Playlist
Show Playlist
Hide Playlist
Mitral Regurgitation – Systolic Murmurs
-
Reference List Physical Examination.pdf
-
Download Lecture Overview
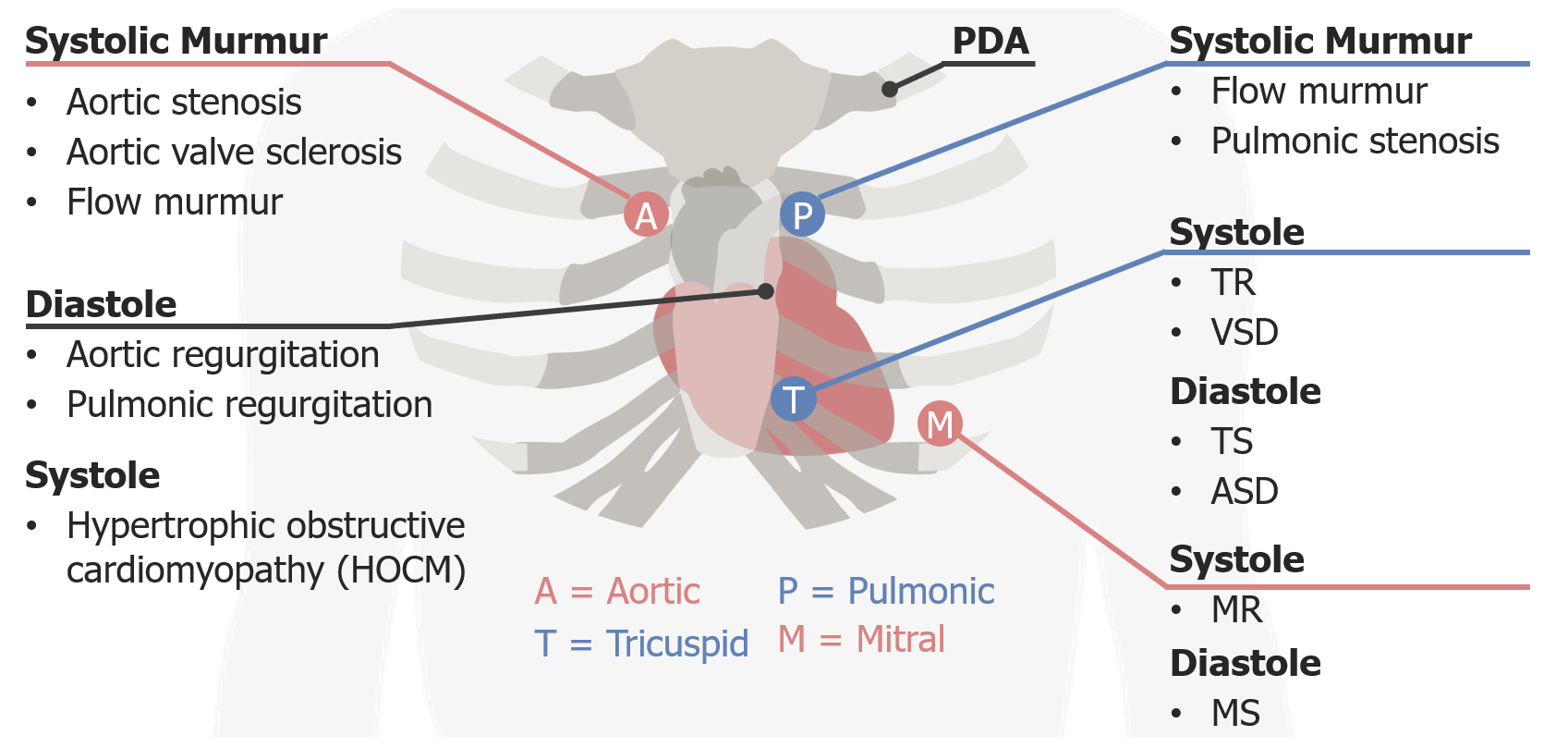
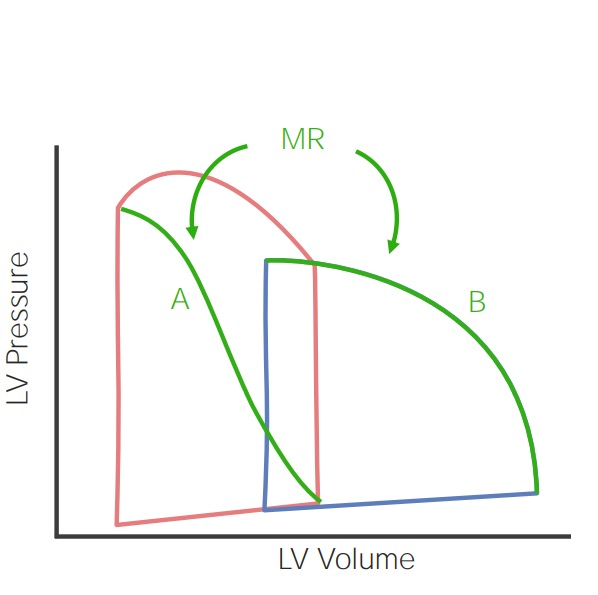
00:01 Alright, so the next murmur we're going to look at is that of mitral regurgitation. 00:04 This is an extremely common murmur which you will definitely hear within the first 10 to 20 patients you listen to on the wards. 00:11 A mitral regurgitation, unlike aortic stenosis, will be predictably be heard over the mitral area, so we're going to listen best to it down here at the apex. 00:20 A note about the apex by the way. 00:24 You know, the aortic and pulmonic areas are very clear, right? They're just to the left and right of the sternum throughout the 2nd intercostal space. 00:32 It's very predictable, a very discreet specific location. 00:35 The same thing goes with the tricuspid area, down here in the left lower external border at the approximately 4th-5th intercostal space. 00:45 In contrast, the aortic -- the mitral area at the apex is really going to be different depending upon the patient, it's not going to be in the exact or the same place, you know, 2 cm distal to the nipple line. 00:57 It's going to vary depending upon the patient so unlike finding these areas, when you're trying to look for the mitral area, you have to migrate around until you find the place where your mitral valve is loudest. 01:09 So, with that said, if I'm listening for a mitral regurgitant murmur, I'm going to be migrating around to find the place where it's loudest. 01:16 Again, L-I-S-P. I is for intensity. 01:20 The grade of this murmur, unlike aortic stenosis, does predict the severity of the mitral regurgitation itself and the extensive disease in the mitral valve, so intensity will matter. The shape for a classic mitral regurgitation murmur is so called holosystolic. 01:38 That is it's the same from beginning to end and it may last for a short time in systole or throughout systole, but either way it should be of a constant amplitude. 01:47 So the typical onomatopoeia phrasing that we use to describe a mitral regurgitation murmur is also high in pitch and it goes like this [making a sound]. 02:01 You can hear that it's the exact same amplitude, almost the square wave form in sound from one beat to the next. 02:08 The timing, again, can occur throughout systole or early or late. 02:12 It doesn't help too much with deciding that the extent or severity of the mitral regurgitation so much as the amplitude or intensity or grade of the murmur would. 02:23 So, let me take a listen for mitral regurgitation. 02:33 As its high pitch incidentally you'll note that I'm using the diaphragm. 02:37 And now let's say that I can sort of hear a murmur but I'm not a 100% convince that it's there, maybe it's a 1 out of 6 murmur or perhaps I'm worried that maybe this is just a murmur of aortic stenosis which as I said could be all the way down there. 02:52 Fortunately, in cardiology, there are a number of different bedside maneuvers that we can do which predictably will increase or decrease the amplitude of a variety of murmurs. 03:03 And so the first one of these that we are going to demonstrate is called the handgrip maneuver. 03:07 If you would mind grabbing that towel for us. 03:09 So the handgrip maneuver is designed to increase afterload, so when I have him squeeze that towel with all his might for 10 seconds, he's going to be contracting all the muscles in his upper extremities which is going to increase peripheral vascular resistance. 03:26 That means that when his left ventricle contracts, he's trying to forcibly eject blood out of the aorta and out into his the great vessels of his upper chest and neck, there's going to be some resistance. 03:39 And so, if you already have a diseased mitral valve, when that left ventricle contracts and is trying to push blood outwards, some of it is going to get pushed backwards to an incompetent mitral valve. 03:51 So this maneuver, handgrip, is an attempt to accentuate or exaggerate his mitral valve murmur, his mitral regurgitation. 04:00 So let's give that a try. Importantly, I want him to do it for 5 or 10 seconds. 04:05 Go ahead and squeeze it with all your might. 04:18 Great, so in this case, fortunately our patient does not have mitral regurgitation, but this would be the way to bring it out if I thought that it was going to be there.
About the Lecture
The lecture Mitral Regurgitation – Systolic Murmurs by Stephen Holt, MD, MS is from the course Examination of Cardiovascular and Respiratory System.
Included Quiz Questions
Which features are the MOST accurate descriptions of the murmur of mitral regurgitation?
- Located at the apex of the heart, heard during systole, the intensity of the murmur predicts the extent of valvular disease
- Located at the apex of the heart, heard during diastole, may radiate to the right carotid area
- Located anywhere in the chest, heard during systole, the intensity of murmur correlates with the degree of valvular disease
- Located usually at the right upper sternal border, heard during systole, may radiate to the right carotid area
- Located at the left lower sternal border, heard during diastole, the intensity of murmur does not correlate with the degree of stenosis
How does the handgrip maneuver affect a heart murmur due to mitral regurgitation?
- The intensity of the murmur gets louder due to increased afterload.
- The intensity of the murmur gets louder due to increased preload.
- The intensity of the murmur gets louder due to decreased afterload.
- The intensity of the murmur gets louder due to increased contractility.
- The intensity of the murmur gets softer due to increased afterload.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
1 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |
1 customer review without text
1 user review without text