Playlist
Show Playlist
Hide Playlist
Necrotizing Enterocolitis
-
Slides GIP Necrotizing Enterocolitis.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
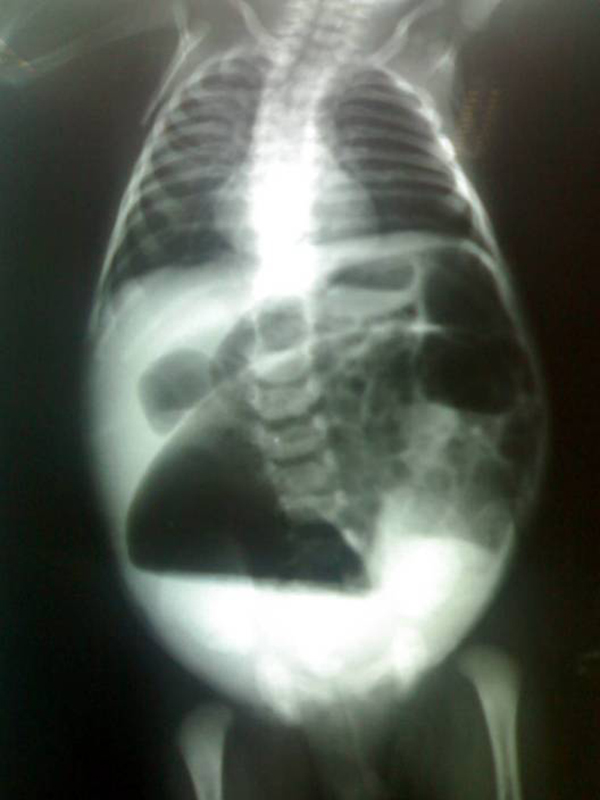
00:01 Welcome. We're going to talk about a particularly troublesome and potentially lethal disorder called necrotizing enterocolitis. 00:10 Necrotizing enterocolitis or NEC is inflammation with ulceration and necrosis, hence, the name necrotizing that occurs in neonates and primarily affects the terminal ileum and the colon. 00:25 The epidemiology of this. So, it's the most common cause of GI emergencies and intestinal perforation in premature infants and the key phrase there is premature infants. 00:37 So, prematurity is going to be a major risk factor for this entity. 00:41 Overall, necrotizing enterocolitis occurs in approximately one in 1000 live births. 00:48 The incidence however goes up quite a bit if you have prematurity and up to 5% of preterm infants admitted to the neonatal intensive care unit will develop necrotizing enterocolitis. 01:02 There is no single identified cause. There are a number of risk factors. 01:08 Then, again, number one for you to remember and tuck away forever is being born less than 32 weeks of age. 01:16 This is going to be a combination of an immature gut, perhaps abnormal GI colonization of the gut with certain microbiota. 01:26 This may be immature vasculature. But no single identified cause is going to be able to be pointed to. 01:36 A low birth weight, totally independently of prematurity can also give risk to this entity. 01:43 And then, there is a lot of epidemiologic evidence that formula feeding, especially, cow-based, bovine-based milk formulas can give rise to NEC and that may be due to the microbiota that particularly thrive on casing derived formulas. 02:02 Perinatal stress and it's not just, oh, the mom is stressed out. 02:06 But the fact that there may be shock and or sepsis due to infection is also a risk for NEC in the newborn. 02:16 Interestingly, there seems to be an association with congenital GI or cardiovascular defects. 02:22 Some of this may be because those defects are also associated with prematurity but there may be a completely independent and genetic association. 02:32 In terms of the pathophysiology, it's attributed to a poorly regulated innate immune systems. 02:37 So, again, in the premature infant, the immune system is not exactly ready to rock and roll and if there are microbiota that the immune system somehow is prime to respond to, that can lead to adverse accumulation of inflammatory mediators and ultimately, severe injury. 02:58 We've already kind of hinted at many of these associated findings that may predispose to NEC but certain genetic conditions, premature delivery leading to intestinal immaturity, an imbalance in intestinal microvascular tone, so, an immature vasculature, abnormal microbial colonization, and increased immunoreactivity. 03:26 So, all of these and maybe all of these are required in some measure to give rise to NEC. 03:34 This is a schematic to try to give you a sense of how the various factors may coalesce to give rise to necrotizing enterocolitis. 03:42 Here we have our immature immune system, our immature epithelium, and we have colonization by some bacteria indicated in the lumen. 03:53 There may be damage not otherwise specified and this may be due to ischemia, this may be due to inflammatory mediators, but the lightning bolts represent injury. 04:06 As we get injury, we're going to have increased inflammatory cell recruitment which will increase permeability to all of the organisms that are present within the GI tract. 04:17 Those GI microbes, again, dependent on the specific microbiota may have increased production of hydrogen gas and methane gas and other fermentation products which may dilate the bowel. 04:29 As you have increased bowel dilation, you will have increased pressure and compromise of a vasculature that may be relatively immature. 04:38 A combination of all of those things, we go from healthy pink cells to kind of unhealthy dead epithelial cells with translocation of the bowel flora into the peritoneum. 04:51 The clinical presentation is as you might expect. So, there is ongoing necrosis of the colon and distal ileum. 05:00 There is non-specific feeding intolerance with vomiting because we are not passaging things through the entire GI tract. 05:07 With necrosis of the colon, we may get hematochezia that is present on a diaper. 05:14 There will be abdominal distension and abdominal tenderness and most worrisome is that there are completely absent bowel sounds. 05:24 A stethoscope placed on the abdomen hears nothing. And that's kind of ominous. 05:29 It can rapidly progress within hours to irreversible hypotensive septic shock. 05:36 So, how are we going to make an expeditious diagnosis? This is a bad, lethal disease. 05:42 We need to find out sooner rather than later that it's happening in your patient. 05:46 An x-ray will commonly show dilated loops of bowel with air fluid levels as shown on the left-hand side. 05:55 And what's being shown on the right-hand side is a particularly ominous finding. 05:58 If you have bowel with air within the walls of the bowel, that's called pneumatosis intestinalis. 06:05 It means that you have bacteria within the walls of the bowel which means that they're translocating and the patient is at extreme risk of developing septic shock very shortly. 06:16 Ultrasound may be a method of analysis but a plain x-ray works just find. 06:21 The laboratories, if there is extensive bleeding, there will be anemia. 06:25 We will expect to see leukocytosis with the left shift. However, in very severe disease, you may have relative myelosuppression and there may even be leukopenia. 06:36 And as we are getting necrosis, we are actually activating, recruiting, and thrombosing vessels with - and losing platelets so there'll be a relative thrombocytopenia. 06:47 Stool will show an occult blood but frequently, it's bright red blood. 06:53 There's hematochezia. How are we going to manage this once we made the diagnosis? We want to get antibiotics on board as soon as possible to stave off a septic shock picture and unfortunately, the bowel is dead. 07:08 There's nothing to be done other than to resect it and we need to resect it. 07:13 As a result, the neonate will survive hopefully but will have a short bowel syndrome for the rest of their life. 07:23 Not a happy ending for a very important and serious disease. 07:28 But at least, now, you have some fundamental understanding of necrotizing enterocolitis.
About the Lecture
The lecture Necrotizing Enterocolitis by Richard Mitchell, MD, PhD is from the course Small and Large Intestines Disorders.
Included Quiz Questions
What is the strongest risk factor for necrotizing enterocolitis?
- Prematurity
- Hypertension
- Infection
- Vascular malformation
- Formula feeding
What pathologic mechanisms lead to necrotizing enterocolitis? Select all that apply.
- Immature immune system
- Bacterial colonization
- Epithelial damage
- Serosal hyperplasia
- Decreased epithelial permeability
What is the most worrisome clinical examination finding in necrotizing enterocolitis?
- Absent bowel sounds
- Nausea
- Constipation
- Hematochezia
- Hematuria
Which of the following are radiographic findings that are consistent with necrotizing enterocolitis? Select all that apply.
- Pneumatosis intestinalis
- Volvulus
- Multiple air-fluid levels
- Dilated loops of bowel
- Abdominal mass
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |