Playlist
Show Playlist
Hide Playlist
Bowel Obstruction
-
Slides GIP Bowel Obstruction.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
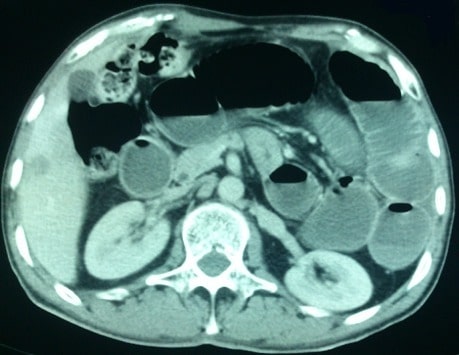
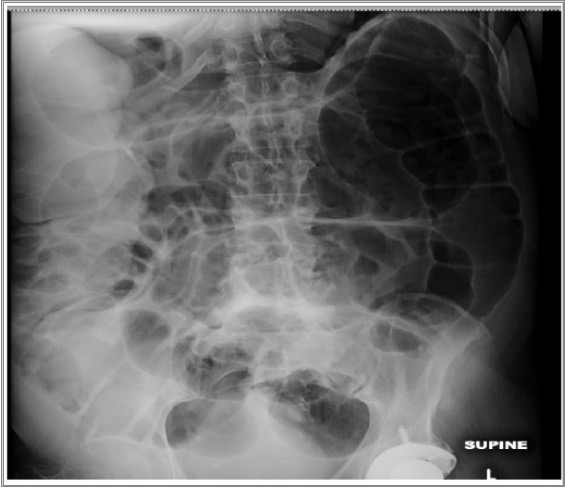
00:01 Welcome. In this talk, we're going to be covering bowel obstruction. 00:05 So, this is obstruction of the small bowel or the colon. 00:09 And there will be different causes in each location or there may be slightly different manifestations and different ways that we're going to diagnose that. The epidemiology overall. 00:19 So, if we're talking about small bowel obstruction, the average age when this is occurring is somewhere around 60 years and the frequency is pretty much the same in men and women. 00:31 Interestingly, between 2% and 4% of emergency department visits in the US have been attributed to small bowel obstruction. 00:38 And if we're talking about obstruction, anywhere in the small and large bowel, 80% of these obstructions mechanically are occurring within the small bowel. 00:48 On the other hand, large bowel obstruction, it's going to be 20% of all intestinal obstructions. 00:54 It is the initial presentation in about a third of cases of colorectal cancer and the average age of presentation, particularly, when it's malignant is going to be slightly older or 70 years. 01:07 The pathophysiology. So, the reasons why there's obstruction of bowel, small or large, it's a long list. 01:14 And you may not want to just memorize it but just think about, well, how can the bowel become obstructed? For small bowel obstruction, we're going to talk about mechanical causes and functional causes. 01:26 So, mechanical means that there's something actually that we can put our hands around and say, "That's why it happened." Functional means the bowel is just not moving and that can be a source of obstruction as well. 01:39 For mechanical obstruction of the small bowel adhesions due to prior intraabdominal surgeries, are far and away the most common. 01:46 But tumors and metastatic tumor from other places seeding into the bowel or involving parts of the bowel mesentery may be a reason. 01:56 Hernias, so, outpouchings in various areas, abdominal ventral hernias can be a cause, Crohn's disease because it causes strictures as there's inflammation and scarring. 02:08 Gallstones that actually physically occlude the lumen. 02:13 Volvulus which is a separate talk elsewhere but volvulus of the small bowel is a twisting of the bowel on its pedicle and you're literally tying the small bowel in knots. 02:25 Intussusception, also covered in a different talk is where the bowel is like a telescope and the proximal bowel goes into the distal bowel. 02:36 Or you can have a foreign body ingestion, just a large bit of hair as a bezoar can be a reason to have a mechanical small bowel obstruction. 02:46 I said that there was mechanical. There's also functional. 02:49 So, the term ileus in quotes there refers to a lack of intestinal muscle contraction. 02:55 This is a normal consequence of most abdominal surgeries and is usually transient. 03:00 But inflammation of the peritoneal cavity, peritonitis, trauma, intestinal ischemia, a host of medications, even electrolyte abnormalities, acidosis and hypokalemia can be causes for ileus. 03:16 If you're trying to remember one of the most common cause for small bowel obstruction, SBO, here are your ABC's. 03:24 Adhesions, number one, fibrous bands from one part of the peritoneum to the other that catch up the bowel and literally, allow us to have a volvulus. Bulges or hernias and cancer, neoplasms. 03:40 And again, it's not going to be a small bowel primary cancer but metastatic cancer that involves the serosa or the vasculature of the small bowel. 03:51 Those are your ABC's of most common small bowel obstruction. 03:56 Let's switch gears and talk about large bowel obstruction. 03:58 And again, two flavors, one is mechanical and one is going to be functional. 04:02 Of the mechanical causes of large bowel obstruction, the most common is going to be colorectal cancer. 04:07 Remember, that's about a third of the presentations of colorectal cancer are obstruction. 04:14 Metastatic cancer, ovarian, pancreatic, lymphoma, almost any cancer that wants to go to the large bowel and all of them can, can lead to a large bowel obstruction. 04:24 In a separate talk, we've already mentioned the volvulus that can involve the colon. 04:30 Sigmoid colon being far and away the most common site of volvulus in the colon, sigmoid. 04:37 Cecal volvulus is more common in women but is much less common than the sigmoid volvulus. 04:45 And volvulus is the most common benign cause of a small bowel - the most common benign cause of a large bowel obstruction. 04:45 And volvulus is the most common benign cause of a large bowel obstruction. 04:50 And then, strictures. Areas where we have fibrosis due to scarring, perhaps, old inflammatory bowel disease, etc. 04:58 That's mechanical. Functional large bowel obstruction is also, can be also called ileus even though it's not in the ileum, this is ileus refers to lack of intestinal muscle contraction. 05:11 It's really a pseudo obstruction and in some other areas in your textbooks, you may see this referred to as Ogilvie's syndrome. 05:20 Any of a variety of causes including surgery, severe systemic illness, trauma, spinal anesthesia can all lead to functional bowel obstruction just not having any peristalsis. 05:34 In the vast majority of cases, this will be transient and if you correct the original problem, severe systemic illness, say, sepsis, then, the bowel will wake up and go about its normal peristaltic process. 05:50 What is going on in kind of a pathophysiologic level? Well, when the bowel is obstructed, then, everything that's coming from above just keeps coming, food, water, saliva, normal turnover of bowel epithelium, any secretions that come will continue to come and you'll have accumulation, not only of those kind of liquid and solid materials but also of swallowed air. 06:17 That's proximal to the area of obstruction. That accumulation is now compounded by the fact that bacteria there are happily fermenting everything that's not going any further. 06:30 We have an area of stasis and the bacteria will also contribute to air and we'll get a massive dilation. 06:39 Intraluminal pressure will go way up. As that happens, we are putting increased pressure on the bowel wall. 06:45 So, now, it's hard to get vascular flow into the bowel wall. 06:49 The arterial blood pressure can actually be exceeded by the increased intraluminal pressure. 06:54 This is compounded by now the inflammation that is going to be occurring with the compromised blood supply in ischemia and we will have edema and transudation of fluid in the lumen, exacerbating the entire situation. 07:07 When we finally get compromised arterial flow to the point that we get ischemia or infarction, now, we will have perforation, we will have peritonitis. So, that's what's going on when we have an obstruction. 07:21 The clinical presentation kind of follows from the pathophysiology and all of these are non-specific findings. 07:29 They can occur for a variety of other reasons but are associated also with bowel obstruction. 07:35 So, pain and distension, nausea and vomiting, constipation. You're not moving stool to get out. 07:41 If you have bleeding because of ischemia, you may have melena, blood in the stool. 07:47 Clearly, the patient is not going to be able to eat. They're not going to feel like eating or drinking and will be losing fluids into the GI tract, so, there'll be dehydration. 07:56 If there is ischemia and infarction, there'll be fever. 08:00 The bowel sounds, it's very - I mean, you put a normal stethoscope on someone's abdomen and if they're normal, you'll hear gurgling. 08:07 When you hear nothing, it sounds scary. And as the bowel distends, it may become tympanic. 08:15 So, if you percuss over the surface of the bowel, it will sound like a drum. 08:20 If that distended area is filled with fluid, it may sound dull. 08:26 The diagnosis. So, the diagnosis is going to be a clinical history and a sufficiently high suspicion of what's going on. 08:32 You're going to want to evaluate electrolytes to make sure that you correct acidosis and any other sodium, calcium, potassium, chloride, etc. abnormalities. 08:42 We will expect to see elevator renal parameters, particularly, in patients who are dehydrated. 08:46 As we get ischemia and infarction, we will expect to see lactic acidosis. 08:52 There will be leukocytosis in that setting as well with an elevated white blood cell count and in that being predominantly neutrophils. If there's bleeding that's been going on chronically, we may have anemia and in the setting of tumors being a cause for the obstruction, we may see elevated levels of tumor biomarkers such as carcinoembryonic antigen or cancer antigen 19. 09:13 On x-ray, we're going to see air fluid levels and dilation of the proximal segment of the bowel that has been obstructed. 09:21 And in most cases, we won't see any air in the colon. The obstruction has occurred someplace more proximal. 09:29 Normal bowel should have some air scattered throughout all segments including the colon. 09:35 If there's a large bowel obstruction, we may have as you see on the far right-hand side, a completely dilated lumen with or without air fluid levels. There may be not any fluid in there. 09:47 How do we manage this? So, the medical management for a functional obstruction. 09:51 This is not mechanical but functional. IV hydration to make sure the patient is tanked up and has adequate blood pressure. 09:58 Correction of any abnormalities of electrolytes. Put the bowel at rest. We're not going to allow them to eat. 10:04 You will put in an NG tube and probably do a decompression of the stomach. Nothing by mouth, nil per os and that is NPO. 10:14 And then, empiric antibiotics if you're really worried that there is ischemia or perforation. 10:19 For mechanical obstruction, we need to remove that obstruction. 10:23 That may involve endoscopy to pull out something that's in there or it may involve ultimately, depending on the cause, whether it is a tumor, where it is an adhesion, we may have to have a surgical intervention. 10:38 With that, we've covered the various aspects of a bowel obstruction.
About the Lecture
The lecture Bowel Obstruction by Richard Mitchell, MD, PhD is from the course Small and Large Intestines Disorders.
Included Quiz Questions
What percentage of colorectal cancer cases present with large bowel obstruction?
- 30%
- 15%
- 80%
- 50%
- 5%
What is the most common cause of small bowel obstruction?
- Adhesion
- Tumor
- Hernia
- Gallstone
- Volvulus
What is the most common cause of large bowel obstruction?
- Colorectal cancer
- Volvulus
- Stricture
- Ileus
- Pseudo-obstruction
Which is NOT part of the active processes leading to perforation from bowel obstruction?
- Hernia
- Bacterial fermentation
- Accumulation of products
- Compromised blood flow
- Increased intraluminal pressure
Which is NOT a finding of bowel obstruction?
- Murphy sign
- Melena
- Dehydration
- Decreased bowel sounds
- Tympany
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |