Playlist
Show Playlist
Hide Playlist
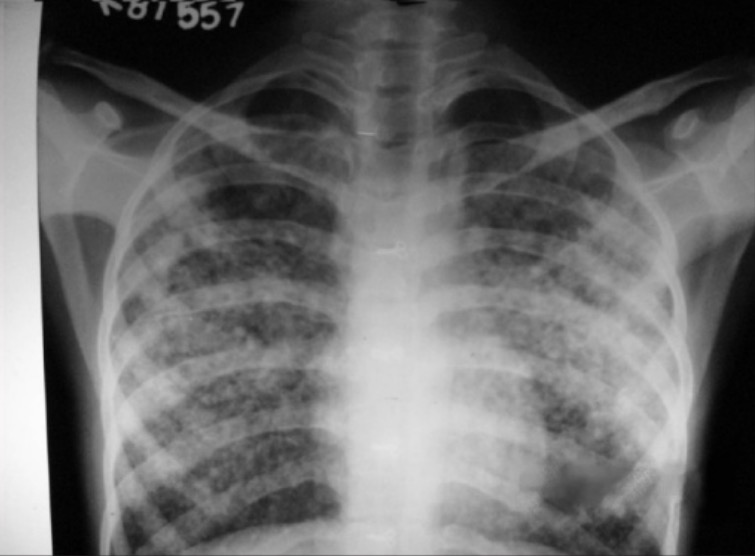
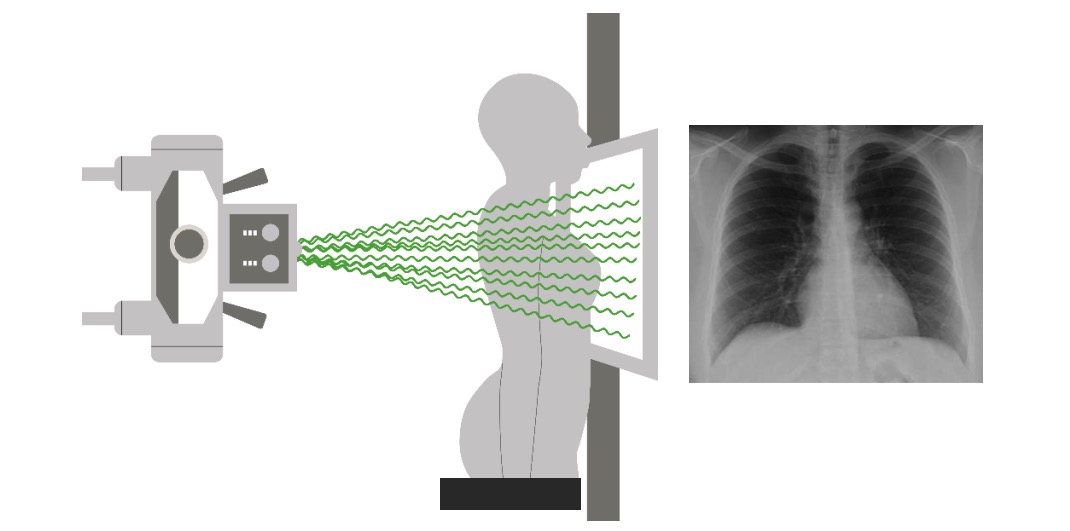
Pulmonary Edema: Definition
-
Emergency Medicine Bord Pulmonary edema and CHF.pdf
-
Download Lecture Overview
00:01 Hi! We’re gonna be talking about acute pulmonary edema and decompensated heart failure. 00:06 Before we get started I just wanna say that this is one of my favorite patient diagnosis to treat in the emergency department. 00:14 And the reason that I enjoy treating this patient is because oftentimes they come in looking very sick. 00:20 They can be sweaty and diaphoretic and they can be very short of breathe and having a hard time speaking. 00:27 And with a few key interventions, oftentimes we can turn these patients around. 00:32 And we can get them feeling and looking so much better. 00:35 So we’re gonna start up by reviewing, what is pulmonary edema? So what does it mean when we say that the patient is presenting with pulmonary edema? Basically, what this mean is that they have a fluid filling their lungs. 00:47 This can be due to a variety of reasons, most common reason that we see is decompensated heart failure. 00:53 It can be also due to substance used potentially or various other reasons. 00:59 You know generally we’re talking here about a patient who has flash pulmonary edema. 01:04 And what that means is that means that the pulmonary edema developed acutely. 01:07 It developed like that, it developed very, very quickly. 01:11 Now, we’re gonna start up by talking about a case. 01:16 So this is a 75-year-old woman who comes to the emergency department. 01:20 She's complaining of shortness of breath. 01:22 So what else do you wanna know? The questions you wanna ask are similar to questions you wanna ask other patients who have presented with shortness of breath. 01:32 So when did it start? Like I said, we’re talking here about a flash pulmonary edema. 01:36 A very sick patient who has fluids in their lungs. 01:39 Oftentimes this starts suddenly, now there maybe a little bit of a gradual presentation if a patient has kind of gradually worsening fluid in their lungs and then all of a sudden it got worse. 01:50 What makes it better or worse? We’ll talk about the classic things that makes it better or worst in a moment, but generally patients will be referring to you know walking or exertion, making their symptoms worst. 02:02 You also wanna asks about any other associated symptoms such as fever, cough, leg swelling, chest pain. 02:08 Because although here we’re talking about acute flash pulmonary edema and decompensated heart failure. 02:14 There are a lot of things in the differential here, when patient presents with the similar symptoms, so they could have pneumonia, they could be having a heart attack. 02:22 This is a pretty broad differential, so here we’re gonna be talking about this one specific diagnosis. 02:29 But associated sometimes can help role out or evaluate for other things. 02:33 You also wanna ask about medication compliance. 02:36 We'll be talking about this in a few moments but medication non-compliance is one of the big reasons that patients develop worsening heart failure or worsening fluid in their lungs. 02:47 So what are the classic signs and symptoms of pulmonary edema and CHF? One of the big things is shortness of breath with exertion. 02:55 So what the patient is gonna tell you is that, they’re gonna say, "Normally, I can walk, you know, a mile, or I can walk around the block three times. 03:03 I normally take my dog out and can do a nice walk. 03:06 And now I get short of breath when I walk to the bathroom or when I walk up a flight of stairs." So this is oftentimes a change in a patient’s ability to exert themselves. 03:15 They walk or exert themselves a small little bit and they develop shortness of breath. 03:21 The other big signs and symptoms of pulmonary edema would be orthopnea and PND. 03:28 So what is orthopnea means? It means that when you lay down flat, the shortness of breath worsens. 03:35 Now why is that? The reason for that in pulmonary edema and heart failure is because when you lay down flat, all the fluids kind of settles out and causes the patient to be short of breathe. 03:47 One of the big question you ask to kind of sort out if the patient is having orthopnea is by asking them how many pillows they sleep on. 03:54 So normally do you sleep on two pillows and now you’re sleeping on four. 03:58 Oftentimes patients will say that they are having a sleep sitting up and like a recliner chair, so that’s what orthopnea means. 04:06 PND stands for paroxysmal nocturnal dyspnea what that means is that the patient is kind of sound asleep and all of a sudden they wake up, feeling very short of breath and the classic thing that a patient will tell you is that, "I wake up feeling very short of breath." And they’ll go either outside or open they'll open their window to get some fresh air. 04:26 Another classic symptom for heart failure. 04:29 For flash pulmonary edema, again, this is gonna be a sudden onset mostly. 04:34 So it’s gonna be one minute they’re okay or they're a little short of breath and then all of a sudden they’re in significant respiratory distress. 04:42 Patients may also have associated leg swelling and that’s due to the backup of fluid. 04:48 If the heart isn’t pumping effectively, the fluid can back up into the legs. 04:52 It can back up very severely to the point where the patient can get a lot of scrotal swelling in the groin area. 04:58 So even in the abdominal area. 05:01 So the fluid can back up quite a lot and cause some edema. 05:04 You know, not everyone who presents with heart failure and flash pulmonary edema will have these symptom. 05:09 But if it’s there, it can further support this diagnosis.
About the Lecture
The lecture Pulmonary Edema: Definition by Sharon Bord, MD is from the course Respiratory Emergencies.
Included Quiz Questions
What is the most common cause of pulmonary edema?
- Decompensated heart failure
- Pneumonia
- COPD
- Severe asthma
- Pulmonary tuberculosis
Which of the following is NOT a sign/symptom seen with pulmonary edema associated with heart failure?
- Fever
- Shortness of breath with exertion
- Orthopnea
- Leg swelling
- Paroxysmal nocturnal dyspnea
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |