Playlist
Show Playlist
Hide Playlist
Plexopathy
-
Slides 04 Plexopathy Neuropathology II.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
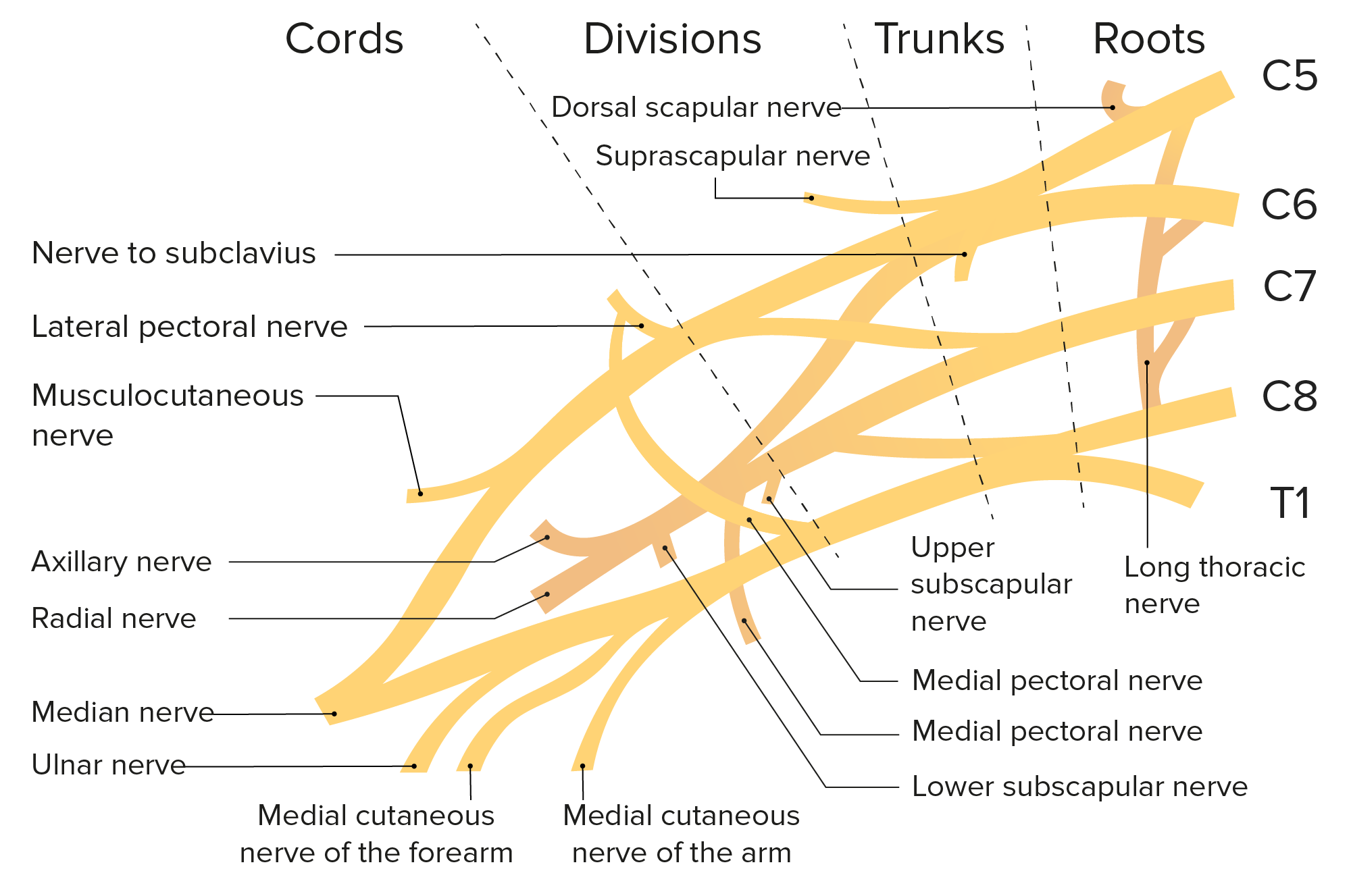
00:01 Our topic here under peripheral neuropathy is initially plexopathy. 00:07 What does that refer to? Think of the brachial plexus. 00:13 So from neuroanatomy, you should know your brachial plexus quite well. 00:17 You’ll have your roots and your nerves, branches and so on and so forth. 00:21 And as we go through some of these important neuropathies or plexopathies, obviously, we’ll take a look at important clinical features. 00:32 Your brachial plexus, formed by C5 to T1 nerve roots. 00:38 And the possible injuries, we’ll get right into the pathology. 00:41 Erb’s palsy: What happens here? C5 and C6 injury. 00:47 What’s it the caused by? Overstretch of the neck from shoulder during delivery is important. 00:54 Causes C5-C6 dermatome loss and waiter’s tip position, shoulder’s weakness. 01:03 Erb’s palsy. 01:04 You’ve seen this before. 01:05 Waiter’s tip. 01:08 Klumpke’s palsy: C8-T1 injury from over abduction of the arm causing, well, anesthesia and weakness in ulnar distribution, what does ulnar mean to you? The medial aspect, right? Klumpke’s, C8-T1. 01:26 Erb’s palsy, C5-C6. 01:30 Then we have what’s known as your Parsonage-Turner syndrome. 01:35 Acute brachial plexus neuritis. 01:38 It could be seen in diabetes mellitus, autoimmune disease such as SLE, and also during vaccination. 01:47 It has been recorded to have caused or possibly trigger what’s known as Parsonage-Turner syndrome, acute brachial plexus neuritis. 01:57 Our topic, I’m in the peripheral nerves, peripheral neuropathy. 02:02 Specifically, plexopathies. 02:04 And with the plexopathies, you’re focusing upon the roots from C5 to T1. 02:12 The lumbo-sacral plexus. 02:15 The lumbar plexus between L1 to L4. 02:18 Obturator nerve, thigh adduction. 02:22 Femoral nerve, hip flexors and knee extensors. 02:26 The sacral plexus will be L4 to L5, S1 to S4, clinically. 02:32 Sciatic nerve is important. 02:34 Common peroneal, tibialis anterior is what it’s going to supply and then the tibial, plantar flexor and we have our inverters. 02:45 Take a look at the picture on the right. 02:48 You should have a firm understanding from neuroanatomy your lumbosacral plexus and then branched into, specifically, lumbar plexus and your sacral plexus.
About the Lecture
The lecture Plexopathy by Carlo Raj, MD is from the course Other Diseases: Hydrocephalus, Neuromuscular Disease, Plexopathy, and Mononeuritis.
Included Quiz Questions
Erb palsy is caused by injury to which of the following nerve roots?
- C5, C6
- C6, C7
- C7 C8
- C8, T1
- C7, T1
Klumpke palsy is caused by injury to which of the following nerve roots?
- C8, T1
- C6
- C7
- C7, C8
- T1
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
It made it so much easier for me to understand and go through this topic