Playlist
Show Playlist
Hide Playlist
Barrett Esophagus with Case
-
Slides Gastroenterology 05 Esophageal Diseases.pdf
-
Reference List Gastroenterology.pdf
-
Download Lecture Overview
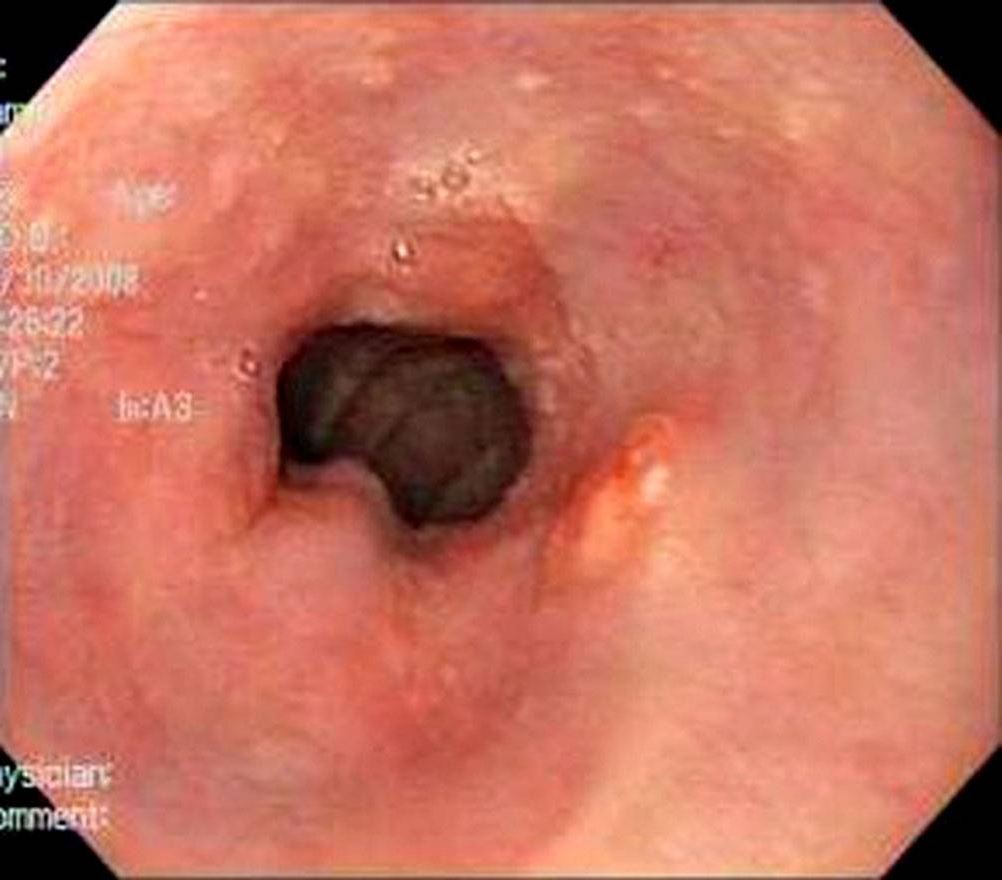
00:01 We'll move on to our next case. We have 73-year-old man seen in clinic for follow-up of his GERD. 00:07 He has had heartburn for the last 15 years. 00:10 Previously well controlled on pantoprazole. 00:12 In the last few weeks, he has noticed worsened symptoms and a sour taste in his mouth despite taking his pantoprazole as directed. 00:20 He has no dysphagia, weight loss, or vomiting. Vitals are normal. 00:25 Exam is unremarkable. 00:26 His upper endoscopy shows a small hiatal hernia and dark, pink-colored mucosa in the distal esophagus. 00:33 Biopsies are taken that show columnar epithelium with high-grade dysplasia. 00:39 So what is the best next step in management? Let's look at some key features here. 00:44 He has longstanding GERD for the last 15 years, he has worsening symptoms despite appropriate therapy, and luckily, he has no alarm symptoms of dysphagia, weight loss, or vomiting. 00:58 However, his endoscopy has some suspicious findings on it that we'll talk about in a bit. 01:04 So let's talk about Barret esophagus. 01:08 This is when normal squamous epithelium in the distal esophagus is replaced by a metaplastic columnar epithelium. 01:16 It often has this gross appearance on endoscopy showing here at the right where you can see a clear transition between salmon-colored mucosa to the normal esophageal mucosa. 01:27 Some of the risk factors include older age, male gender, white ethnicity, GERD, hiatal hernias, obesity, and smoking. 01:38 This an important condition to recognize because it is pre-malignant that has a small per year risk of progressing to esophageal adenocarcinoma. 01:49 The diagnosis must be made by upper endoscopy and then taking biopsies to examine histology. 01:56 Treatment is with a twice-daily proton pump inhibitor and if the patient has high-grade dysplasia on their biopsy performing endoscopic ablation. 02:07 So now we'll go back to our case. 02:11 We have a 73-year-old man with longstanding GERD, worsening symptoms despite appropriate therapy, no alarm symptoms, but these suspicious findings on his endoscopy. 02:22 So this appearance of pink-colored mucosa in the distal esophagus with columnar epithelium should prompt you to think of Barret esophagus. 02:32 Because he has high-grade dysplasia, the best next step involves endoscopic ablation to prevent progression to cancer.
About the Lecture
The lecture Barrett Esophagus with Case by Kelley Chuang, MD is from the course Disorders of the Esophagus and the Stomach.
Included Quiz Questions
Which of the following is the best treatment strategy for Barrett's esophagus with high-grade dysplasia?
- Endoscopic ablation
- Proton pump inhibitors
- H2 inhibitors
- Chemotherapy
- Surgery
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |