What is Metacognition?
The term “metacognition” refers to thinking about cognition(1), or to the knowledge, monitoring, and evaluation of one’s thinking. When 17th-century philosopher René Descartes declared “I think, therefore I am,” he was essentially thinking about thinking, and subsequently making conclusions about existence. He was engaging in a form of “meta-thinking,” a process that is a central tenet of contemporary philosophy.
Perhaps a more relatable example of metacognition at play is when someone thinks to themselves, “How will I remember this?” or, “Do I really know this?” Whether they are referring to a phone number, shopping list, cranial nerves, or existence, the subject of the thought is thinking itself.
In the classroom, metacognition may include students recognizing which concepts they are having trouble grasping, identifying strategies that have worked for them in the past with other difficult concepts, and trying those strategies one by one. A student with good metacognitive skills regularly reflects on their learning and understands their own strengths and challenges. They may seek out feedback on their performance and use that feedback to improve their learning and study habits.

Metacognition has been increasingly described and investigated within the field of cognitive psychology over the past two decades(2), and its implications have become apparent in various other fields as well. At the same time, advancements in the field of neuroscience have brought a deeper understanding of the neuroscientific underpinnings of cognitive learning strategies, which now applies to metacognition as well.
Recent evidence from neuroimaging reveals that the frontal cortex is particularly important in metacognitive processes and is separable from memory processes themselves(2,3). This suggests that despite variability in learners’ memory abilities, improvement on a meta level is still possible, with potential implications for learning.
Metacognition is important in medical education because it helps us understand how students learn and which teaching methods work best. It’s part of self-evaluation to ask, “Do I know what I think I know?” Unfortunately, educators still do not commonly discuss metacognition with students and often simply assume that students have already developed metacognitive skills.
Studies show that the use of metacognition among medical students varies greatly, and that few students are explicitly taught metacognitive strategies.
Medical students’ self-monitoring is insufficient
A recent study on medical student insights and the use of metacognition revealed that students tend to monitor their self-regulated learning with inappropriate cues(4), and that those lacking metacognitive skills often rely on weak study practices such as rereading and reviewing materials; use ineffective, passive learning strategies; and are overconfident in their abilities(5,6). Students also rely on exam dates and deadlines to pace and schedule their studying, rather than preparing detailed plans in line with their educational goals(7).
Increased metacognition boosts performance and reduces errors
Students with higher metacognitive awareness are focused on mastery learning, have higher motivation, and have better performance(8), while students who display mastery avoidance tend to have academic difficulties and show poor metacognitive awareness(9). It has been posited that explicit instruction on metacognition and metacognitive skills positively affects critical thinking skills as well as diagnostic accuracy.
When taught along with the importance of reflective practice for the avoidance of metacognitive biases, this has the potential to reduce diagnostic errors and improve patient safety(10). Incorporating metacognitive strategies into the classroom helps students plan, monitor, and evaluate their own learning(4).
Figure 1: Medical students with different approaches to learning but similar perception of readiness for an exam. Student 1 (left) represents how most students approach learning. Student 2 (right) performed significantly better on the test.

Figure 1 illustrates how good metacognitive skills make a difference in how medical students learn. Student 2 did significantly better than student 1, for example, and student 1, whose predicament is shared by many students, was left wondering what went wrong. Both students, however, despite having very different metacognitive abilities and study strategies, felt confident and ready to take their exam.
This brings us to one of the biggest pitfalls in learning: metacognitive bias and the illusion of knowing(11), which learners experience when they “feel” they have learned a concept, when in fact it is still primarily in their working memory. In reality, they have yet to do the hard work of establishing solid links and pathways to the neocortex, where durable memory resides.
Researchers have consistently demonstrated that learners overestimate their knowledge and expertise. In a 1999 study, psychologists David Dunning and Justin Kruger examined students’ knowledge and perceived expertise on certain topics. The results showed that students who were below a certain threshold of knowledge overestimated their expertise, a phenomenon that is commonly referred to as the Dunning-Kruger effect(12).
Figure 2: The Dunning-Kruger effect is represented by the peak on the left. Despite limited competence, confidence levels are very high.
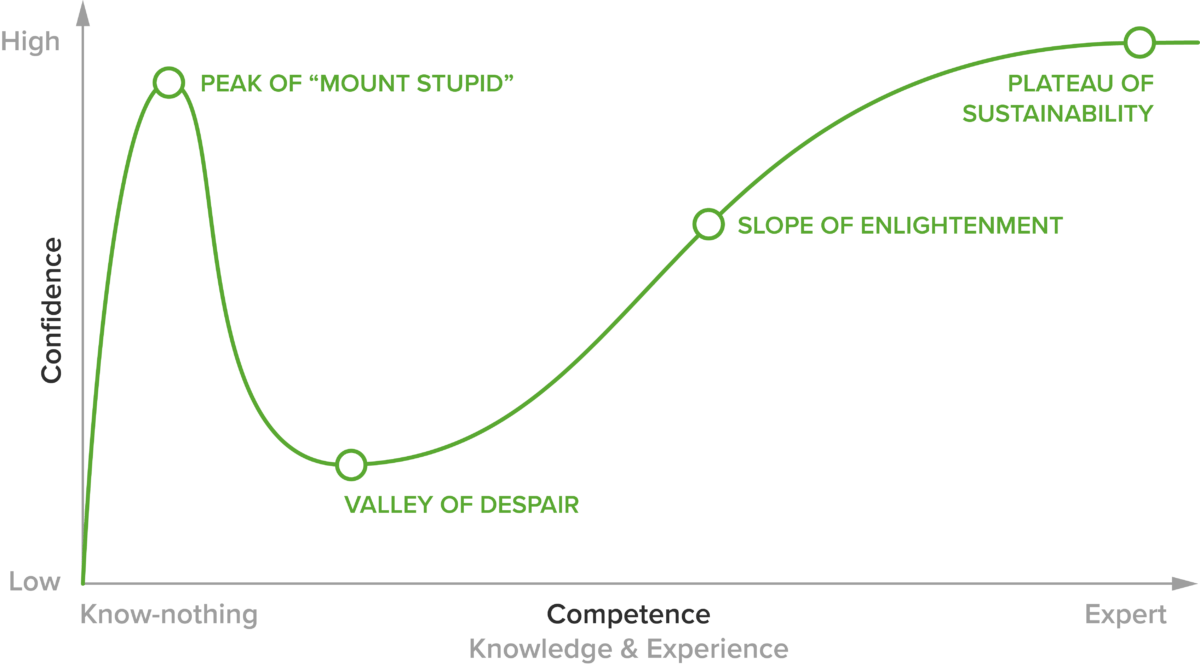
This phenomenon was consistently described in later studies across different fields. One practical example of the Dunning-Kruger effect at play is with the use of flashcards, a study tool used by many medical students. The literature shows that students are likely to prematurely “drop” flashcards before they have actually mastered the topic, resulting in negative effects on learning. The effectiveness of study tools that rely on self-regulation ultimately depends on the student’s metacognitive ability(13).
We now have an understanding as to how poor planning and improper study techniques adversely affect learning at a neurobiological level. Sleep deprivation hinders neuroplasticity and neural consolidation, and excessive stress can adversely affect neurochemical processes crucial to forming effective thought processes(14–16). The perception of success, whether accurate or not, can lead to dopamine release, resulting in a pleasurable sensation.
Conversely, adverse performance creates an unpleasant stimulus. This results in students being tempted to convince themselves that they have mastered a concept when this is in fact not the case. Furthermore, the transient storage capabilities of working memory can lead to the illusion of understanding the concept(11). Thus, metacognitive skills are crucial to optimizing the learning process.
Elements of Metacognition
Metacognition can be looked at as comprising two distinct elements: metacognitive knowledge and regulation(17), which are further divided into the sub-elements shown in Figure 3.
Figure 3: The various elements of metacognition
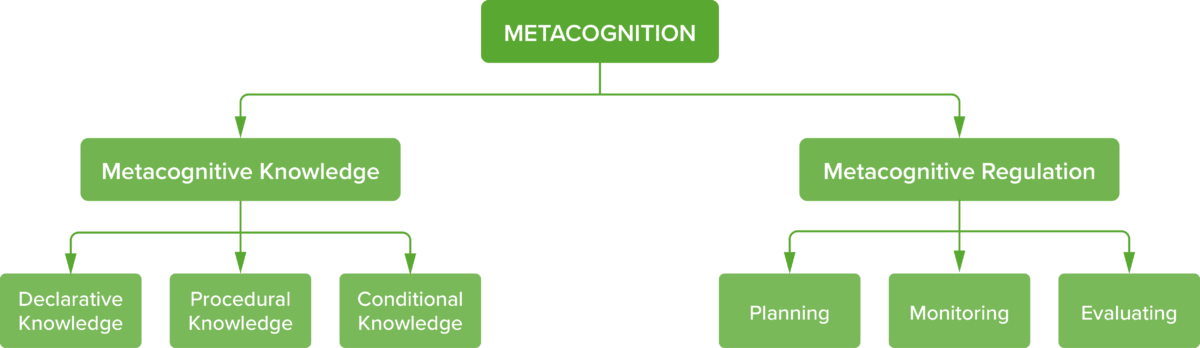
Metacognitive knowledge
Metacognitive knowledge is composed of three parts: declarative knowledge, procedural knowledge, and conditional knowledge(17,18).
#1 Declarative knowledge
Declarative knowledge refers to what the learner knows about themselves and their learning processes. It also involves metamemory, or the awareness of one’s own memory. Students may ask themselves what previous experiences they had with the topic and what strategies helped them learn and remember; they may also try to identify their strengths and weaknesses.
#2 Procedural knowledge
Procedural knowledge is awareness about task execution, such as how learning strategies will be used. For example, a student may know that spaced retrieval is an effective method, but not have the skills or knowledge needed to implement it. Educators may need to model appropriate strategies for given tasks(17).
#3 Conditional knowledge
Conditional knowledge refers to the learner’s ability to decide which learning strategies to apply to a given task. For example, creating note cards may be an effective strategy for remembering the steps of a procedure or identifying anatomical structures, but it would be a poor strategy for higher-order skills such as determining a differential diagnosis.
Metacognitive regulation
Metacognitive regulation refers to the learner’s ability to monitor and control their cognition as learning happens. Planning generally occurs before learning does, and combines metacognitive knowledge with assessing the task and resources at hand, and setting goals(5,8,19). Monitoring refers to the active processing of assessing understanding and determining whether learning strategies are effective. Evaluation involves the learner determining if their plan and strategies were effective(5,19).
In a 2015 study, researchers measured first-year medical students’ metacognitive skills at the beginning and end of their academic year, and demonstrated correlations with academic performance. However, although the students’ knowledge about metacognition was unchanged, they did have improved metacognitive regulation, suggesting that understanding how to regulate metacognition plays a bigger role in academic success(20).
Implementation in Medical Education
Planning
Learners are more effective when they can assess the task given, estimate the time needed to complete the task, determine what resources they may need, and activate prior knowledge related to the task. Giving students explicit objectives helps them activate prior knowledge and attend to relevant information (5). Planning can also be furthered with the use of pre-assessments and self-questions, such as:
- What do I already know about this topic?
- How can I prepare for this session?
- How much time will I need?(19)
Students should be encouraged to create a timeline to complete assignments, practice, and review, instead of waiting until the due date. They should also be encouraged to make their own learning goals, which has been shown to increase metacognition, decrease procrastination, and increase help-seeking behaviors(5,8).

Faculty development workshop
Learn how to integrate learning trends and theories like metacognition into your faculty’s teaching approach, motivate educators, and help students succeed.
Monitoring and evaluating
Student-centered learning approaches
Student-centered learning approaches that use active learning strategies help increase metacognition. As discussed in our previous article, active learning strategies help construct knowledge by relating new information to prior knowledge. Tactics such as generating and elaborating help students monitor their learning.
Reflection
Reflection, especially when it incorporates self-questioning and identifying uncertainties, also helps students monitor and evaluate their learning. Additionally, problem-based learning, even when used in just 10% of a given curriculum, has been shown to improve student metacognition(5,21).
Expert modeling and “think–aloud” exercises
Medical educators can encourage students to monitor their learning by using expert modeling and “think-aloud” exercises for both the educator and students. Educators can use think-aloud strategies to model their own expert content knowledge, sequencing of tasks, and metacognitive strategies(5,19) while student think-aloud exercises are also effective in helping students identify similar processes that may contain gaps in their understanding. Thinking aloud during problem solving and case-based exercises can highlight students’ ability to plan and monitor their cognitive processes(4).
Peer reviewing
Educators can also encourage students to practice peer review, which is a technique where one student reviews the progress and abilities of their peers. This technique can be an effective tool to help learners better understand their capabilities, both by helping them more accurately assess their own skill levels and through receiving additional feedback from their peers(22).
Cognitive offloading
Another application of metacognitive evaluation is cognitive offloading(23). This is the process of storing information outside of memory (in a notebook or on a smartphone, for example) to help reduce the cognitive load needed to process and retain the information. The decision to store something somewhere is metacognitive in nature. Following the same logic, the decision to move information from a learner’s working memory to long-term memory, which essentially entails the utilization of evidence-based metacognitive strategies, is ultimately a decision of meta-memory(24).
Frequent feedback
Metacognitive tools can also be provided outside of the classroom by giving students opportunities for frequent, formative feedback, such as encouraging self-testing with practice problems and providing practice exams(17). Educators can also provide checklists and rubrics so that students can monitor their own progress(5). Encourage students to review feedback that is given, not just track their grades.
Figure 4: Metacognitive regulation: Planning, monitoring, and evaluation
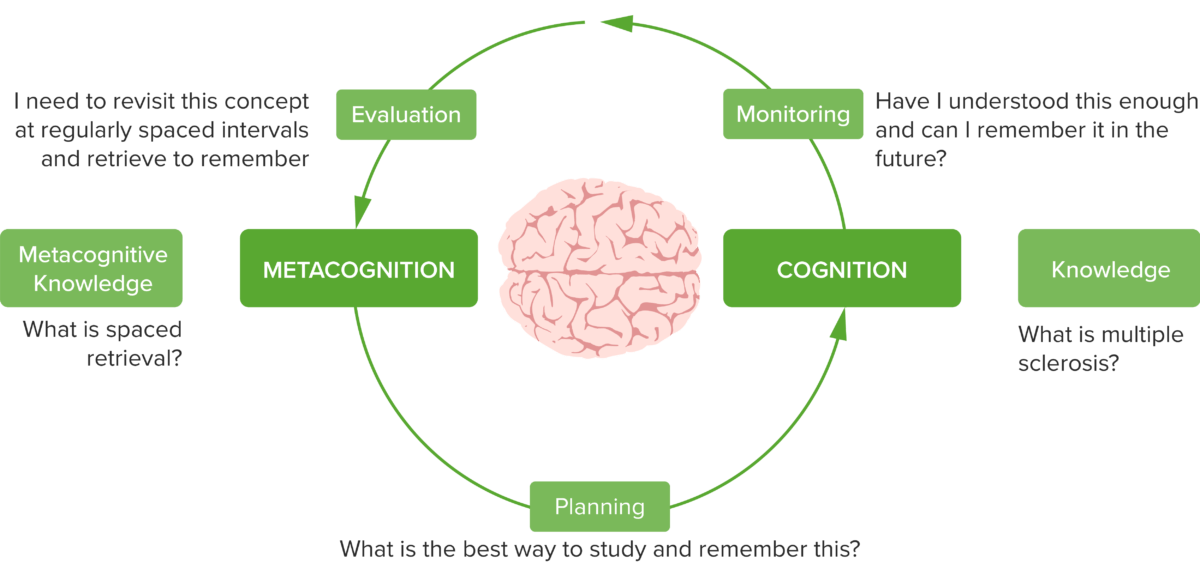
Look back at our earlier example in Figure 1. In what ways was Student 2 using metacognition? (answer at the end)
U-Behavior: incentivizing good practices
Making students aware of metacognitive strategies is a good first step, but it may not be enough. Even if students attempt new strategies, they may still revert to familiar techniques like cramming.
In a study conducted at Colorado State University led by education professor James Folkestad, researchers implemented a program called U-Behavior, a system that was used to track students’ progress and provide visual feedback. In an earlier version of the study(25), students were encouraged to use spacing and interleaving with a series of low-stakes quizzes. Compliance was poor, however, despite the students knowing the superiority of these strategies. Most of the students reverted to massed practice as they pursued the highest score on each quiz.
Later studies(26) altered the format by decreasing the importance of quiz grades; instead, grades were based on the students’ behavior in taking the quizzes—whether the students used spacing and interleaving in taking the available quizzes versus taking them to complete them by a deadline or get a high score. This was far more effective, not only in changing students’ behavior but also in improving their grades and long-term retention of the material.
The researchers have been able to replicate these results across terms and in other courses. This is a strong indication that educators need to not only make students aware of good strategies but also find ways to incentivize good practices.
Technology
Students who have access to high-yield interactive materials have more effective decision-making strategies, improved motivation, and better goal-setting skills, especially when combined with instructor feedback(27). Technology provides unprecedented access to resources but also can inundate students with information and options.
Educators can aid student learning and improve metacognition by helping students learn how to select relevant and efficient resources. Technology can be used to provide pre-assessments, which inform learners as well as educators about students’ prior knowledge and potential needs. Using learning platforms to provide spaced retrieval, online quizzes, and discussion tools helps students monitor their learning by providing formative feedback, and can also serve as a tool for cognitive offloading and leveraging metamemory.
Furthermore, the use of technology to help implement a flipped classroom approach has been shown to improve metacognitive awareness and regulation(28). Integrating technology can also reduce educator workload in the long term as well by automating useful tools, creating and curating reusable resources, and providing automated feedback on student progress.
Learning analytics in the online environment can be used to observe student behavior and progress, and provide another source of data-driven feedback. Learning platforms contain rich data for educators to monitor and use.
If available, useful data may include when quizzes are accessed, how many attempts are made, the total time spent, and the frequency of attempts made near the due date(29). These insights can give instructors a measure of student metacognition and learning habits by analyzing how they are using spaced retrieval, how they are planning and executing their time, and identifying items of concern that the instructor may wish to address.
Your digital teaching assistant
The Lecturio platform boosts student scores and engagement, saves time, and increases faculty retention. Learn more →
Examples of Metacognitive Strategies
Metacognition strategies for educators
- Don’t assume that students instinctively have good metacognitive skills. These skills need to be taught and reinforced.
- Build desired features into your classroom teaching: Explicit objectives, pre-assessments, self-questions, spaced retrieval, active learning, formative feedback, and think-aloud exercises help build student metacognition, which, in turn, improves student learning and retention.
- Use technology to let students direct their own learning and track their own progress.
- Recognize red flags of metacognitive lapses, such as poor planning, overconfidence, and performance avoidance.
- Implement frequent low-stakes tests.
- Reward students for using effective learning strategies.
- Remember that It is not enough to simply explain the importance of a strategy: It is also important to make sure that the educational design reflects this importance and directs the students toward the use of these strategies.
Metacognition study strategies for learners
- Students should plan and prepare for their learning experience. They should regularly ask questions such as: What do I already know? What tools and resources will I need? How long will it take? Do I really know what I think I know? How can I be sure of this?
- Students should monitor their learning by frequently reviewing material, practicing regularly, quizzing themselves, and identifying points of confusion.
- Students should avoid weaker study habits such as cramming and rereading, which may be familiar but are not effective for durable learning.
- Students should review feedback regularly. They should be given opportunities to discuss their findings and any confusion they are experiencing with classmates and/or their instructor.
- Students should embrace technology to facilitate concept practice and gain immediate feedback. Directing students to relevant resources can make technology even more effective.
Reflection Questions
(Please select all that apply)
1. Which of the following statements are true?
a. Metacognition is the process of thinking about one’s thinking.
b. Research has yet to demonstrate the value in rewarding students for good metacognitive practices.
c. Good students tend to have good metacognition skills.
d. Metacognition is relevant only to pre-clinical students, as clinical students need more hands-on experience.
2. Why is metacognition important for learning and memory?
a. Students typically don’t know how much they don’t know.
b. Metacognitive knowledge is essential for metacognitive regulation.
c. Metacognitive strategies are perceived as being easy to use by students.
d. Better metacognition can result in better patient safety.
3. At what point in the teaching process does metacognition play a role?
a. Before delivering content to students.
b. At the curriculum development stage.
c. During assessments.
d. During a lecture.
4. What are metacognitive strategies?
a. Thinking aloud while solving a problem
b. Reviewing feedback you have received
c. Reflecting on how your learning is going
d. Self-quizzing and peer quizzing
5. Which of the following is an example of metacognition?
a. Quizzing yourself over the material
b. Rereading lecture notes
c. Highlighting information in a textbook
d. Summarizing and annotating lecture notes
6. What are some ways you can apply the use of metacognition to your own learning? Practice metacognition, think of some answers to this question, and share them with your colleagues!
Correct answers: (1) a,c. (2) a,d. (3) a,b,c,d. (4) a,b,c,d. (5) a, d.




