Playlist
Show Playlist
Hide Playlist
Cardiac Case: 44-year-old Man with Indigestion during Exertion
-
Cardiac Case 44-year-old Man with Indigestion during Exertion.pdf
-
Reference List Cardiology.pdf
-
Download Lecture Overview
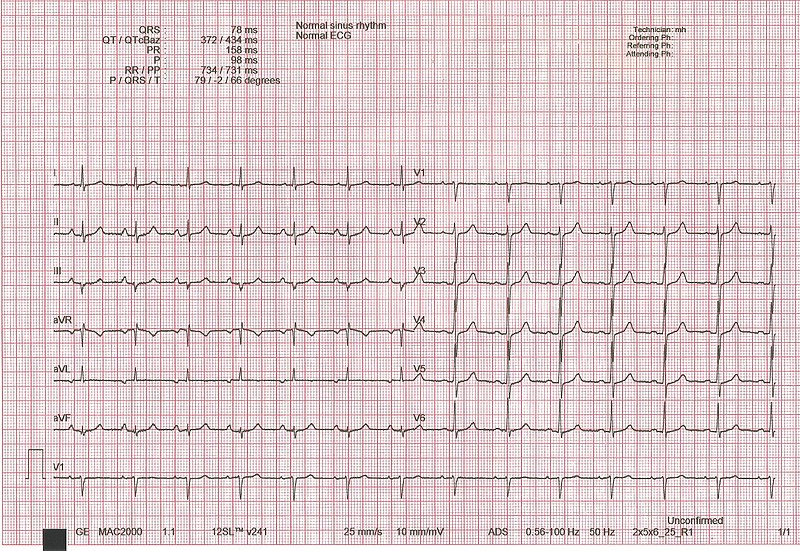
00:01 This 44-year-old man comes into the office complaining of indigestion that occurs only when he climbs stairs or carries heavy packages in from the car. 00:11 The discomfort occurs over his sternum, over his breastbone, and goes away a few minutes after he rests and stops exertion. 00:20 His history is as follows. 00:22 He recently recovered from a viral upper respiratory infection, a cold. 00:26 He smokes two packs of cigarettes and has been doing that for 24 years. 00:31 He has a history of hypertension that's been plus minus controlled, and he's been told he has abnormal cholesterol values and we order an electrocardiogram. 00:41 So the important aspects here is exercise brings on chest discomfort. 00:47 And he has coronary heart disease risk factors. 00:53 So let's look at his EKG. 00:56 And here take a look at it for a few minutes and see what you think. 01:07 So this ECG has some abnormal S, T and T waves. 01:13 But it's really nonspecific. 01:15 It's not like the last one where we saw the nice squared off ST segment depression. 01:21 So this could be consistent with ischemia though. 01:23 And because it's nonspecific. 01:25 But maybe he has a low blood potassium. 01:28 There could be many causes of this. 01:30 He could also be hypoxic because he may have lung disease from all of his years of smoking cigarettes. So the ECG doesn't show us a myocardial infarct, but it does show us some abnormalities in the STNT waves. 01:44 And as said, there could be many causes. 01:46 Ischemia drugs can sometimes do this. 01:49 Hypoxia. As I mentioned, sometimes infections. 01:52 There could be central nervous system disease, a stroke, many, many others. 01:57 So it's not a specific ECG. 02:01 So we're thinking from the story that he has angina pectoris because he gets chest discomfort when he climbs the stairs. 02:07 That's consistent with angina consistent with myocardial ischemia, lack of blood flow in the heart muscle. 02:13 So what are the the diagnostic tests that we could do? Well, we could do abdominal ultrasound, but I don't think we're going to do that. 02:21 We could do a CT coronary calcium scan that would tell us if there's atherosclerosis. 02:27 Um, or we could do an ECG exercise test. 02:31 That's probably the best test to start with an ECG exercise test if the patient didn't want to do that, you could do coronary calcium and see if there was a lot of atherosclerosis there. 02:42 The abdominal ultrasound might be done if the coronary workup turned out to be negative. And you were looking for peptic ulcer disease, or like the last case, a coli, a cholecystitis or a cholelithiasis, that is a stones in the gallbladder. 02:58 And of course, we're going to look at his his cholesterol lipids to confirm that he's at risk for atherosclerosis. 03:06 So let's say we decide that this man does indeed have angina pectoris. 03:12 Let's say he has a stress test that's positive. 03:15 So the first step wouldn't be to rush to the cath lab and put in a stent, but it would be to do medical therapy first. 03:22 We would give him a statin to lower his cholesterol values. 03:25 Then we would control his blood pressure with antihypertensive drugs, probably a beta blocker, and possibly either an angiotensin receptor blocker or an angiotensin converting enzyme blocker. 03:37 We would give him a platelet activation blocker, probably low dose aspirin, perhaps 81mg, and he might at some point, depending on how positive his exercise test, he might down the road get coronary angiography and a possible stenting of a blocked coronary artery. 03:56 How would we decide that? We would look to see how nasty his exercise test looked, if at a very low level of exercise, he had marked street depression and severe, long lasting angina that would push us in the direction of angioplasty, because we would be worried that there was a lot of myocardium not getting blood flow. 04:14 But suppose the medical therapy worked, his angina goes away or his chest discomfort goes away. He leads a normal life, he gets his cholesterol level down and he's perfectly happy. The long term results are just as good with medical therapy as with angioplasty. So we wouldn't rush him to angioplasty. 04:33 And of course we'd want to work with him for smoking cessation. 04:36 If he continues to smoke, his likelihood of suffering a heart attack or living a shorter life increases significantly. 04:44 And usually we refer such a patient to a cardiac rehabilitation program where there's education, graded exercise, and where the exercise physiologists and the nurses watch the patient carefully to make sure that when he exercises, it's safe. 05:01 One other footnote for this case, of course, the example I gave you um, this man's heart rate is quite fast, and you couldn't send somebody with a fast heart rate like this for exercise testing. 05:13 Of course, this was the initial tracing from this patient when he was in pain and worried and seeing the doctor for the first time. 05:20 When you send him for exercise testing, his heart rate has to be down in the normal range again. Um, and it was before he was referred for exercise testing.
About the Lecture
The lecture Cardiac Case: 44-year-old Man with Indigestion during Exertion by Joseph Alpert, MD is from the course Cardiovascular Cases.
Included Quiz Questions
Abnormal ST segments and T waves are least likely attributable to which of the following?
- Decreased LDL cholesterol level
- Ischemia
- Hypoxia
- Infections
- CNS diseases
In this patient with symptoms of indigestion that are worse with exertion, all of the following tests would be included in the workup except which of the following?
- HIDA scan
- Abdominal ultrasonography
- CT coronary calcium scan
- ECG exercise test
- Serum lipids
A 44-year-old man comes to the office because of indigestion when climbing stairs or carrying heavy packages. The discomfort happens over his sternum and disappears a few minutes after he stops exertion. He has a 5-year history of hypertension, abnormal cholesterol values, and a recent upper respiratory infection. He has smoked two packs of cigarettes daily for 24 years. Which of the following is not an indicated therapy for this patient?
- Cholinergic antagonists
- Medical therapy with a statins
- Antihypertensive drugs
- Platelet activation blocker
- Coronary angiography and possible stenting of a blocked coronary artery
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Dr. Alpert provides such a clear & concise overview about high-yield diagnosis & management strategies! Thank you for creating this very helpful lecture series!