Playlist
Show Playlist
Hide Playlist
Neonatal Hyperbilirubinemia (Neonatal Jaundice)
-
Slides NeonatalHyperbili Pediatrics.pdf
-
Download Lecture Overview
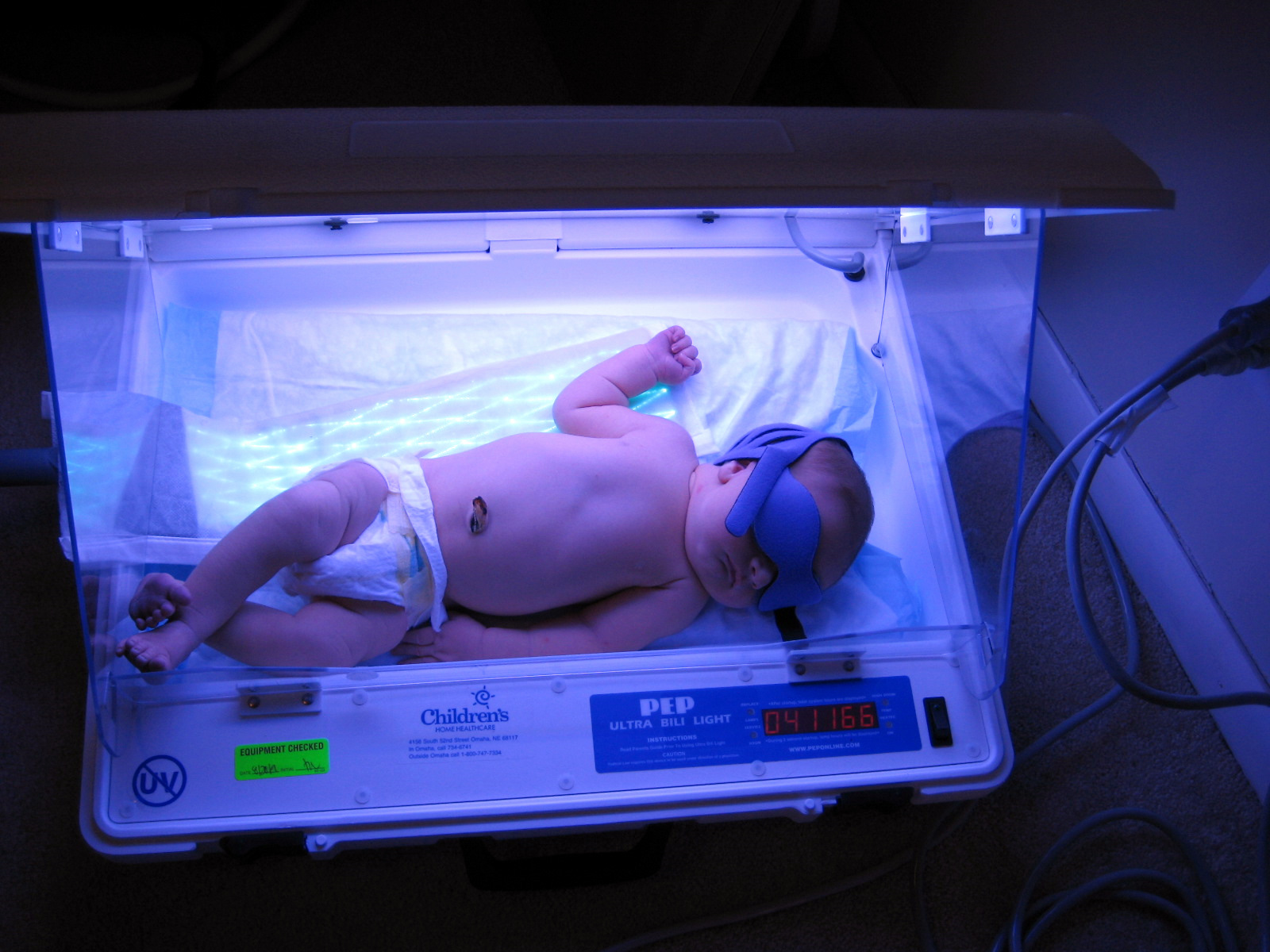
00:01 In this lecture, I’m going to discuss hyperbilirubinemia in the newborn. 00:07 Okay. 00:08 Here is a child with hyperbilirubinemia. 00:11 This is almost always a completely benign condition. 00:15 But it can be either physiologic or pathologic. 00:19 And it is important for you to be able to distinguish the difference. 00:23 Remember, almost half of infants will have visible jaundice after birth as a result of hyperbilirubinemia. 00:31 So in newborns, basically, they have a higher hemoglobin and at that period in their life then never again. 00:38 This results with an increased release of hemoglobin because of red blood cell breakdown. 00:44 Remember, newborn red blood cells have a shorter half life, about 70 days, compared to adult red blood cells around 120 days. 00:54 And during the newborn period, there is less efficient hepatic conjunction of the bilirubin and excretion into the intestinal tract. 01:04 So let’s go through the physiology of it. 01:07 There’s breakdown of hemoglobin and other heme proteins. 01:10 This results in an unconjugated bilirubin, which is about half the time bound to albumin. 01:17 If there is free bilirubin in high levels, this cross into the blood brain barrier and cause kernicterus. 01:25 And kernicterus is brain damage. 01:27 That’s bad. We want to avoid that. 01:29 So we have this whole system of getting the unconjugated bilirubin out of the blood. 01:35 It gets conjugated in the liver and then the conjugated bilirubin is extruded through the biliary tract and into the stool, which is secreted as stercobilinogen, which is what makes our stools brown. 01:50 However, some of it does go through enterohepatic circulation and get reabsorbed and go back up and do it again. 01:58 Additionally, a small percentage will go to the kidneys and be peed out as urobilinogen. 02:06 So hyperbilirubinemia in an infant may not just be a problem with increased red blood cells breaking down or a problem with the conjugation or extrusion of the bilirubin through the normal systems. 02:21 It could be a sign of another problem. 02:23 And so we worry a little bit about these babies and we think could there be something else going on. 02:28 An example is hemolytic anemia. 02:31 So an infant who’s having an autoimmune hemolytic anemia and that’s common and we’re going to talk about it in a little bit. 02:38 Those infants are going to have more red blood cell breakdown than a regular baby would. 02:42 And they will generally turn yellow. 02:45 Infants who are infected for whatever reason can present with jaundice. 02:51 Infants with metabolic disease can also present with jaundice and make sense that infants with liver disease may present with jaundice as well. 03:01 So we see a baby, we think any of these things could be going on. 03:06 Let’s talk a little bit first about what happens if we don’t fix the problem. 03:09 In infants with very high levels of unconjugated hyperbilirubinemia, this can result in Kernicterus and you can see a brain here of a baby who’s had deposition of bilirubin in his brain parenchyma where those two green arrows are pointing. 03:25 This is bad for these children. 03:27 It can result in brain damage or death. 03:29 And in particular, affects the basal ganglia, which are responsible for coordination of movement among other things. 03:37 Okay. What if it’s hyperbili but it’s conjugated hyperbili rather than unconjugated? This is much rarer, but we have to know the difference because patients with conjugated hyperbili do not respond to light therapy the way our unconjugated babies do. 03:56 So we need to know what it is so we know how to treat it. 03:59 There are many different causes and they’re generally intrahepatic problems. 04:03 An example would be bile duct obstruction or a choledochal cyst, which is preventing drainage of that bile. 04:10 Alagille syndrome is whole syndrome among which they have problems with bile and bile duct extrusion. 04:17 They may have galactosemia, which can absolutely cause a conjugated hyperbili. 04:22 They may develop alpha-1 antitrypsin deficiency which can cause the liver damage from the build up of that alpha-1 antitrypsin in the liver and therefore, they can get problems with conjugation of their bilirubin. 04:34 They may have a protein metabolism defect, cystic fibrosis, or even neonatal hepatitis. 04:40 So there are many reasons, even that I didn’t list, that can cause a conjugated hyperbili in infants.
About the Lecture
The lecture Neonatal Hyperbilirubinemia (Neonatal Jaundice) by Brian Alverson, MD is from the course Neonatology (Newborn Medicine).
Included Quiz Questions
Which of the following is a common cause of unconjugated hyperbilirubinemia in neonates?
- Physiologic jaundice
- Choledochal cyst
- Bile duct obstruction
- Cystic fibrosis
- Neonatal hepatitis
Neonates have an increased tendency to develop hyperbilirubinemia. Which of the following is a cause of this?
- Elevated hemoglobin
- Increased red blood cell lifespan
- Increased hepatic conjugation
- Decreased enterohepatic circulation
- Increased bile excretion
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Excellente lecture as usual. Gives a clear overview of the disease and its causes.