Playlist
Show Playlist
Hide Playlist
Urea Cycle Disorders
-
Slides MetabolicDisorders Pediatrics.pdf
-
Download Lecture Overview
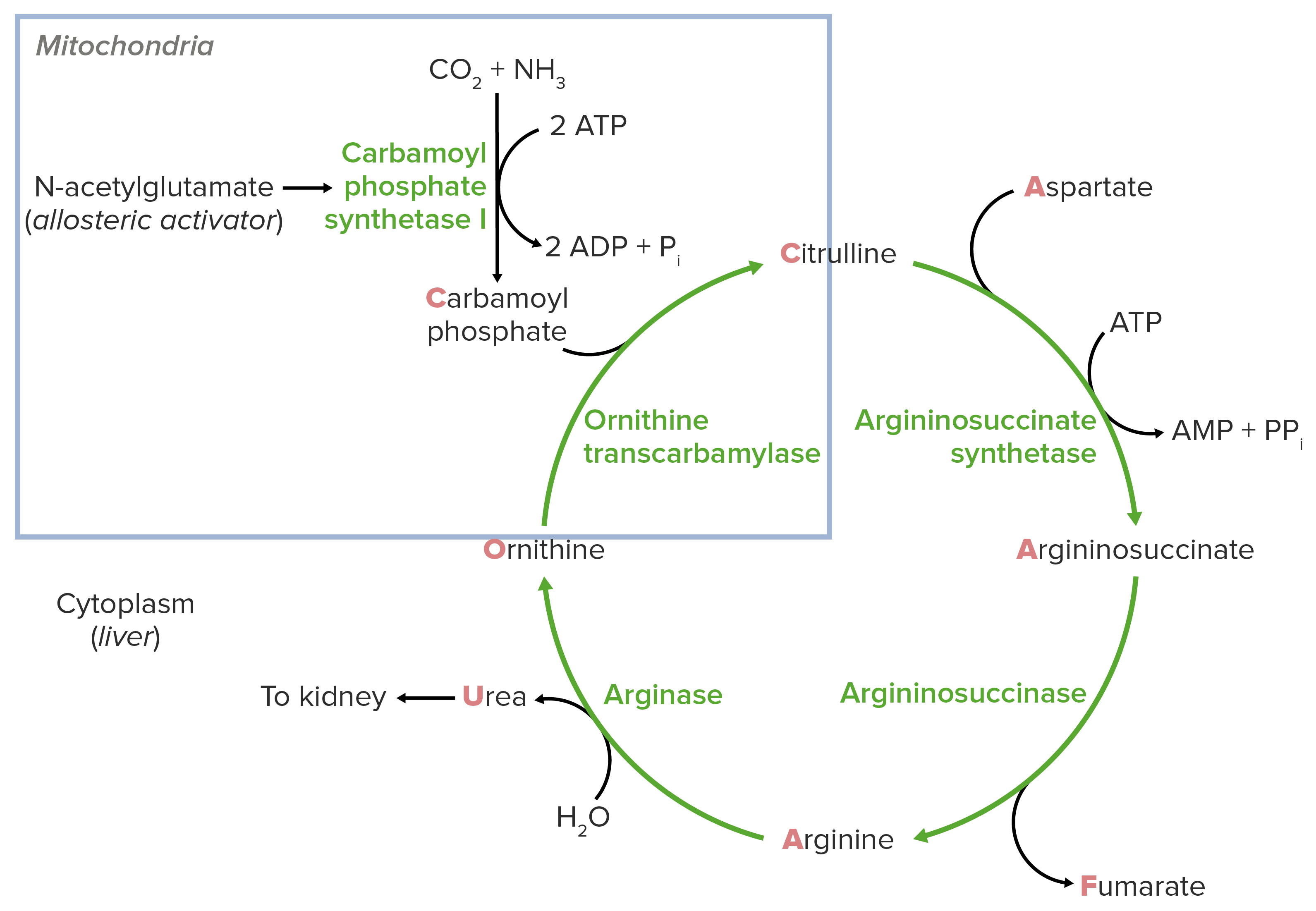
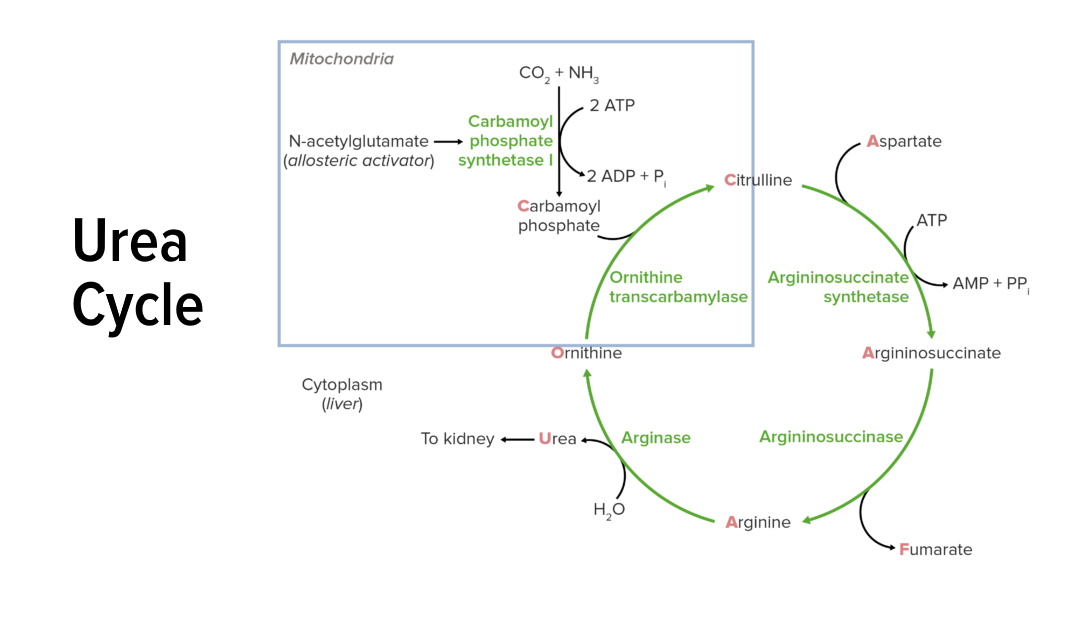
00:02 Let's switch now to the urea cycle defects. 00:04 These are problems with patients have problems getting rid of nitrogen waste. 00:10 Almost all of them are autosomal recessive with the exception of ornithine transcarbamylase deficiency or OTC. 00:20 OTC is X-linked, which means girls get it mildly or not at all, boys get it very badly. 00:28 This family of diseases will typically present with increased ammonia levels and ammonia toxicity. 00:38 There is a variability in how severe it can be but they can be quite severe. 00:43 And these patients with hyperammonemia develop long term cognitive problems. 00:49 So treatment of these urea cycle defects includes medicines that allow disposal of ammonia by bypassing the urea cycle and allowing excretion of ammonia. 01:05 Drugs for these are unusual. 01:07 In other circumstances you might not even have seen these or use these drugs before unless you've taken care of one of these patients. 01:14 Examples would be sodium benzoate and sodium phenylbutyrate. 01:18 Sometimes we can use arginine hydrochloride and if the meds aren't enough and the patient is having bad ammonia crisis, we can also do dialysis. 01:28 But the key drugs are sodium benzoate and sodium phenylbutyrate. 01:33 So in the acute setting, where a patient is coming in a very high ammonia levels. 01:39 We're gonna first stop giving any protein at all. 01:42 We want them to get no more additional nitrogen in their diet. 01:46 We're gonna give them medicines to bypass the urea cycle, more sodium benzoate and more sodium phenylbutyrate. 01:53 But those things are a little bit different but you get the idea. 01:56 Lastly, if it's severe, we'll give them dialysis. 02:00 The idea is to completely remove that nitrogen from their body because any minute with a high nitrogen level is really bad for their brain. 02:07 So that's all I have for you today, about all these metabolic defects. 02:12 They are incredibly complicated and challenging to remember. 02:16 And this is just an overview, but I hope it'll be enough for you and if you review a few times I'm sure you'll get it well. 02:22 Thanks for your attention.
About the Lecture
The lecture Urea Cycle Disorders by Brian Alverson, MD is from the course Pediatric Endocrinology.
Included Quiz Questions
On routine investigation, an infant is found to have high ammonia levels and you suspect ornithine transcarbamylase deficiency. What is the first medication you put this child on?
- Sodium benzoate
- Sodium chloride
- Sodium 2-mercaptoethanesulfonate
- Sodium phosphate
- Sodium polystyrene sulfonate
What is the mode of inheritance of ornithine transcarbamoylase deficiency?
- X-linked recessive
- X-linked dominant
- Autosomal dominant
- Autosomal recessive
- Mitochondrial
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
3 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Very good - thanks so much! Really helped to get my head around these.
Excellent lecture. I now feel more comfortable with recognising inborn errors of metabolism.
1 customer review without text
1 user review without text