Playlist
Show Playlist
Hide Playlist
CHARGE and VACTERL
-
Slides CHARGEandVACTERL Pediatrics.pdf
-
Download Lecture Overview
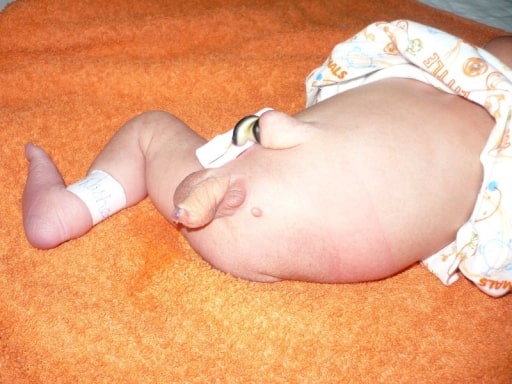
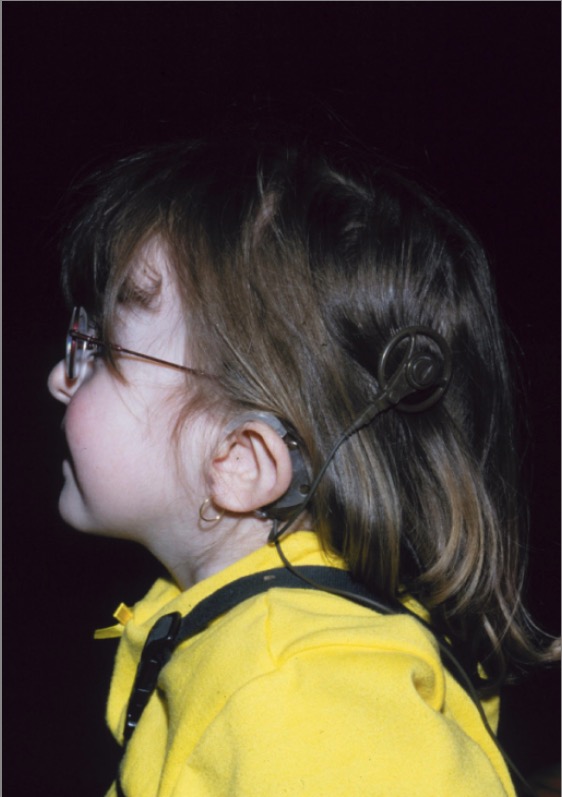
00:00 In this lecture, we'll discuss CHARGE and VACTERL syndromes. I'm bringing these 2 together mostly because in both these syndromes each letter stands for a symptom that the patient has. They do have some overlap, for instance both can present with TE fistulas but generally speaking they don't really have a whole lot in common with each other except that we have to remember what all the letters stand for. CHARGE syndrome. CS occurs in approximately 1 in 10,000 live births. Most cases result from mutations in the CHD7 gene, which you don't need to memorize. Rarely, CS is inherited in an autosomal dominant or other pattern of inheritance. The recurrence risk of having another child with CS if an unaffected couple already has 1 child with CS is 1-2%. Okay, what does CHARGE stand for? The C is for coloboma which is that abnormality of the iris where the pupil extends through it. You can see that in this patient's left eye, on the right side of the screen. These patients will have heart defects. 01:04 They may have choanal atresia, atresia of the choanal variety. Remember that's where you can't insert the tube down past into the stomach, it gets stuck in the back of the nose. They may have retardation, we don't like to use that word anymore but it fits with the letter. This is really an intellectual disability. They may have genital malformations and they may have ear anomalies as you can see in this patient here. So, let's go through them a little more carefully. There are major and minor clinical features. The ocular coloboma is a major clinical feature. It can be unilateral or bilateral. Choanal atresia or choanal stenosis is either unilateral or bilateral and it's a bony or membranous choanal atresia or stenosis in the back of the nose such that you can't get pass the nose and down into the pharynx. They may have cranial nerve abnormalities such as a facial palsy, hypoplasia of the auditory nerve, leading to ear problems like you saw with E and they can have ear abnormalities such as auricular malformation, cochlear defects, or temporal bone abnormalities. These children are often deaf. There are also minor clinical features. These include genital hypoplasia in males that can mean a micropenis or cryptorchidism and in females that can mean a hypoplastic labia. 02:32 They often have development problems such as intellectual disability. They will have cardiovascular defects and this can be many things but often Tetralogy of Fallot or a common AV canal or an aortic arch problem. They may have growth problems so they'll have short stature and occasionally this is because of growth hormone deficiency. They may have interesting facial features or certainly unique facial features such as a square face with a broad and prominent forehead and prominent nasal bridge and a flat midface. And then there are other findings. One of them is tracheoesophageal fistula and then also a cleft palate. So those are the major and the minor criteria how do we make the diagnosis. A definite diagnosis of CHARGE can be made if 4 major or 3 major and 3 minor criteria are present. A possible diagnosis is made if 1-2 major and several minor characteristics are present. If we suspect either a possible or a definite diagnosis, we will do molecular testing to detect a pathogenic mutation in the CHD7 gene. The testing will show the abnormality in 90% of the definite diagnostic cases, but only 70% of the cases with a possible diagnosis will show a mutation. 03:47 In the next slide, we'll see a comparison of the different criteria used for CHARGE syndrome. 03:52 They have overlapping features, but the most recent criteria by Dr. Hale from 2016 incorporate the clinical features with the genotypic finding of an abnormal CHD7 gene, if it is present. The table is shown for educational purposes only and is not intended to be memorized or considered as testable material. So how do we manage these patients? Well, in neonates, they may well have respiratory distress because of their choanal atresia. Choanal atresia can be a big problem for infants who are trying to breathe. They may have heart abnormalities, which we have to intervene with immediately such as Tetralogy of Fallot or a common AV canal. And they may have feeding difficulties which can lead to difficulties with growth. From the brain standpoint, we worry about low muscle tone which predisposes to exhaustion and thus often a difficulty with feeding. They often need frequent rest and we need to assess their cranial nerve function as well and make sure their hearing is okay, these children need hearing tests. For their growth and development, we intervene with psychological and school evaluations. We will often do individualized learning plans for these children in school. And we're going to keep surveillance on them. We're going to be following their cardiac echos, their renal sonograms, repeating dilated eye exams, and of course the audiologic evaluation. 05:17 So let's switch gears now to VACTERL. VACTERL is 1-2 per 10,000 births. The recurrence risk is there for families who have had 1 child with VACTERL. If they have had 1 affected child, the recurrence risk is 0.5-2%. If they have had more than 1 affected child, the recurrence risk is about 20%. There are many risk factors for this. First of all, there could be none, it's just a sporadic case. It's a little bit more common in Caucasian males, it may be more common in type 1 diabetic mothers, and it's also more common in patients who have thalidomide exposure. So it's a combination of genetic and environmental causes for VACTERL. So what does VACTERL stand for? Well, the V stands for vertebral anomalies, A is anal atresia which is a surgical emergency in newborns. If you have an atretic anus, you can't pass your meconium and they're going to be obstructed. They will have cardiac defects and that's the C. Ventricular septal defect is the most common, but it could be something else. 06:23 Tracheoesophageal fistula happens commonly in these patients and this can be in most types quite incompatible with life past the first day or so. The only type that can really persist is the H type, and that's the minority of cases. Patients may have renal anomalies or malformations, which can be problematic. And they can have significant limb defects as in this patient or they can just have slightly less dramatic ones such as renal dysplasia or polydactyly and syndactyly. 06:53 So, what test do we get in a patient who has VACTERL? Well, we're certainly going to get a spinal ultrasound to make sure that this is contiguous and that they have a functioning and complete spine. We also will get a spinal x-ray for similar reasons. We will typically echo these patients to rule out the VSD or whatever the cardiac problem is and likewise we'll get a renal ultrasound to make sure that system is good. And lastly, we will observe them carefully for respiratory distress and feeding problems. These children may require G-tubes and other things assuming that they're structurally okay to eat and don't have a TEF or anal atresia or something else that requires surgery defects. So that's my review of CHARGE syndrome and VACTERL syndrome. Thanks for your time.
About the Lecture
The lecture CHARGE and VACTERL by Brian Alverson, MD is from the course Pediatric Genetics. It contains the following chapters:
- CHARGE Overview
- VACTERL Overview
Included Quiz Questions
Which of the following is NOT a finding in CHARGE syndrome?
- Gastroschisis
- Coloboma
- Heart defects
- Ear anomalies
- Choanal atresia
Which of the following is a major criterion of CHARGE?
- Coloboma
- Square face with broad forehead
- Intellectual disability
- Tetrology of Fallot
- Genitourinary anomalies
How many criteria must be present for a definite diagnosis of CHARGE syndrome?
- 3 major criteria and 3 minor criteria
- 2 major criteria and 2 minor criteria
- 2 major criteria and 4 minor criteria
- 1 major criteria and 4 minor criteria
- 3 major criteria
Which of the following is not a feature of VACTERL association?
- Choanal atresia
- Cardiac defects
- Tracheoesophageal fistula
- Renal dysplasia
- Polydactyly
A child presents with coloboma, choanal atresia, anosmia, and a short, wide ear with little lobe. Which of the following is the most likely diagnosis?
- CHARGE syndrome
- TORCH infection
- VACTERL association
- Down syndrome
- Pierre Robin sequence
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
great lecture with sufficient information to answer all my questions