Playlist
Show Playlist
Hide Playlist
When Babies Stop Breathing: ALTE, BRUE and SIDS
-
Slides ALTBRUESID Pediatrics.pdf
-
Download Lecture Overview
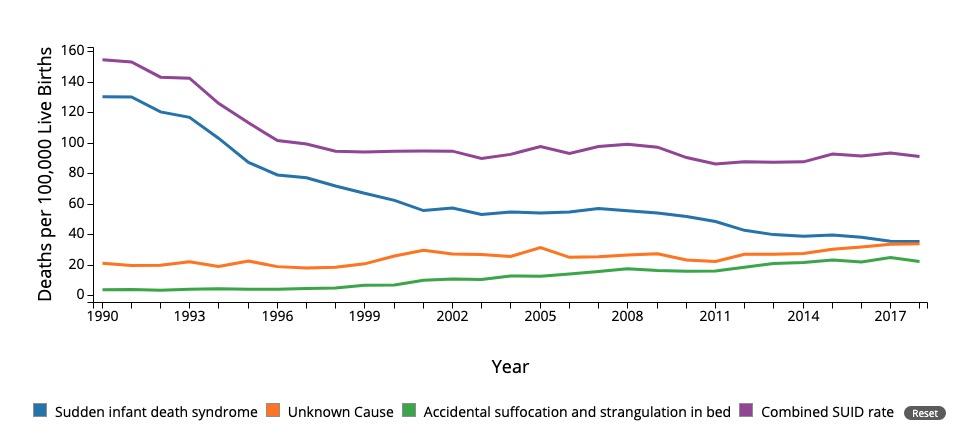
00:01 So in this lecture, we’ll review what to do when babies come in and the parents say, “My baby stopped breathing.” This is so incredibly common and yet can be caused by so many different things, but the vast majority, it’s no big deal. 00:17 So figuring this out can be very confusing. 00:20 I’ll briefly review what an ALTE is, although that word has now been replaced by a BRUE and I will also talk about SIDS or sudden infant death syndrome. 00:30 Sp let’s get through the terminology. 00:33 ALTE stands for apparent life-threatening event. 00:36 This is what we call it when the patient came in, a baby came in and parents say, “Oh, my baby stopped breathing and turned blue.” And so you’ll just say, “Okay, this is an ALTE.” We got rid of the word ALTE because the concern was that parents were misinterpreting the phrase life-threatening as actually life-threatening. 00:56 The whole point is ALTEs were not life-threatening. 01:00 So they’ve replaced this with the term brief resolved unexplained event, which is now the term we use and describe these events, although the definitions are slightly different between ALTE and BRUE and I’ll get into that. 01:14 And then SIDS is sudden infant death syndrome, that’s what we used to think was associated with ALTEs and BRUEs, but in fact is not. 01:22 So we’ll talk about that separately. 01:25 First let’s start about ALTE. 01:27 ALTE was defined in 1986 as an episode that is frightening to the observer and it had to last for more than 20 seconds. 01:35 Remember, young babies will hold their breath frequently for up to 20 seconds and that’s normal. 01:41 They had to have a change in color and they have marked in muscle tone, usually they go floppy. 01:47 They have a choking episode and they have gagging or something along those lines and then it was defined as an ALTE. 01:54 And then we would say, “Your baby had an apparent life-threatening event” and the parent would only hear life-threatening and they are very scared. 02:00 Well, in fact, the vast majority of time, these are not at all life-threatening and they are almost normal baby behavior. 02:08 So we’ve changed the ALTE to BRUE. 02:12 A BRUE is a brief resolved unexplained event and we put this out in a guideline in 2016. 02:20 So brief means it lasted less than one minute. 02:24 Resolved means the child has now returned to baseline. 02:27 They have normal vital signs. 02:29 They have normal appearance. 02:30 It was an event, it’s over. 02:32 Unexplained means there is no other diagnosis to explain this. 02:36 If they had this because they had bronchiolitis or pneumonia, well it was bronchiolitis or pneumonia that caused the problem. 02:43 And event, it had to be an event and the event had to include pallor or cyanosis, absent or decreased breathing, a change in tone, and altered responsiveness. 02:55 If a child meets these criteria, they had a BRUE. 03:00 So we used to think of these entities like this. 03:05 Before the invention of the word BRUE, we thought, “Well jeez, some of these who have ALTE may go on develop SIDS or sudden infant death syndrome.” In fact, in the 1970s, we might have called it pre-SIDS. 03:18 It turns out there is no connection or whatsoever between ALTEs and SIDS. 03:23 This is really what it is, babies who have ALTE and babies who have SIDS. 03:29 Well, of course, a baby who had SIDS might have an ALTE, but in general, if your babies had an ALTE and my baby hasn’t, the risk of SIDS has nothing to do with the ALTE, it has to do whether we’re smoking or whether the baby has good sleep hygiene, et cetera. 03:45 Babies who have a BRUE are subset of the babies who we would previously have called an ALTE. 03:52 For example, a baby with bronchiolitis who held their breath would previously have been considered to have an ALTE caused by bronchiolitis, whereas now that baby is not having a BRUE, that’s just bronchiolitis. 04:05 Okay. 04:06 So what are some diagnoses that can cause a BRUE? Well, it turns out there are thousands of diagnoses that can cause this problem. 04:17 So we have to be thoughtful about what do you think is going on with this patient that might be putting this child at risk or was this just a normal baby doing baby-like things. 04:30 So how do we do this? When the vast majority of these kids are normal, how do we rule out literally hundreds of diagnoses? Okay, here’s an example of a case we might see. 04:42 An infant comes in who is three weeks old. 04:45 There is no significant pregnancy or birth history. 04:48 The child has a strong history of spitting up after feeds and has Sandifer sign. 04:54 Remember from our GI lectures, Sandifer sign is when babies arch their back and turn their head to their side as a response to refluxing acid. 05:03 So the parents were at home and the baby had just fed and then he arched his back and his eyes bulged and he turned blue around the mouth. 05:11 Mom patted him on the back and he started breathing again, but the episode lasted for way too long. 05:17 She was terrified, maybe 45 seconds, so she came rushing into the emergency room because she is afraid something is wrong with her baby. 05:26 We see this all the time. 05:28 So does reflux, which this baby clearly have, cause apnea in babies? Good question. 05:37 So they did a retrospective study of 119 premature infants who had ALTE. 05:43 This study was done when we are using the word ALTE and they measured 6,000 episodes of reflux with a polysomnography which is lots of probes measuring respiratory rate and airflow with the nose and heart rate and pulse ox and they also did a pH probe which could measure acid coming up the esophagus inside. 06:04 And what this showed is that 1% of infants had a reflux episode that was associated with holding their breath more than 15 seconds. 06:13 So I said, "Oh, look, there were some infants who had a refluxy episode and they held their breath." The problem was that a third of those cases, they held their breath and then had the refluxy episode. 06:27 So that is not clear that this causes a problem, it may be that babies hold their breath and then they reflux. 06:36 That said, we see this so commonly, many of us are fairly confident that reflux can cause babies to hold their breath. 06:45 So maybe we should treat these infants for reflux, prevent them from holding their breath again. 06:51 The answer is probably not. 06:54 So blocking stomach acid in babies increases risk of pneumonia six folds, increases the risk of gastroenteritis two folds, increases the risk of C. diff infections and increases the risk in tiny babies of necrotizing enterocolitis. 07:11 So if blocking acid is bad, we have to ask ourselves, was this event so significant that this child really needs to go on, say, a proton pump inhibitor when there’s a risk? But remember, these infants are not at increased risk for something like death from holding their breath. 07:31 So oftentimes, we will try other tricks in terms of helping them with reflux. 07:36 We will say, "How about we thicken the feeds in severe cases?" This can reduce reflux events without adding acid blockade, however, thicken the feed does cause infantile obesity which can in turn increases risk of adult onset diabetes. 07:53 So we only want to thicken the feeds in very severe cases. 07:57 Most of the time, we recommend positioning tricks which probably don’t work, but more commonly what we recommend is smaller feeds more frequently. 08:07 That may be all this child needs and good burping. 08:11 Okay, let’s do another case. 08:13 An infant is five months old and comes in with two weeks of upper respiratory infection symptoms. 08:19 There have been worsening cough, it’s worse at night and then last night or tonight, there was an episode where the baby was coughing and arched his back and his eyes bulged and he turned blue around the mouth. 08:30 And it lasted 45 seconds and mom was terrified and she rushed into the emergency room. 08:35 He’s all better now. 08:38 Well one thing we have to worry about is pertussis. 08:41 Pertussis causes infants to die from coughing episodes. 08:46 In adults, it just causes prolonged cough but in infants, it can actually cause death. 08:52 Children and in infants with pertussis can have feeding difficulties, tachypnea, cough and gagging. 08:58 It is not associated with fever. 09:00 These infants lack the whoop from the whooping cough because they lack a respiratory musculature that helps them breath in quickly. 09:09 They may appear very well and have sudden paroxysmal cough and apnea and cyanosis is typical in infants under six months of age. 09:19 So infants may become apneic or have cyanosis as often as 15-30% of the time when they get pertussis. 09:28 So, we need to make sure this infant doesn’t have pertussis, if the story is consistent with that. 09:34 Certainly, if somebody else in the family has been coughing for a long time and this infant has predominantly cough, we will probably check them for pertussis. 09:42 That said, treating pertussis doesn’t make the child get better, so we often hospitalize these children and watch them for signs of worsening respiratory status and once they are deemed to be stable, they might be sent home. 09:56 Here’s what is happening with the United States right now in terms of rates of pertussis. 10:00 You can see at the beginning of this chart, there was high rate of pertussis and in around 1948, the pertussis vaccine was introduced. 10:10 And you can see there was a dramatic reduction in rates of pertussis which were caused, which saved countless lives and this vaccine was working really great until about the year 2000 and now, we’re starting to have an upswing. 10:25 This upswing is mostly because the strains of pertussis seemed to be changing. 10:30 We probably need to reorganize our vaccine, but that said, we are now seeing outbreaks of pertussis. 10:38 So if you see case of pertussis, you have to report it because we can control spreads through azithromycin. 10:44 That doesn’t help the patient but it controls spread maybe and that way, we can limit the extent and the spread of the disease. 10:52 Another more common cause of apnea in infants is just plain old bronchiolitis. 10:57 This is a viral infection of the lower airways of children and they frequently causes infants to have an apneic episode. 11:06 Okay. 11:06 Here’s another case, a five-week-old was afebrile and had no URI symptoms, this is not bronchiolitis. 11:14 The brother died suddenly as an infant of an unknown cause, so the family is scared of SIDS and tonight, there was an episode where the baby was acting normally and then became completely limp and turned blue around the mouth. 11:27 Mom patted on the back, he started breathing, called 911, and she was terrified. 11:33 This is very concerning. 11:35 We’ve got a problem here. 11:36 There’s a history of SIDS in the family, may be there’s a genetic problem and this baby wasn’t really doing something where we can explain why this child suddenly became limp. 11:48 We're worried in this case perhaps of cardiac causes of apnea in children. 11:53 So around 2% in infants who have an apneic event may have a cardiac cause, it’s more common in those children with known structural heart disease or structural heart disease that is obvious on exam. 12:06 So realistically, when you examined this child, if you hear a wild whopping murmur, chances are this is a cardiac cause. 12:13 If you notice nothing on exam, it’s unlikely this is cardiac. 12:17 But in this case, we might worry about an arrhythmia. 12:22 Arrhythmias, SVT is the most common and sometimes in families, they can have a gene which causes a prolonged QT interval. 12:33 This can present in patients and families, especially in patients with deafness, they can have Jervell and Lange-Nielsen syndrome or they may have Romano-Ward which is a little more common and is not associated with deafness. 12:45 If you’re worried about a prolonged QT, you want to get an EKG to check and check that QT interval and also look for other signs. 12:54 If the EKG is normal and the exam of that child is normal, and the child has been growing well, this is not cardiac disease causing this apneic episode. 13:04 Another diagnosis for this child is child abuse. 13:09 This is terrifying, but it’s true. 13:11 Between 2 and 11% of patients in two different studies with ALTE had it from undiagnosed child abuse. 13:20 You should think about subdural hematoma as a potential cause of altered mental status in a child. 13:28 And as you can see, this can be fairly common. 13:31 They don’t always have clear bruising about the head. 13:34 Sometimes, patients have shaken baby will have no external findings, but you only see it on a head CT such as this where you can see the blood is accruing in the subdural space. 13:48 So if a baby has one of these brief resolved unexplained events, what do you do? Okay, so the baby has a BRUE, you can find nothing on history and physical to explain it, then we’re going to risk stratify. 14:02 If the child is greater than 60 days, born after 32 weeks gestation so is not too premature, there was no CPR provided and lasted less than a minute and it was a first event, this child is low risk. 14:18 And with appropriate counseling and provision of CPR training, maybe as an outpatient, that child can probably be sent home. 14:25 So for low risk children, we probably don’t require labs or imaging. 14:30 They can be sent home with reassurance and we can refer them for CPR training. 14:35 As effective as live CPR trainings are CD sets that you can sell that will train people how to use CPR, and that is effective. 14:44 However, if they meet any of these criteria, they are high risk and we typically will admit these patients and watch them overnight. 14:52 We will do testing if something shows up on either history or physical or something happens overnight that cues us into underlying cause, one of those hundreds of causes we went through earlier. 15:05 And then, we will discharge them typically after 24 hours of observation if there is no clear cause, again, with CPR training. 15:13 Remember, multiple instances of ALTEs and/or BRUEs in children may be a sign of child abuse, so screen the parents also carefully. 15:23 How is it getting along with their child is really important question.
About the Lecture
The lecture When Babies Stop Breathing: ALTE, BRUE and SIDS by Brian Alverson, MD is from the course Pediatric Emergency Medicine.
Included Quiz Questions
The risk of which of the following has not been shown to increase with antacid medication in infants?
- Sudden infant death syndrome
- Pneumonia
- Gastroenteritis
- Clostridium difficile infection
- Necrotizing enterocolitis in premature infants
Which of the following is true regarding the term ALTE (apparent life-threatening event)?
- It has been replaced by new terminology.
- It requires extensive laboratory workup.
- It is recently introduced for brief nonconsequential events in infants.
- A brief period of cyanosis in a child with bronchiolitis is a typical example.
- Hypotonia does not fit into the definition.
According to the 2016 guideline by the American Academy of Pediatrics, which of the following falls under the definition of brief, resolved, unexplained event (BRUE)?
- Sudden cyanosis for 20 seconds in an otherwise healthy child
- Bronchiolitis with pallor and fever
- Hypotonic posture in a neonate with febrile fits
- Sudden pallor in a child presenting with diarrhea
- Decreased level of responsiveness for 10 minutes
Which of the following groups of antibiotics is used as primary agents in the treatment and prevention of pertussis?
- Macrolides
- Cephalosporins
- Tetracyclines
- Quinolones
- Sulfanamides
Which of the following is the most common form of congenital long QT syndrome?
- Romano-Ward syndrome
- Jervell and Lange-Nielsen syndrome
- Brugada syndrome
- Noonan syndrome
- VATER syndrome
A 3-month-old child born at 38 weeks gestation is diagnosed with a 1st episode of BRUE (brief, resolved, unexplained event). Which of the following is the most appropriate next step in management?
- Refer for CPR training and send home.
- Do chest imaging including echocardiography.
- Admit the baby to the hospital.
- Perform extensive laboratory workup and electrocardiography
- Perform brain CT
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |