Playlist
Show Playlist
Hide Playlist
Scars
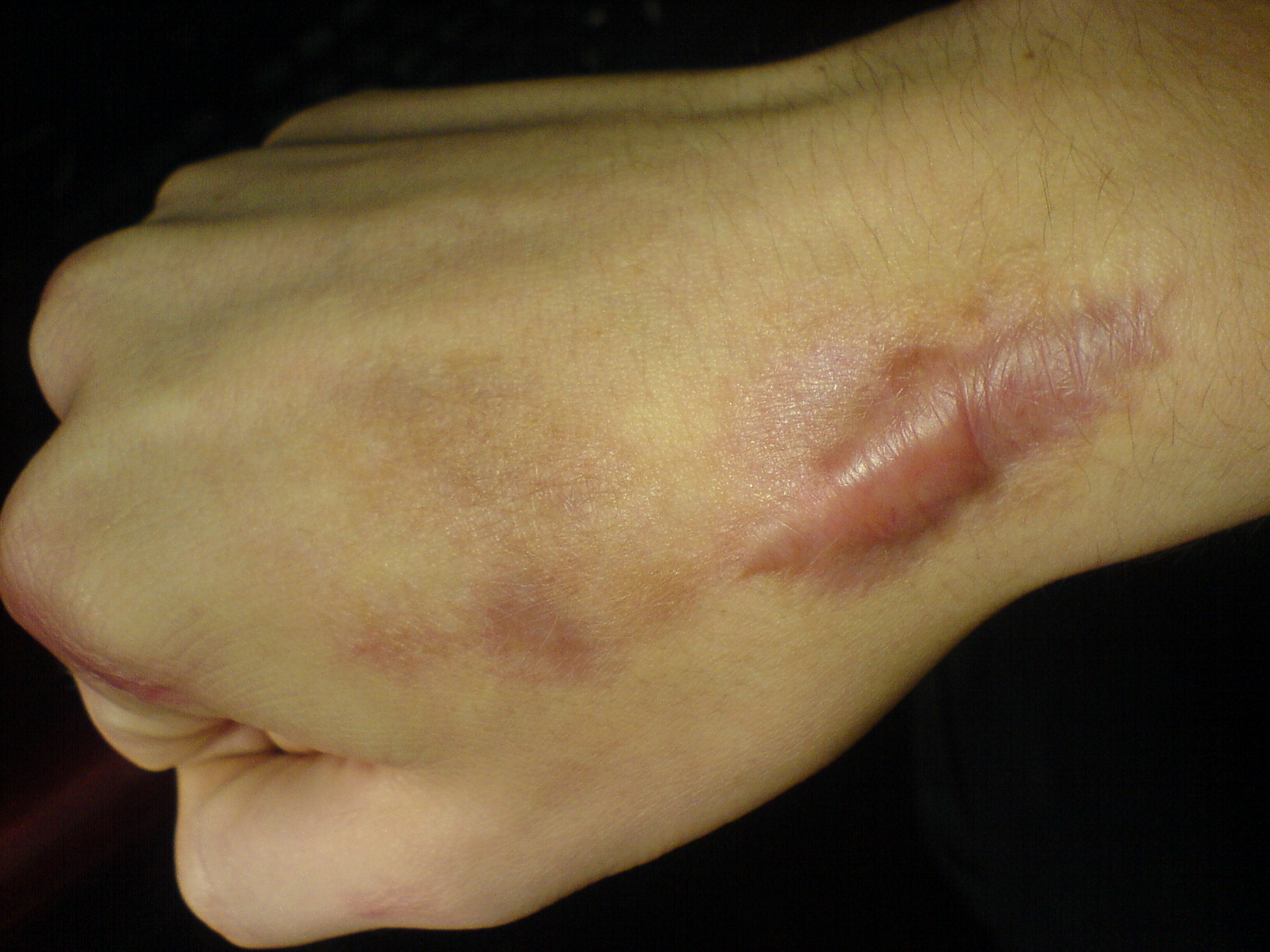
00:01 Lifting head and flexing the hip simultaneously. 00:02 We touched upon it very briefly. What's the top one? Keloid. And what's the bottom one? Hypertrophy. That's from CABG and that’s from an acne. But in your exam they will give you any sort of trivial surgery or a trivial trauma to the skin resulting in a keloid scar. 00:29 Now, so they'll give you a scenario which would be something along these lines. 00:35 The patient had ear lobe piercing or some form of surgery a few months ago or a year ago. 00:46 On the shoulder or one of the sites they will give you sternum or shoulder, and they'll give you a -- African. Same thing, the dark skin. Same thing, they'll give you, the two options would be hypertrophic and keloid. Okay. As I said, these pathology questions are final medical student level. Only the anatomy is slightly different, the physiology, pathology you'll be absolutely fine with your basic knowledge. There's nothing really new in these things. Okay. So keloid outgrows original scar, it can develop up to a year later, predilection for the sternum, shoulder and ear lobes. And hypertrophy is different. Diagnosis? Yes, neurofibromatosis. Neurofibroma. 01:55 What are the associations? What does it associated with? Von Recklinghausen's. 02:03 What else? Multiple endocrine neoplasias. So, Neurofibromatosis I, Neurofibromatosis II, and MEN I, MEN II. Now, I really don't understand how you remember this, but if you can remember this MEN I, II and IIA. People have told me different ways to remember, I still forget it. But you need to know this, part A and part B, they ask you multiple endocrine neoplasias. Does anybody know a way to remember it? Three Ps, two Ps one M, and then two Ms, one P. The mnemonic, for instance, MEN I has got three Ps. MEN IIA has got two Ps, one M. And then MEN IIB has got, I don’t know where the third M come from. But two Ms and one P. Basically, yeah MEN I is the pancreatic, and then above in the neckline, parathyroid and pituitary. 03:10 MEN IIA and IIB are your pheos, and then it just depends whether you’ve got, again neck, so the parathyroid or whether you’ve got marfanoid. So Marfan’s is MEN IIB, actually. 03:26 It’s quite simple when you actually learned it. If you’ve got a pheo, you’re a II of some form. 03:31 Then IIB is your Marfan’s and a pheo. And IIA is your parathyroid and your pheo. 03:39 So remember two Ps, remember pheo, IIA? I don’t know how to describe it. 03:51 No, no. You are right. So three Ps yeah. 03:53 So II is your pheos. You know for a fact IIA has got two Ps and you know it’s got parathyroid and pheo. And IIB is a pheo but it’s Marfan’s as well. If there’s no pheo, it’s MEN I. Okay, correct. You are right. You know, I could not really feel how to remember this. But I suppose, as she said three Ps go for MEN I. Okay, but you need to know the MEN syndromes. 04:46 Now very quick. What is the diagnosis? Dupuytren's. This is why, the reason for the slide; you'll get a -- No, in this question? Yes, high serum lipids is the wrong answer. 05:15 There are all risk factors, all others are risk factors for Dupuytren's. Okay. And this is quite important. Commonly quoted but no evidence. So in your exam, they have taken this off now. So it's very unlikely they're going to confuse you with this because I'm sure some of you may know Professor McRoger. He's retired now, he was a plastic surgeon here in Manchester. They did a lot of study and they clearly identified there is no relation between any of those. So they wrote to the college and the old questions have been removed which said vibrating tools, phenobarbitone, alcoholic liver disease. There's no evidence. 06:00 Even in the Oxford handbook it says, but in the new guidelines, these are the only four things, race, male sex, diabetes, positive family history. Only the four things have got a clear evidence or a clear correlation. So be careful when you get in the exam, if you get alcohol, epilepsy, phenobarbitone, think well what are they really coming at. 06:29 You know this, don't you? What are the things you will examine in the hands? What else, plantar fibromatosis, penile fibromatosis, relation with Duputyren’s. Management. Okay you know all this. Conservative. What's next? What is a new -- Yes, this is the one. Clostridial collagenase. Okay, so this is coming up in the exam now. What is the most appropriate treatment in a patient with early stage Dupuytren's? You can go for clostridial collagenase. 07:24 If you have a single digit disease, a little bit of flexion, you can avoid surgery just by injecting a little bit of collagenase and physically pushing it down, breaking the collagen. 07:37 So that has become the newer modality and the more on the first line management. 07:46 Yes, because you always have these options, don't you? You can always do the fasciotomy, fasciectomy or dermofasciectomy. But this is a newer one which has been introduced in the exam now. I think this is still the order. If you can avoid the collagenase, you can avoid it. So if you are able to splint it, and do some physio and try to straighten the finger, fair enough. But it doesn’t really work. We always give them night splintage and all those, but very little evidence to show it works. 08:26 So this is quite accepted in the exam now, clostridial collagenase. It's licensed as Xiaflex. Amputation, you can use it as a last option.
About the Lecture
The lecture Scars by Stuart Enoch, PhD is from the course Medical Scenarios.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |