Playlist
Show Playlist
Hide Playlist
Pathogenesis of Glomerular Disease
-
Slides GlomerularDiseaseOverview RenalPathology.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
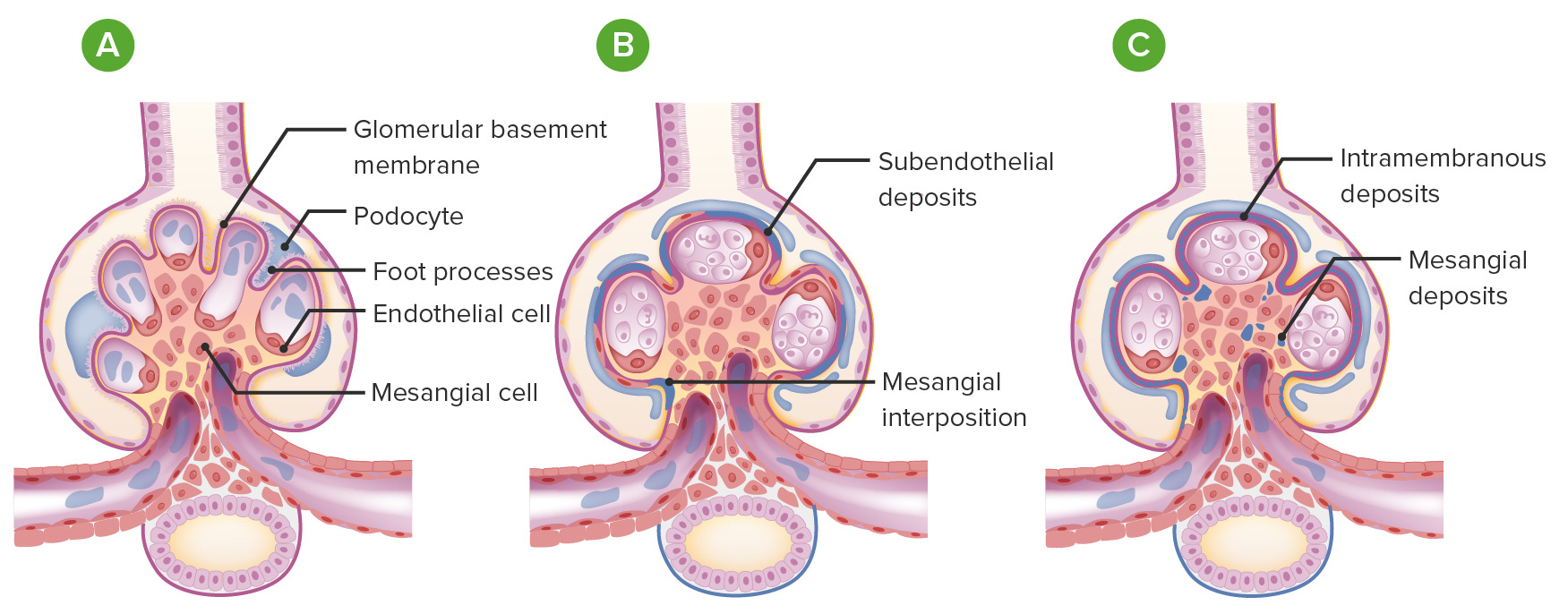
00:00 light microscopy H&E, we have immunoflurorescence, and number 3 electron microscopy. Let's move on. 00:00 Here in a cartoon form, we are showing you pathogenesis of glomerular disease and I will show you two major issues. The first one that you are seeing here, let me just set up this picture. This picture that you are seeing is the glomerulus. Next, what you are seeing there in blue, purple? That is going to be your podocyte. How can you confirm that? A podocyte should have food processes. You see that box around that podocyte in that blue cell. We are going to take that section and we are going to blow it up over anterior right. So now we have amplified it or blow it up, and that dark blue structure or the violet structure that we are seeing is a huge podocyte with a nucleus. And then we are seeing food processes. Identify those first. Next, you see that orange line. It looks like paint or if you take a brush looks like you paint it with an orange brush. Well, that's your glomerular basement membrane, isn't it? So now what we do is along with that orange line, which is your glomerular basement membrane and the epithelial cell, are you either going to deposit some of these immunoglobulins either underneath the epithelial site or you are going to deposit it where? Underneath endothelial site. And what you are clearly seeing here, ladies and gentleman is immune complexes that are being deposited underneath the endothelial cell. Between the endothelial cell and the basement membrane on that first picture where it's circulating, you noticed that that is a subendothelial deposit. 01:39 First and foremost, would light microscopy show you this? No. Would electron microscopy show you this? Absolutely. And number 3, immunofluorescence, but then recognizes beign what kind of pattern? Granular. Let us now move into the membrane a little bit. The one in the middle that you see there is you have immunoglobulins and what do these immunoglobulins do? These immunoglobulins are literally only attacking the glomerular basement membrane. 02:08 That is it. We will call this in situ. What does in situ mean? Membrane. Doesn't it? So literally here all you have is immunoglobulins that are attacking some antigen of my glomerular basement membrane. This is a type II hypersensitivity. This is antiglomerular basement membrane diseases. 02:27 There are no complexes that are being formed and no deposits. So, therefore, on let us say electron microscopy, maybe you find changes within the membrane. Great, but then here, immunofluorescence. 02:42 Immunofluorescence will show you, you see that orange basement membrane are completely containing immunoglobulins. So, therefore, the entire basement membrane is going to be "laid up." So this gives us our linear pattern. Then, moving over to the far right, the two things that are occuring here. Take a look at the difference between the one on the middle and the one on the right. The one on the right, not only are you attacking the membrane, but where else are you depositing? It is depositing underneath what is that blue cell that we called earlier? That is a visceral epithelial cell. That is a podocyte and so, therefore, the fact that you have involvement of the membrane and you have deposits underneath the epithelial cell. This is no doubt membranous glomerulonephritis, involvement of the membrane in what kind of hump or deposit? A subepithelial deposit. So therefore, electron microscopy would be relevant here and immunofluorescence will show you what? A granular pattern. 03:50 Through these pictures on immunofluorescence will then give you granular pattern, which two? The one on the left with subendothelial, the one on the right with subepithelial and the one in the middle immunofluorescence would be what pattern? Linear. Just to make sure we have complete our discussion. If you take a look at the big picture on your left of the entire glomerulus or a section of the glomerulus, the middle there that you are seeing in green is a mesangium. And then just to make sure we're clear that orange cell that we're seeing with subendothelial is the endothelial cell and so therefore that would be your capillary lumen. Everything is in properly annotated here. Spend a little time. 04:33 Make sure that you take a look at the text from the previous discussions, arrive here, take a look at the picture and let's now continue forward with more pathology. 04:44 So real quick, let me just have your highlight subepithelial deposit. Take a look at it. Underneath the epithelial cell maybe immune complexes, what would you then call this? Immunofluorescence. 04:57 This would be granular. On the bottom, subendothelial. Underneath the endothelial cell, immune complexes once again granular. Everything else has been properly annotated here for you. These are circulating in immune complexes. Let me give you an example now. Let us build down a little bit of foundation. Subepithelial, I will give you PSGN, which one? Post-streptococcal glomerularonephritis, subepithelial. Subendothelial would be something like a SLE prototype known as DPGN, diffuse proliferative glomerularonephritis. How did I know that? Years and years and years of learning and practicing. You will get this done as well in which at that point you might have to memorize a little bit. Here strictly what are you doing? The immunoglobulins are attacking the basement membrane only. May I ask you something? Do you find any immune complexes here? No. So therefore, on immunofluorescence, what kind of pattern would you call this? Very good. Linear. Welcome to Goodpasture, type II hypersensitivity. And then finally a picture here is showing you not only involvement of the membrane. Take a look, but then also what kind of deposit would you call that underneath that epithelial cell? Obviously, it is subepithelial. 06:18 What would be my diagnosis here? Take a look. This is membranous glomerulonephritis. Further exapanding upon the overview picture that we began with and then further dissecting into each individual pathologies. Type III hypersensitivity, immune complexes.
About the Lecture
The lecture Pathogenesis of Glomerular Disease by Carlo Raj, MD is from the course Glomerulonephritis.
Included Quiz Questions
Which of the following is a characteristic feature of Goodpasture syndrome?
- Linear immunofluorescence pattern
- Granular immunofluorescence pattern
- Subepithelial immune complex deposition
- Subendothelial immune complex deposition
- Intramembranous immune complex deposition
Which of the following is a characteristic feature of diffuse proliferative glomerulonephritis?
- Subendothelial immune complex deposition
- Linear immunofluorescence pattern
- Subepithelial immune complex deposition
- Anti-basement membrane antibodies
- Mesangial immune complex deposition
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |