Playlist
Show Playlist
Hide Playlist
Preload and the Frank-Starling Law – Cardiac Mechanics
-
Slides Physiology-Cardiac-Mechanics.pdf
-
Download Lecture Overview
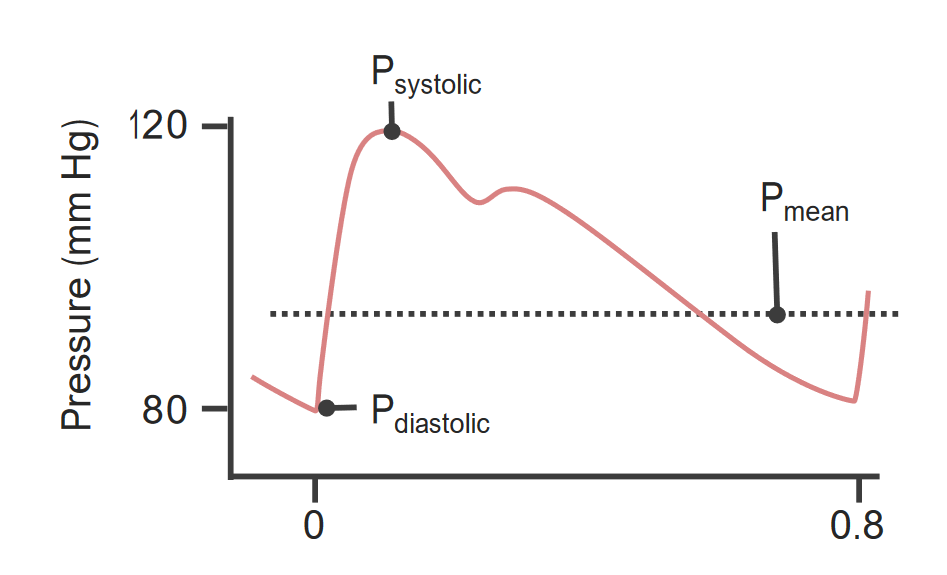
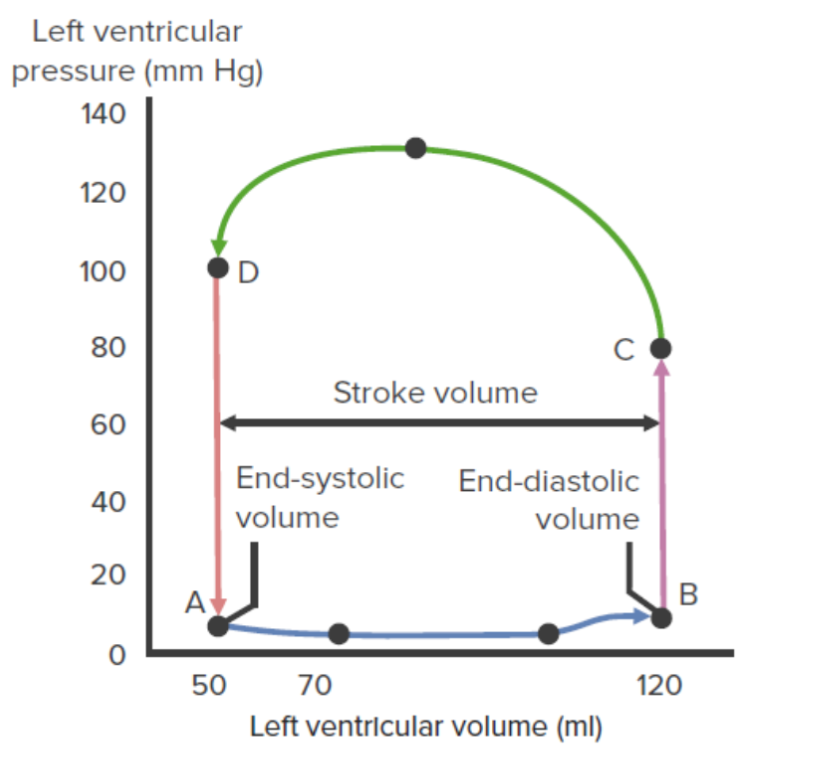
00:02 So, now, let’s get into preload. Preload is very important for the filling component of the heart. 00:08 That is your left ventricular end-diastolic volume. 00:12 That's the maximum amount of volume you have in your left ventricle prior to a contraction. 00:18 Interestingly, when you talk about preload, it’s actually about a fiber length that we’re most concerned about. 00:25 How much stretch is there on the left ventricle before you contract it again. 00:30 Those kind of thoughts can be easily seen with things like a balloon. 00:35 You're filling a balloon until it gets to a certain point or tautness, and that's when you know it's full. 00:41 But until that point, you have a large space to fill. 00:45 The valsalva maneuver is a great way to show how preload affects arterial blood pressure. 00:54 This tracing can be seen here where we have arterial blood pressure in the red I'm tracing. 01:02 This is measured in millimeters of mercury. 01:05 During normal breathing, you can see normal systolic and diastolic blood pressures. 01:10 If you engage the valsalva maneuver, this is increasing expiratory pressure. 01:17 So in our example, this increase in expiratory pressure is 20mmHg. 01:23 That creates a decrease in preload cause there's more pressure within the thoracic cavity compressing some of the large vessels allowing for blood to return to the heart. 01:35 What initially happens is there is a decrease in blood pressure because there is a decrease in preload. 01:44 Eventually pressure goes up slightly in the late phase 2 part, as you get an increase in contractility and in heart rate. 01:55 During the recovery phase, when you release the valsalva, that means preload is now exaggerated. 02:02 You first get here a small drop in blood pressure, and then a large increase in blood pressure with very long pulse pressure. 02:11 This is the phase 1, 2, 3, and 4 of the valsalva. All dealing with how preload, the volume returning to the heart affects the arterial pressure. 02:26 When looking at preload, there are couple of intrinsic mechanisms associated with the muscle. 02:34 And here, let's explain those to a greater degree. 02:37 It depends on how much you fill the heart, how much it's going to be able to contract. 02:43 The more it's full, the harder it can contract. The less it's full, the less hard it can contract. 02:49 So, let’s look at that diagrammatically. 02:52 When you have a low preload, you don't fill the heart as much. 02:56 And therefore, at any given left ventricular pressure, you can only push out so much stroke volume. 03:03 If you fill the heart more at that same level of contractility, you can push out more blood. 03:11 What factors affect preload? Two of the biggest ones are venous blood volume and venous compliance. 03:19 So, the more blood volume you have, the more return of blood you have to the heart. 03:25 If your veins are less compliant, meaning that they are constricted, the more blood you'll be able to return to the heart. 03:34 That has to do with increasing venous pressure, and specifically, it a lot depends on how compliant your left ventricle is to accept this new level of preload. 03:45 The amount of contractility of the top portion of the heart also affects your preload because it's going to be pushing in that last little bit of blood. 03:54 The harder the atrium contract, the more preload you get. 03:58 Another factor that affects preload, which is a little bit more indirect, it’s one of those secondary effects. 04:05 If you increase the amount of afterload, you will not be able to push as much blood out on any given stroke of the heart. 04:14 If you don't push as much blood out, you have more blood left over after each stroke. 04:20 Interestingly, if you have more blood left over, you can fill it to a greater degree. 04:26 So, in fact, if there is an increase in afterload and you don't get as much blood out per stroke, on the next time the heart beats, it will contract harder. Why? Because you filled it to a greater degree. 04:40 The last two items that affect ventricular preload are heart rate and inotropy. 04:48 These two items are normally associated with more cardiac output. 04:54 But if you slow the rate of the heart, you don't have it beat as fast, it has more time to fill. 05:01 So, one way to get more preload is don't beat the heart as fast and you can be on diastole for a longer period of time. 05:11 Ventricular inotropy works on a similar principle, in which if you decrease the strength of the contraction, therefore you have a greater end-systolic volume. 05:24 The next beat of the heart, you'll fill it to a greater degree and that increases your preload. 05:31 So, let's look at this preload concept on a graph. Because this will land the principle. 05:36 And even though this is a hard one, you'll get it if you can see it in action. 05:40 So, when we look at graph like this, let’s talk through the different axes. 05:45 The first axis we’re going to have is the x-axis. It's going to be left ventricular end-diastolic pressure. 05:53 On the y-axis, we’re going to have stroke volume. So, those are our two variables. 06:00 If we start off in a condition, which is A. If we move from A to B, we have increased the left ventricular end-diastolic pressure. 06:12 At that point, you’ll have a greater stroke volume that will occur. So, let's go through that a little bit more detail. 06:20 If you increase left ventricular filling pressure, that is an index of what? Preload. 06:27 That index of preload will cause then an increase in stroke volume. 06:32 This relationship is called the Frank-Starling mechanism or Frank-Starling principle. 06:38 This principle or relationship allows for this inherent property of cardiac myocytes. 06:47 It's interesting you're not actively using more ATP to generate this stronger contraction. 06:54 You're simply letting the myocytes stretch more and then they’ll contract back harder. 07:00 This is also referred to as a length-dependent activation. 07:06 So, it matters at what length you are, what level of contraction you'll get. 07:14 So how does preload affect pressure-volume loops? Everybody's favorite, pressure-volume loops. 07:22 And with a pressure-volume loop, we have a normal indices, which stack out at the top and the bottom portion of the graph. 07:31 These are our places in which we cannot go out of. It provides our minimal and maximal components in the figure. 07:41 A normal pressure-volume loop looks like this, where you start off filling the heart along the bottom axis. 07:49 You have a vertical line, which is the contraction of the heart. You have an ejection portion and then a relaxation portion. 07:57 How does preload change that? Preload should allow you to fill to a greater degree. 08:02 If you're filling to a greater degree, you should be what? Increasing that volume. 08:08 As you do that, you make a bigger pressure-volume curve. You increase end-diastolic volume and you increase stroke volume. 08:17 All because of the increase in venous return. Now, let's look at this if we have a decrease in venous return. 08:26 Therefore, you’re going to have now a shorter curve that decreases left ventricular end-diastolic volume and decreases stroke volume. 08:36 Nice ways to think of changes in the pressure-volume loop. How would you get such pressure-volume loop changes? Well, a good example of an increase in venous return is if you get extra volume added to your blood, maybe you were hooked up to an IV and infused in volume through, let's say, isotonic saline. 08:59 A decrease in volume could be just the opposite. Maybe you've undergone dehydration and you've lost body water. 09:06 So, those are two examples of both either an increase or decrease in venous return.
About the Lecture
The lecture Preload and the Frank-Starling Law – Cardiac Mechanics by Thad Wilson, PhD is from the course Cardiac Physiology.
Included Quiz Questions
Which of the following parameters increases ventricular preload?
- Increased atrial inotropy
- Increased ventricular inotropy
- Decreased afterload
- Decreased ventricular compliance
- Increased heart rate
Which of the following parameters decreases ventricular preload?
- Decreased atrial inotropy
- Decreased venous compliance
- Increased afterload
- Decreased ventricular inotropy
- Increased ventricular compliance
Which of the given parameters is related to the Frank-Starling law of the heart?
- Stroke volume and end-diastolic volume
- Heart rate and preload
- Venous pressure and ventricular compliance
- Preload and afterload
- Stroke volume and end-systolic volume
Why does the Valsalva maneuver initially decrease blood pressure?
- The increased intrathoracic pressure leads to decrease venous return. This leads to decreased preload.
- The decreased intrathoracic pressure leads to increased venous return and then decreased preload.
- The increased intrathoracic pressure leads to increased venous return and an increase in preload.
- The increased intrathoracic pressure leads to increased venous return. This leads to increased preload.
- The decreased intrathoracic pressure leads to decreased venous return and then decreased preload.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
2 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
So good this is life changing .Our lectures are so bad lately and this is helping immensely . Thank you so much !
Very clear and simple to understand! Dr. Wilson love and enjoy what he teaches!