Playlist
Show Playlist
Hide Playlist
Smooth Muscles: Structure Function
-
Slides 03 SmoothMuscle MusculoskeletalSystem.pdf
-
Download Lecture Overview
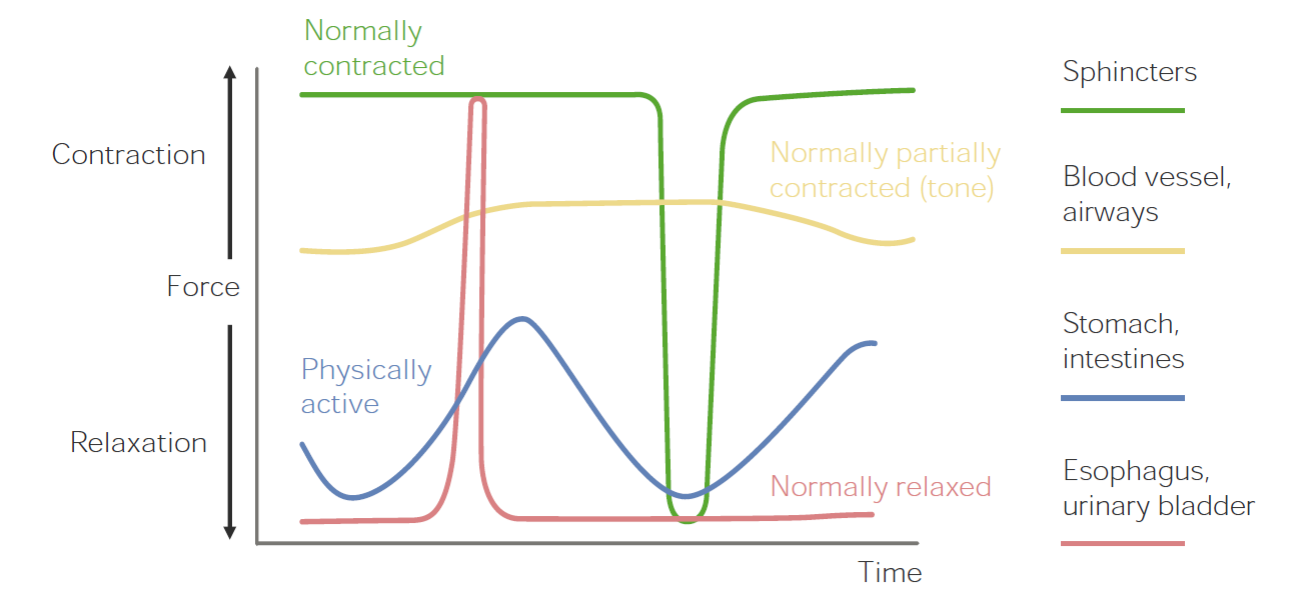
00:01 You can see smooth muscle is named because it’s non-striated appearance. 00:07 Striations will be lines that occur. 00:10 And when we went through the skeletal muscle, you noticed that there were varying components that you can see individual lines in the muscle itself. 00:19 Why this occurs is because there are a number of different processes. 00:24 Smooth muscle has a larger degree in which it can shorten. 00:28 So a smooth muscle can shorten to a greater degree than skeletal muscle. 00:34 They also have a large number of intermediate filaments that help maintain its structural integrity. 00:40 They have thick filaments and thin filaments just like skeletal muscle. 00:46 They also have these dense bodies and these dense bodies help maintain that structural relationship of thick and thin filaments. 00:56 The other thing that’s different is they are mechanically coupled at least in the single unit or phasic smooth muscle via gap junctions. 01:05 It can be seen here. 01:08 Now, let’s talk through the various ways in which smooth muscle develop force as which there are a number. 01:15 The first we’ll talk through is in this type of graph where we have force on the Y-axis and time on the X-axis. 01:26 This is one type of force production in which force production is high almost all the time until you see a relaxation and then it returns back to a high amount of force. 01:39 The good example for this are sphincters in which they are normally contracted and then relaxed for a very short period of time and contract again. 01:51 Other types of smooth muscle work almost in the opposite way in which they are normally relaxed and then they have bursts of activity and then they go back to a relaxed state again. 02:03 A good example of that is urinary bladder tissue in which it’s relaxed most of the time until one wants to urinate. 02:12 Other types of smooth muscle have a partially contracted state almost all the time, and therefore, they have a tonic tone. 02:22 They can constrict to a greater degree, but then will relax only a small amount. 02:28 Good examples of these are blood vessels, where there always will be a tonic amount of vasoconstriction and then you can still vasoconstrict more, but there will be a tonic kind of contracted state. 02:41 And then finally, we have very active type of smooth muscle and where there are lots of oscillations. 02:48 These oscillations are oftentimes driven by such things as slow waves in the GI system. 02:55 These can be phasically active and intestinal muscle is a great example in which you get waves of contraction and relaxation, contraction and relaxation, but the relative force is pretty low. 03:09 So combining all of these together, you can see that smooth muscle has a wide range of functions and that’s probably why it’s present in so many different tissues because it could be contracted normally, partially contracted, phasically active, or normally relaxed. 03:29 How do you get a muscle to contract in terms of smooth muscle? There are two primary ways. 03:37 The first way is via causing an electrical potential across the membrane, which opens up calcium channels to cause calcium-induced calcium release. 03:48 So calcium enters in through the cell from the extracellular fluid into the cell, which engages a calcium channel to release more calcium. 03:58 So that’s done via an electrical mean. 04:02 The other way to do it is by using a ligand or a particular substance to bind to a receptor. 04:08 So good examples here are things like hormones and neurotransmitters that can bind to specific receptors to cause an enzymatic second messenger signal pathway to release calcium into the cell. 04:23 So let’s go through those two in a little bit more detail. 04:26 So let’s go through calcium-induced calcium release. 04:30 Oftentimes, these L-type calcium channels are located in small invaginations in smooth muscle. 04:36 These are located in close proximity to calcium-induced calcium release channels of the SR. 04:43 SR is the sarcoplasmic reticulum. 04:45 Therefore, once there’s a membrane potential change, these calcium channels open to allow little calcium influx into the cell. 04:55 Once the small amount of calcium enters the cell, it activates this calcium-induced calcium release channel to spill out lots of calcium. 05:05 So the calcium that comes into the cell isn’t really involved with the contraction to a great degree. 05:11 The most of the contraction is induced from what is released from the SR. 05:16 That can be seen here right below the caveolae. 05:24 Now, a ligand-gated contraction, seen up here, can be done via again a hormone or a neurotransmitter activating let’s say a G-coupled protein receptor, and the example that we have here activates phospholipase C, which is an enzyme, and that converts a number of substances, but it creates IP3 and DAG, and it’s IP3 that then goes to the SR to bind to an IP3-gated channel to open up to allow calcium afflux into the cytosol. 05:58 So both of these two mechanisms both involve calcium in the cytosol but how they get it out is via a different mechanism: one through calcium-induced calcium release and the other one through an enzymatic process involving phospholipase C and IP3. 06:19 There are a number of calcium-binding proteins that are located in smooth muscle that help regulate its function. 06:26 These smooth muscle-binding proteins will help activate to cause contraction to occur, as well as there are calcium-binding proteins that are there to help sequester calcium or to bind it up so it’s not in its free form. 06:42 Graded contractions are a telltale sign of what smooth muscle does. 06:48 You can have a little calcium release and get a little contraction or a lot of calcium release and get a lot of contraction. 06:55 So it’s all graded by the amount of calcium release, whether it’s done via calcium-induced calcium release or whether it’s done via an IP3 mechanism.
About the Lecture
The lecture Smooth Muscles: Structure Function by Thad Wilson, PhD is from the course Musculoskeletal Physiology.
Included Quiz Questions
Where in the myocyte are the smooth muscle calcium-induced release channels located?
- Sarcoplasmic reticulum
- Plasma membrane
- Caveolus
- Peroxisome
- Mitochondria
Which of the following is NOT a feature of smooth muscle?
- Striations
- Increased intermediate filaments
- Increased gap junctions
- Membrane dense bodies
- Thick and thin filaments
Which of the following initiates the activation of IP3 pathway in the sarcoplasmic reticulum?
- Hormonal activation of a GPCR
- Calcium influx
- Release of DAG
- Increase in ATP
- Use of PLC
Which of the following is usually contracted in a normal state?
- A sphincter
- Large intestine
- Urinary bladder
- Small intestine
- Stomach
Which of the following statements are FALSE regarding smooth muscle contraction?
- Calcium-binding proteins are found on the outer surface of the smooth muscle cell membrane.
- Either calcium-induced calcium release or ligand-mediated calcium release can be used by smooth muscle for contraction.
- The amount of calcium released dictates the amount of contraction.
- Smooth muscle can be in a contracted state, partially contracted, phasically active, or relaxed.
- L- type calcium channels are commonly located in caveolae.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |