Playlist
Show Playlist
Hide Playlist
Modes of Ventilation: Pressure Support
-
Slides ModesOfVentilation RespiratoryPathology.pdf
-
Reference List Pathology.pdf
-
Download Lecture Overview
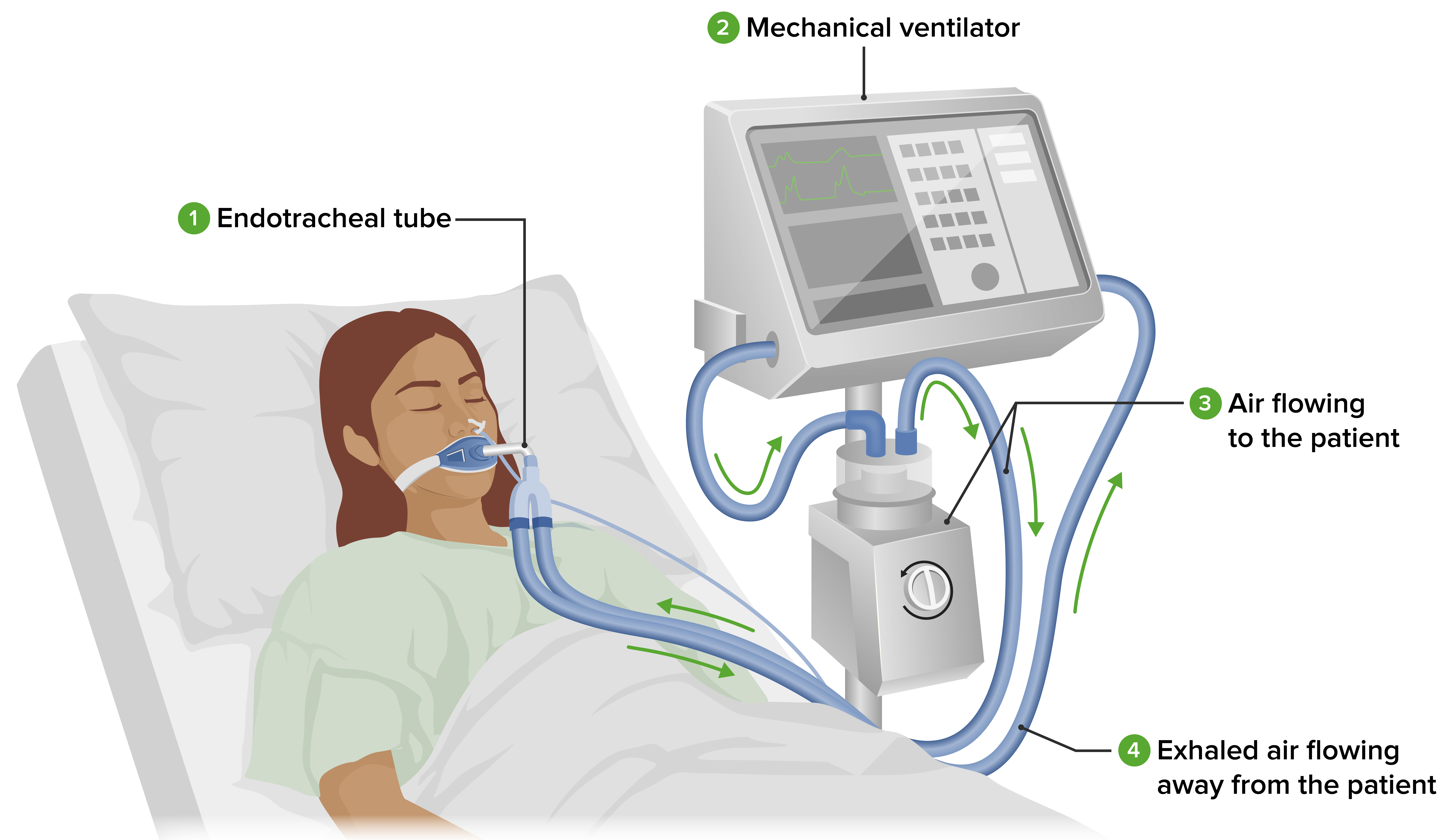
00:02 Let's continue. Okay. Now, what is this pressure support? Well, we have two different types of positive air pressure. And you want to be familiar with both types. Extremely common when you do your rotations. We already talked about CPAP. That means continuous positive airway pressure. Now, used to be once upon a time, that this was cheaper. That was important for you to know, wasn't it? Because if you find that CPAP was cheaper than BiPAP and you had two answer choices, you would go with CPAP. But, understand. Now because of advancement, BiPAP is economically just as reasonable as CPAP. Now what does that even mean? So, continued mean that you are going to introduce positive pressure into the airways so that you can do what? Good. Increase the volume of the lung. So, what does BiPAP even mean? Well, our discussion earlier, when we talked about severe respiratory failure type 2. What does type 2 respiratory failure mean to you? Good. Apart from the fact that you have hypoxemia with a PO2 less than 60, you also have retention of carbon dioxide. What's problematic? Definitively above 40. So now you are retaining your carbon dioxide which means you have impairment of your exchange. May I ask you something? What might you want to do as a clinician so that you can blow off that carbon dioxide which is type 2 respiratory failure? Just because you introduce oxygen into the alveoli which is CPAP, which is something that you want to think about in terms of managing a patient with obstructive sleep apnea, and that might be effective there. But just because you are introducing oxygen into the alveoli, does that mean that you are blowing off your carbon dioxide? How do you blow off your carbon dioxide? Oh, exhalation. So, why not come up with technology or technique or maneuver or pressure support which then allows not only for the patient to then be introduced with air, but then also what? Good. Exhalation. This is bilevel positive airway pressure. 02:09 Welcome to BiPAP or BPAP. Both one and the same. By Bi-level, we mean that not only are you assisting your patient with inspiration airway pressure, but you are also doing what please? You are also helping the patient blow off that carbon dioxide with expiration or exhalation. Is that clear? Of the two answer choices. So here you have identified a patient with COPD. You found that the pH has decreased. Okay. You find that the CO2 is elevated meaning above 40. So, you tell me what kind of respiratory failure? Type 2. 02:45 What type of ventilatory support would you like to then provide? You have two answer choices that you have now dwindle it down to. CPAP or BiPAP? You will correctly and confidently choose BiPAP. Because you want to get rid of that carbon dioxide. 03:01 Is that clear? Now, as we move on, we will then talk about ETT. It stands for endotracheal intubation. 03:10 So, if your patient, and we will talk about this upcoming. But endotracheal intubation and ventilator, well, here, there are certain goals and objectives that you want to keep in mind at this point in your education and then as you move on into rotations and when you actually insert it or intubate your patient, well there are other things that you will move into further detail. Let's take a look at the graph, shall we? So, we have the patient down at the bottom with flow. So, flow inside into the lungs means what to you? Inspiration. 03:39 Inspiration, hence the hump. So the flow is going to increase into lung during inspiration. 03:45 Is that understood? Do not confuse this with the loops that we did, loop spirometry. Can we quickly recap that? Because that is important and that we want to make sure you have in your head with great detail. That loop spirometry that we looked at, at the upper half was what? Expiration. The inner loop was what? Inspiration. That is different. Is that clear? This is strictly in terms of your natural breathing. The flow is what you are paying attention to. The flow is going to increase into lung upon inspiration. Okay. So now this patient requires help. And remember, once again, you want to make sure that you reach a nice and plateau level in which there is enough air that you are introduced through inspiratory, IPAP, stands for inspiratory positive airway pressure. You have a minimum and a maximum threshold. So right in that middle is where you wish to be. As far as you as clinician So therefore, you keep increasing the positive pressure. What does that mean to you? You are introducing air into the lungs. Good. What is the physio? The physiology without the ventilation means negative pressure. Keep those separate. So now, you are being the lungs, you are introducing positive pressure, you introduce positive, so that you introduce more air into the system, but you do not go beyond the max. You see the top dash line? That is the max. Why? You go above max, you might be introducing quite a bit of, well, injury to the alveoli. Remember, you don't want to get to the point where it gets so big that you are causing damage. Maybe tension pneumothorax or maybe, remember that conversation we had where, and we'll talk about this again, not to worry. If that alveoli becomes so fat and you have a fat alveoli in your lungs, guess what? You are compressing the adjacent structure. What is that adjacent structure? Good. Your pulmonary capillaries. You knock that out, you'll have all kinds of issues. Pulmonary hypertension, may be right-sided issues. So, your target, what you see there, at the very end of the graph, on your right, it says target VT. What VT mean? Tidal volume. So, this is a patient that requires help to reach a target volume or tidal volume in which the patient is able to breathe comfortably having proper gas exchange. Let's take a look. 06:03 So, we talked about BiPAP. ETT stands for endotracheal tube. Patient initiates a breath, then gets support with it. And usually, a backup rate is always set. Okay, so that is more of a clinical type of backdrop, but there is the full picture of what you are doing here with pressure support. Your graph becomes the most important point. Understand what a BiPAP is and we talked about that in great detail. 06:26 Continue.
About the Lecture
The lecture Modes of Ventilation: Pressure Support by Carlo Raj, MD is from the course Respiratory Failures.
Included Quiz Questions
Which of the following is true regarding mechanical ventilation?
- BiPAP assists with inspiration and expiration.
- BiPAP assists with inspiration only.
- BiPAP assists with expiration only.
- CPAP has become more expensive over the years.
- BiPAP provides negative pressure support to the alveoli.
Customer reviews
1,0 of 5 stars
| 5 Stars |
|
0 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
1 |
Very poor explanations need to provide answers for questions he asks he assumes too much.