Playlist
Show Playlist
Hide Playlist
Necrotizing Enterocolitis
-
Slides NecrotizingEnterocolitis Surgery.pdf
-
Download Lecture Overview
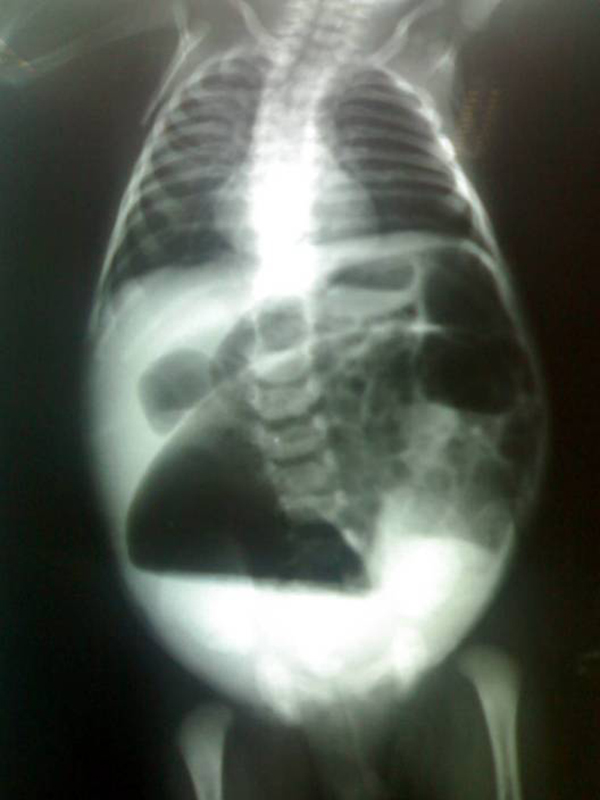
00:01 Welcome back. 00:02 Thanks for joining me in this discussion of necrotizing enterocolitis in the section of pediatric surgery. 00:09 Necrotizing enterocolitis is usually associated with premature babies and the onset of necrotizing enterocolitis (also called NEC) is usually after the first several weeks of life. 00:24 Although there is an association with bottle-fed babies and that the symptoms occur generally after the first few feeds, babies who are not bottle-fed can certainly develop necrotizing enterocolitis as well. 00:38 So, on the examination, don't be fooled if the patient is not bottle-fed. 00:45 What are some physical findings of a baby who has potential NEC? Vomiting, diarrhea, perhaps abdominal distention, coupled with some wall erythema, although, note, an abdominal wall erythema is potentially a late finding. 01:02 And sometimes babies have bloody stools. 01:07 How does this baby look to you? Well, it's difficult to tell sometimes based on looking at the baby alone. 01:14 Oftentimes, pediatricians will tell you babies who fail to thrive... 01:18 again fail to thrive, meaning they're not progressing day by day as expected. 01:24 If you look closely here in this picture, the baby has a little bit of erythema around the central abdomen. 01:30 Abdominal distention is difficult to tell, particularly in a newborn. 01:35 All of their abdomens look a little protuberant. 01:38 Now, let's visit some specific findings. 01:42 Babies who are noted to be apneic or have respiratory failure. 01:46 These are also important findings in any baby who isn't doing well and has failure to thrive. 01:53 Lethargy. 01:56 Shock and hypotension. 01:58 Again, much like abdominal wall erythema, shock and hypotension is potentially a late finding in NEC. 02:06 And coagulopathy. 02:09 This is very similar in adults who develop disseminated intravascular coagulopathy (DIC). 02:18 The Bell criteria are used to stage NEC into three categories. 02:22 Stage I is the mildest form, with non specific symptoms such as lethargy, unstable temperature, apnea, abdominal distention and vomiting. 02:30 Stage II is more severe and have absent bowel sounds and abdominal tenderness. 02:34 Stage III is the most severe and can encompass bowel perforation. 02:38 The slide has the full criteria that you can check out but you don't have to memorize them. 02:44 What might you find on routine laboratory studies? Here, you see the chemistry shows a hyponatremia, potentially a low chloride, and in certain circumstances, decreases in the hemoglobin and hematocrit, particularly if the baby has hematochezia or bleeding per rectum.
About the Lecture
The lecture Necrotizing Enterocolitis by Kevin Pei, MD is from the course Special Surgery.
Included Quiz Questions
Which of these findings are NOT seen in a patient with necrotizing enterocolitis?
- Increased bowel sounds
- Erythema of the abdominal wall
- Vomiting and diarrhea
- Abdominal distention
- Hematochezia
What findings would you expect in a baby with necrotizing enterocolitis?
- Coagulopathy
- Hypertension
- Subacute proximal muscle weakness
- Abscess
- Constipation
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
Most reliable content with clear and accurate for easy understanding