Playlist
Show Playlist
Hide Playlist
Bone Metabolism Case: 68-year-old Woman with High Serum Calcium Level
-
Slides Calcium Metabolis.pdf
-
Reference List Endocrinology.pdf
-
Reference List Metabolic Bone Disorders.pdf
-
Download Lecture Overview
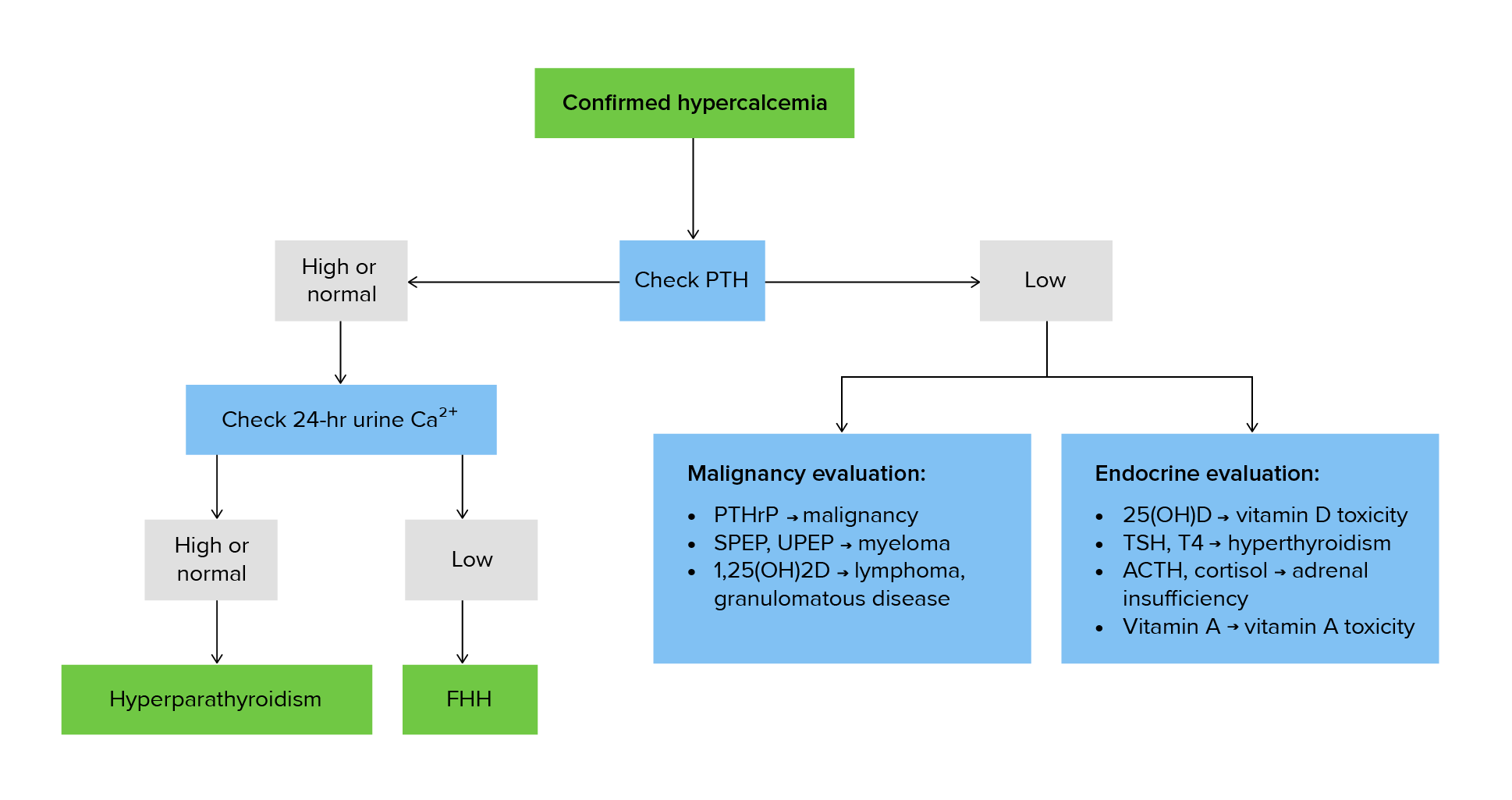
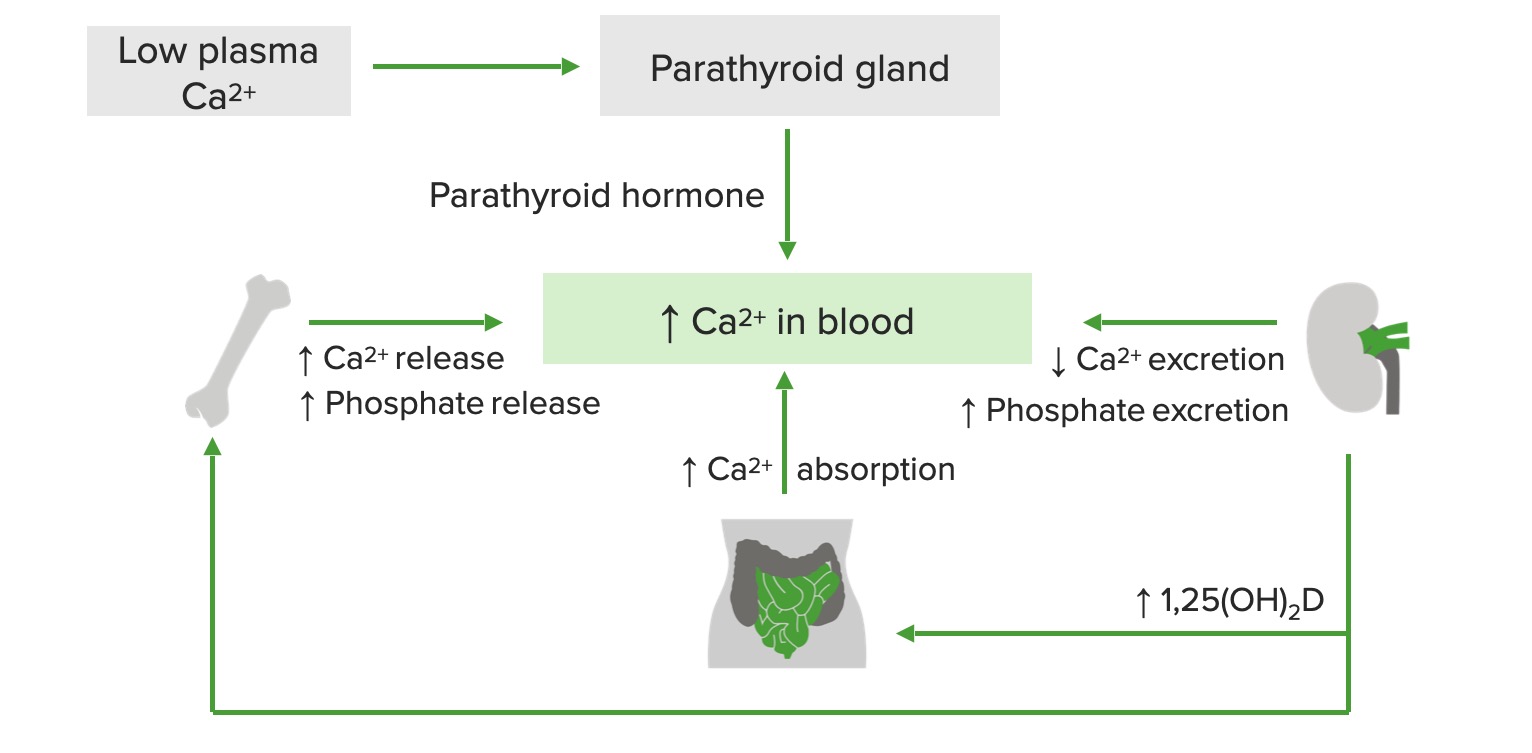
00:01 Let's go on to a case. 00:03 On routine exam, a 68-year old female patient is discovered to have a serum calcium level of 11.5 mg/dL. 00:11 Follow up lab test show an elevated PTH level with a low serum phosphorus and mildly elevated alkaline phosphatase. 00:20 24-hour urine calcium level is elevated. 00:23 Review of symptoms includes complaints of fatigue, constipation, diffuse bone pain for which she has been taking vitamin D. 00:32 Past medical history is significant for type 2 diabetes mellitus for 25 years and essential hypertension for around 15 years. 00:40 The patient has a history of kidney stones. 00:43 The family history is unremarkable. 00:46 What is the most likely diagnosis and what should you do next? Here we have an incidentally discovered elevated calcium level. 00:54 When a more in-depth history is taken and the systems are reviewed, we appear to have the classic symptoms of stones, bones, abdominal groans but no psychiatric overtones. 01:09 In association with an increase serum calcium, she has also elevated parathyroid hormone levels, a low serum phosphorus and an increased alkaline phosphatase. 01:18 She also has increased urinary secretion of calcium. 01:22 The conclusion here that this constellation of symptoms and signs, presentation of hypercalcemia with the association of low phosphorus, high calcium and elevated PTH is classic for the diagnosis of primary hyperparathyroidism. 01:40 Let's talk a little bit about primary hyperparathyroidism. 01:43 Repeat measurements of calcium and PTH should be confirmed to make the diagnosis. 01:47 The serum phosphorus level may be low or in the lower range of normal. 01:52 We should also check a 25-hydroxyvitamin D level because decreased vitamin D may lead to a compensatory increase in PTH and worsen the condition. 02:03 It certainly doesn't help in this patient that she's taking vitamin D supplementation as well. 02:09 Urinary calcium measurement should be performed with the 24-hour measurement of urinary calcium to differentiate primary hyperparathyroidism from the much rarer familial hypocalciuric hypercalcemia. 02:22 And we'll review this at the end of the section in a table.
About the Lecture
The lecture Bone Metabolism Case: 68-year-old Woman with High Serum Calcium Level by Michael Lazarus, MD is from the course Metabolic Bone Disorders.
Included Quiz Questions
A 65-year-old woman presents with complaints of fatigue and constipation. Her serum calcium level is 11.5mg/dL (2.87 ml/L) [normal range: 8.4–10.2mg/dL; 2.1–2.6 mmol/L]. What other associated findings in this patient would most likely be expected with this condition? Select all that apply.
- Renal calculi
- Low 24-hour urine calcium level
- Type 2 diabetes
- Low serum phosphorus
- Bone pain
What test should be performed in a patient with asymptomatic hypercalcemia to confirm the diagnosis of primary hyperparathyroidism? Select all that apply
- Repeat calcium level
- Urinalysis
- Ultrasonography of the thyroid gland
- Serum parathyroid hormone
- Serum 25-hydroxyvitamin D
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |