Playlist
Show Playlist
Hide Playlist
Alcohol and Substance Use Disorders
-
Slides SubstanceUse ChronicCare.pdf
-
Download Lecture Overview
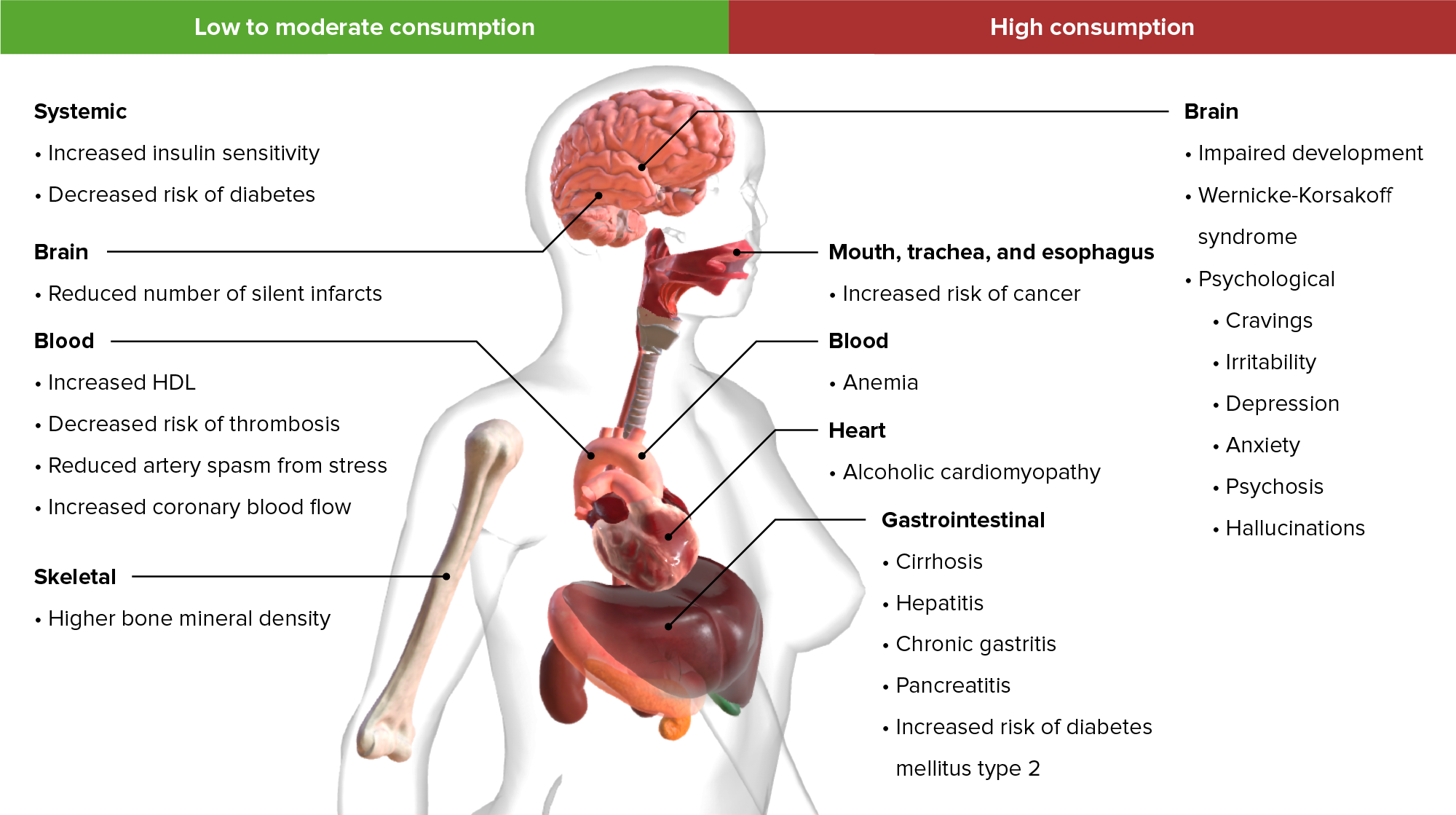
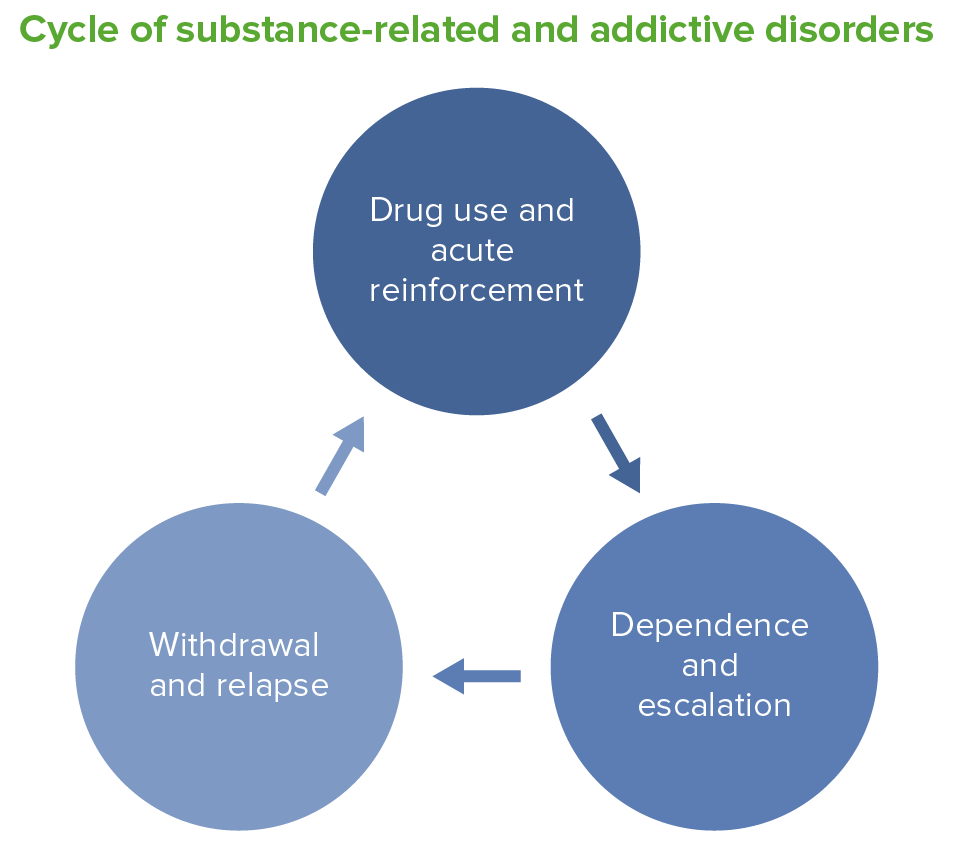
00:01 Okay. 00:01 Let's talk about something that may be difficult for patients to bring out and describe, but is critically important for their care and is also important for USMLE and that’s substance use disorders. 00:14 Let’s start with a little case here. 00:16 We’ve got a 19-year-old young man. 00:18 He’s here for his routine wellness visit. 00:20 And so, what does the United States Preventive Services Task Force recommends screening in him when we talk about potential substances for abuse. 00:31 Is it, A, marijuana or should we be screening for prescription drug abuse? How about screening for heroin use or alcohol use? USPSTF recommends only screening for alcohol use among these different substances. 00:47 So, let’s talk about alcohol use disorders. 00:49 They’re very common. 00:50 7% of American adults have some alcohol use disorder. 00:54 It’s the third leading preventable cause of death. 00:58 And so, therefore, we recommend screening for alcohol use and brief interventions for problem drinking. 01:06 Now, CDC has a pretty liberal definition of problem drinking. 01:10 So, men up to – should be drinking up to four drinks per day. 01:15 Other organizations would say that really two drinks per day is the maximum limit for men, but certainly five drinks a day would be too many and a total of 14 drinks per week. 01:28 Women have a more strict threshold because they don't have the alcohol dehydrogenase that men do, so therefore they should be drinking, at the maximum, three drinks per day. 01:39 But some organizations again would say, actually one drink per day should be the maximum for women and less than seven drinks per week. 01:49 All right. 01:50 So, what about treatment for alcohol use disorders? There are some medications available that you should be aware of in clinical practice before your exam. 01:58 Acamprosate and naltrexone are both more effective than placebo in improving alcohol use disorders and improving rates of abstinence from alcohol, with a pretty low number needed to treat. 02:11 I think that treatment of substance use disorders is a real challenge. 02:15 Rates of relapse in terms of drinking, smoking, whatever substance you’re talking about are fairly high. 02:20 So, a number needed to treat between 11 to 20 is fairly low. 02:25 Disulfiram is a classic drug that promotes a severe reaction in terms of nausea and vomiting when patients take alcohol after disulfiram, but that’s not been proven to be as effective. 02:38 So, really, these newer drugs – well, and naltrexone has been around a long time, just now used for alcohol use disorders. 02:45 They are better choices for patients. 02:48 Acamprosate requires three times a day dosing, whereas naltrexone is a little bit easier to take. 02:53 It’s daily. 02:54 Acamprosate should be avoided in severe renal illness, whereas naltrexone unfortunately shouldn't be used in hepatitis and cirrhosis, which is pertinent because so many patients with alcohol use disorders have hepatitis and cirrhosis. 03:07 And just keep in mind too that, while disulfiram and alcohol almost always equals nausea and vomiting, nausea and vomiting are still very common with both acamprosate and naltrexone too. 03:18 Those are the most common side effects. 03:22 So, for other substance use disorders, beyond tobacco and alcohol, there is no – there are no screening recommendations, even though we know that the use of substances among adolescents is fairly high. 03:35 Nearly half of 12th graders have used some illicit substances in the past year. 03:40 And then, overall, worldwide, over 22 million adolescents and adults have either substance abuse or substance dependence. 03:47 Terrible outcomes associated with substance use. 03:51 Let’s talk about marijuana use, and that's really undergone a revolution in the United States as the – there's been this wave of legalization across the country. 04:00 How has that affected use among adults? We see both rates of use and disorder going up. 04:07 And disorder means that the patients either have – they’re dependent upon marijuana or they’ve had some adverse reaction due to taking marijuana. 04:18 And the rates of both have gone up. 04:19 That’s due to the legalization. 04:21 Also due to the – and the increase in the disorder is probably due to the increased potency of today's marijuana versus the marijuana of 10 years ago or 10 years before that. 04:31 It’s generally a more potent product. 04:34 Interestingly though, in that same period, we’ve actually seen a stabilization of marijuana use among high school students and the use actually decreased during that legalization period between 1998 and 2013. 04:48 Still over 38% or so had tried marijuana. 04:54 Use before age 13 is a real problem because it's when it's used before age 15 that marijuana is associated with its worse effects on cognition and also as a gateway drug for other substances such as opiates and amphetamines. 05:11 And you can see the current use in the past month was about 22% among high school students. 05:19 Just to focus on adolescents for a minute because these really are to me a significant high risk group. 05:26 Substance use in this group tends to have longer-lasting, more durable and negative effects on health versus a use among adults. 05:36 So, alcohol use, most US adolescents had used alcohol in the past month. 05:41 Use of hallucinogens and ecstasy is still fairly rare, but, boy, watch prescription drugs. 05:47 That's the big riser, particularly in the past 10 years is that adolescents are using a lot more prescription drugs and misusing those drugs than previous. 05:57 This includes drugs, of course, like opiates, but also benzodiazepines and stimulant drugs too. 06:05 And it’s worth noting that the rates of prescription drug overdose during that period, certainly among adolescents, but this is among all US citizens, vastly outweigh those of illicit drug overdose. 06:19 So, it's much more – the emergency department sees a lot more prescription drug versus illicit drug overdose these days. 06:27 And that's a real shame and something we need to change. 06:32 So, one question that has excellent sensitivity in detecting substance abuse or misuse is how many times in the past year have you used an illegal drug or used a prescription medication for non-medical reasons. 06:45 You don't have a lot of time in clinical practice. 06:48 If you had to choose one question, this would be it. 06:52 Some advocate routine screening with urine testing for potential drugs for abuse, and that’s actually not recommended widely because it doesn't start the conversation the right way. 07:06 And it's not an enlistment of a partnership between patient and clinician. 07:11 So, I generally try to discourage use and national organizations do too. 07:17 In counseling subjects, when you find a substance use disorder, definitely you want to keep it objective, avoid judgment, use motivational interviewing techniques, help the patient understand how that substance may be standing as a barrier in their own lives, maybe it's related to their family or their social obligations, maybe it’s something related to school or work, but try to find what motivates them and then use that as a tool to help them to move towards abstinence, hopefully, or at least cutting back because the goal in general for substance abuse is abstinence, but now there's more of an acceptance of harm reduction techniques and a great example would be avoiding needle sharing among patients with IV drug abuse. 08:04 That's a critically important public health goal. 08:07 It’s going to reduce risks of hepatitis and HIV, but the goal for the individual patient is abstinence because drugs like heroin can ruin lives. 08:18 You have to commit to a long-term treatment regimen, and so this is not for somebody who's the casual user, these are for patients with a stronger history of opioid abuse. 08:29 But it’s something that can be initiated at home. 08:31 They don't have to be an inpatient to use it. 08:34 And using naloxone now has become more regular and given to patients in kits, such that they can – if there is a case of overdose related to the use of buprenorphine or when it's mixed with drugs, other opiates or heroin, then naloxone can be an absolute lifesaver in the field, particularly for low resource populations like homeless populations. 09:01 Methadone is an older drug, but still can be effective for those with chronic opioid addiction. 09:09 It reduces opioid abuse and the associated risk of harm such as overdose. 09:15 Naltrexone is generally less effective overall in terms of the prevention of opioid abuse in the long run. 09:25 It also has a risk of hepatotoxicity and requires routine monitoring of liver function tests, which can be hard in a population with a high use of substances just because follow-up can be erratic. 09:41 So, with that, that just walks you through some of the more common substances, things you might see on your examination as well as the treatment of substance abuse. 09:49 Hope it was helpful.
About the Lecture
The lecture Alcohol and Substance Use Disorders by Charles Vega, MD is from the course Chronic Care. It contains the following chapters:
- Substance Use Disorder
- Medical management of Opioid Abuse
Included Quiz Questions
How many alcohol drinks per week increase health risks in men < 65 years?
- More than 14
- More than 12
- More than 10
- More than 8
- More than 6
Which of the following medications are first-line medications for the treatment of most patients with alcohol abuse?
- Acamprosate and naltrexone
- Phentermine and naltrexone
- Methadone and acamprosate
- Methadone and disulfiram
- Topiramate and phentermine
What is the most commonly abused substance in the United States?
- Alcohol
- Prescription drugs
- Amphetamines
- Opioids
- Bath salts
Which of the following medications is most appropriate for the treatment of alcohol abuse in patients with liver failure?
- Acamprosate
- Naltrexone
- Methadone
- Disulfiram
- Topiramate
Screening for which of the following substances is most recommended in a time-limited primary care setting?
- Alcohol
- Marijuana
- Prescription opiates
- Prescription benzodiazepines
- Heroine
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |