Playlist
Show Playlist
Hide Playlist
Cervix – Female Reproductive System
-
Slides 09 Human Organ Systems Meyer.pdf
-
Reference List Histology.pdf
-
Download Lecture Overview
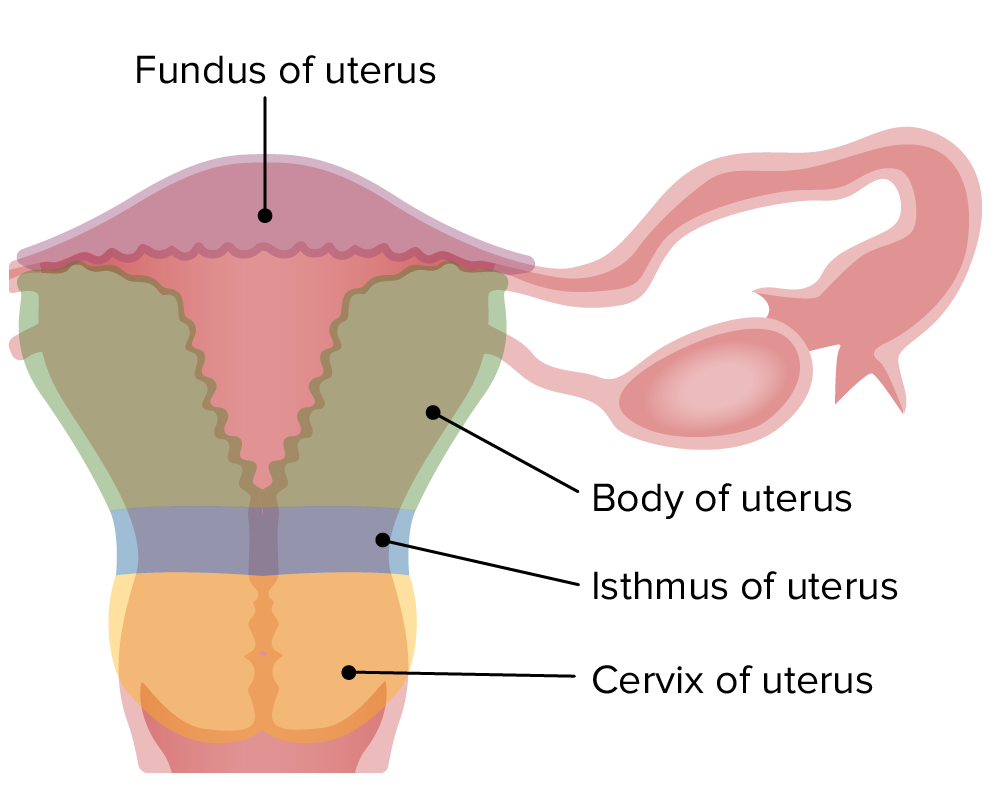
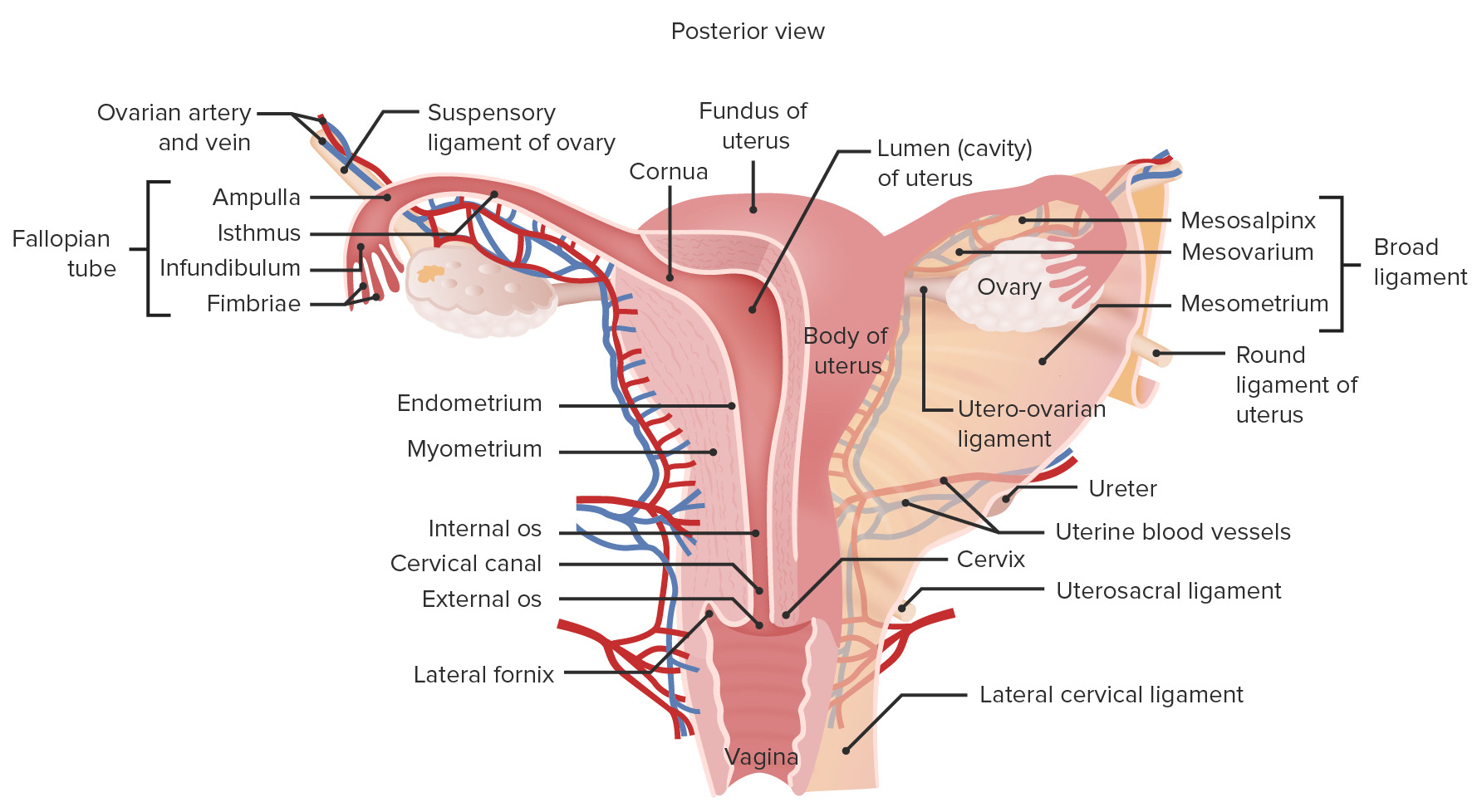
00:00 Now let’s look at the cervix and the vagina. Shown on the diagram, you can see the cervix in the vagina. I want to just bring your attention to the label of the cervix there. You can see part of the cervix, which is really an extension, a component of the uterus, part of the cervix extends into the vaginal cavity or tube. 00:30 The part of the cervix that is still adjacent to the lumen of the endometrium is called the endocervix, and the part that’s protruding and the epithelium is exposed to the vaginal lumen is called the ectocervix. And they are two very important parts of the cervix at the junction of vagina because the epithelium changes. Sections of the cervix are shown here in this slide. 00:58 There are three histological sections indicated. On the top left-hand side is a low magnification of the cervix. And the epithelium on the far left side of that section turns around the loop and then enters into the vagina area. Down the bottom left hand side, you can see identified cervical glands. These cervical glands are housed within the cervix mucosa. These glands secrete mucus. And the mucosa of the cervix doesn’t undergo the cyclical changes as dramatically as the endometrium in the uterus. It doesn’t have a spiral artery. So, the mucosa is not shed from the cervix. But the mucus secretion does change. These glands get very active at the time of ovulation. They secrete 10 times the amount of mucus that they secrete at other times of the ovarian and also the menstrual cycle. And that mucus changes its nature. It becomes very very watery, and that’s conducive for the transport of sperm up through the cervix into the uterus and beyond into the uterine tube. At other times, the mucus is very viscous. It provides a barrier to both sperm transport, as well as possible bacteria and other pathogens trying to make their way up into the uterus and beyond. 02:39 On the top left-hand slide, I’ve labelled the transition zone. This is the zone where the mucosa, the epithelial lining of the cervix which is columnar in nature, the epithelial cells are columnar. It changes as it comes to the junction with the epithelium of the vagina. It changes to be a stratified squamous epithelium. Stratified squamous epithelium is the epithelium designed to reduce wear and tear. And that’s required in the vagina as being the copulatory organ in the female. This transition zone can, at some stages, go through metaplasia. It can change its nature and give rise to cancerous cells. But luckily, the cells lying the cervix, the epithelial cells exfoliate themselves. They lost, in other words, from the surface and they get exfoliated into the vagina. So a Pap smear can sample these cells, and therefore, you can detect, or the technologist, the pathologist can detect whether any cancerous cells are amongst those exfoliated cells.
About the Lecture
The lecture Cervix – Female Reproductive System by Geoffrey Meyer, PhD is from the course Reproductive Histology.
Included Quiz Questions
Which of the following is INCORRECT?
- The cervix produces a steady rate of mucus secretions throughout the menstrual cycle.
- The ectocervix projects into the vagina.
- The cervix is low, hard, and slightly open to allow blood flow during the menstrual cycle.
- The upper cervix is lined by columnar epithelium.
- The lower cervix is lined by stratified squamous epithelium.
Which of the following is secreted by glands in the cervix?
- Mucus
- Serous secretions
- Estrogen
- Progesterone
- Androgens
Which of the following types of epithelium lines the vagina?
- Stratified squamous
- Stratified cuboidal
- Pseudostratified columnar
- Stratified columnar
- Simple squamous
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |