Playlist
Show Playlist
Hide Playlist
Perforated Viscus: Diagnosis
-
Emergency Medicine Bord Perforated Viscus.pdf
-
Download Lecture Overview
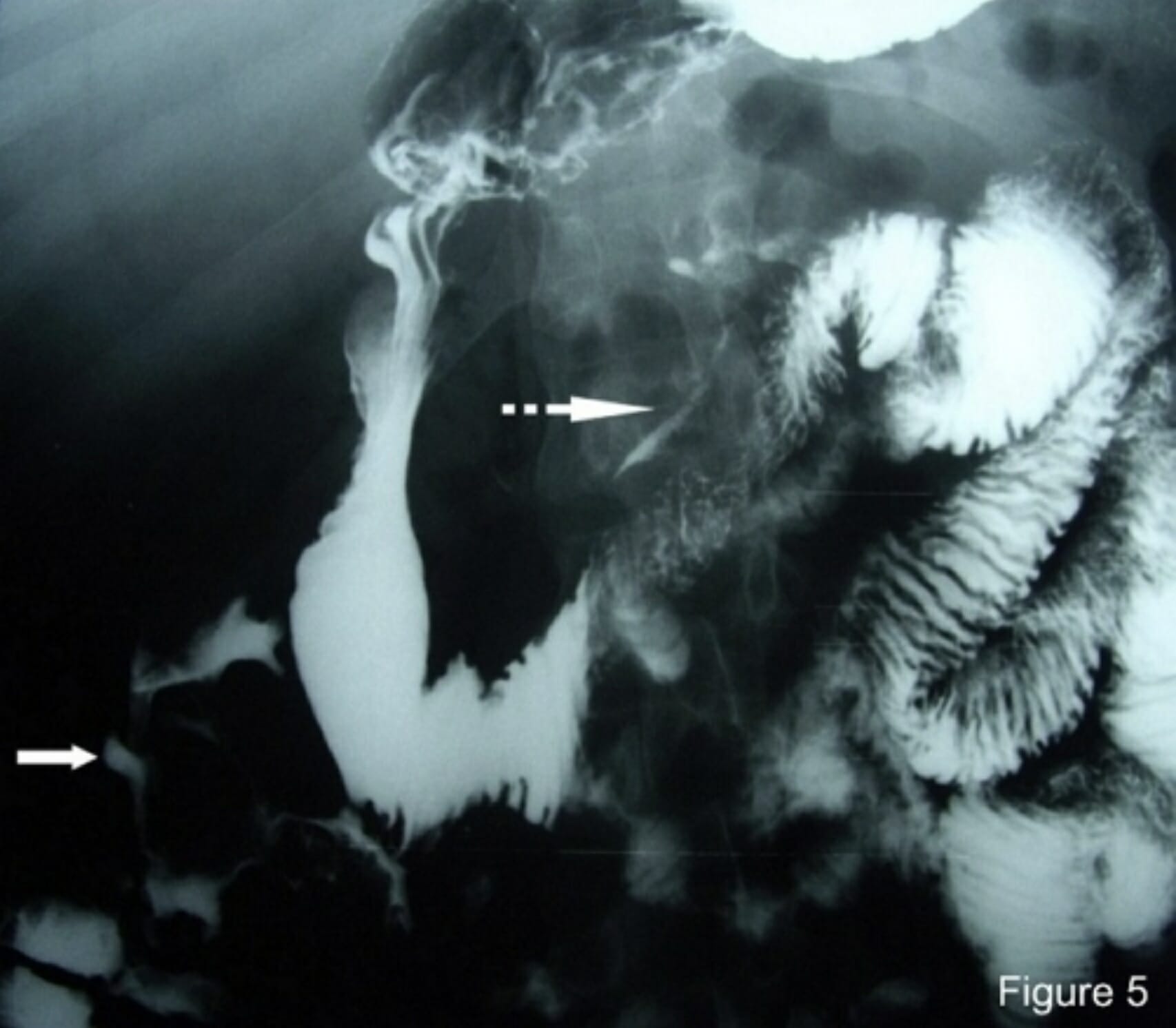
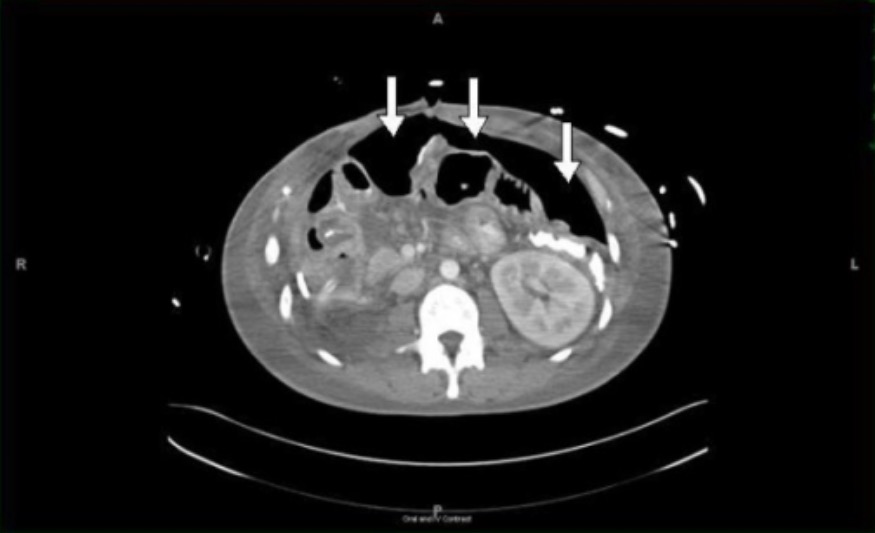
00:02 How do we go on to diagnose this? So we wanna think about standard lab testing. 00:07 So what are our standard labs that we wanna do? We wanna start thinking about preoperative labs. 00:12 If you have a patient, when you examine them and they’re very uncomfortable and they have guarding and rebound tenderness on their belly, start thinking about the fact that your patient may need an operation. 00:25 You can check a lactic acid level. 00:27 A lactic acid level indicates that there has been decreased blood flow to the tissues, possible infection, possible ischemia. 00:35 You wanna check a urine HCG level for all women of childbearing age, you wanna make sure you’re checking a urine HCG. 00:44 And potentially, you wanna consider checking a lipase. 00:48 There potentially can be some relation between pancreatitis and a perforated peptic ulcer and also, a lipase can help support a diagnosis of pancreatitis if that’s present. 00:59 Paint associated with a peptic ulcer would be located in a similar place to pain associated with pancreatitis, so up in the upper portion of the abdomen. 01:08 Thinking about imaging, plain film x-ray would be your first study of choice, followed by CT scan and then, we’ll talk about ultrasound as well. 01:18 Now, plain film x-ray can be obtained very rapidly. 01:23 It can be performed at the bedside. 01:25 When you’re getting a plain film because you’re worried that someone has a perforated viscus or free air in their abdomen, you wanna be sure that you perform an upright chest x-ray or a lateral decubitus film. 01:37 The reason for that is if you think back to your physics class, you know that air goes up and other things go down. 01:46 So if you have free air in your abdomen, by taking an upright chest x-ray, so what we mean by that is that the patient is sitting upright, you are going ahead and you’re gonna see that the air if it’s there will go to the top of the abdomen. 02:01 So on this x-ray you could see the label that says D is the diaphragm, so that’s the line for the diaphragm. 02:08 The label that says G is the gas under the diaphragm. 02:12 There’s not supposed to be that black space there. 02:15 The diaphragm and the liver are supposed to be touching on the x-ray. 02:21 Again, the pros here are that this is performed at the bedside. 02:24 It’s easy to do, it can generally be obtained quickly, your patient doesn’t leave the Emergency Department, so it’s safe in that regard. 02:33 The cons here are that this has a poor sensitivity and specificity for free air. 02:38 Free air is detected only about 50% of the time in laparotomy proven perforation. 02:44 So in half of the patients who have been to the operating room who have a perforated viscus, this was not seen on x-ray. 02:52 There was no free air seen on x-ray. 02:54 So I can’t stress enough to you that while this is a good easy quick first test to get, you do not stop with the x-ray. 03:02 If you are concerned and worried based on your exam and the symptoms the patient is having that they have free air, you have to move on to additional testing. 03:09 The sensitivity and specificity of this test is not great. 03:14 So the next test you should think about getting would be a CT scan. 03:18 A CT scan is the test of choice when concerned for perforation. 03:22 The pros here, what are the advantages of a CT scan? A CT scan can detect small amounts of free air. 03:29 It can determine the underlying problems. 03:32 So if your patient needs to go to the operating room for free air or a perforated viscus, it’s gonna tell the surgeon, do they have a hole in their stomach? Do they have a hole in their large intestine? Do they have a hole somewhere else? It can give you an idea as to what is going on, what caused the perforation, what needs to be fixed, and it can also detect other things in your differential diagnosis more than x-ray. 03:54 So let’s say you send your patient to the CT scanner and you really think that they have a perforated viscus but they come back and it turns out they have appendicitis, or diverticulitis, or another ideology of their pain, your CT scan can tell you that. 04:10 Your x-ray cannot tell you that. 04:12 The x-ray cannot give you that additional piece of information. 04:16 The cons are is that it takes more time, your patient leaves the Emergency Department. 04:21 I mentioned that sometimes these patients can be very sick. 04:25 They can have low blood pressure, they can have altered mental status. 04:28 You may be hesitant to send them to the CT scanner. 04:32 They leave the Emergency Department for a short period of time but this is really your best test of choice that’s gonna give you the most information here. 04:41 The other con is that it does expose patients to ionizing radiation. 04:45 Again, I think in medicine, we always have to think about things in a risk benefit ratio, and if you’re worried that someone has free air in their abdomen, the risk of getting that test is very minimal. 04:58 So looking at the CAT scan for perforated viscus, what are the concerning things that you see? So looking at the CT scans in the anterior abdominal wall, just beneath the soft tissues, you could see the area of black space. 05:11 That’s an area of free air. That should not be there. 05:15 This patient has concern that they have a perforation or a hole somewhere in their intestines. 05:21 Either it’s in their stomach or their small or large intestine. 05:24 Ultrasound is the last imaging modality to discuss. 05:28 Ultrasound is utilized with increased frequency nowadays. 05:31 It can detect free air. 05:35 It can also show enhancement of a peritoneal strip, and the pros here are that it can be performed very easily at the bedside. 05:43 The cons are that this requires a skilled individual to perform. 05:47 This isn’t necessarily a common indication that emergency medicine physicians study when they’re in residency or beyond to look for on ultrasound, so this will require a skilled ultrasound technologist, a skilled radiologist to take a look at the images and see if that is in fact there.
About the Lecture
The lecture Perforated Viscus: Diagnosis by Sharon Bord, MD is from the course Abdominal and Genitourinary Emergencies.
Included Quiz Questions
Which standard laboratory test must be done in all women of child-bearing age presenting to the ED for abdominal pain?
- Urine HCG
- CBC
- Lipase
- Lactic acid
- Electrolyte panel
What is the test of choice in patients with suspected perforated viscus?
- CT scan
- Plain film x-ray
- Ultrasound
- MRI
- Angiogram
In requesting a plain film x-ray, several views are needed in order to adequately assess the presence of free air in the abdomen. Which of the following x-ray views is NOT useful in the evaluation of a perforated viscus?
- Oblique abdominal view
- Upright abdominal view
- Supine abdominal view
- Upright chest PA view
- Lateral decubitus film
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |