Playlist
Show Playlist
Hide Playlist
Tracheoesophageal Fistula (TEF)
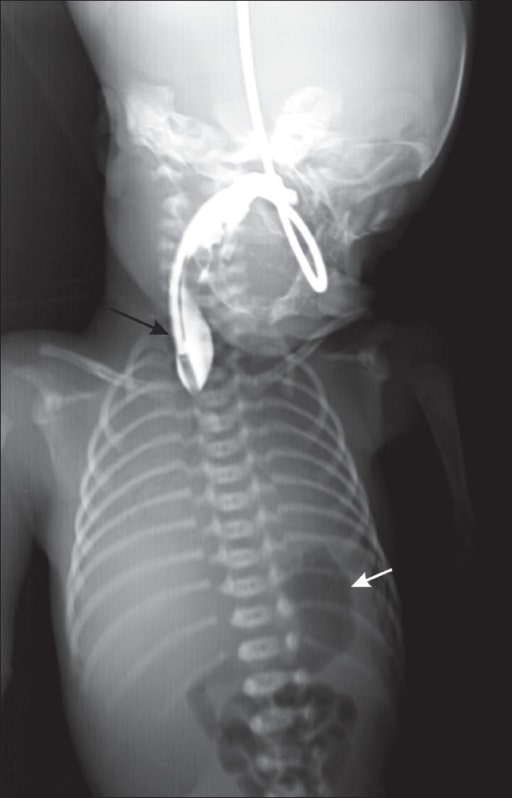
00:01 In this lecture, we’re going to discuss tracheoesophageal fistula. 00:06 So TEF or tracheoesophageal fistula is an abnormal congenital connection between the trachea and the esophagus. 00:16 There are five types. 00:19 Type 1 is by far the most common. 00:22 This is an atresia with a fistula between the distal esophagus and the trachea as is pictured here. 00:29 You can see the esophagus basically stops. 00:33 The stomach is connected to trachea. 00:36 So these patients will show up very, very early. 00:39 Their first meal, it ain’t going anywhere. They’ll spit up. 00:44 A smaller percentage, 8%, have a completely atretic stomach and esophagus. 00:50 In other words, there’s not fistula. 00:52 There’s simply a blind and looped esophagus and a blind and looped stomach. 00:57 These infants should have no gas bubbles in their intestines on an X-ray, and will spit up very quickly after eating. 01:03 This represents 8%. 01:05 You can see we’ve already accounted for most of tracheoesophageal fistula. 01:10 Almost the rest are the third type and this is an H type of fistula. 01:16 The H type fistula is basically a connection between the trachea and the esophagus. 01:23 There’s a little bridge. 01:25 So these infants are interesting and that they can present a little bit later on. 01:31 Basically, at some point, their gastric contents do dribble into the lungs and they get respiratory distress often with eating. 01:39 So this is fistula without any atresia compared too the last one, which was an atresia without any fistula. 01:46 There are two other very rare types that you might hear about. 01:50 One is where the proximal esophagus feeds into the trachea. 01:54 There is no path to the stomach. 01:57 The other is the same except there is a path to the stomach, the proximal esophagus enters the trachea and then the distal esophagus arises from the trachea a little bit farther down. 02:10 When we see TEF, about half of patients will have an associated anomaly. 02:16 An example might be CHARGE syndrome. 02:19 In CHARGE syndrome, they may have coloboma as you can see in this patient here with that black pupil that’s extending down in the patient’s left eye. 02:28 They may have heart defects or an atresia such as choanal atresia. 02:33 Or they may have retardation or what we like to call intellectual disability. 02:38 They may have genital malformations or they may have ear anomalies. 02:42 CHARGE, C-H-A-R-G-E, and those are symptoms they may have. 02:47 They may also have tracheoesophageal fistula. 02:51 Another defect more classically associated with tracheoesophageal fistula is VACTERL. 02:57 Again, each of these letters count for a symptom that these patients have. 03:01 V is vertebral defects. 03:03 A is anal atresia. 03:05 C is cardiac defects, particularly a VSD and the TE stand for tracheoesophageal fistula. 03:14 They also have renal anomalies or malformations and they have limb defects such as radial dysplasia, polydactyly or syndactyly. 03:24 So most TEF presents almost immediately after birth. 03:30 These patients have food that cannot get into the stomach in most cases. 03:35 This results in immediate emesis and rapid dehydration outside of the uterus. 03:41 Additionally, gastric contents may enter the lungs resulting in respiratory distress. 03:49 So the diagnosis of TEF is usually made because it’s impossible to get the NG tube into the stomach. 03:56 These infants are sick. 03:58 We place an NG in and we can’t get it into the stomach. 04:01 Instead it coils up in the proximal esophagus. 04:04 So we put in the NG, we take an x-ray and, wow, look at that NG, it didn’t go in. 04:09 Maybe this child has a TEF. 04:12 Alternatively we can make a more definitive diagnosis by doing endoscopy. 04:18 We scope, we look down there, it’s a blind loop. 04:22 So the H type fistula is the one I think that comes to mind the most often because it’s more subtle. 04:31 This is only four percent of all cases of TEF. 04:35 But this one can present later on in life. 04:38 It’s basically a fistula that’s small. 04:41 So there can be a delay in diagnosis. 04:44 Patients present with coughing, wheezing, and struggling with feeds and reflux. 04:51 As you can see in this picture, the food goes down the esophagus and then somehow gets into the trachea and can cause problems. 04:59 Some of the food keeps going. 05:03 So that’s my summary of TEF in children. 05:07 Thanks for your time.
About the Lecture
The lecture Tracheoesophageal Fistula (TEF) by Brian Alverson, MD is from the course Neonatology (Newborn Medicine). It contains the following chapters:
- Tracheoesophageal Fistula (TEF)
- CHARGE Syndrome and VACTERL
Included Quiz Questions
What is the most common type of tracheoesophageal fistula?
- Proximal esophageal atresia with fistula between distal esophagus and trachea
- H-type fistula
- Atresia without a fistula
- Proximal esophagus feeds into trachea without a path to stomach.
- Proximal esophagus enters trachea and distal esophagus arises from trachea further down.
How many types of tracheoesophageal fistula are there?
- 5
- 1
- 2
- 3
- 4
Which type of tracheoesophageal fistula is most likely in a neonate who presents with early drooling, choking, and inability to feed and the presence of air in the stomach on X-ray?
- Proximal esophageal atresia with fistula between distal esophagus and trachea
- H-type fistula
- Atresia without a fistula
- Proximal esophagus feeds into trachea without a path to stomach.
- Proximal esophagus enters trachea and distal esophagus arises from trachea further down.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Awesome lecture! I'm grasping better the concepts by first watching these vids and then reading my books. Thanks
Another great lecture. I think this diagnosis is very important to have in mind when a neonate presents with feeding difficulties and/or respiratory distress.