Playlist
Show Playlist
Hide Playlist
Modes of Ventilation: Ventilator Airway Pressure
-
Slides ModesOfVentilation RespiratoryPathology.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
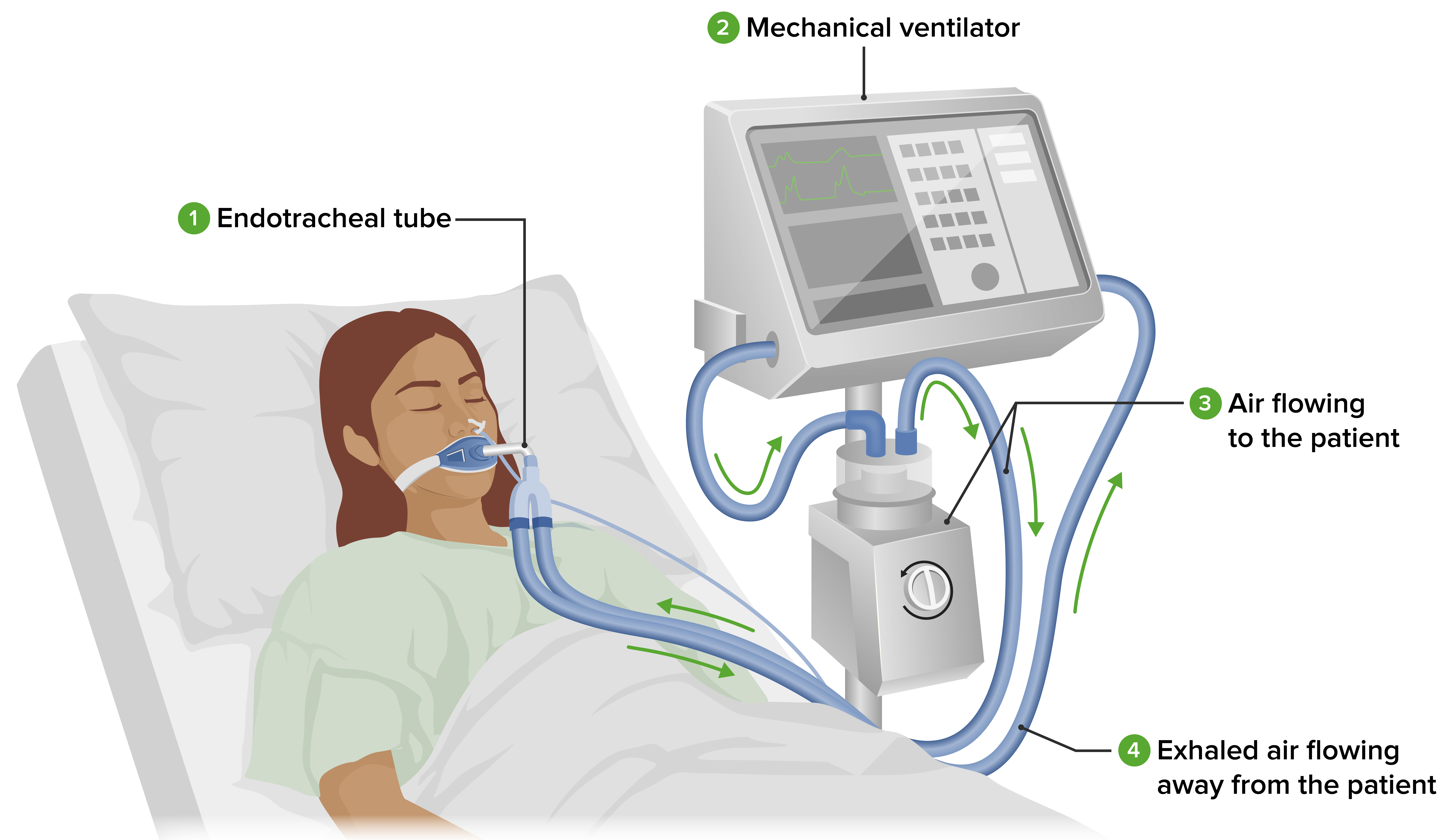
00:00 Airway pressure on the ventilator. Airway pressure on the ventilator, what kind of issues do you want to take a look at with this? Well, the ventilator will support out a peak pressure. 00:10 So what does that mean? Well, you are going to now introduce positive pressure, aren’t you? You are introducing positive pressure throughout the airways and then eventually, what is the objective? The alveoli. Keep that in mind. Let me show you a figure here that is going to give you a nice little analogy to exactly that. This is the airway pressure measured in the endotracheal tube with each breath. Listen, airway pressure is what you are focusing upon here, I will show you. Now, more important though is the pressure in the lungs, in the plateau pressure, which is measuring the distending pressure of whom? The alveoli. 00:46 So, for example, you take a look at this image. In this illustration, shows you a bubble and that then represents the lung or the alveoli. But then you actually have the airway to the left proximally. So, you can increase pressure in two places. That airway pressure or the lung. Think of this as kind of being like a balloon. So, you have a straw in the balloon. 01:08 The pressure in the balloon is more important, that is the lung, than the pressure in the straw, isn’t it? But in the mean time that you need to make sure that you are able to properly measure the pressure in the airway. So the goal of this is to minimise the trauma to the lung leading to further lung injury or even perhaps, remember, if you increase the lung volume so much, you might actually introduce some type of pneumothorax. Something like a tension pneumothorax. What does that mean? Well, that is your ball and valve effect. 01:39 A simple analogy there. You put air into a football. Air doesn’t leave. The football is the lung, tension pneumothorax. You are putting air into the pleural cavity. Air is not coming out. What are you creating? Tension. Keep that in mind. We will have that discussion when the time is right. In ARDS the goal plateau pressure is less than 30 cm H2O. You need to know the units that you are gonna use here for pressure, specifically. 02:13 Complications of mechanical ventilation. Lot of this should be pretty straight forward, but nonetheless, let's make sure that we are clear. While you put in endotracheal tube, understand that there might be organisms that you are introducing into the pulmonary system. 02:26 Not good. What about these organisms? Often times, resistant. Scary. Pneumothorax, we talked about, mean to say that you have enough pressure. At some point in time, there might be a little bit of tear of your parenchyma in which air then escapes into the pleural cavity upon inspiration, it doesn’t leave, often times, tension. We will talk about auto PEEP coming up and that will make perfect sense to you. Remember once again, as you increase the pressure at some point, it may then cause barotraumas. Tracheal damage. You literally are going, well, might break a couple of teeth when due intubation and you might actually introduce lesions into the trachea. If it lasts two weeks or longer, your next step of management, so that you avoid further damage, a tracheostomy. Critical care, always worry about myo or perhaps neuropathy. 03:20 So, mechanical ventilation complications are things that you want to keep in mind. Okay,
About the Lecture
The lecture Modes of Ventilation: Ventilator Airway Pressure by Carlo Raj, MD is from the course Respiratory Failures.
Included Quiz Questions
Which of the following is not a recommended goal of mechanical ventilation?
- Increase the PaCO₂ to more than 45 mmHg.
- Minimize oxygen to prevent toxicity.
- Minimize PEEP.
- PaO₂ of more than 60 mmHg.
- Balance the effects of high FiO2 with high PEEP.
Which of the following conditions most likely requires a high FiO2 and PEEP?
- Acute respiratory distress syndrome
- Tuberculosis
- Asthma
- Emphysema
- Lung abscess
Which of the following measures can lead to barotrauma during mechanical ventilation?
- Setting the inspiratory positive airway pressure to a maximum level.
- Setting the respiratory rate of mechanical ventilation.
- Setting the tidal volume of the mechanical ventilation.
- Minimizing the exposure time to positive pressure ventilation.
- Setting the amount of positive pressure required for reaching the tidal volume.
Which of the following is the most appropriate tidal volume recommended in a patient with ARDS?
- 6 mL/kg of body weight.
- 10 mL/kg of body weight.
- 8 mL/kg of body weight.
- 16 mL/kg of body weight.
- 12 mL/kg of body weight.
Which of the following is the goal plateau pressure used in the management of acute respiratory distress syndrome?
- < 30 cm H2O
- < 30 mmHg
- < 40 cm H2O
- < 40 mmHg
- < 13 cm H2O
Which of the following statements is false?
- The plateau pressure measures the airway pressure.
- The plateau pressure measures the distending pressure.
- Airway pressure is the pressure measured in the endotracheal tube with each breath.
- The plateau pressure measures the pressure in the lungs.
- The goal is to minimize lung injury or pneumothorax.
What is the recommended timeline during which tracheostomy can be used as a management strategy?
- If mechanical ventilation lasts for at least 2 weeks.
- If mechanical ventilation lasts for at least 2 days.
- If mechanical ventilation lasts for at least 2 months.
- If mechanical ventilation lasts for at least 4 weeks.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |