Playlist
Show Playlist
Hide Playlist
Polycystic Ovary Syndrome (PCOS): Diagnosis and Fertility Considerations
-
Slides PCOS ReproductiveEndocrinology.pdf
-
Download Lecture Overview
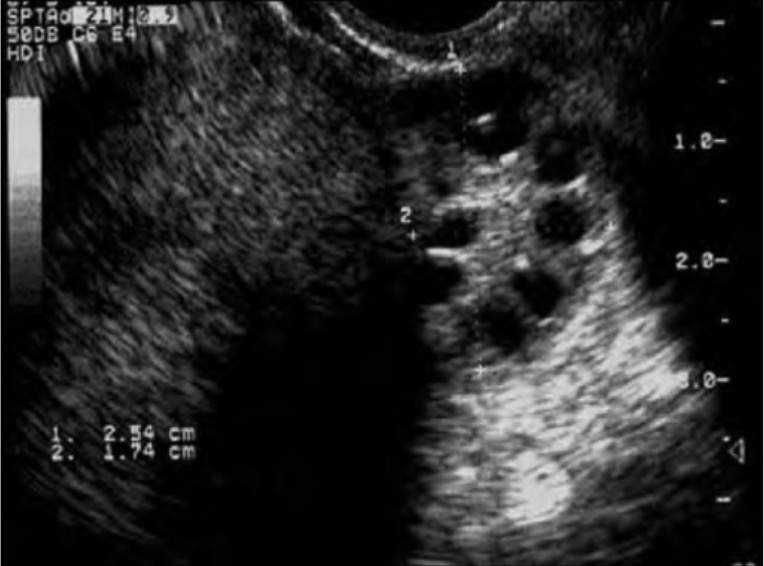
00:00 In this lecture we will be reviewing PCOS or polycystic ovarian syndrome. PCOS affects approximately 5 to 10% of reproductive age women in the US making it most common endocrine disorder in women. 00:18 These patients often present with oligoovulation, infertility, and hirsutism. Let's go over the clinical guidelines to make the diagnosis of PCOS. Patients must demonstrate both clinical and/or biochemical signs of elevated androgens. They must also have oligoovulation or anovulation. 00:39 Remember this is important these diagnoses are a diagnosis of exclusion. There can be other causes of androgen excess in ovulation that must be ruled out first. In the Rotterdam criteria, the patient must meet 2 out of 3 of the criteria. She may have elevated androgens either clinically or biochemically, anovulation, and polycystic ovaries. Again, she has to meet 2 out of 3. Let's review what the ovary of a PCOS patient would look like on ultrasound. You classically see it defined or described as pearls on a string. You can see here in this figure that they are closely related follicles that appear like pearls on a string. This is another image which shows that very well. If you see this image on your exam, remember PCOS. Let's talk about the evaluation of a woman with PCOS. It's very similar for a woman with hirsutism. You can read more about hirsutism in our lecture entitled Hirsutism. Remember to ask women about the age of menarche, description of their cycles, the duration of their menses or the number of days that they bleed, other diagnoses, and their OB history. Remember to ask the patient about other family members who may have hirsutism as we think PCOS may be inherited. Also remember to ask about obesity in the family. The overwhelming majority of patients with PCOS are obese and she may have a family history of it. Ask about infertility in both the patient and her family and don't forget high-risk ethnicities can actually have other disorders such as CAH. There are certain medications that can also lead to hirsutism. Let's now talk about the long-term risk factors associated with PCOS. 02:37 Here you'll see a gross pathologic picture of a patient who's having surgery. This is her ovary actually filleted open and you can see here the follicles that we just saw on the ultrasound. 02:49 However, let's return to the associated problems with PCOS. She has elevated risk of cardiovascular disease, diabetes later on in life, endometrial carcinoma, psychosocial dysfunction, and infertility Let's now talk about the evaluation that we would do if we saw a patient with PCOS. We typically get a serum total testosterone and normal is 20 to 80 ng/dL. DHES is not sensitive or specific but we usually include it to rule out adrenal processes. There is no uniformly validated and accepted test for measuring insulin resistance. Most physicians will send a 2-hour glucose tolerance test to uncover any occult diabetes or insulin resistance that may be present. Also if the patient knows her menstrual cycle and is in the follicular phase, we will do a morning or a.m. 03:46 17-OHP. If it's less than 200, this is normal; however, if it’s between 200 and 400 we will need to do an ACTH stimulation test to uncover nonclassical CAH. For more information about CAH, please listen to the lectures associated with that topic. Remember that PCOS is a diagnosis of exclusion so we also send a TSH to look for thyroid abnormalities that can lead to anovulation. 04:14 We also check a prolactin as we know that prolactin can be elevated in PCOS patients. Let's now talk about the Ferriman-Gallwey scoring system. This is not actually clinically used and I doubt will be on your exam; however, if you see this in a question think hirsutism. It's not clinically relevant for us because many patients will wax or shave their hair and then we can't really score them because it's based on the amount of hair in different positions and locations in the body. 04:48 Don’t forget that we need to include CAH or congenital adrenal hyperplasia in our differential diagnosis. Obviously, these patients would have non-classical CAH with some residual enzyme activity. For more information, look at the lectures associated with congenital adrenal hyperplasia. 05:07 We should also keep in mind that idiopathic hirsutism can be a cause of hirsutism. This was formerly called familial hirsutism. This is likely due to an excessive activity of the 5-alpha reductase enzyme in the hair follicle. This is also a diagnosis of exclusion. Our differential diagnosis for PCOS needs to include Cushing's syndrome. This can be a life-threatening syndrome that we need to rule out effectively with a 24-hour urine. I discussed more about Cushing's syndrome in the Hirsutism lecture if you like to find out more. Let's review the management of PCOS. The first line management is oral contraceptive pills. They work in several ways. In the anterior pituitary, they decrease LH. LH causes the ovary to make less testosterone and there's less free testosterone. 06:02 Also, the liver increases sex hormone binding globulin which increases the binding of free testosterone. Let's review a checklist. If a patient has a diagnosis of PCOS, then we should actually give them OCPs in the form of estrogen and progestin. This suppresses LH secretion and overall will help with hirsutism. Estrogen stimulates sex hormone binding production and OCPs will decrease adrenal production of DHES. Progestins actually inhibit 5-alpha reductase activity in the skin, therefore the combined oral contraceptive pill is best. If a patient has insulin resistance, we should consider using metformin to help overall with this insulin resistance and potentially a bit of weight loss; however, metformin is not primarily used to induce weight loss nor is it used for ovulation induction. You may have read that in old literature. That's no longer accepted. Let's now talk about how we would manage a patient who desires to become pregnant. 07:11 Many PCOS patients struggle with infertility. Traditionally, we did ovulation induction with clomiphene citrate and we know that clomiphene increases the frequency of GnRH pulsatility and ovarian follicular development. 50% of women will ovulate on 50 mg of Clomid and the average dose per cycle should not exceed 750 mg; however, current literature suggests that we should letrozole as a primary agent. Clomiphene citrate can lead to twins or multifetal pregnancies which have obstetric complications while letrozole, an aromatase inhibitor, has more monofollicular recruitment. Thank you for listening and good luck on your exam.
About the Lecture
The lecture Polycystic Ovary Syndrome (PCOS): Diagnosis and Fertility Considerations by Lynae Brayboy, MD is from the course Reproductive Endocrinology.
Included Quiz Questions
Which of the following criteria is associated with polycystic ovarian syndrome?
- Rotterdam criteria
- Jones criteria
- Duke criteria
- Light criteria
- Amsterdam criteria
Which of the following would you expect to find on pelvic ultrasound in a patient with PCOS?
- Pearls on a string appearance
- Snow storm appearance
- Heart shaped uterus
- Streak ovary
- Bull's eye appearance
Which of the following is NOT associated with PCOS?
- Type I diabetes
- Cardiovascular disease
- Infertility
- Psychomotor dysfunction
- Endometrial carcinoma
A 20-year-old woman presents with hirsutism and primary amenorrhea. Her total testosterone level is 69 ng/dL. Blood glucose and TSH were normal and prolactin levels were mildly elevated. Her morning 17-OHP was normal. What is the most likely diagnosis?
- Polycystic ovarian syndrome
- Partial CAH
- Complete CAH
- Cushing's syndrome
- Hyperprolactinemia
Which of the following enzymes is most likely implicated in idiopathic hirsutism?
- 5-alpha reductase
- DHEAS
- 17-hydroxylase
- 21-hydroxylase
- 11-hydroxylase
Which of the following answer choices is the most effective treatment option for patients with PCOS and desire pregnancy?
- Use of clomiphene citrate
- Starting on OCP
- Stopping OC pills after regularization of the cycle
- Decreasing the weight of the person
- Use of metformin
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Good information, I learn a lot about POS. Thanks a lot i like it very much