Playlist
Show Playlist
Hide Playlist
Rapidly Progressive Crescentic Glomerulonephritis
-
Slides KidneyDisorders RenalPathology.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
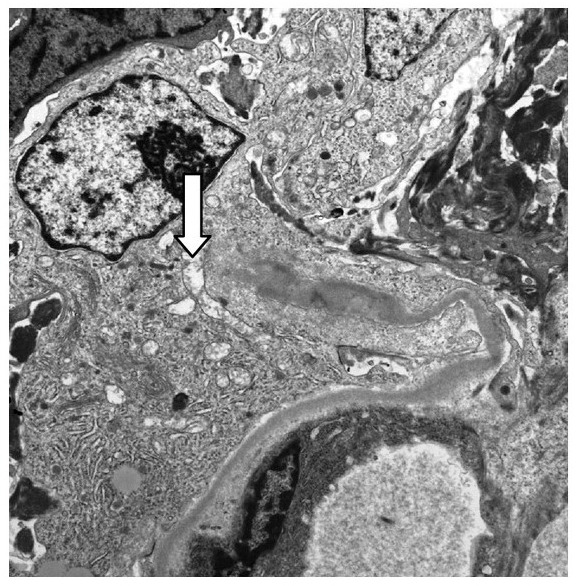
00:01 Rapidly progressive crescentic glomerulonephritis, rapidly progressive glomerulonephritis. 00:07 I want you to get in the habit of thinking of RPGN as having crescentic cells. 00:15 It doesn’t have to all the time but remember, in the clinical vignettes that you’ll be reading and such, they want you to get the diagnosis, you just have to know as to what you’re looking for. 00:25 Now, a couple of things that are important, number one, clinical syndrome, syndrome, syndrome, that might be primary, secondary type of glomerular disease. Stop there. 00:35 Syndrome, what does that mean? Syndrome means many causes, right. 00:41 So up until this point if you ever thought that RPGN was coming from only one glomerulonephritis, no, not the case. 00:51 Second point, and this is probably incredibly important. 00:55 I can say and you should know that in terms of classification of your kidney, nephritic or nephrotic, which one do you think it only arises from? And this you can say with certainty that it is nephritic. Is that clear? So when you have your let’s say minimal change disease, focal segmented glomerulosclerosis, some of your nephrotic disorders, those will never go into RPGN. 01:20 Is that understood? Under nephritic, which ones could they be? Well, we’ve got a bunch. 01:24 We have post streptococcal glomerulonephritis, we could have maybe perhaps IgA, maybe we’ll have - you might have known it in the old name or formally known as Wegener, really? It was formally known as Wegener? Correct, so we’ll get into all this upcoming. 01:38 That’s point number one. 01:39 Clinical syndrome might be primary or might be secondary. 01:42 We’ll be spending a lot of time with secondary. 01:45 Next, what is the definition of rapid and I’ve mentioned this a few times. 01:49 The fact that your kidneys are going to go into renal failure, take a look at this. 01:53 Within three months, that’s 12 weeks. That is amazing. 01:57 Would you tell me about diabetic nephropathy and to what point you’d go into renal failure? Decades, decades, years upon years, so the fact that you’re going into renal failure so quickly is extremely, extremely significant. 02:13 Now, let me give you a definition of histology of crescentic cells. 02:17 These crescentic cells are not podocytes. 02:21 Up until now, everything that we’ve done with anything, with immune-complex deposition, later on, we’ll do fusion of your podocytes is your visceral epithelial cell. 02:33 What is this? Parietal epithelial cell. 02:36 What does parietal mean? Remember that picture that I showed you in a cartoon where it was effectively showing the outer layer lining the Bowman’s space and that’s your parietal epithelial cell, they might start undergoing what’s known as crescentic proliferation. 02:53 If they start undergoing crescentic proliferation, what space are they occupying? Bowman’s space. 02:59 What happens to filtration? Gone. 03:00 What happens to kidney? Gone. 03:02 What other associations? We’ll go through a bunch. 03:05 So under RPGN, it’s the first time that we’re discussing any associations. 03:10 These include our Goodpasture, also called anti-glomerular basement membrane disease. 03:17 What kind of immunofluorescence pattern? Good, linear. 03:21 Also, we have our ANCAs which stands for Anti-neutrophil cytoplasmic antibodies, ANCAS, either p-ANCA or c-ANCA. 03:31 Let’s take a look at that crescentic glomerulonephritis. 03:34 Would you take a look at this light microscopy? That’s what this is. 03:38 My goodness gracious, do you find any Bowman’s space? No, not one iota of space. 03:48 So death within three months, welcome to RPGN. 03:54 So here, in the bowman’s space, complete occupation and death of Bowman’s space obliteration of the space by crescentic cells is the definition of RPGN. 04:05 Now, what we are seeing here is actual, a PSGN patient, a poststreptococcal glomerulonephritis with a global hypercellularity in the middle, and then on the outskirts, this patient underwent RPGN changes with crescentic proliferation completely obliterating that Bowman’s space. 04:25 Fifty percent of the entire urinary space is gone, the cells will then encase and compress as you see here, you see the tuft? The tuft is in the middle.
About the Lecture
The lecture Rapidly Progressive Crescentic Glomerulonephritis by Carlo Raj, MD is from the course Glomerulonephritis.
Included Quiz Questions
Which of the following conditions is associated with rapidly progressive crescentic glomerulonephritis?
- Goodpasture syndrome
- Crohn disease
- Ulcerative colitis
- Rheumatoid arthritis
- Scleroderma
Approximately how long can an untreated patient with rapidly progressive crescentic glomerulonephritis survive without hemodialysis?
- 3 months
- 6 months
- 1 year
- 2 years
- 3 years
Where does the proliferation of parietal epithelial cells take place in crescentic glomerulonephritis?
- Bowman capsule
- Loop of Henle
- Distal convoluted tubule
- Collecting duct
- Descending limb of a nephron
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Doctor, you are great! I've been struggling with nephrology for some time, and after trying many sources and attending multiple classes, I can finally say I found something that really makes everything very clear. I'm having some really beautiful days studying now. Thank you!