Playlist
Show Playlist
Hide Playlist
Prostate Gland – Male Reproductive System
-
Slides 07 Human Organ Systems Meyer.pdf
-
Reference List Histology.pdf
-
Download Lecture Overview
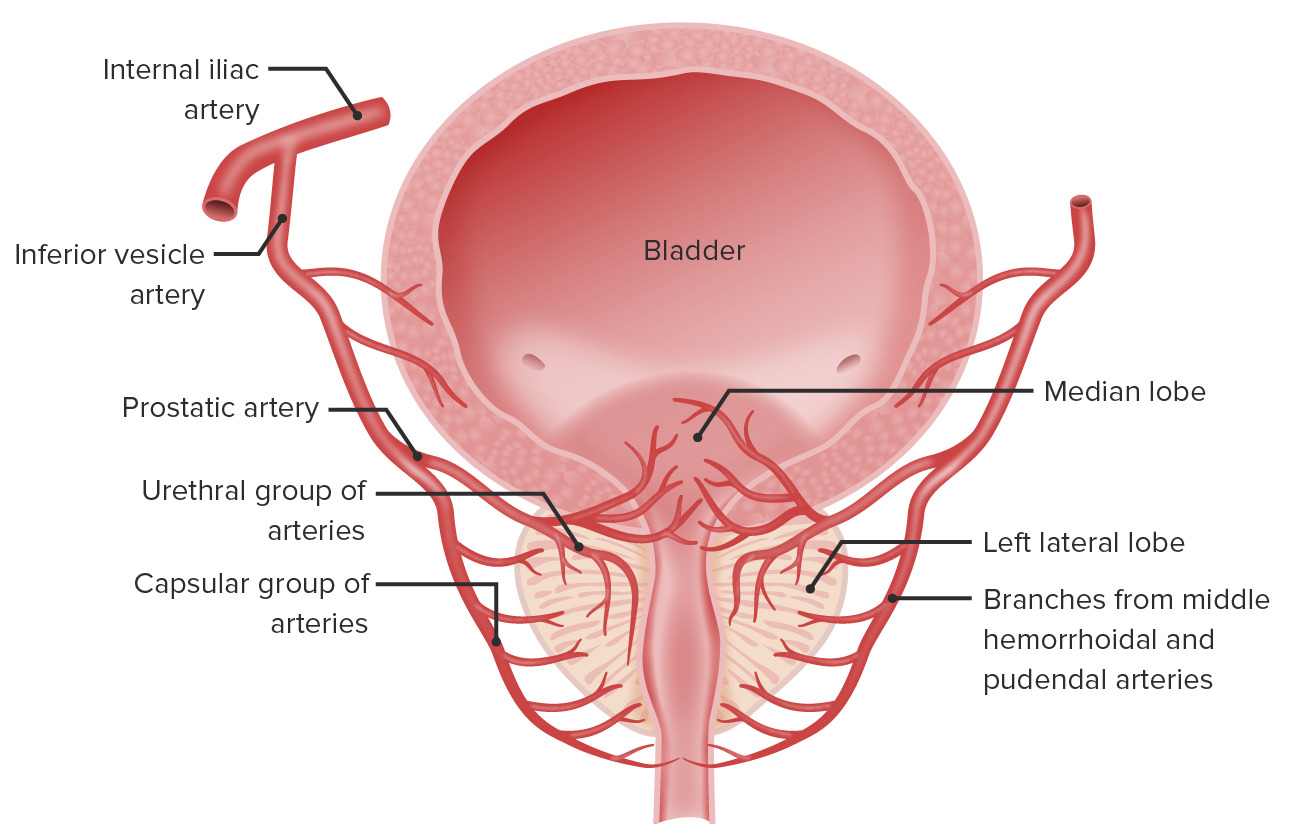
00:00 The prostate gland is the largest accessory gland. It secretes a watery slightly alkaline fluid. It also secretes fibrinolysin which liquefies the semen. Whereas, the seminal vesicle secretes a yellowish, whitish solution that’s rich in fructose. When you look at the structure of the prostate gland, there are separate units illustrated on the diagram. 00:37 Look closely at the urethra, and also, at the ejaculatory duct coming into the prostatic tissues. Around that area, immediately around the urethra, is an area or a zone, if you like, consisting of what’s labelled there as mucosal glands. Then there is a middle submucosal gland layer, and then an outer peripheral or the main prostatic gland layer. 01:11 These three separate zones are quite significant as I’ll explain to you in a moment. 01:18 The glandular tissue, even though they are restricted within these three zones, three separate zones, and the products are delivered via the ducts into the urethra, the glandular tissue, if you look at all through these zones, is very similar. The epithelium is generally described as being columnar, but there is variation in the sort of arrangement of the epithelium that you often see at various parts of the prostatic gland. And these epithelial surfaces can often become nodular, and that creates a problem. If it occurs in the glandular tissue immediately around the urethra, then it can impinge on the lumen of the urethra, and therefore, make urination a long slow process. This increases as the males age. 02:15 There is another characteristic also of the prostate, and that is the presence of prostatic concretions called corpora amylaceas. These build up again with age. They become calcified. 02:33 And again, if they build up in a zone immediately around the urethra, then they can impinge on the urethra, and therefore again, make urination a long slow process. Now, these cells also can become cancerous. Prostate cancer is the most common cancer in males. 02:59 And it tends to occur in the outer peripheral main prostatic glands. And there, the cancers can develop and take over a lot of the mass of that outer peripheral zone. And that can be digitally palpated through a rectal examination. But the problem is that when these cancers grow within the prostate and maybe even start to impinge on the urethra, and the male experiences a long slow urination process, then it’s too late because by that stage, the prostate cancer has metastasized. It’s spread to other parts of the body. The prostate gland secretes many components of the seminal fluid. One is prostate-specific antigen. It’s secreted into the seminal fluid or into the secretions of the prostate, but a bit of it also leaks across into the blood stream. So it can be detected in blood. And in normal individuals, the levels are lessened about four nanograms per mil. But in prostate cancers, the secretion of this prostate-specific antigen can increase. So, a blood test can reveal higher concentrations of this prostate-specific antigen or PSA in the blood. And that is an indication that there are these cancerous cells present in the prostate. So, males are encouraged over a certain age to have a regular blood test to detect the levels of this PSA. 04:57 Same as females, have a regular Pap smear to detect the presence of cancer cells that may be exfoliated from the cervix into the vagina. And similarly, breasts can be scanned. The mammary gland can be scanned for the presence of cancer cells in the breast, because both the change in the hormonal environment throughout the female menstrual cycle and genetic predisposition are risk factors for breast cancer. So there are these different methods of scanning both female and male reproductive organs to try and detect these cancerous events.
About the Lecture
The lecture Prostate Gland – Male Reproductive System by Geoffrey Meyer, PhD is from the course Reproductive Histology.
Included Quiz Questions
Which of the following statements regarding prostate secretions is MOST ACCURATE?
- The prostate secretes a thin, opalescent, alkaline fluid that liquefies semen.
- The prostate secretes a thick, clear, acidic fluid that contains fibrinolysin.
- The prostate secretes a thin, opalescent, acidic fluid that contains fructose.
- The prostate secretes a thick, clear, alkaline fluid that helps coagulate semen.
- The prostate secretes a watery, alkaline fluid containing sperm.
Which of the following is NOT an established area/zone of the prostate?
- Tubular
- Peripheral
- Anterior fibro-muscular
- Central
- Transition
The epithelium of the urethra is mainly composed of which of the following types of cells?
- Columnar
- Pyramid
- Simple squamous
- Cuboidal
- Stratified squamous
Which of the following terms refers to inert concretions of amyloid in the prostate and other tissues?
- Corpora amylacea
- Nodules
- Glandular tissue
- Mucosal glands
- Lymphoid glands
Which of the following is most frequently used for screening of prostate cancer as it increases in the serum of patients with the disease?
- Prostate specific antigen
- Testosterone
- Protein binding antigen
- Luteinizing hormone
- Estrogen
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |