Playlist
Show Playlist
Hide Playlist
Otitis Media (Middle Ear Infection) in Children
-
Slides OtitisMediaExternaMastoiditis Pediatrics.pdf
-
Download Lecture Overview
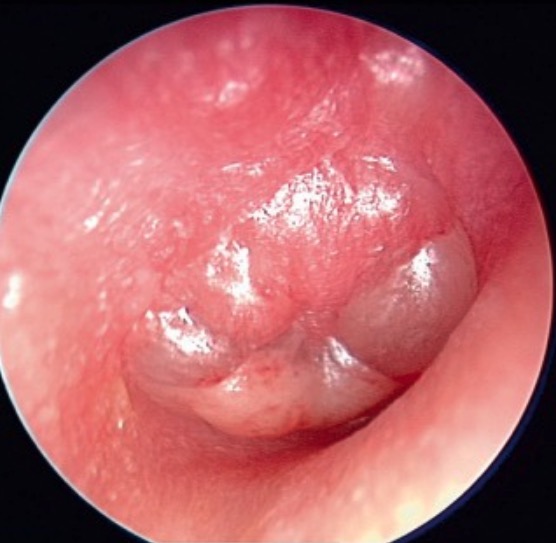
00:01 In this lecture, we will review otitis media, mastoiditis and otitis externa, basically all problems with pediatric ears. 00:12 Let’s start with otitis media. 00:14 Here’s a picture of an ear. 00:16 As you can see, there’s the external ear and the ear canal. 00:20 That’s infected in otitis externa. 00:22 Behind the tympanic membrane is this red chamber here, which is the middle ear. 00:27 That’s where otitis media occurs and that area is drained by a tube that goes down to the nose. 00:34 When that tube is closed off or inflamed, you can create an otitis media as bacteria grow in that chamber and the pressure builds up and it becomes very uncomfortable. 00:45 That’s otitis media. 00:48 So, acute otitis media is generally an acute bacterial infection. 00:55 This is to be distinguished with otitis media with effusion which is usually non-infectious. 01:01 This may be something like allergy or a reaction to secondhand smoke causing a poor drainage of that tube and buildup of pressure but not with primarily bacterial growth. 01:14 So let’s talk about infectious otitis media first. 01:18 Ninety percent of children will get it before the age two. 01:22 The peak age is between 6 months and 18 months of age and it’s usually associated with a viral URI. 01:31 Basically, you have a viral infection and that closes off that drainage tube and then bacteria can take over and start growing in that middle ear chamber. 01:43 The classic pathogens are Strep pneumo, nontypeable H. flu and Moraxella catarrhalis. 01:50 Strep pneumo, nontypeable H flu and Moraxella catarrhalis, common question on tests. 01:58 So are there some risk factors? Sure, especially risk factors for upper respiratory infections like daycare exposure or being alive during the winter months is plenty risk alone. 02:12 But there are other specific otitis media risk factors, so that when they get that cold it turns into an ear infection. 02:19 One is secondhand smoke exposure. 02:22 Another one is an infant that does not breastfeed. 02:26 Breastfed infants are far less likely to develop otitis media than non-breastfed infants. 02:32 Infants with a cleft palate or other craniofacial anomaly may have an abnormality of the drainage of that Eustachian tube. 02:41 Patients with Down syndrome, for example, can have large tonsils and adenoids which can interfere with drainage and they are at increased risk for otitis media. 02:50 Also, if a family didn’t get a vaccine for strep pneumo, they are at increased risk for otitis media. 02:57 So how does otitis media present? Generally with fever and fussiness, ear pain and sometimes grabbing at ears. 03:06 Although be careful, there is age at which kids sort of discover their ear and that doesn’t necessarily mean there is something wrong. 03:13 Certainly, if there is otorrhea or pus coming out of the ear, that’s a clear sign that not only there has been an infection but it is perforated. 03:23 The good news for the patient is once it perforates, it’s far less painful, because that pressure has been relieved. 03:30 So let’s talk about otoscopy. 03:33 This is when you look at a patient’s ear. 03:35 Here’s a normal ear. 03:37 You can see some landmarks like the bony structures, the malleus and the incus. 03:41 You can’t see the stapes, it’s farther end. 03:43 And you can see a normal light reflex there, it looks pretty good. 03:49 Here’s the caveat though and I’m just going to bring this up and say it, is that you have probably as a student seen lots of people look in the ears and say, “Oh, looks red to me," "Looks infected" or "Looks normal to me” and they didn’t insufflate. 04:03 Without pneumatoscopy, that’s when use that bulb to move the eardrum back and forth, you’re actually doing a far worse exam and I don’t care how good you are at ears. 04:15 I don’t care if you’re the best ear doctor on the planet. 04:18 If you’re not doing pneumatoscopy, you’re having a hard time distinguishing those ears that are middle ground. 04:24 Certainly, we have all looked in there and seen a horrible ear and didn’t need to do pneumatoscopy. 04:29 But on those borderline cases, if that ear is moving, that means that Eustachian tube is patent because the pressure can be relieved by blowing down that Eustachian tube. 04:39 So, a mobile ear is far less concerning and we can probably save ourselves a lot of infected eardrum treatments if we simply check with pneumatoscopy first, because if that ear is moving, you should be much less concerned. 04:53 So movement is the most important part of the ear exam and without that bulb, you really aren’t checking for it. 05:00 So here is an example of an infected ear, you can see it’s bulging. 05:05 You can see, you no longer can clearly see the bony landmarks of that ear. 05:09 This is a bad ear infection. 05:12 Here is a serous otitis. 05:14 It’s bulging a little bit, but it’s not too bad. 05:17 You can see that there is some bulge there. 05:20 So how do we manage otitis media? Well, we have made the diagnosis. 05:25 The patient has a purulent appearing TM and it’s not moving. 05:30 Well, if the child is over six months of age, the first step may well be watchful waiting. 05:36 Not every otitis media requires antibiotics. 05:39 This is especially true in non-severe infections and what you might do is watch off antibiotics for two to three days and then treat if it doesn’t improve. 05:48 Some practitioners like to give them on a script to say wait two days. 05:51 If it’s still bothering them, then fill it. 05:53 There is a lot of variability in practice. 05:56 One thing that's clear though is we should treat for fever and pain with ibuprofen and that’s indicated. 06:02 Okay. 06:03 So if we decide then to treat, it’s a severe case, it’s a kid under six months of age or it’s been two days and it’s not getting better, then our first line antibiotic is amoxicillin high dose which is 80-90 mg per kilo per day divided twice a day. 06:20 Why high dose? Well, there is one bacteria in particular that develops resistant to amoxicillin by altering its penicillin binding proteins, that’s Streptococcus pneumoniae. 06:32 If you have a patient with Strep pneumo which is the number one bacterial cause of otitis media, you’re going to need the higher dose to encourage the penicillins to be more in the bound form with the penicillin-binding protein. 06:45 In other words, by raising those, you sort of the force that equation to the right. 06:50 You create more binding. 06:52 Okay, if the high dose amox fails, then we may say, maybe there’s a resistant gram negative. 06:59 Strep pneumo is almost ubiquitously sensitive to high dose amox. 07:03 So then, you would go to Augmentin because you’re adding a beta lactamase that will be treating the resistant forms of H. flu non-typeable or Moraxella catarrhalis. 07:14 Alternatively, you may also use ceftriaxone, but we’re trying to limit the amount of ceftriaxone we use in this world since resistance to third generation cephalosporin is going to be a problem of your generation even more than it is of mine. 07:29 Lastly, if it’s still not responding, you might consider ENT referral for a myringotomy and a culture. 07:36 Myringotomy will immediately relieve the pain and the culture will give you a sense of why exactly this patient isn’t responding to the standard antibiotics. 07:45 Okay. 07:46 We also want to refer to ENT if there’s a problem that is chronic in nature or if a patient is getting recurrent otitis media. 07:54 They may be able to put in tympanostomy tubes. 07:57 Here you can see an ear where they have inserted a tube into the tympanic membrane to allow for continuous drainage. 08:03 This is great. 08:04 Now this patient doesn’t need their Eustachian tube to drain. 08:07 There is one coming straight out of the eardrum. 08:10 This prevents buildup of pressure and prevents that backlog of bacteria growing behind that tympanic membrane. 08:17 It may improve hearing, but it does not improve long-term speech problem and this is not recommended for hearing issues and speaking issues alone. 08:26 It’s really for recurrent or chronic otitis.
About the Lecture
The lecture Otitis Media (Middle Ear Infection) in Children by Brian Alverson, MD is from the course Pediatric Emergency Medicine.
Included Quiz Questions
Which of the following is indicated in a 4-year-old boy with a first episode of otitis media?
- High-dose amoxicillin
- Normal dose amoxicillin
- Azithromycin
- Amoxicillin/clavulanate
- Trimethoprim-Sulfamethoxazole
Which of the following is a risk factor for otitis media in children?
- Secondhand smoke exposure
- Breast feeding
- Vaccination
- Warm weather
- Introduction of solid food to the diet of the infant
An 8-month-old child has been diagnosed with acute otitis media based on symptoms and physical examination. Which of the following is the most appropriate management at this time?
- Watchful waiting for 2-3 days
- Culture-directed antibiotic therapy
- Surgical drainage
- Follow-up within 1 week without therapy
- Start antibiotic treatment immediately
Which of the following is an appropriate therapy for chronic otitis media?
- Tympanostomy tube
- Long-term high-dose amoxicillin
- Prophylactic amoxicillin-clavulanate
- Regular surgical drainage
- Steroids
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Thank you Dr. Alverson for this concise and easy to understand lecture. Even though it is a straight forward topic, as a student I believe I really benefited from your delivery.