Playlist
Show Playlist
Hide Playlist
Idiopathic Intracranial Hypertension
-
Slides 08 Headache Neuropathology I.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
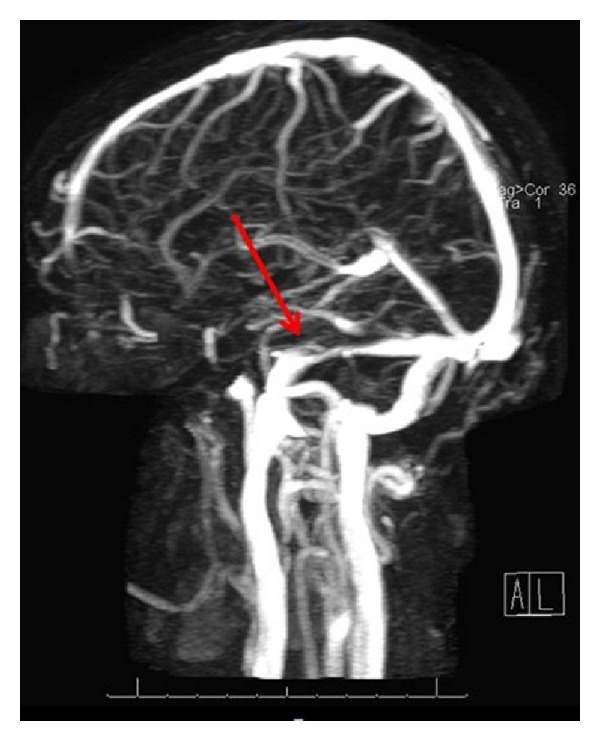
00:01 Our topic continues with subacute and chronic headache. 00:04 Here, we’ll take a look at pseudotumor cerebri. 00:07 Who’s your patient? Patient comes in with this chronic headache, also called idiopathic intracranial hypertension. 00:14 In other words, this is your IIH. 00:18 Now, idiopathic because we don’t know exactly as to what causes it. 00:21 We do know that there’s a particular drug that you should be extremely familiar with that might be a possible etiology, and that’s your ATRA, all-trans retinoic acid. 00:31 Well, pseudotumor cerebri, as the name implies, pseudo means false, a tumor-like lesion, or should I say tumor-like manifestation. 00:41 By that, we mean there’s a headache taking place. 00:43 You’ll find papilledema on fundoscopic examination but absolutely no evidence of a tumor. 00:50 Described as diffuse, dull, ache, pressure. 00:53 Remember, this is chronic headache. 00:55 Onset is a gradual but often progressive. 00:57 Headache is often worsened by laying down and by physical activity. 01:02 Blurred vision is common. 01:04 Horizontal diplopia is occasionally seen, and bilateral cranial nerve VI abducens palsy can be seen. 01:12 So this will be a good time to review quickly, please, the functions of your abducens cranial nerve VI, And papilledema is quite prominent. 01:20 Keep that in mind. 01:22 What does papilledema mean to you? You do a fundoscopic examination and you find there around optic disc, it looks like sun rays. 01:29 Very bright, huh? That’s your papilledema. 01:32 Now, with that papilledema, you would think that, “Oh my goodness, that must be prominent.” You’re worried about intracranial pressure being increased, and that is not a good thing. 01:41 So, keep that in mind. 01:43 We’ll take a look at epidemiology of pseudotumor cerebri. 01:47 75% of your patients will be females. 01:49 That’s where your focus should be. 01:51 She, will be in her reproductive age between 20 to 40. 01:55 Vast majority of these females are obese, more common during pregnancy, also seen with steroid therapy, vitamin A toxicity, which I was referring to earlier, your ATRA, all-trans retinoic acid, and maybe perhaps, even tetracycline antibiotics. 02:13 Make sure you know that these are possible causes or medications that may result as an adverse effect of pseudotumor cerebri. 02:24 Diagnosis: Imaging initially to rule out a mass lesion because there is no mass. 02:29 Lumbar puncture to document -- document -- opening pressure. 02:35 elevated at 250 to 450 millimeters, the water pressure in lateral decubitus. 02:43 It is important that you know the specifics for opening pressure, please. 02:49 CSF should otherwise be normal. 02:53 Formal visual field testing because of papilledema. 02:56 Early defect is enlargement of blind spot and slight peripheral field constriction. 03:04 Remember, there is prominent papilledema in these patients, so early on, you would find such defects. 03:11 Management: Well, here, lumbar puncture, weight loss, carbonic anhydrase inhibitors, Diamox, shunt, optic nerve fenestrations. 03:23 You do want to relieve some of that pressure that’s taking place with idiopathic intracranial hypertension, AKA, pseudotumor cerebri. 03:36 Summary of pseudotumor cerebri: Female, early, young, obese. 03:41 Preventive medicine: Weight loss. 03:44 Signs and symptoms: Blurred vision, headache. 03:47 The differentials include, if you remember, we talked about venous sinus thrombosis during pregnancy. 03:53 Please be very careful, because during pregnancy with estrogen, it may result in the thrombus formation in the sagittal or the transverse sinus. 03:59 I even showed you an image where the transverse sinus was absent. 04:05 That’s venous sinus thrombosis. 04:08 Here, we have pseudotumor, mass lesion, migraines as being differentials. 04:15 Diagnostic: Lumbar puncture. 04:16 We talked about earlier, specifically the pressure of 250 to 450 millimeters of water. 04:22 specifically the pressure of 250 to 450 millimeters of water. 04:22 Treatment: Weight loss, carbonic anhydrase inhibitors, and shunting.
About the Lecture
The lecture Idiopathic Intracranial Hypertension by Carlo Raj, MD is from the course Headache – Pathophysiology.
Included Quiz Questions
What is the approximate opening pressure that would be expected on a lumbar puncture in an obese patient with idiopathic intracranial hypertension?
- 250 to 450 mmH2O in the lateral decubitus position
- 250 to 450 mmH2O in the sitting position
- 50 to 100 mmH20 in the sitting position
- 50 to 100 mmH20 in the lateral decubitus position
- 150 to 200 mmH20 in the lateral decubitus position
Which of the following is the most appropriate medication for a patient with a headache due to idiopathic intracranial hypertension?
- Carbonic anhydrase inhibitors
- Calcium channel blockers
- Beta-blockers
- Triptans
- Amitriptyline
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |