Playlist
Show Playlist
Hide Playlist
Major Histocompatibility Complex (MHC) and MHC Disparity
-
14 Slides Transplantation Immunology.pdf
-
Reference List Immune System.pdf
-
Download Lecture Overview
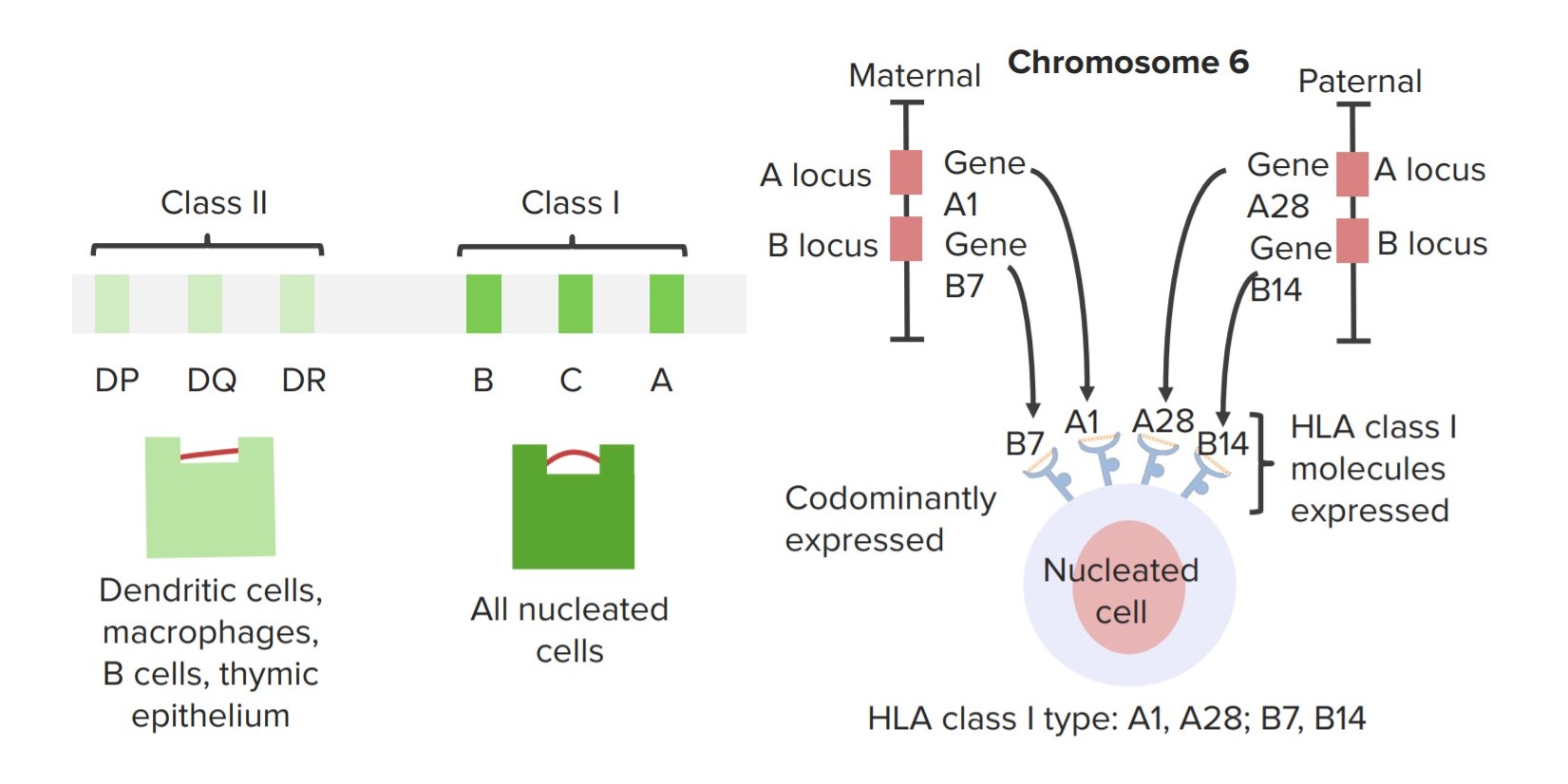
00:01 There are a number of different gene products that contribute towards graft rejection that are seen as foreign by the recipient. 00:10 By far the most important is the major histocompatibility complex. 00:16 It’s a complex of genes that encode these proteins. 00:19 They’re involved in histocompatibility, in other words tissue compatibility. 00:24 And they’re the most important, hence the name MHC - major histocompatibility complex. 00:31 We inherit from our parents three MHC Class I genes - HLA-A, HLA-B and HLA-C. 00:43 The product of these genes are present on all nucleated cells. 00:50 MHC Class II comprises HLA-DP, -DQ and -DR. 00:59 The products of these genes are present on dendritic cells, macrophages, B-cells and thymic epithelium. 01:08 This is in addition to the MHC Class I molecules because of course dendritic cells, macrophages, B-cells and thymic epithelium are nucleated cells. 01:17 And all nucleated cells have Class I. 01:19 So these particular cells have both Class II and Class I. 01:25 The MHC is present on chromosome 6. 01:27 And we inherit one set of genes from our mother and one set of genes from our father. 01:32 So we’re-- here we have the HLA-A locus on the maternally inherited chromosome. 01:38 And this particular individual has the variant of HLA-A called A1. 01:46 And at the B locus, they have the variant B7. 01:51 The genes from the paternal chromosome will also be expressed because these genes are co-dominantly expressed. 02:01 And this individual has inherited HLA-A28 from the father and also HLA-B14 from the father. 02:11 And of course there’ll be the HLA-C and the Class II genes present on the professional antigen presenting cells that we just mentioned - dendritic cells, macrophages, B-cells, thymic epithelium. 02:24 So this individual will be HLA Class I type A1, A28, B7 and B14. 02:37 The MHC gene complex is by far the most polymorphic gene complex that we have; in other words, at each locus in the genome there is the potential for huge variability between one individual and another. 02:53 And here we can see the approximate number of different variants for the different MHC molecules. 03:00 So for the Class II molecule HLA-DP, the α-chain can be encoded by more than 40 different sequences. 03:10 We’ll each have one particular sequence inherited from our mother and one particular sequence inherited from our father. 03:15 But there’s a-- the potential to have any one of 40 or so different sequences. 03:21 For DQ, there are more than 50 different variants that have been described. 03:26 For DR there’s only about seven different variants for the α-chain. 03:32 Turning to the Class I, for HLA-B there are over 4000 different sequences. 03:41 You’ll inherit two of these, one from your mom and one from your dad. 03:44 But the potential different sequences that you could inherit, there are over 4000. 03:50 For HLA-C, over 2000 different variants have been described. 03:55 And for HLA-A, over 3000 different variants have been described for the α-chain of the MHC Class I molecule. 04:04 Variability within the peptide binding groove of MHC Class II molecules is contributed by both the α-chain and the β-chain. 04:12 And for HLA-DP, there are over 600 variants described for the DP β-chain. 04:19 Over 900 variants for the DQ β-chain. 04:24 And around about 2000 variants for the DR β-chain. 04:30 The β-chain of MHC Class I is non-polymorphic, it doesn’t vary from one individual to another and it’s not part of the peptide binding groove. 04:40 Let’s look at the disparity between different individuals with respect to MHC. 04:47 So here we have two individuals, one of which is DP2 and DP8. 04:54 Remember one gene variant inherited from the mother, one from the father. 04:59 The other individual is DP1 and DP5. 05:03 So they don’t share any DP sequence. 05:06 Both of their DPs are different. 05:10 The one individual has DQ7 and DQ9, the other DQ3 and DQ4. 05:16 So again, they’re completely different at the DQ locus. 05:20 However at the DR locus, they both have DR2. 05:25 Although the other variant of DR that they have differs. 05:28 One has DR4, the other has DR5. 05:31 But there’s a match here at the DR2 level. 05:36 Looking at the class I genes, the one individual is A2 and A6, the other individual is A4 and A6. 05:45 So again there is one of these alleles that is matched between these two individuals. 05:50 They differ at the B-- HLA-B with one of the alleles but not the other. 05:56 So they share B1 but a different one has B3, one has B4. 06:02 And then at the C-- HLA-C allele, they are totally different. 06:07 So there is partial sharing between these individuals, in that they share DR2, HLA-A6 and HLA-B1. 06:19 Looking at the influence of MHC matching on graft survival, we can see here that the greater the number of mismatched HLA alleles, then their survival at five years in this instance, of renal allografts decreases. 06:37 So in other words, the closer the match, the better the chance of longer term survival of the graft.
About the Lecture
The lecture Major Histocompatibility Complex (MHC) and MHC Disparity by Peter Delves, PhD is from the course Transplantation Immunology. It contains the following chapters:
- A Closer Look at the Major Histocompatibility Complex
- MHC Disparity between Individuals
Included Quiz Questions
Which type of major histocompatibility complex (MHC) 1 locus is the most polymorphic? (HLA: human leukocyte antigen)
- HLA-B
- HLA-A
- HLA-C
- HLA-DQ
- HLA-DR
Which of the following cells do NOT express either major histocompatibility complex (MHC) class 1 or MHC class 2?
- Red blood cells
- Macrophages
- B cells
- Dendritic cells
- Monocyte
Which of the following regarding major histocompatibility complex (MHC) molecules is INCORRECT?
- DP, DQ, and DR α chains are equally polymorphic.
- Genes are located on chromosome 6.
- Genes from maternal and paternal MHC are codominantly expressed.
- Beta-2 microglobulin of MHC Class I is non-polymorphic.
- Beta chain of DR is the most polymorphic region on MHC Class II.
How does the number of HLA mismatches correlate with long term survival?
- The higher the number of mismatches, the lower the chance of long term survival.
- The higher the number of mismatches, the higher the chance of graft acceptance.
- The higher the number of mismatches, the lower the chance of chronic rejection.
- The lower the number of mismatches, the lower the chance of long term survival.
- Number of mismatches has no effect on long term survival.
Customer reviews
5,0 of 5 stars
| 5 Stars |
|
5 |
| 4 Stars |
|
0 |
| 3 Stars |
|
0 |
| 2 Stars |
|
0 |
| 1 Star |
|
0 |