Playlist
Show Playlist
Hide Playlist
Ventral and Incarcerated Hernias
-
Slides Hernias Surgery.pdf
-
Download Lecture Overview
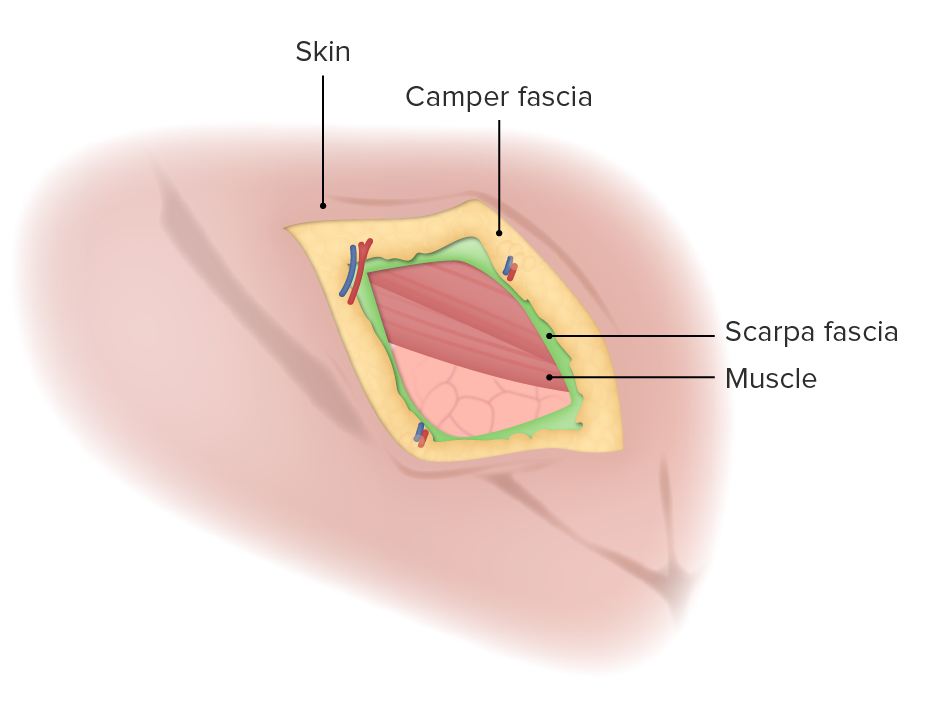
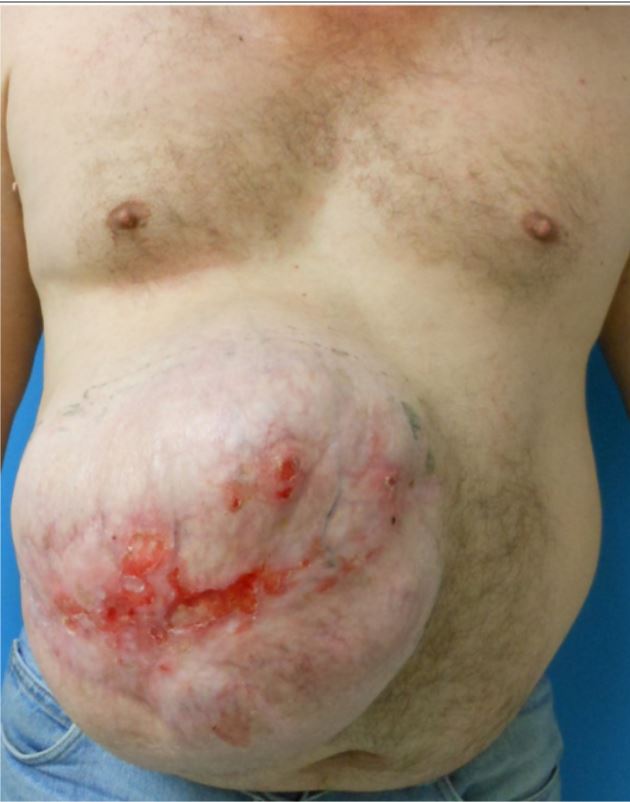
00:01 Let’s move on to ventral hernias. Here’s an anatomy of a ventral hernia. A ventral hernia is a common term for any hernia on the anterior surface of the abdomen. You may have heard these terms also as ventral or umbilical. But basically, a ventral hernia is located anywhere else on the abdomen as long as it’s in the anterior abdomen. You’ll notice that the symptoms and findings of ventral hernias can be very similar to those of inguinal hernias. Again, one may notice a bulge, nausea/vomiting if there’s a small bowel obstruction, and similarly obstipation if there’s small bowel obstruction, once again the inability to pass flatus or have bowel movements. Very commonly, patients who have had previous surgeries develop incisional hernias after surgery. This image shows a laparoscopic repair of a previous midline incision. 01:10 The common scenario that I see in my practice are patients who have had exploratory laparotomy incisions through the midline. Particularly under duress, the fascia is closed. The patient recovers. Years later, they develop an incisional hernia. This can be repaired laparoscopically. 01:28 An incisional hernia is also categorized as a ventral hernia. What are the risks? These slides will be familiar from the inguinal hernia; again repetitive heavy lifting whether it’s part of exercise or part of your daily work; chronic coughs, again smokers, COPDers, asthma patients; and chronic constipation. Weight gain is a particularly high risk for ventral or incisional hernias. This is why oftentimes when patients have gained significant amount of weight, I counsel them that we need to wait until they lose weight before the repair as they have a very high recurrence rate. Same thing, basically anything that increases Valsalva or intraabdominal pressure may lead to a risk of developing hernia. 02:14 Here’s a picture of a ventral hernia rather. It’s a large Here’s a picture of a ventral hernia rather. It’s a large ventral hernia. If you look closely at the image, you’ll see that the patient had a previous skin graft to cover it. This is what we call significant loss of domain, which means that the abdominal wall which should be midline is now retracted laterally and the intestines are exposed. So, to prevent the intestines to be freely exposed to air, oftentimes we put a skin graft to temporarily cover. This patient, the common scenario would be a trauma patient who required an emergent exploratory laparotomy. 02:52 Again, diagnosis: The physical examination usually is enough. This can be limited just similarly to inguinal hernias by equivocal exam or limitations such as morbid obesity. Particularly for incisional or ventral hernias, it can be very helpful to get cross-sectional imaging such as a CT scan abdomen/pelvis. This is my management schematic of ventral hernias. Again, I think of it as reducible and not reducible. Remember that when the ventral hernia or incisional hernia is large, it’s unlikely that the intestines will get stuck. You can imagine when you have a big defect, the intestines can move through back and forth versus a small defect, if intestines come out, they can potentially get edematous and get stuck. Similarly to inguinal and femoral hernias, reducibility usually guides how you manage it. Reducible hernias can be electively repaired. Again, strangulated or incarcerated hernias will likely require either emergent or urgent repair. This is a fairly new development which is a laparoscopic inguinal hernia repair. Laparoscopy has some advantages, although it's an oversimplification to think that laparoscopy is always better. A laparoscopic incisional hernia repair requires the insertion of a dilating balloon in the preperitoneal space. Recall from earlier slides that the abdominal wall has multiple layers differentiated between above and below the arcuate line. 04:29 Below the arcuate line, just as a reminder, all layers go above to form the anterior rectus sheath except the transversalis fascia. In this situation, this space is a potential space that a balloon can get into the preperitoneal space and allow us to perform a unique repair of the inguinal hernia which has been traditionally repaired in an open fashion. Here, you see the balloon dilating the preperitoneal space. Notice that there, the pubic symphysis is your guide. All the intestines are now below this balloon. We never violate the abdomen because we don’t violate the peritoneum. 05:07 That’s why it’s called a preperitoneal approach. Once the balloon has been fully expanded, the space is now insufflated. The camera is inserted into the space and it allows us to perform the inguinal hernia in an inside outward approach as opposed to the traditional outward inside approach. High-yield facts for your examination: Incarcerated hernias are irreducible but not necessarily strangulated. If a clinical scenario presents to you where the patient has a strangulated hernia, the next step of management should be immediate surgery. Remember for strangulated hernia, typically the patient may have some pain over the bulge but we can’t allow that intestines or whatever the content is to slip back without examination. Remember, when it’s strangulated, it may have its blood supply cut off and that segment of intestines need to be examined prior to your repair. No imaging studies should be pursued when an exam is consistent with a strangulated hernia. You should pursue surgery. Remember, although we don’t offer surgery to everybody, hernias don’t go away on their own. In fact, over your lifetime, hernias typically get larger with daily activity, weight gain, weight lifting, exercise, so on and so forth. 06:30 Thank you very much for joining me on this discussion of groin and ventral hernias.
About the Lecture
The lecture Ventral and Incarcerated Hernias by Kevin Pei, MD is from the course General Surgery.
Included Quiz Questions
Which of the following is NOT true about ventral hernias?
- All ventral hernias are umbilical hernias.
- A ventral hernia is a hernia on the anterior surface of the abdomen.
- An umbilical hernia is a hernia located by the belly button.
- All umbilical hernias are ventral hernias.
- Symptoms can include bulges through the abdominal wall, obstipation, nausea, and vomiting.
Which of the following is NOT a known risk factor for developing a ventral hernia?
- Anorexia
- History of a prior abdominal wall incision
- Heavy lifting
- Chronic cough
- Chronic constipation
Which of the following statements about the diagnosis and treatment of ventral hernias is TRUE?
- Surgical intervention for an irreducible strangulated hernia is more emergent than for an irreducible incarcerated hernia.
- A physical exam is not sufficient for identifying strangulation of the bowel.
- A CT scan is required to diagnose ventral hernias regardless of the patient’s body habitus.
- All reducible ventral hernias must be surgically repaired.
- Surgical treatment of an incarcerated hernia is elective.
In cases of strangulated hernia diagnoses, what is the recommended next step in management?
- Immediate surgical repair
- Confirm the diagnosis by CT scan.
- Manual reduction in the emergency room
- Endoscopy
- Elective surgical repair
Customer reviews
4,0 of 5 stars
| 5 Stars |
|
0 |
| 4 Stars |
|
1 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
much more details on the diagnosis could have been provided....on the whole I really pleased to find a website like this....please continue to develop the site...its really good