Playlist
Show Playlist
Hide Playlist
Resulting Condition: Hereditary Spherocytosis
-
Slides Cellular Pathology - Interface with the Outside World.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
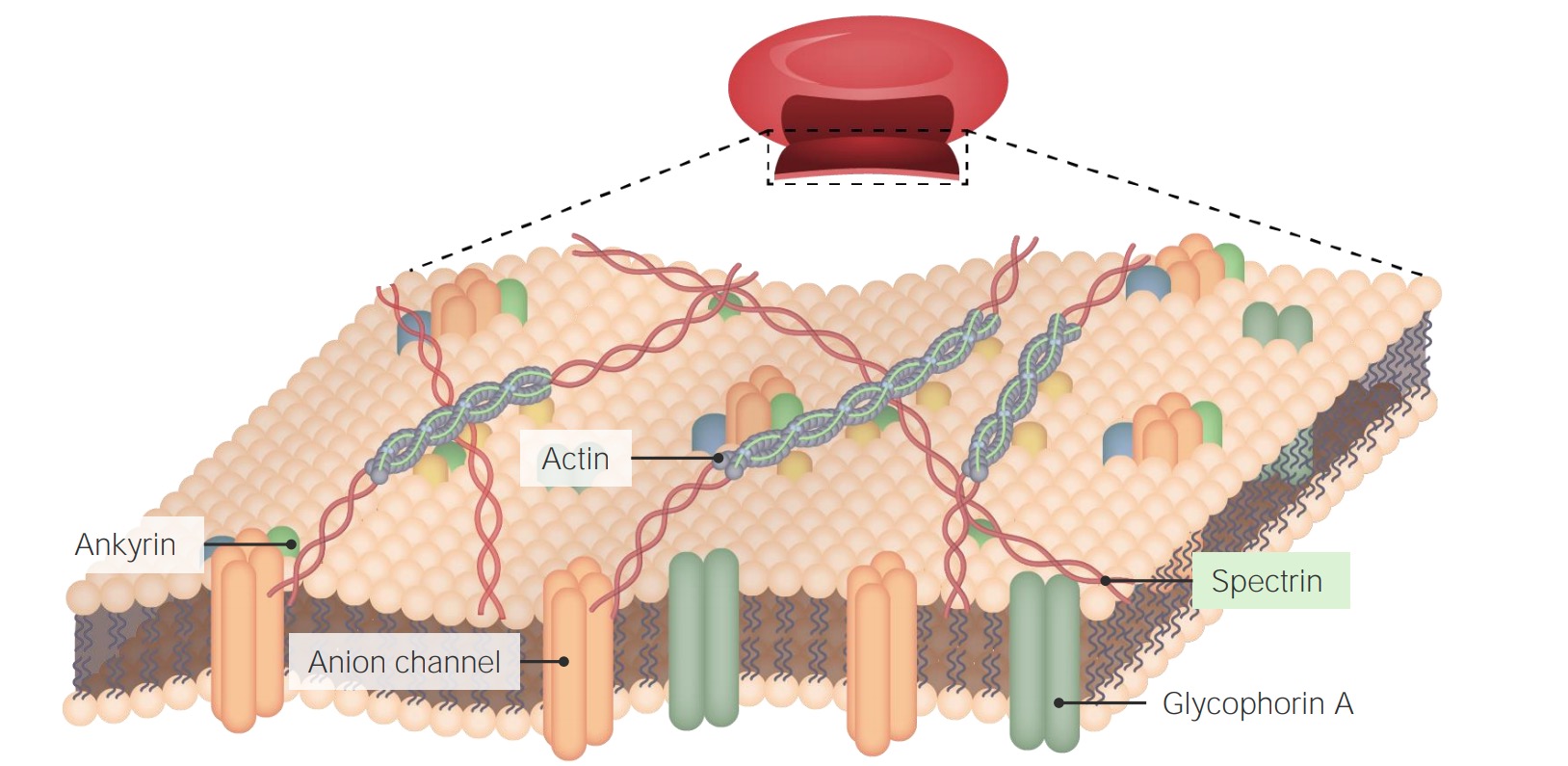
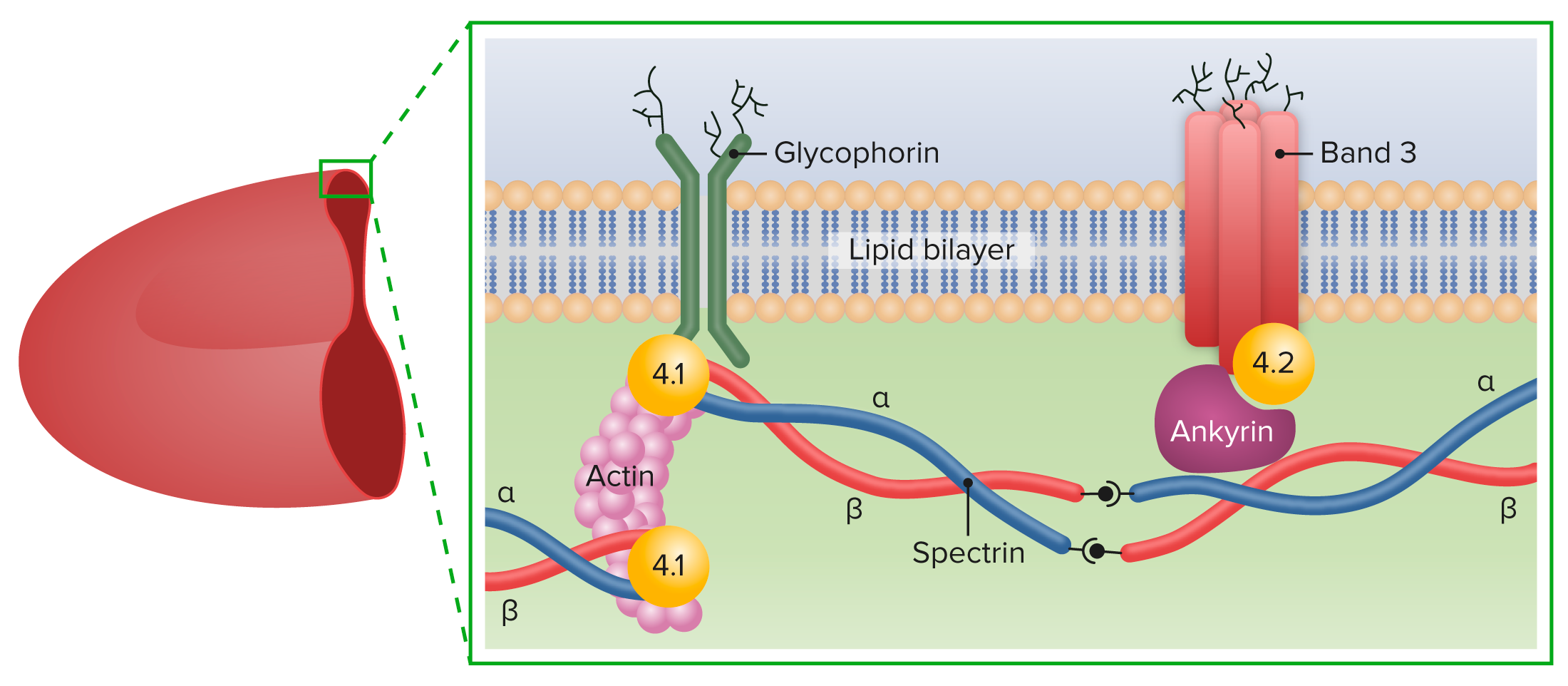
00:01 If you don't have normal levels of spectrin or normal transmembrane proteins, you get a disease. 00:08 Okay, so again, structure, biology, it makes a difference. 00:12 This disease is hereditary spherocytosis. 00:15 It turns out it's the most common hemolytic disease, meaning that the red cells lyse genetic hemolytic disease of the European and American -- North American population. 00:28 Okay, it's an autosomal dominant hemolytic disorder, meaning the red cells lyse. 00:34 Why does that happen? Well, we have defective spectrin synthesis. 00:38 Remember, spectrin was one of those springy things in between the transmembrane proteins holding the inner peripheral configuration. 00:45 When we don't have adequate spectrin, we don't have a normal biconcave disk. 00:50 You can also have defective ankyrin or protein 3 and some of the other ankyrin proteins. 00:55 You have reduced -- as a result of this, reduced membrane stability, and as they go through capillaries, these cells tend to rupture. 01:04 So, on the left is shown kind of a normal appearance of a peripheral smear. 01:08 The cell in the middle with blue things in it, that's a neutrophil. 01:12 We'll spend more time with Mr. Neutrophil in subsequent talks. 01:16 But around it are a whole bunch of erythrocytes. 01:18 And erythrocytes have that central area of power where it looks whiter, and that's because it's a biconcave disk. 01:24 So, when you're looking through the middle of it, there's not much hemoglobin. 01:28 Okay, that's normal. 01:30 On the other side is a patient with hereditary spherocytosis with a spectrin deficiency. 01:35 And we don't have nice biconcave disk, we've got round cells. 01:40 In fact, maybe the round cells are -- some are normal size, but some are much smaller. 01:45 And that's because as they've gone through capillaries, they've been sheered off. 01:50 Portions of this, membrane have been sheered off. So, this is a hemolytic disorder. 01:55 One protein. And in fact, the protein synthesize. 02:00 It's just not synthesized in the normal amounts or it's got kind of a point mutation in it that limits its ability to interact with the transmembrane proteins. 02:09 So, it's -- forms spheroidal, non-deformable, rigid, little erythrocytes that get sheered off, and patients present with jaundice. 02:19 They're constantly breaking down red cells, so they're constantly making a lot of bilirubin that they can't clear. 02:24 So, we're looking at the sclera of this gentleman's eyes, and it's yellow because of jaundice, too much bilirubin. 02:30 As we break down the hemoglobin from all these red cells that are rupturing, we're also going to make gallstones. 02:38 So, bile-associated, hemoglobin-associated, heme-associated gallstones. 02:43 Clearly, the patients are gonna be anemic. 02:46 They're gonna be short of breath, they're gonna be fatigued. 02:48 They will have all the other problems. 02:50 And interestingly, because the marrow is in overdrive to try to make up for all the rupture of the red cells, you can get aplastic or hemolytic crises. 03:00 So, an intercurrent infection can cause the marrow to just say, "Forget it. It's not gonna do anything." And that becomes an aplastic crises where you're not making any components of the marrow. 03:10 Or you can have hemolytic crises where you have subtle changes in the ionic environment or in temperature that will cause hemolysis all at once. 03:19 So, a patient will have a normal hematocrit of 35% and suddenly go down to 20%.
About the Lecture
The lecture Resulting Condition: Hereditary Spherocytosis by Richard Mitchell, MD, PhD is from the course Cellular Housekeeping Functions.
Included Quiz Questions
What is the etiology of hereditary spherocytosis?
- Defective spectrin synthesis
- Loss of complement inhibitory proteins
- Autoimmune-mediated destruction of the red blood cells
- Abnormal structure of the hemoglobin molecule
- Impaired protection against oxidative stress
What is the morphologic hallmark of hereditary spherocytosis?
- Spheroid, rigid erythrocytes
- Heinz bodies
- Macrocytosis
- Increased central pallor
- Schistocytes
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |