Playlist
Show Playlist
Hide Playlist
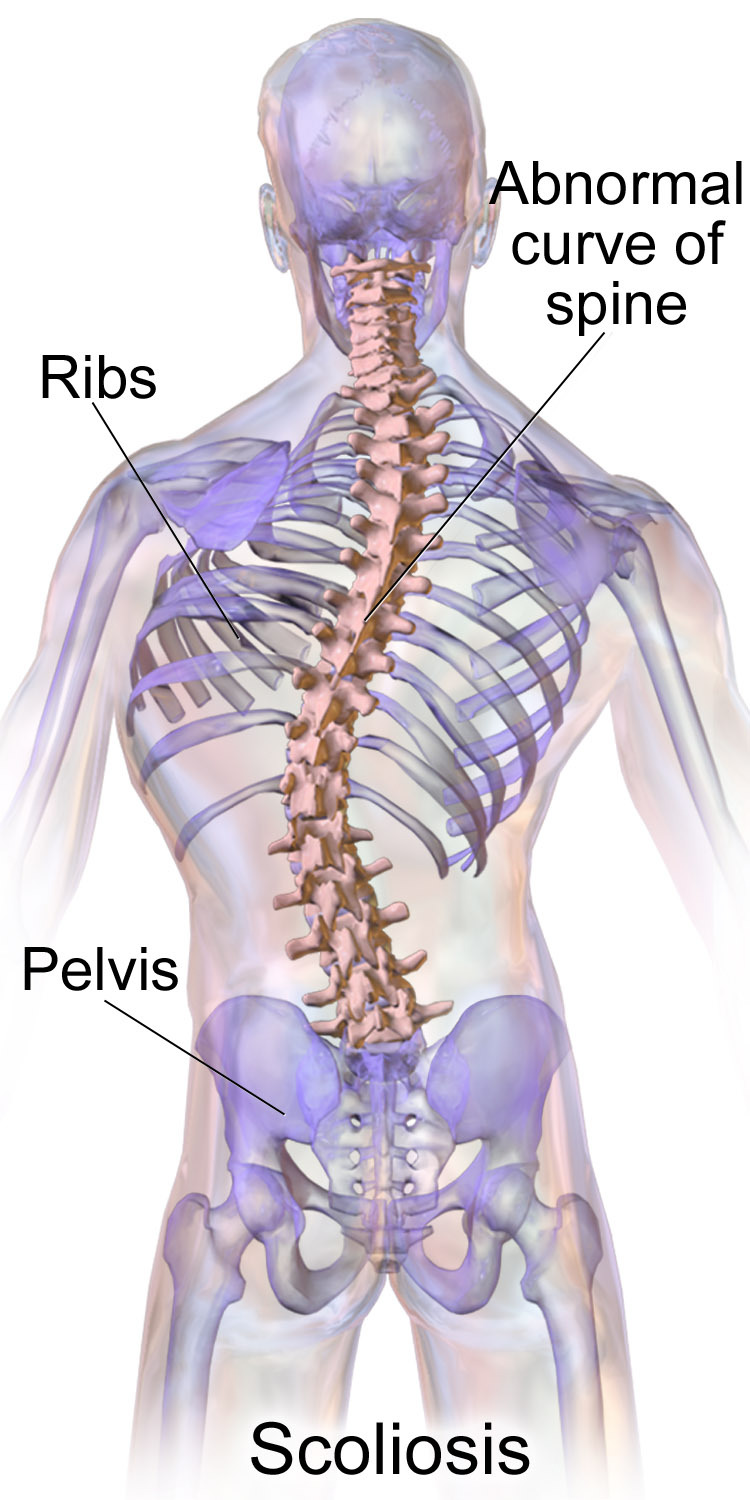
Radiographic Evaluation of Scoliosis
-
Slides Scoliosis.pdf
-
Reference List Osteopathic Manipulative Medicine.pdf
-
Download Lecture Overview
00:01 The radiographs are standardized. 00:03 They are postural - meaning they are weight bearing and they are posterior to anterior. 00:09 The indication is when you have a 7 degree finding on the scoliometer. 00:15 you need to move to an x-ray as well and look for an obvious spinal curve on x-ray. 00:21 The thoracic or lumbar assymetry that you see on physical exam is gonna be different when done with an x-ray. 00:28 And this is an important standardization, an important marker of what's going on with the spine. 00:34 So initial radiograph of scoliosis should be done standing, i.e. weight bearing, full-length that should get the whole spine and give you the relationship of the spine to other areas, and you want tp get a PA and a lateral. 00:47 The PA view minimizes the radiation needed, and it doesn't get the soft tissue of the organ systems so it's safer because you're gonna be doing it on a regular basis. 00:56 and that's the opposite view of a typical chest x-ray which is typically an A-P so it's looking from behind. 01:05 When you get the initial radiograph, it should get the whole spine and the body. 01:12 It is looked at as a single x-ray so you get a good sense of what the person looks like and again, you do not want to do an anatomic x-ray, you don't take the weight off the person, you want it standing, postural so you get a good sense of what's going on. 01:29 The scoliosis will change whether it's weight-bearing or non-weight bearing. 01:33 So again, the standardixation for an x-ray in evaluating for scoliosis is postural. 01:39 It's standing, and it's posterior to anterior. 01:43 For true leg-length discrepancy, not a short leg syndrome, you wanna make sure that that's fixed and treated to help minimize what's going on. 01:52 And if you want to determine the scoliotic curve, you want to fix the leg-length discrepancy before you go ahead and do the x-ray. 02:00 You also can get lateral bending films which will tell you what the functional ability is and over time that will be a good sense of what actions and activities or motions are lost, and it will give you a better sense of when you might need a surgical intervention. 02:14 Here's a description of the Cobb method of radiographic evaluation. 02:18 How do you measure the spine with the x-ray? Where do you put the lines and where do you get the angle? So thpis is gonna show you where you're gonna put the line on the superior border of the highest vertebrae which is where the scoliosis begins. 02:31 And you extend that line towards the concavity of the curvature and where those two lines meet will give you the Cobb angle. 02:41 And the description is right here, and that's how you're gonna go ahead and get the assessment. 02:47 If you wanna check for curve progresson, you wanna get regular P-As and regular measurements of the angle to see how it's changing. 02:56 You also wanna know the convexity and name the scoliosis based on the side that has the convexity. 03:02 You want to identify the apical vertebrae where the curvature starts, and we classify this into cervical C2 to C6, Cervicothoracic C7 to T1, Thoracic T2 to T11, Thoracolumbar T12-L1, Lumbar L2-L4, or Lumbosacral L5 or below. 03:20 A typical curve in adolescent scoliosis is a double courve, that's typically right thoracic and left lumbar. 03:27 The other thing the x-ray will do, at least the first x-ray will give you a sense is to whether or not there anre congenital anomalies or changes in the musculoskeletal system that need to be followed or evaluated differently. 03:38 You get a sense of the paraspinal masses, and how they're affecting it. 03:42 It will tell you whether there is the presence or absence of hemivertebrae or a wedged vertebrae or a partial vertebrae there. 03:49 And it will tell you if the vertebral body has any erosions or risk of cancer or other abnormalities. 03:55 Those are things that you should take into consideration. 03:59 Oftentimes, the radiologists would check the interpedicular space to assess for widening or shortening. 04:07 This will tell you if there's a risk for spinal cord tumor or spinal cord injury, syringomyelia, or cavitation that exists within a spinal segment. 04:16 So these are just general things you want to take into consideration. 04:20 When you have a patient with scoliosis, one thing we do is determine the bone age. 04:24 You want to know when they're gonna be growing and how long they're gonna be growing. 04:28 There are a number of different ways to check bone age. 04:31 One is an x-ray of the apophysis looking at the hips, looking for Risser sign. 04:36 You can check an x-ray of the apophysis of the distal radius, the ulnar and the small bones of the hand, that's called the Tanner and Whitehouse method. 04:43 You can check an x-ray of an elbow and that's called the Sauvegrain method. 04:48 And you could do a simple olecranon x-ray to get a better sense. 04:52 We're gonna go through the four different types of bony aging. 04:56 For the Risser sign, you want to get an x-ray of the iliac apophysis and you wanna see how much ossification you have of the iliac apophysis. 05:08 A Risser sign is a visual grading of that. 05:11 If there's no ossification, that's a zero (0) and a zero means they have a long way to go in growing. 05:18 If 25% of it is ossified, you get a 1. 05:21 25-50%, a 2. 05:23 3 would be 51-75%. 05:25 Greater than 76% is a 4. 05:27 and full bony fusion of the apophysis is a 5. 05:31 So that's one way. 05:33 The next way to measure for bone age is get an x-ray of the distal wrist looking at the radius, the ulna and the small bones of the hand. 05:42 And this is called the Tanner-Whitehouse method. 05:44 And what you're looking for is whether or not the bony areas have filled up what their relationship is and how much further growth they have. 05:54 So we have good ways of seeing growth from the wrist x-ray. 05:58 The third method is an x-ray of the elbow called the Sauvegrain method. 06:03 And you'll look at the four ossification centers - the lateral condyle, trochlea, the olecranon and the proximal radial epiphysis. 06:09 And you score it in a 27 point scale and then plot it in the graph. 06:13 And the last x-ray, the fourth x-ray is the x-ray of the elbow just assessing the ossification centers of the elbow. 06:19 It's called the simple olecranon method and it basically looks to see if you have a single ossification, a half-moon ossification, or there is a rectangular shape ossification center on the elbow. 06:33 Once you see the things have fused, you know that the growing has completed. 06:37 With complete fusion, you can say that bone age has reached skeletal maturity. 06:44 Occasionally, x-rays are not enough. 06:46 If you have an early onset of scoliosis, the need to move to an MRI is heightened. 06:53 If the patient has other symptoms that make you worry about cancer or malignancy, you need to move to an MRI. 06:58 If you're worried about traumatic fracture or other bony abnormalities possibly an osteogenesis imperfecta or frequent breaks, you may want to go to an MRI. 07:08 And if you're worried about a tumor or an infection, a CT or an MRI is also indicated for further information in order to get the best treatment possible. 07:18 if this patient has any neurologic symptoms like headache, neck pain, weakness, foot drop; If they have a loss of abdominal reflex or assymetric lower extremity reflexes if you notice atrophy in one area or another, or pes cavus in the chest, those are signs that you need to look further and you may want to get an MRI to evaluate the scoliosis. 07:38 If you have any abnormal findings on plain radiographs, then you want to go further and you wanna confirm those findings on the CAT scan or MRI more likely an MRI because it gets soft tissue and will give you further information that you're not geting on x-ray. 07:54 When do you need to refer a patient with scoliosis? Well the answer is anybody with a severe curve should be seen by an orthopedic specialist. 08:02 If the angle is severe, and you can't get a good measurement then you may want help getting the measurement because that's critical for knowing what you're gonna do long-term. 08:13 Patients who have a Cobb angle between 20 and 29 degrees may eventually need surgical intervention and getting them to the orthopedist early is gonna be helpful. 08:23 If they have a Cobb angle greater than 30 degrees, and you know you're gonna have some organ involvement getting the orthopedic specialist involved is gonna be good. 08:32 And any rapid progression of the Cobb angle more than 5 degrees in a single visit space indicate something may be changing quickly and that patient should be referred to an orthopedist. 08:46 At the same time of referral, it is important to maintain your measurements, continue what you're doing and stay involved in the care because you're gonna be monitoring and taking care of this patient, long-term. 08:59 You don't want to send them to an orthopedist for incidental finding. 09:02 It's mostly gonna be for definitive treatment or just help in measuring and figuring out how to name and how to witness the disease going forward.
About the Lecture
The lecture Radiographic Evaluation of Scoliosis by Tyler Cymet, DO, FACOFP is from the course Osteopathic Treatment and Clinical Application by Region.
Included Quiz Questions
True or false: The initial radiographic evaluation for scoliosis should be a standing full length PA (posterior to anterior) x-ray of the spine.
- True
- False
Which of the following radiological evaluations could be used to check for bone age or skeletal maturity? (Select all that apply.)
- Risser sign (iliac apophysis)
- Tanner and Whitehouse method (wrist and hand bone X-rays)
- Sauvegrain method (elbow ossification centers)
- The (simpler) olecranon method (olecranon apophysis)
- Bone scan
Which of the following indicates the need for a referral of a patient with scoliosis to an orthopedic specialist? (Select all that apply.)
- Scoliometer measurement (angle of trunk measurement) of greater than or equal to 7 degrees
- Cobb angle between 20 and 29 degrees in a premenarchal girl or a boy age 12–14 years
- Cobb angle greater than 30 degrees in any patient
- Progression of Cobb angle of more than 5 degrees in any patient in two consecutive visits
- Positive Adams forward bend test
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |