Playlist
Show Playlist
Hide Playlist
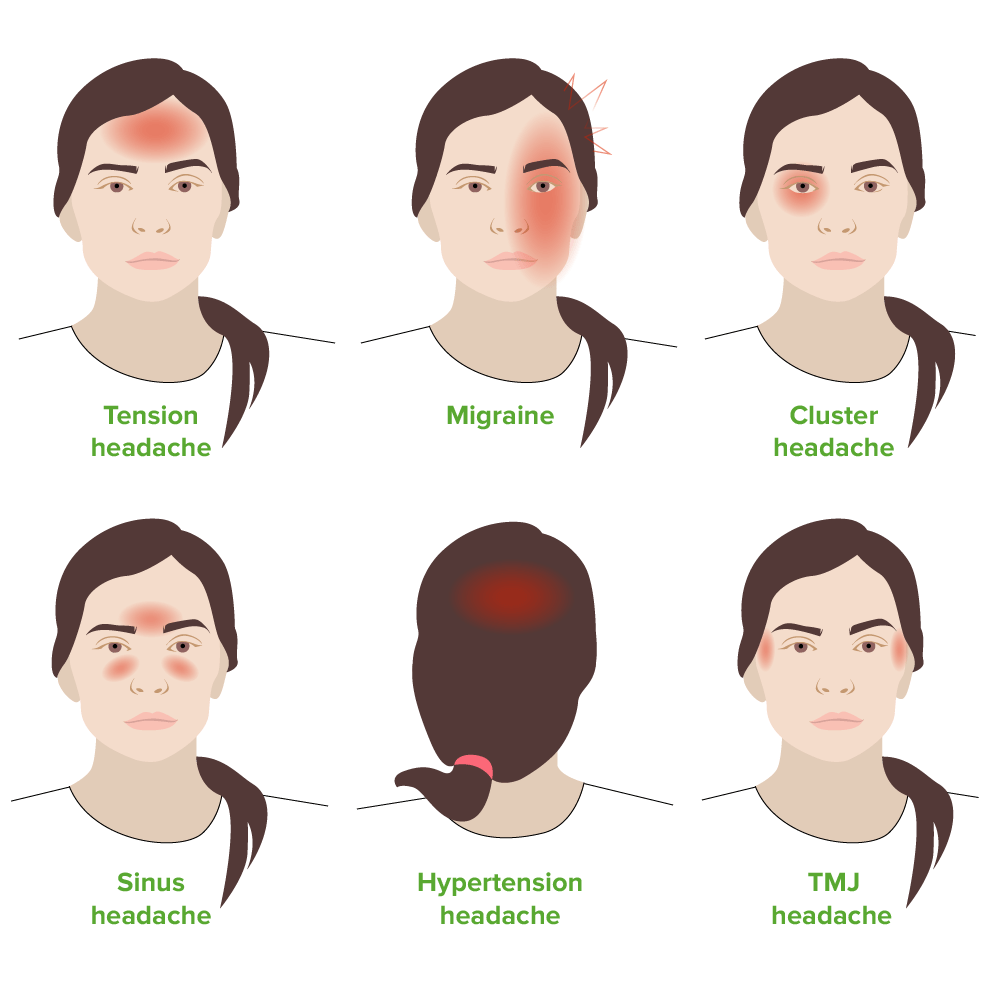
Tension-type Headache and Acute Migraine Headache: Management
-
Slides Headache AcuteCare.pdf
-
Download Lecture Overview
00:01 For tension-type headaches, treatment includes over-the-counter analgesic. 00:05 Those are generally going to be effective. 00:07 Acetaminophen, NSAIDs, not really a difference in terms of efficacy. 00:11 Prefer acetaminophen for safety. 00:13 And really, you want to think about limiting the use of rescue medications for all of these types of headaches because we think about those main categories of tension and migraine, but actually right behind them is medication rebound headache or analgesic rebound headache. 00:30 Anything that’s used for acute analgesia, in this case acetaminophen or NSAIDs, in migraine’s case can be ergot medications or triptans, overuse of those products can promote a rebound headache, which is a difficult thing to get out of because it cycles. 00:46 You take your take your analgesic, you get some relief, but then the headache comes back, so you take more analgesics and it's a self-propagating cycle that can really be debilitating for patients. 00:57 Therefore, if patients have frequent tension-type headaches, consider prevention, consider prophylaxis with a drug like amitriptyline, low dose, can be effective for prevention of tension-type headaches and break that analgesic overuse cycle. 01:13 But SSRIs don't really work. 01:15 Other types of treatment that work for tension headaches, biofeedback and relaxation therapy can be effective. 01:20 Psychotherapy can be effective and even acupuncture has been shown to be effective as well. 01:24 So, there’s some non-medical options for patients with tension headache because everybody's had at least one tension headache in their lifetime. 01:33 For acute migraine headache, over-the-counter NSAIDs are frequently effective, so that's a good place to start, particularly if the pain is not that severe. 01:42 But 24 hours later, many times the pain might be returning. 01:46 You’re going to use behavioral treatment and recommending rest and lowlight for everybody. 01:51 Triptans are, I think, the most commonly used acute analgesic for migraines specifically. 01:58 In terms of Triptans, they’re all similarly effective. 02:01 There is not one that really stands out from the others in terms of efficacy. 02:04 So, therefore, the route of administration is really important. 02:08 Oral drugs may not be tolerated among a patient who is really nauseous and vomiting, so there are other options. 02:16 Obviously, subcutaneous injections, but also nasal spray formulations of drugs that can be – not only avoid that GI pathway, but also can work a little bit faster for patients with severe symptoms. 02:31 So, it’s really the route of administration I think trumps the actual drug in terms of its efficacy because they all work about the same, but they also have similar warnings in terms of avoiding among patients with active cardiovascular disease and really being careful of using triptans among patients taking SSRIs as both those agents can increase serum serotonin levels and promote serotonin syndrome. 02:58 So, migraine prophylaxis, here’s something that’s very nderused, yet highly effective. 03:03 When the headache frequency is at least twice a week, it's time to think about prophylaxis because, again, patients get in the cycle of these analgesic overuse type headaches and these rebound headaches. 03:15 And the number needed to treat among patients with migraine frequent headaches is really low. 03:22 If you treat 10 patients, 2 to 4 are going to have a significant reduction in their headache frequency of 50%. 03:29 So, it doesn't take much to make a big difference in terms of headache frequency. 03:33 And prophylaxis can also reduce severity of the headaches as well. 03:37 How do you initiate prophylaxis? What do you use? Beta blockers tend to be one of the most popular choices. 03:42 Generally, they’re pretty well tolerated and you don’t need high doses in order to have efficacy against migraine. 03:48 Similar for tricyclic antidepressants which can be associated with more side effects. 03:53 Topiramate can be used as well. 03:56 It may be a little bit more expensive and it’s also associated with some side effects. 04:00 And divalproex, very similar. 04:03 Other agents to consider, there's a lot of different options. 04:07 Some studies have shown that gabapentin is effective. 04:09 Other studies have shown that calcium-channel blockers are effective. 04:13 The four that I listed here, beta blockers, TCAs, topiramate, divalproex are the ones that have probably the strongest trials demonstrating efficacy. 04:23 But if one doesn't work, you can switch to the other. 04:26 I would recommend that instead of just giving up altogether because these patients really do suffer. 04:31 And these drugs can really be quite effective for reducing headache severity and frequency as well. 04:38 Calcitonin gene-related peptide antagonists are a newer group of medications which may also be considered when other therapies are contraindicated or ineffective. 04:50 And with that, I hope that – again, we all have headaches, so you’ve learned how to manage your own headaches a little bit better, but certainly with your patients as well. 04:59 Thanks.
About the Lecture
The lecture Tension-type Headache and Acute Migraine Headache: Management by Charles Vega, MD is from the course Acute Care. It contains the following chapters:
- Tension-type Headache
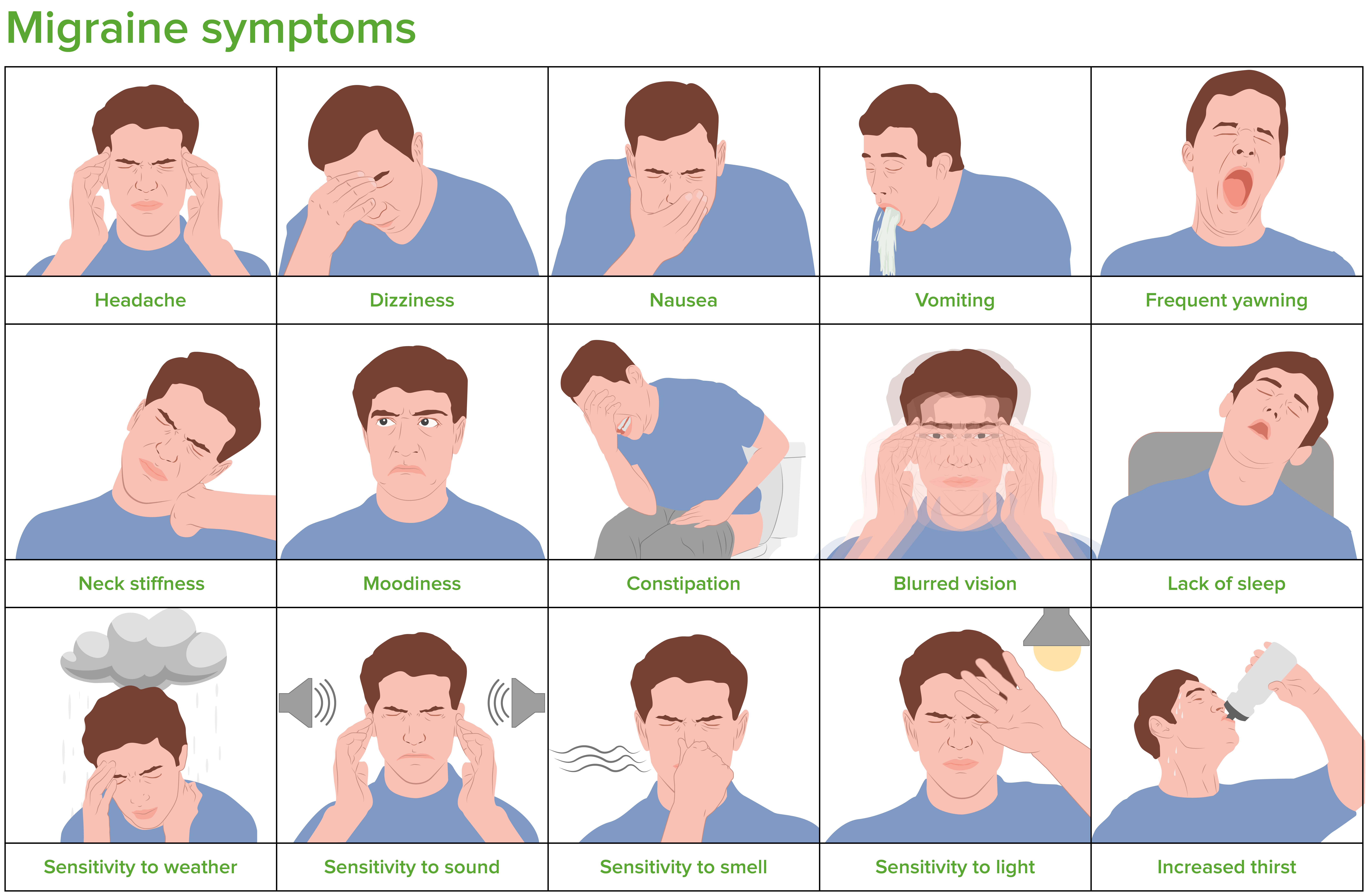
- Acute Migraine Headache
Included Quiz Questions
Which of the following is the most appropriate first-line treatment for tension-type headache?
- Ibuprofen
- Caffeine
- Ibuprofen + caffeine
- Diphenhydramine
- Intramuscular ketorolac
Which of the following medications is NOT typically recommended for migraine prophylaxis?
- Fluoxetine
- Beta blockers
- Tricyclic antidepressants
- Valproate
- Topiramate
Which of the following medications is most appropriate in migraine headache that does not respond to nonsteroidal anti-inflammatory drugs?
- Sumatriptan
- Intramuscular ketorolac
- Valproate
- Amitriptyline
- Topiramate
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |