, so obviously, if it’s a female and it’s a child, that will be clitoromegaly, but how... what do you call excessive masculinization in a boy? It’s just called precocious puberty. 08:39 What does that mean? It’s just puberty comes way early in that boy because of increased masculinization. 08:45 Then you have 3 beta-hydroxysteroid dehydrogenase. 08:48 Once again, very, very rare; something called male pseudo-hermaphroditism, keep that in mind for 3 beta-hydroxysteroid. 08:57 Once again, these two enzyme deficiencies only make up three percent.
About the Lecture
The lecture Congenital Adrenal Hyperplasia (CAH) – Adrenal Insufficiency by Carlo Raj, MD is from the course Adrenal Gland Disorders.
Included Quiz Questions
What enzyme is most commonly affected in congenital adrenal hyperplasia?
- 21-beta-hydroxylase
- 17-alpha-hydroxylase
- 3-beta-hydroxysteroid dehydrogenase
- 11-beta-hydroxylase
- Desmolase
What is NOT seen in congenital adrenal hyperplasia due to 21-beta hydroxylase deficiency?
- Decreased androgen production
- Decreased cortisol levels
- Bilateral adrenal hyperplasia
- Increased ACTH
- Variable production of mineralocorticoids
What causes virilization?
- Increased androgen production
- Increased progesterone production
- Decreased cortisol production
- Increased ACTH
- Decreased aldosterone
What is NOT a characteristic of 21-beta-hydroxylase deficiency?
- Low serum DHEA
- Hyponatremia
- Hyperkalemia
- Hypotension
- Increased levels of 17-OH progesterone
What is NOT a characteristic of 11-beta-hydroxylase deficiency?
- Lack of virilization in female patients
- Hypertension
- Hypokalemia
- Increased levels of 11-deoxycorticosterone
- Increased serum DHEA
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
In my opinion, Dr. Raj's lectures are truly unique. He makes learning fun and has a real way with words. I'd absolutely recommend his lectures—just be sure to take some notes and get ready to laugh a few times!