Faculty Blog
Lecturio Pulse
Stay updated with our articles on evidence-based learning and teaching in health professions education written with educator needs and challenges in mind.
Latest Articles
Cutting-edge knowledge for medical educators
All Articles
Learning Science
Teaching Strategies
Education Leadership
All Articles

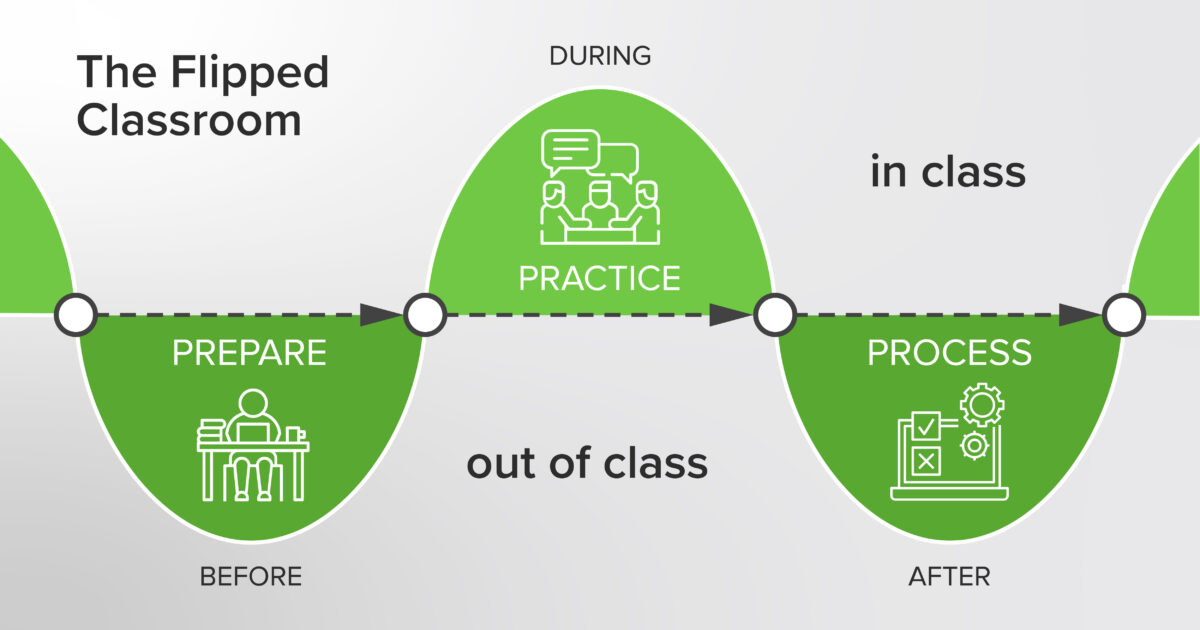
The Flipped Classroom in Medical Education: A Strategic Blueprint for Digital Transformation
Medical schools are undergoing a necessary digital transformation by adopting flipped classroom models to maximize clinical instruction time. This evidence-based approach uses expert-led digital content for foundational learning, freeing faculty to lead high-value clinical reasoning sessions. This guide offers a strategic blueprint for institutions to implement these modern pedagogical shifts efficiently while improving student performance and engagement.

2026 NCLEX-RN Changes: A Guide for Nursing Faculty
Starting April 1, 2026, the NCLEX-RN will introduce updated clinical expectations, including a focus on health equity and internal device monitoring, while maintaining its core content category weights.

From Passive Screens to Active Minds: This AAMC Faculty Toolkit Turns E-Learning Into Active Learning
Discover new ways to use AI and digital tools for active learning.

AI in Question Writing: Boost Productivity & Preserve Pedagogy
Discover how educators can use AI to streamline question writing, improve quality, and enhance student engagement, without losing human oversight.
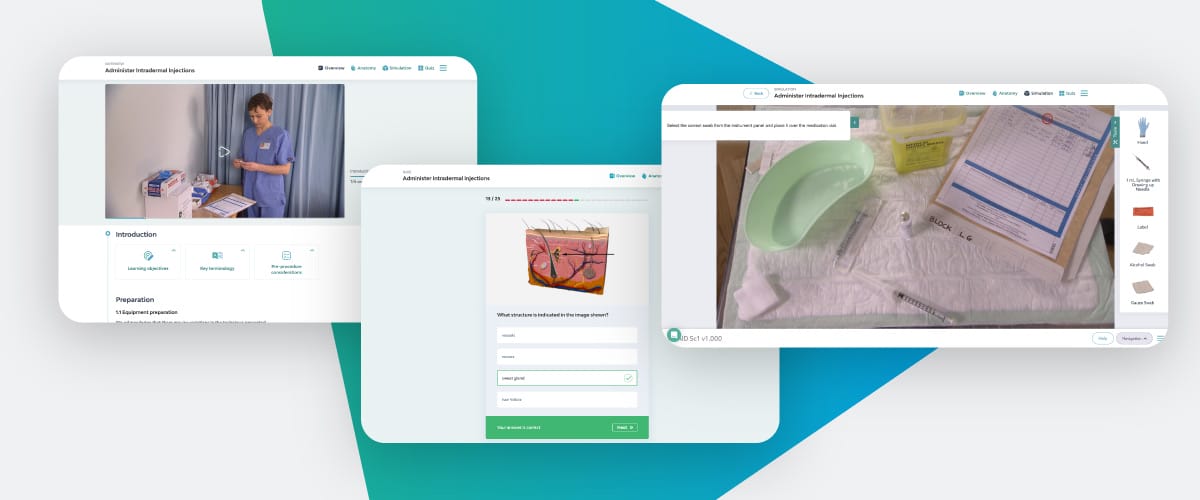
Simulation for Training: Transforming Medical and Nursing Education
Explore simulation in healthcare education. Learn the methods, benefits, and challenges of using simulation to train safer, more competent clinicians.
Lecturio Acquires SimTutor to Expand its Digital Healthcare Training Portfolio
Lecturio strengthens its global reach with new interactive, simulation-based learning solutions for healthcare professionals.

How Lecturio Supports the Remarkable Period of Growth in the PA Profession
Lecturio celebrates the hard work and expertise of PAs, and those who prepare them for practice, this PA Week.

Celebrating DOs on AACOM Advocacy Day 2025: How Lecturio Supports the Next Generation of Osteopathic Physicians
AACOM Advocacy Day is a yearly event where osteopathic deans, students, faculty, and advocates come together to speak up for the future of osteopathic medical education (OME).

HHS Nutrition Mandate September 10th Response Deadline: Lecturio Supports Medical Schools
An immediate solution to the Department of Health and Human Services’ mandate.
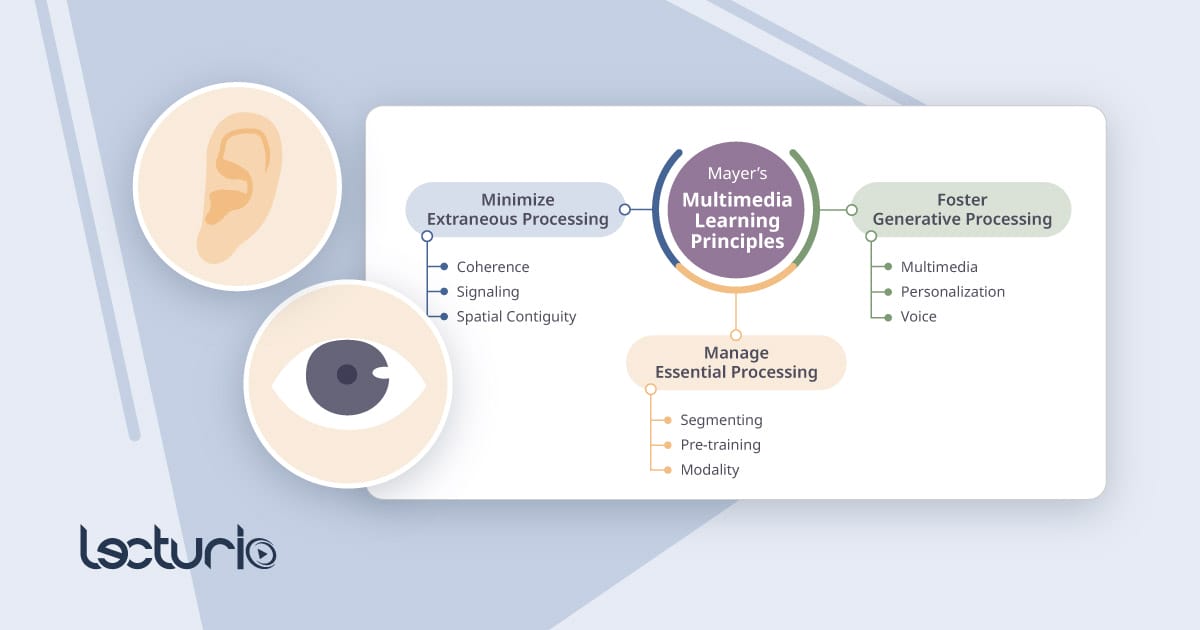
How Lecturio Videos Bring Mayer’s Multimedia Principles to Life
Discover how our platform videos are built on the latest developments in learning science.
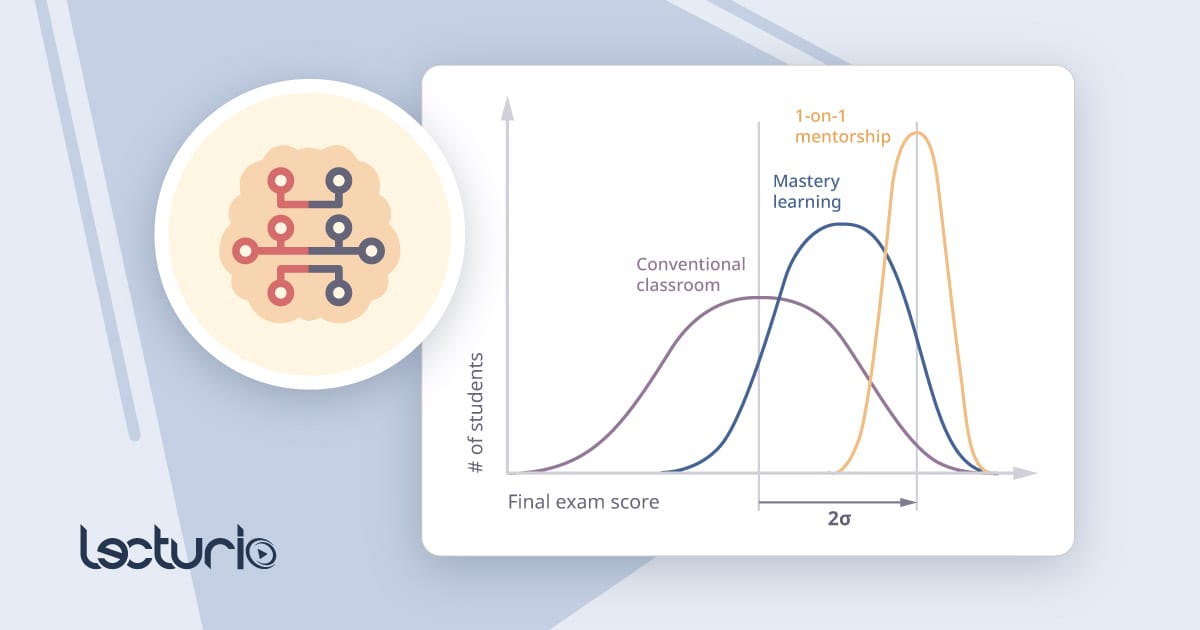
Solving Bloom’s 2 Sigma Problem with Lecturio’s New AI-Powered Learning Tools
In 1984, Bloom proved one-on-one tutoring could boost student performance to the top 2%. Lecturio’s new AI-powered tools bring that level of personalized learning to medical students at scale.

SpeakNursing: A Powerful Partnership for Clinical Fluency
This new tool developed by Carnegie Speech and Lecturio is designed to help nurses achieve fluency in clinical English.

Lecturio Pulse: World No Tobacco Day
Explore evidence-based material on drug use and disease management.

Lecturio and Sigma Theta Tau Announce Exclusive NCLEX Partnership to Empower the Next Generation of Nurses
Lecturio and Sigma Theta Tau, the world’s second-largest nursing organisation, have entered into an exclusive partnership.

Learning Science Leader: What you need to know about leadership in healthcare education
Learn how to promote the quality of education and clinical practice with effective leadership.
Lecturio AI Tools: Empowering Educators by Streamlining Workload
Discover Lecturio’s comprehensive suite of AI tools, designed to save time and ease faculty workload.

Lecturio Named One of TIME Magazine’s Top 25 EdTech Companies in the World
TIME and Statista have named 350 companies changing education, with Lecturio coming in at #23 in the global ranking.

New Advanced Qbank Feature for Nursing Educators
Discover Lecturio’s brand-new Qbank feature, which categorizes practice questions within our educator platform.

The Digital Transformation of Care: A New Era for Nursing Practice
View insights from the latest instalment of our Global Webinar Series with nurse futurist Dr. Bonnie Clipper.

Raising the Bar: South University’s Lecturio Success Story
Learn how South University (SouthU) implemented Lecturio in their nursing program to reduce faculty workload, improve student engagement, and increase certification exam outcomes.

Women in Medical Education: Leading Progress Amid Challenges
Read our latest Pulse newsletter on women in medical education, and how Lecturio is promoting their roles.

Teaching Clinical Reasoning and Clinical Judgment: Strategies for Medical and Nursing Educators
Learn effective strategies for teaching clinical reasoning and clinical judgment in health professions education.

Lecturio Acquires NEJM Healer in Major Expansion of Clinical Education Capabilities
Lecturio has acquired clinical reasoning education and assessment tool NEJM Healer from the New England Journal of Medicine (NEJM) Group.

How to Teach Pharmacology to Nursing Students
Learn to teach pharmacology with a free sample lesson plan from Rhonda Lawes PhD, RN from Oral Roberts University and Jacquelyn McMillian-Bohler, PhD, CNM from Duke University School of Nursing.
Bridging the Gap: Enhancing Nursing Student Success with Lecturio at ORU
Read how the integration of Lecturio into Dr. Valentz’s Pathophysiology nursing course at ORU changed the learning outcomes of students by overcoming the limitations of traditional methods and improving engagement and performance.

How to Teach Diversity in Nursing with Lecturio
A sample lesson plan based on the DEIB course taught by Angela Richard-Eaglin, DNP, MSN, FNP-BC, CNE, FAANP, CDE from Yale University and Jacquelyn McMillian-Bohler, PhD, CNM from Duke University School of Nursing.

Assessments: New Uses for an Old Tool
Educators and students alike often think of an assessment as the final stop on the path of learning. Our current understanding of cognitive and neuroscience has taught us, however, that assessments can be an invaluable learning tool as well as a means of evaluation. Properly designed and well-written assessments can determine mastery of material, grade or rank students, measure student progress, reinforce learning, motivate students, and provide feedback to instructors (1). Assessments include more than just written exams; they encompass any form of evaluation or appraisal of a student’s educational progress by formal or informal means.
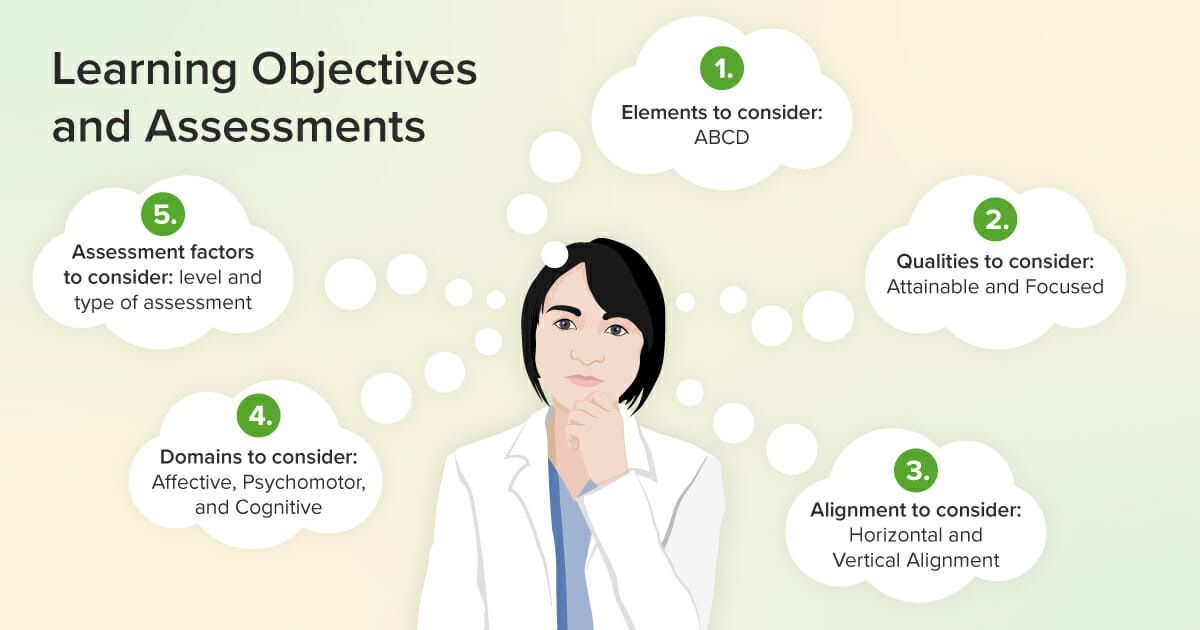
Learning Objectives and Assessments: Evidence-Based Recommendations for Optimal Efficacy [Incl. Seminar]
We can’t see learning happen, so how do we know it has occurred? Educators rely on observable behaviors as indicators of students’ skills, knowledge, and dispositions. Observable behaviors might include creating a concept map, demonstrating suturing skills, or communicating compassionately with patients. If a student could not successfully perform these before instruction and can perform them after, it is presumed learning has occurred. These desired observable behaviors are defined and communicated in learning objectives: concise statements of what a learner will be able to do as a result of instruction (1).
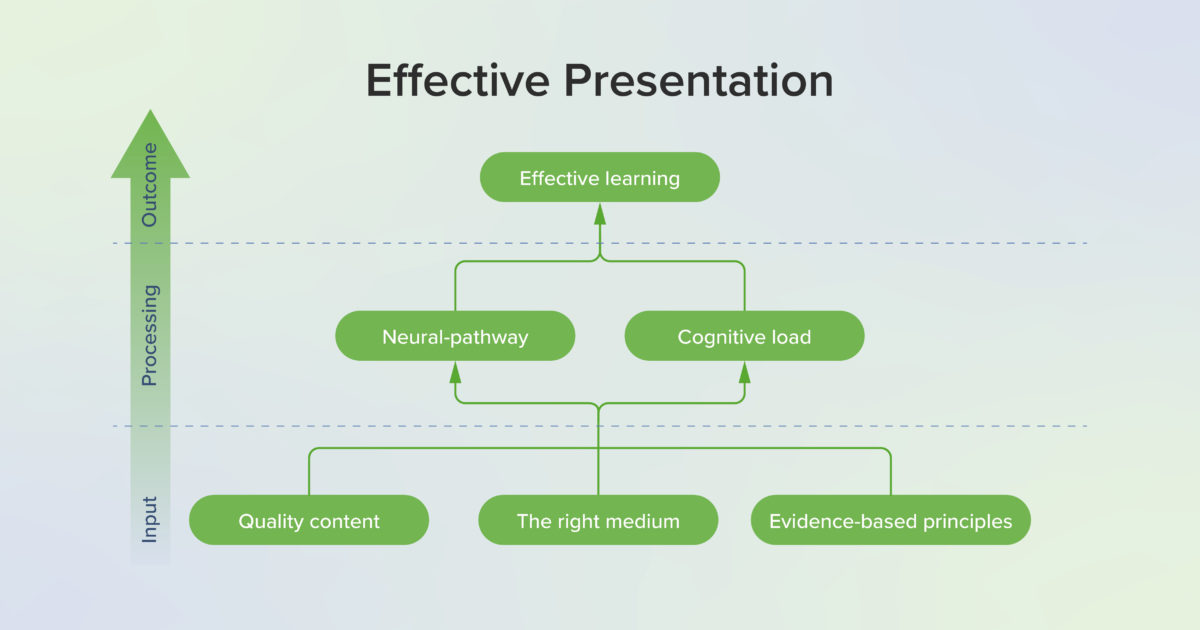
Effective Presentations: Optimize the Learning Experience With Evidence-Based Multimedia Principles [Incl. Seminar]
The purpose of this article is to introduce effective presentations, which have a set of key qualities: they are appealing, engaging, informative, and concise. Effective presentations gain attention and captivate the audience, but most importantly, they convey information and ideas memorably. Using evidence-based principles in educational multimedia can ensure the development of high-quality learning experiences. In fact, effective presentations have a set of core principles, a host of learner benefits, and a solid foundation in cognitive science. The article also explores the real-world implementation of effective presentations and share a practical application method that educators everywhere can use to develop effective multimedia in their classrooms.
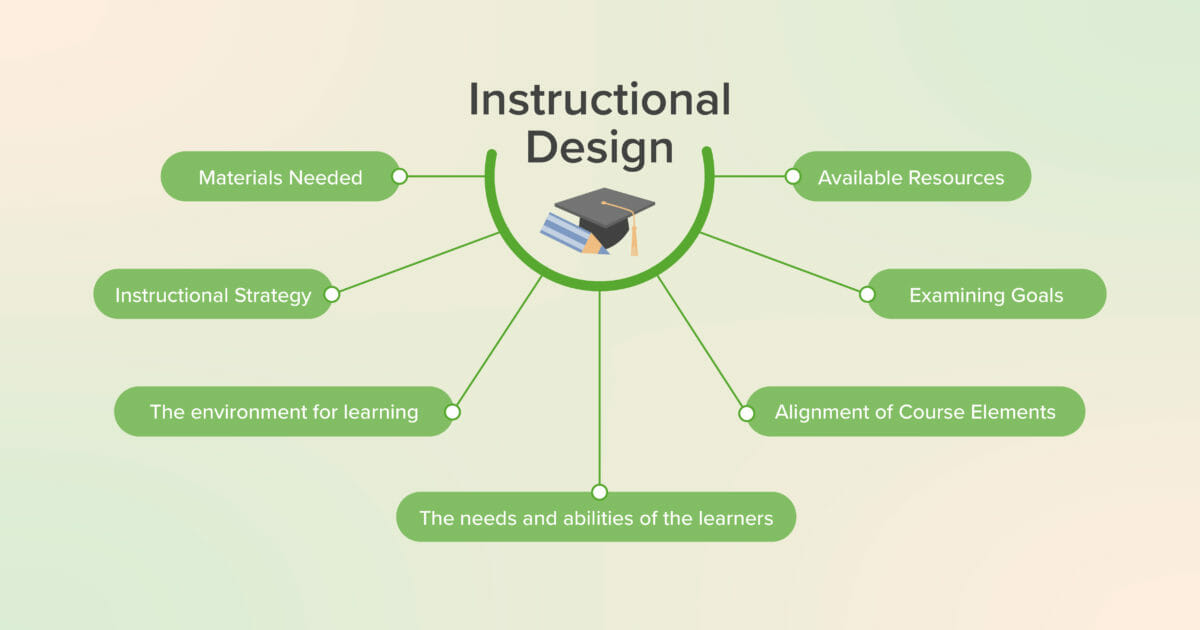
Instructional Design: How Best to Optimize the Learning Process [Incl. Seminar]
Learn about Instructional Design, its benefits, how it helps support the alignment and integration of instructional goals, activities, and resources, and a practical implementation method for daily education practices.

Metacognition in Education: Examples and Strategies
In this article, we explore a concept that has not gained a lot of attention in medical education: metacognition. We start by explaining what metacognition is and why it is relevant for educators and learners. We then dive deeper into the elements of metacognition in the classroom and provide concrete examples of how it can be incorporated by both students and educators.
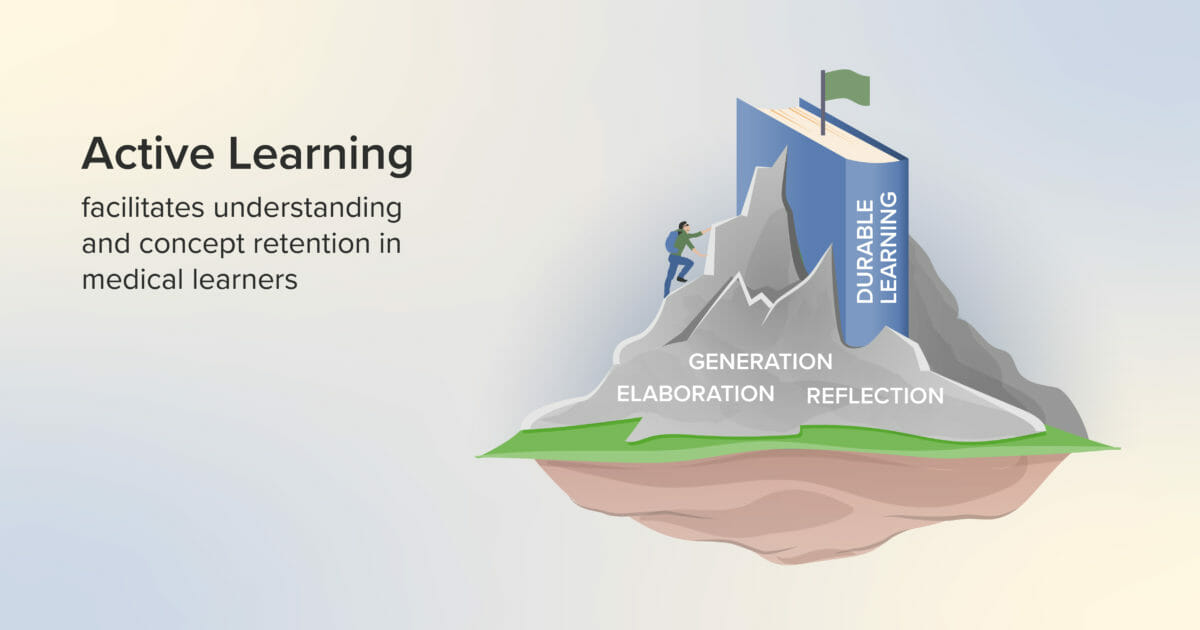
Active Learning Strategies to Improve Student Engagement in Medical Education
Helping students find a purposeful, productive, and effective way to learn is an important goal for medical educators. That goal can be advanced by the implementation of active learning: a set of evidence-supported educational tools that enhance student understanding and proficiency.
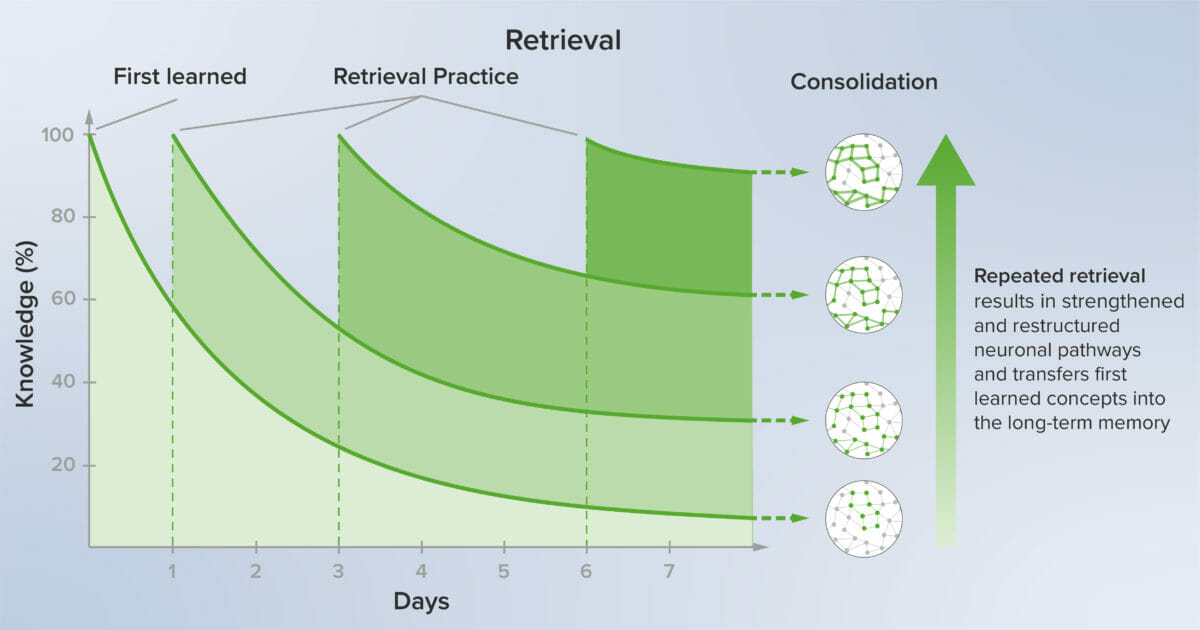
Active Recall and Retrieval Practice in Medical Education
Several evidence-based, data-driven approaches to education promote effective long-term knowledge retention, the most important of which are retrieval-based learning strategies. Retrieval is not only an important evaluative tool in knowledge testing but also one of the most practical ways to make learning durable. The effectiveness of retrieval-based strategies has been convincingly demonstrated in numerous cognitive science studies, and the neurophysiological basis of this effectiveness is becoming better understood. This article reviews the evidence supporting the use of retrieval-based strategies and provides recommendations for their implementation.
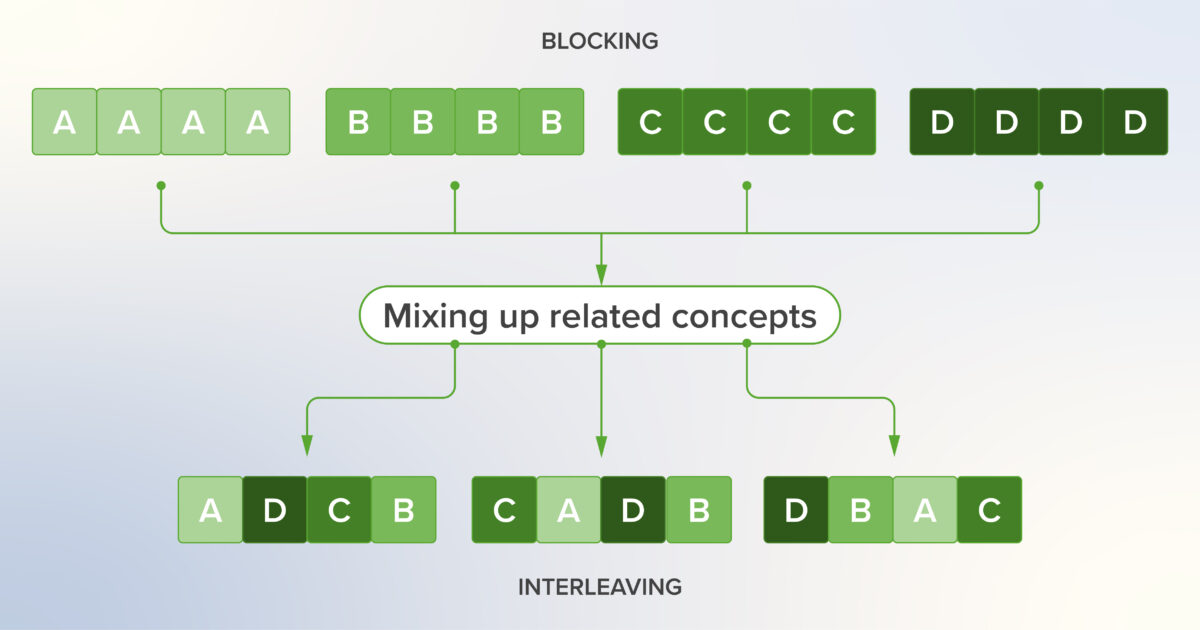
Interleaving: How to Mix Related Concepts to Make Learning in Medicine More Durable
In this article in our durable learning series, we explore a very important concept in learning science known as interleaving. While the value of interleaving has been demonstrated in multiple disciplines, it would appear to be significantly underutilized, especially given its potential benefit. In this piece, we will explain what interleaving is and how it is postulated to work from a neuroscientific perspective. We will also look at the evidence that supports its use and then provide recommendations on how medical educators and learners can incorporate it into their approach to learning.
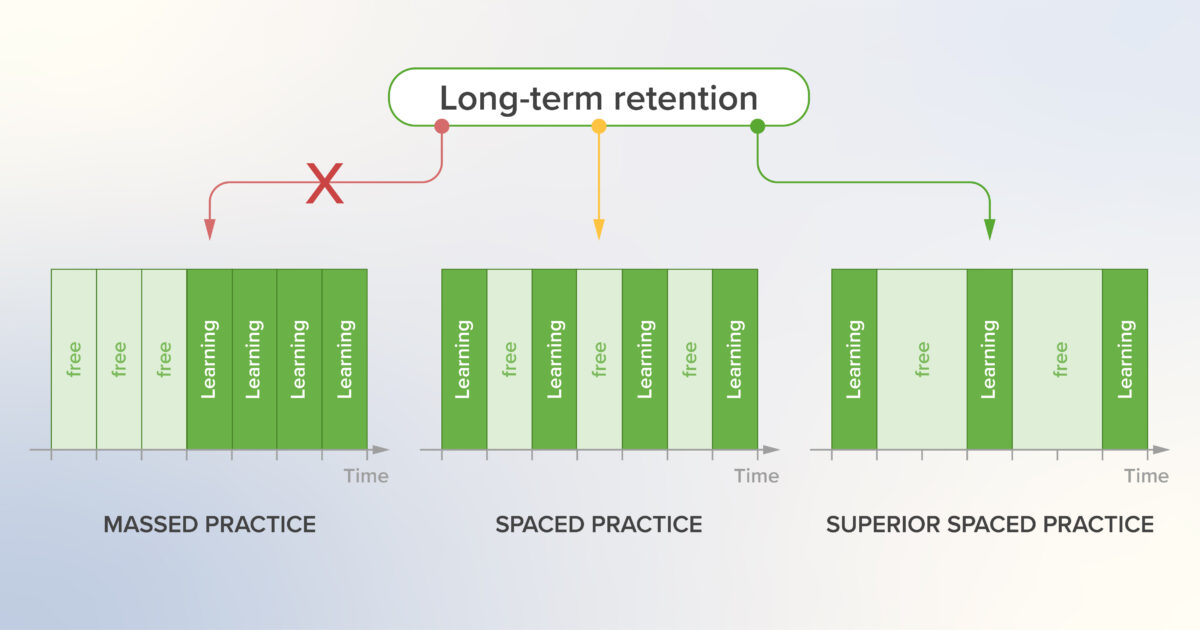
How to Apply Spaced Practice to Make Learning in Medicine More Durable
The purpose of this article is to introduce the learning method called spaced practice, which has been shown to be an effective approach for better retention of information in long-term memory. Spacing as an educational strategy involves spreading out the study of content to be learned over time rather than engaging in protracted study sessions focusing on a single subject. Both cognitive science and neuroscience have reported significant evidence to support the efficacy of spaced learning. It is a powerful learning technique for students and should be integrated into medical education and employed by learners in studying.
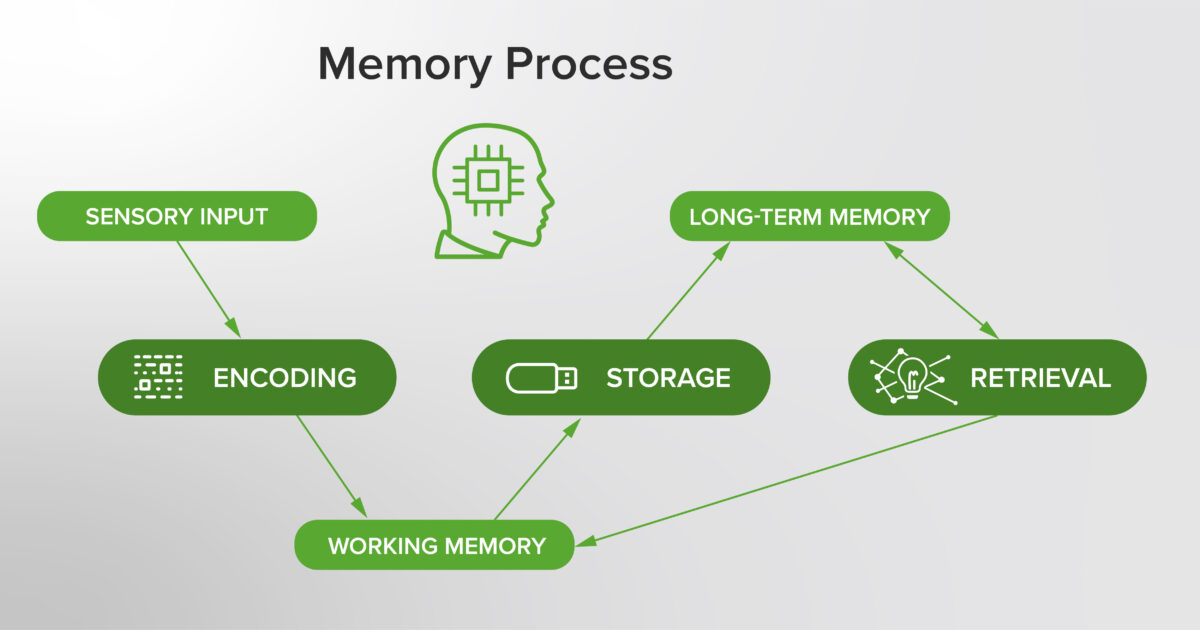
Understanding Memory to Enhance Learning in Medical Education
This article gives an overview of the different types of memory and the process of memory formation, drawing conclusions and exploring how understanding memory can be leveraged within the context of medical education.
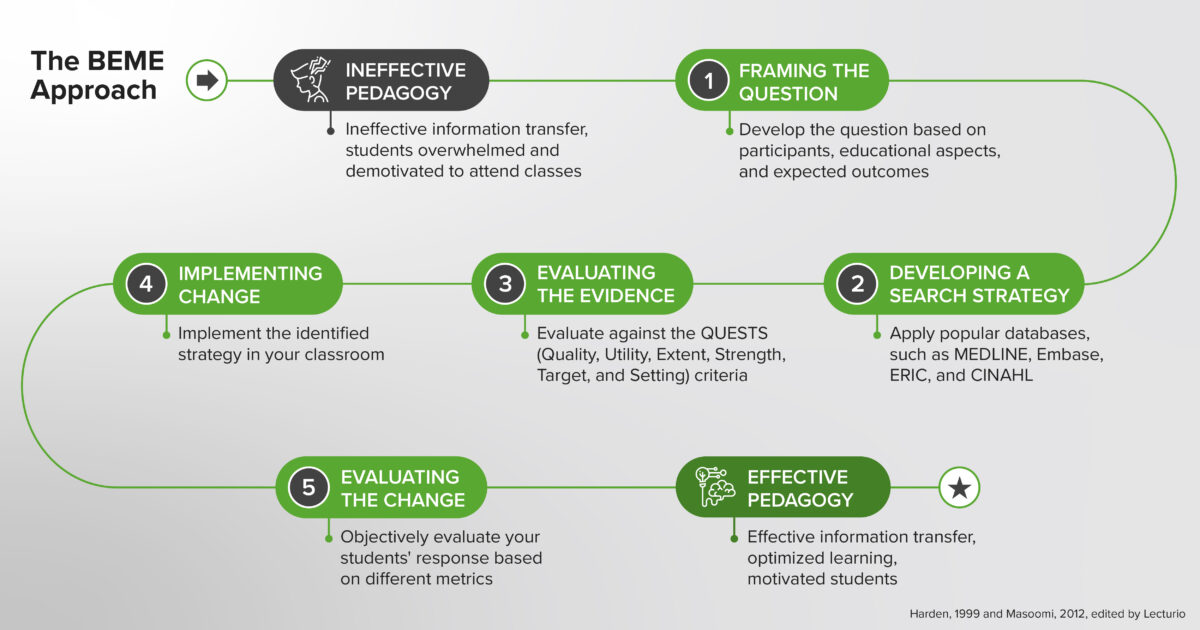
How to Apply Evidence to Tackle Misconceptions in Medical Education [Incl. Seminar]
After reading this article, readers should be able to have a basic understanding of the history of learning, an array of learning theories, and ineffective as well as effective conventions of medical education. This knowledge should allow educators to understand the importance of making evidence-based choices in their teaching practice.
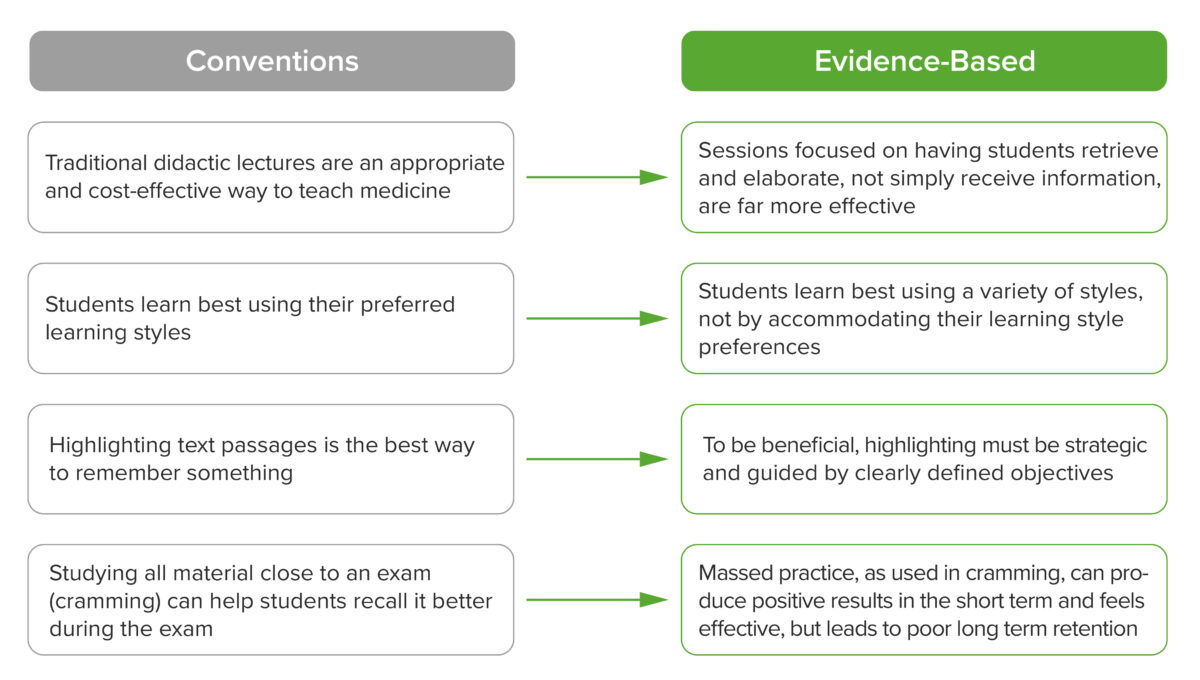
History of Learning: From Theory to Evidence-Based Application in Medical Education
Learning Science

2026 NCLEX-RN Changes: A Guide for Nursing Faculty
Starting April 1, 2026, the NCLEX-RN will introduce updated clinical expectations, including a focus on health equity and internal device monitoring, while maintaining its core content category weights.

From Passive Screens to Active Minds: This AAMC Faculty Toolkit Turns E-Learning Into Active Learning
Discover new ways to use AI and digital tools for active learning.

Simulation for Training: Transforming Medical and Nursing Education
Explore simulation in healthcare education. Learn the methods, benefits, and challenges of using simulation to train safer, more competent clinicians.

Lecturio Acquires SimTutor to Expand its Digital Healthcare Training Portfolio
Lecturio strengthens its global reach with new interactive, simulation-based learning solutions for healthcare professionals.

How Lecturio Supports the Remarkable Period of Growth in the PA Profession
Lecturio celebrates the hard work and expertise of PAs, and those who prepare them for practice, this PA Week.

Celebrating DOs on AACOM Advocacy Day 2025: How Lecturio Supports the Next Generation of Osteopathic Physicians
AACOM Advocacy Day is a yearly event where osteopathic deans, students, faculty, and advocates come together to speak up for the future of osteopathic medical education (OME).

HHS Nutrition Mandate September 10th Response Deadline: Lecturio Supports Medical Schools
An immediate solution to the Department of Health and Human Services’ mandate.

How Lecturio Videos Bring Mayer’s Multimedia Principles to Life
Discover how our platform videos are built on the latest developments in learning science.

Solving Bloom’s 2 Sigma Problem with Lecturio’s New AI-Powered Learning Tools
In 1984, Bloom proved one-on-one tutoring could boost student performance to the top 2%. Lecturio’s new AI-powered tools bring that level of personalized learning to medical students at scale.

SpeakNursing: A Powerful Partnership for Clinical Fluency
This new tool developed by Carnegie Speech and Lecturio is designed to help nurses achieve fluency in clinical English.

Lecturio Pulse: World No Tobacco Day
Explore evidence-based material on drug use and disease management.

Lecturio and Sigma Theta Tau Announce Exclusive NCLEX Partnership to Empower the Next Generation of Nurses
Lecturio and Sigma Theta Tau, the world’s second-largest nursing organisation, have entered into an exclusive partnership.

Learning Science Leader: What you need to know about leadership in healthcare education
Learn how to promote the quality of education and clinical practice with effective leadership.

Lecturio AI Tools: Empowering Educators by Streamlining Workload
Discover Lecturio’s comprehensive suite of AI tools, designed to save time and ease faculty workload.

Lecturio Named One of TIME Magazine’s Top 25 EdTech Companies in the World
TIME and Statista have named 350 companies changing education, with Lecturio coming in at #23 in the global ranking.

New Advanced Qbank Feature for Nursing Educators
Discover Lecturio’s brand-new Qbank feature, which categorizes practice questions within our educator platform.

The Digital Transformation of Care: A New Era for Nursing Practice
View insights from the latest instalment of our Global Webinar Series with nurse futurist Dr. Bonnie Clipper.

Women in Medical Education: Leading Progress Amid Challenges
Read our latest Pulse newsletter on women in medical education, and how Lecturio is promoting their roles.

Lecturio Acquires NEJM Healer in Major Expansion of Clinical Education Capabilities
Lecturio has acquired clinical reasoning education and assessment tool NEJM Healer from the New England Journal of Medicine (NEJM) Group.

Metacognition in Education: Examples and Strategies
In this article, we explore a concept that has not gained a lot of attention in medical education: metacognition. We start by explaining what metacognition is and why it is relevant for educators and learners. We then dive deeper into the elements of metacognition in the classroom and provide concrete examples of how it can be incorporated by both students and educators.

Active Learning Strategies to Improve Student Engagement in Medical Education
Helping students find a purposeful, productive, and effective way to learn is an important goal for medical educators. That goal can be advanced by the implementation of active learning: a set of evidence-supported educational tools that enhance student understanding and proficiency.

Active Recall and Retrieval Practice in Medical Education
Several evidence-based, data-driven approaches to education promote effective long-term knowledge retention, the most important of which are retrieval-based learning strategies. Retrieval is not only an important evaluative tool in knowledge testing but also one of the most practical ways to make learning durable. The effectiveness of retrieval-based strategies has been convincingly demonstrated in numerous cognitive science studies, and the neurophysiological basis of this effectiveness is becoming better understood. This article reviews the evidence supporting the use of retrieval-based strategies and provides recommendations for their implementation.

Interleaving: How to Mix Related Concepts to Make Learning in Medicine More Durable
In this article in our durable learning series, we explore a very important concept in learning science known as interleaving. While the value of interleaving has been demonstrated in multiple disciplines, it would appear to be significantly underutilized, especially given its potential benefit. In this piece, we will explain what interleaving is and how it is postulated to work from a neuroscientific perspective. We will also look at the evidence that supports its use and then provide recommendations on how medical educators and learners can incorporate it into their approach to learning.

How to Apply Spaced Practice to Make Learning in Medicine More Durable
The purpose of this article is to introduce the learning method called spaced practice, which has been shown to be an effective approach for better retention of information in long-term memory. Spacing as an educational strategy involves spreading out the study of content to be learned over time rather than engaging in protracted study sessions focusing on a single subject. Both cognitive science and neuroscience have reported significant evidence to support the efficacy of spaced learning. It is a powerful learning technique for students and should be integrated into medical education and employed by learners in studying.

Understanding Memory to Enhance Learning in Medical Education
This article gives an overview of the different types of memory and the process of memory formation, drawing conclusions and exploring how understanding memory can be leveraged within the context of medical education.

How to Apply Evidence to Tackle Misconceptions in Medical Education [Incl. Seminar]
After reading this article, readers should be able to have a basic understanding of the history of learning, an array of learning theories, and ineffective as well as effective conventions of medical education. This knowledge should allow educators to understand the importance of making evidence-based choices in their teaching practice.

History of Learning: From Theory to Evidence-Based Application in Medical Education
Teaching Strategies

Teaching Clinical Reasoning and Clinical Judgment: Strategies for Medical and Nursing Educators
Learn effective strategies for teaching clinical reasoning and clinical judgment in health professions education.

Assessments: New Uses for an Old Tool
Educators and students alike often think of an assessment as the final stop on the path of learning. Our current understanding of cognitive and neuroscience has taught us, however, that assessments can be an invaluable learning tool as well as a means of evaluation. Properly designed and well-written assessments can determine mastery of material, grade or rank students, measure student progress, reinforce learning, motivate students, and provide feedback to instructors (1). Assessments include more than just written exams; they encompass any form of evaluation or appraisal of a student’s educational progress by formal or informal means.

Learning Objectives and Assessments: Evidence-Based Recommendations for Optimal Efficacy [Incl. Seminar]
We can’t see learning happen, so how do we know it has occurred? Educators rely on observable behaviors as indicators of students’ skills, knowledge, and dispositions. Observable behaviors might include creating a concept map, demonstrating suturing skills, or communicating compassionately with patients. If a student could not successfully perform these before instruction and can perform them after, it is presumed learning has occurred. These desired observable behaviors are defined and communicated in learning objectives: concise statements of what a learner will be able to do as a result of instruction (1).

Effective Presentations: Optimize the Learning Experience With Evidence-Based Multimedia Principles [Incl. Seminar]
The purpose of this article is to introduce effective presentations, which have a set of key qualities: they are appealing, engaging, informative, and concise. Effective presentations gain attention and captivate the audience, but most importantly, they convey information and ideas memorably. Using evidence-based principles in educational multimedia can ensure the development of high-quality learning experiences. In fact, effective presentations have a set of core principles, a host of learner benefits, and a solid foundation in cognitive science. The article also explores the real-world implementation of effective presentations and share a practical application method that educators everywhere can use to develop effective multimedia in their classrooms.

Instructional Design: How Best to Optimize the Learning Process [Incl. Seminar]
Learn about Instructional Design, its benefits, how it helps support the alignment and integration of instructional goals, activities, and resources, and a practical implementation method for daily education practices.
Education Leadership
Sign up for updates on new Lecturio Pulse content
Never miss a pulse. We’ll email you when new articles are published.
Featured Interviews
Insightful discussions with thought leaders in education

Effective Knowledge Acquisition and Retention in Medical Education: View From Malaysia
The exponential rise in knowledge medical students are expected to master poses a great challenge for today’s educators. For medical school leaders, the implementation of new digital technologies and teaching modalities can be a crucial component to modernizing their organization’s approach to meeting this challenge. Lecturio sat down with Dr. Rajesh Perumbilavil, Deputy Dean of Academic and International affairs, to learn more about how Malaysia’s Asian Institute of Medicine, Science and Technology is moving from knowledge overload to knowledge management.

Learn How to “Make It Stick” with Renowned Author Peter C. Brown (Part 2)
Students have to memorize and understand ever-growing amounts of information and concepts in medical school. To conquer that, universities often urge their students to take the latest courses on “Learning How to Learn”, however, they themselves teach the way they have always taught. Students are responding with an all-time low attendance rate and seek outside help to pass their exams, which can lead to bulimic learning and a next generation of so-so doctors. Read below the first part of our interview series with recognized author Peter Brown to learn more about how we at Lecturio use “Make It Stick” concepts to improve student performance and long term retention, but also how you as a teacher can leverage those sticky ideas for your classroom.

Learn How to “Make It Stick” with Renowned Author Peter C. Brown (Part 1)
Students have to memorize and understand ever-growing amounts of information and concepts in medical school. To conquer that, universities often urge their students to take the latest courses on “Learning How to Learn”, however, they themselves teach the way they have always taught. Students are responding with an all-time low attendance rate and seek outside help to pass their exams, which can lead to bulimic learning and a next generation of so-so doctors. Read below the first part of our interview series with recognized author Peter Brown to learn more about how we at Lecturio use “Make It Stick” concepts to improve student performance and long term retention, but also how you as a teacher can leverage those sticky ideas for your classroom.
Learn how Lecturio can support your institution’s goals
Start Your Journey with Lecturio
Interested to learn how we can support your goals at the individual or institutional level?
Schedule a
tailored demo
Let our experts show you our learning platform.
Get a quote for
your institution
Tell us more about your use case and receive a quote.
Have a question?
Our team has an answer!
Email us any questions you would like us to address.