Playlist
Show Playlist
Hide Playlist
Types of Hyperlipidemia
-
Slides Atherosclerosis Cardiovascular Pathology.pdf
-
Download Lecture Overview
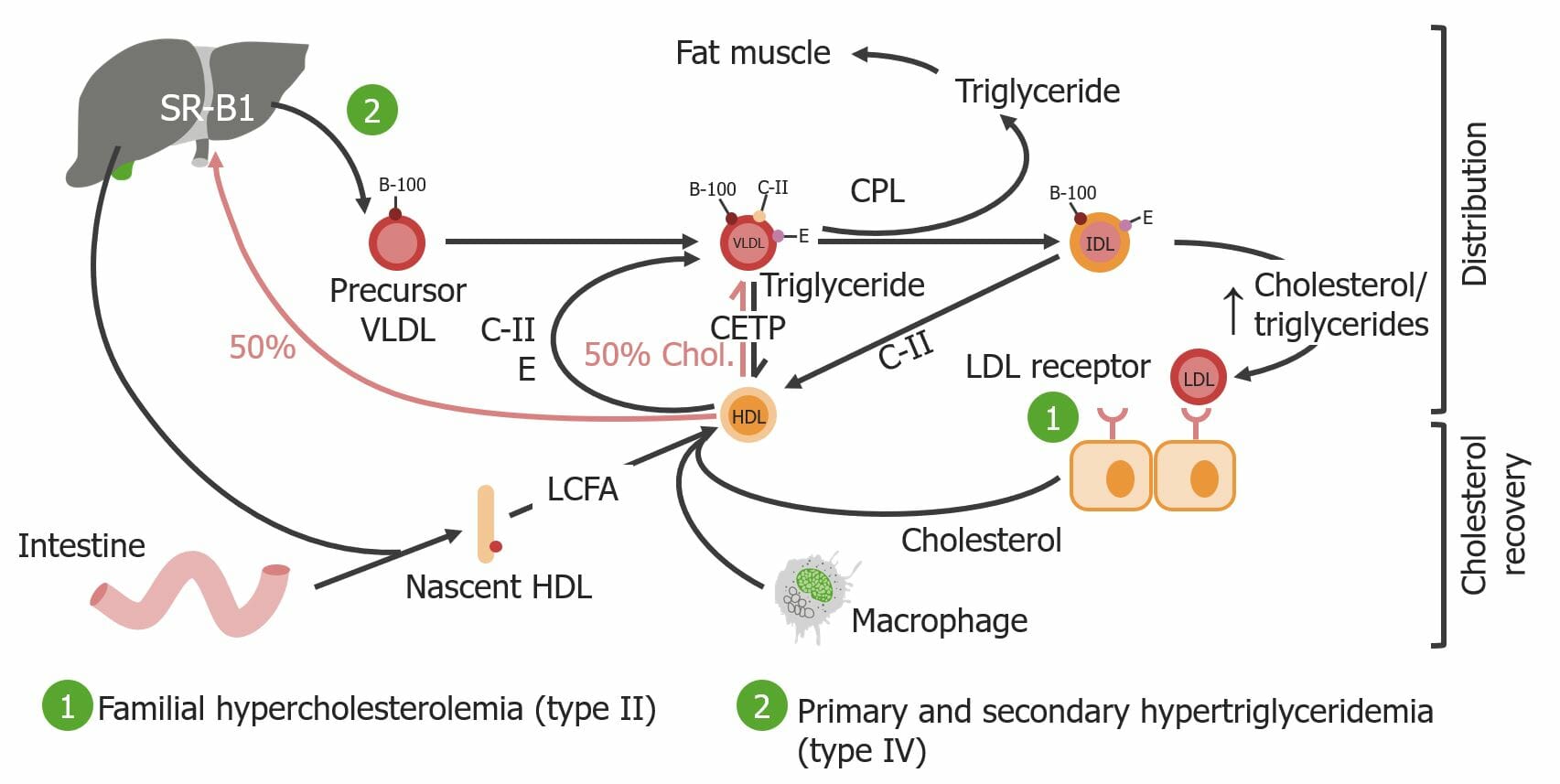
00:00 Now to summarize everything we just talked about, here are the different types of hyperlipoproteinemias. We call this hyperlipidemias. Let us take a look at the one specifically that we just talked out and plugging in the pathology. 00:13 Take your time here. Let us begin with type I. In type I our discussion took its back where you consumed lipids from the mouth and went through the system and ended up at your liver. And as you went through that process and you emulsified, you found a chylomicron, you got into a circulation. What was the name of that enzyme and what was that HDL gave that nascent chylomicron? C-II and lipoprotein lipase. There you have it, please. 00:41 Take a look at the category in column molecular and type I is the fact the C-II in capillary lipoprotein lipase are completely deficient. If that is the case, what are you going to accumulate? Which lipoprotein? Good. Chylomicron. What are going to increase in your patient? Triglycerides. Next, let us talk about type II. If it is type II in the discussion, where there was a lipid being transported from the liver to the tissue. You take me through that quickly. You released what from your liver? L-I-V-E-R liver produces VLDL. It is as simple as that. VLDL will never, I repeat, will never be produced in enterocyte, only from the liver. Next that VLDL contains what? Triglycerides. That VLDL has to be formed into LDL so that it contains cholesterol to go where? To the tissue, to the target. What was the intermediate that was present between VLDL and LDL? It is called IDL. Eventually, you formed your cholesterol, you formed your LDL and your LDL is going to the tissue, how does it go to the adrenal cortex? How does it go to the membrane? How does it go to the gonads? It goes or it is then accepted and engulfed with the help of LDL receptors. Is that important? Oh! my goodness, yes. 02:12 If LDL receptors aren’t working properly and they are deficient, this is, in general, I do not care if it is type IIa or IIb, both will have the predominent theme of LDL receptor deficiency. What you are going to start accumulating in your blood? does LDL mean to you? Cholesterol. What might you then call this, please? Hypercholesterolemia. Now, what is the difference? All that you want to do here is take a look at IIb. IIb is the combination of LDL and VLDL accumulating in your circulation. 02:43 You know that, you'll be in good shape. But the fundamental problem in type II is the fact that you are deficient of LDL receptors. Where? Most likely in the liver. Let us continue. Now we have type III, I want you to focus immediately on molecular column. I want you to focus immediately on that E and you have three horizonal lines. So type III is a problem with apo E. What does that mean to you? Is it a problem with lipoprotein and lipase? No. It was a problem with your remnant being removed and hence it is sometimes called remnant removal disease. What's the other name for this? Familial dysbetalipoproteinemia. 03:20 That must be clear. Then the last one that we will be discussing here will be type IV. 03:25 We have to, why? Because once again obesity is a huge problem in the world really and whenever there is obesity, how well does your insulin work? It doesn't work work properly because you have insulin resistance. So let me walk you through this, first and foremost, VLDL is coming from where? It is coming from the liver, L-I-V-E-R, VLDL. What do you need so that you can form the VLDL or convert your VLDL into IDL require the help of your capillary lipoprotein lipase? Sure we do. So, therefore, insulin works if you remember your biochemistry, pay attention, insulin as long as it is working, normally works to then stimulate capillary lipoprotein lipase so that you can then extract some of that triglyceride from the VLDL. But in diabetes mellitus at some point what happens on insulin levels? It starts dropping, doesn't it? So, If insulin is not there, then your capillary lipoprotein lipase is not working properly. You are going to start accumulating VLDL, a secondary type of hypertriglyceridemia. Welcome to type IV. 1, 2, 3, 4. Four. V-L-D-L, four. You want to take a look at type V. You do that on your own. You know these four, you will be in great shape.
About the Lecture
The lecture Types of Hyperlipidemia by Carlo Raj, MD is from the course Atherosclerosis: Basic Principles with Carlo Raj.
Included Quiz Questions
Which type of hyperlipidemia is associated with the elevation of cholesterol only due to the accumulation of LDL?
- Type IIa
- Type I
- Type IIb
- Type III
- Type IV
Which of the following are elevated in patients with type III hyperlipidemia?
- IDL and VLDL
- HDL and glucose
- LDL receptors
- Bilirubin and lactate
- LDH and CK-MB
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Clear and straight to the point! Potentially difficult stuff becomes super easy with him!
Very good class, very dynamic teacher, excellent for learning, 5 stars