Playlist
Show Playlist
Hide Playlist
Tinea Infections: Management
-
Slides Fungal Skin Infections.pdf
-
Reference List Dermatology.pdf
-
Download Lecture Overview
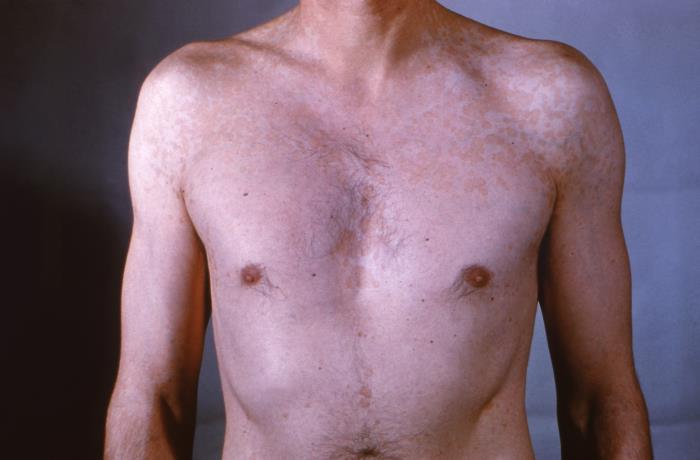
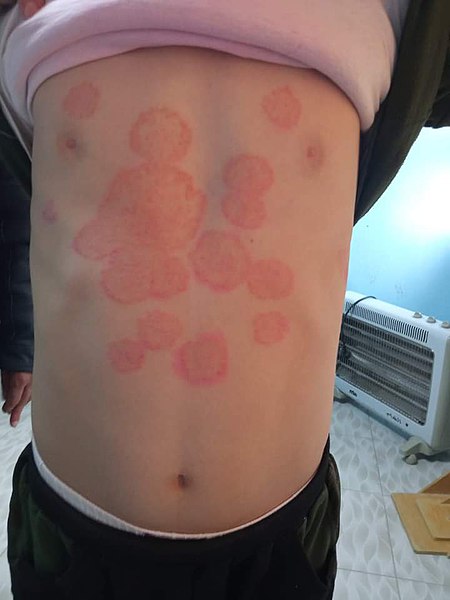
00:01 So we're left with either tinea corporis or the early herald patch of pityriasis rosea. 00:07 Now I'll remind you, pityriasis rosea is not caused by a fungus whereas tinea corporis is. 00:14 So if we can perform some sort of test that will highlight that there's fungus present versus there isn't one, that may really help us with the diagnosis. 00:22 So our test of choice will be to get a scalpel blade, scrape a small amount of that scale onto a slide, and then put a drop of 10% KOH on a slide, add a coverslip and voila, we've got a KOH prep which should really clinch the diagnosis. 00:38 Here we can see evidence of a dermatophyte infection with numerous filamentous branching hyphae and spores. 00:46 Final diagnosis: tinea corporis. 00:51 Alright, let's just review a few key points from our case. 00:54 So our patient's a lacrosse player. 00:56 You know anybody who's playing contact sports, hanging out in the gym with a whole bunch of other guys who are not wearing their shirts, they're gonna be at risk for spreading tinea around. 01:06 So that's a possibility. 01:07 The lesions being itchy and circular, that's a classic presentation for tinea corporis. 01:13 'Ringworm', like I said, past one or two weeks, that's the typical onset for a tinea corporis infection. 01:19 The absence of diabetes is not as concerning in a patient who's a young guy hanging out in a sports locker room. 01:26 But certainly if he had diabetes, that would make a higher risk that he could develop any number of fungal infections particularly candida as I mentioned before. 01:33 And again the lesion itself: singular, raised, annular, erythematous, irregular border, central clearing, that's a good picture of tinea corporis. 01:43 How are we gonna manage it? We pretty much manage all tinea infections similarly, with a caveat we'll get to. 01:49 So tinea cruris, which is around the groin. 01:52 Tinea pedis around the feet, tinea corporis, tinea barbae around the beard line - you're just gonna use topical azoles, you can get away with topical shampoos - ketoconazole creams, that sort of thing. 02:04 It turns out that tinea capitis, much more difficult to treat particularly since it can progress to a cicatricial or scarring alopecia. 02:12 Onychomycosis, when those nails are infested with these fungus, it's a lot trickier to treat it with just something topical so we oftentimes need to use an oral -azole like I said - fluconazole, ketoconazole, etcetera or potentially, terbinafine especially for the toenails. 02:30 Nystatin, well we often think of nystatin as our first line medication for fungal infections, does NOT work against tinea. 02:37 That's really your agent of choice for candida infections And lastly, you want to encourage the patient to you know, use good hygiene keep the area dry, maybe with just baby powder in certain areas that oftentimes get sweaty can do a lot of service just to keep the area dry and control other risk factors as well.
About the Lecture
The lecture Tinea Infections: Management by Stephen Holt, MD, MS is from the course Skin Infections.
Included Quiz Questions
Which of the following medications is best used for the treatment of tinea capitis?
- Terbinafine
- Topical azoles
- Nystatin cream
- Topical steroids
- Oral dicloxacillin
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |